Impetigo contagiosa
| Classification according to ICD-10 | |
|---|---|
| L01.0 | Impetigo contagiosa |
| ICD-10 online (WHO version 2019) | |
The impetigo (from Latin impetigo , usually a scaly or oozing rash '; of impetere "fall", "attack"; and contagiosus "contagious") is a highly contagious bacterial skin disease with a peak incidence in children and newborns. The terms impetigo vulgaris , also "rash", "rash", "lichen", "lichen", "lichen", "lichen", "drag", "drag shit" or "tow ladder" are used synonymously.
root cause
The cause of the infection are bacteria, which spread through the skin with specific pathogenicity factors and can destroy tissue. Both in the large-bubble form (bullous impetigo) and in the small-bubble form, mainly Staphylococcus aureus can be found. With both forms, but especially the small-bubble form, Streptococcus pyogenes ( group A streptococci ) can often be the trigger of the skin disease. Mixed infections are also possible.
Children are most often affected, as the disease can spread epidemically through smear infection in community facilities (schools, kindergartens) or among siblings. Impetigo, however, is also observed in all other age groups, especially in patients with atopic eczema , since micro-trauma when scratching the skin allows the pathogens to penetrate deeper skin layers very easily.
Clinical picture
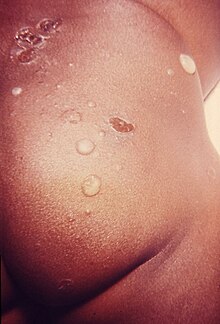
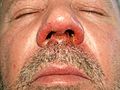
Basically, a distinction is made between a small-bubble and a large-bubble variant of impetigo contagiosa. Both forms begin predominantly on the face with red spots (macules), which quickly turn into blisters filled with water-clear liquid. The vesicles are each surrounded by a narrow zone of inflammation.
Small-bubble impetigo contagiosa
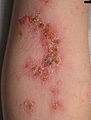
In impetigo contagiosa with small bubbles, the vesicles are often invisible. The walls of the vesicles are very thin, so they burst quickly. The base of the bladder is heavily oozing from exudation . If the liquid dries, characteristic honey-yellow crusts form on the reddened surface.
Large bladder impetigo contagiosa
In large-blistered impetigo contagiosa, numerous vesicles are present. At first they are also filled with water-clear liquid, which, however, initially becomes whitish-gray and then creamy-purulent. If the blisters burst or scratched, red, eroded surfaces that shine with a damp shine appear. In contrast to the small-bubble impetigo contagiosa, hardly any stronger incrustations form.
therapy
According to the current treatment guidelines of the German Dermatological Society, systemic antibiotic therapy is provided in serious cases. Hygienic measures play an important role in the treatment: Avoiding scratching the affected areas of the skin, regular hand washing and regular hot washing of clothing and towels that are close to the body contain the infection and prevent further infections. The fingernails of those affected should be trimmed short so that the possibility of scratching and thus spreading is reduced. Bandaging or covering and avoiding scratching promotes the spontaneous healing tendency of the disease.
Local therapy can be supported with ointments containing antibiotics ( fusidic acid , mupirocin , retapamulin). Disinfecting solutions, baths and poultices can be used in addition. Only advanced cases require systemic treatment with antibiotics (e.g. with cephalosporins ).
course
The incubation period is between two and ten days, possibly longer. The disease is infectious until the open, purulent areas of the skin have healed.
With consistently applied therapy, impetigo contagiosa usually heals without consequences. The skin flakes and crusts separate from healthy skin so that they either fall off or can be removed by hand. The pathogens rarely reach deeper layers of the skin and cause nail bed, nail fold inflammation or abscesses . Community facilities such as kindergartens or schools may only be visited again by the patient after the infected skin areas have healed.
An inflammatory reaction of the kidneys ( post-streptococcal glomerulonephritis ) occurs in about 5% of patients after the infection (only in the small-bubble form ). This usually heals without consequences.
Legal notices
Because of the risk of infection, it should be noted that treatment of impetigo contagiosa in Germany according to § 24 Infection Protection Act (IfSG) i. V. m. Section 34 (1) IfSG " insofar as only doctors are permitted to practice medicine professionally ", which means that alternative practitioners or other health professions are not allowed to perform treatment.
In addition, there are special rules for sick people in public institutions according to § 34 IfSG to prevent spread. According to Paragraph 6 in conjunction with Paragraphs 1 and 3, the management of communal facilities must immediately notify the responsible health department if persons or employees cared for in their facility develop impetigo contagiosa (infectious rhinitis) or are suspected of it.
Individual evidence
- ^ Paul Richter: Contributions to the history of leprosy. In: Sudhoff's archive. Volume 4, 1911, pp. 323-352; here: pp. 335–337 and 340 f.
- ^ A b c d Otto Braun-Falco, Helmut Heinrich Wolff: Dermatology and Venereology. 2005, ISBN 3-540-40525-9 , p. 94.
- ↑ Otto Braun-Falco, Helmut Heinrich Wolff: Dermatology and Venerology. 2005, ISBN 3-540-40525-9 , p. 95.
- ↑ http://www.awmf.org/leitlinien/detail/ll/013-038.html
- ^ R. Jones, T. Fritsche, H. Sader, J. Ross: Activity of retapamulin (SB-275833), a novel pleuromutilin, against selected resistant gram-positive cocci . In: Antimicrob Agents Chemother . tape 50 , no. 7 , 2006, p. 2583-25836 , doi : 10.1128 / AAC.01432-05 , PMID 16801451 , PMC 1489758 (free full text).
- ^ European Medicines Agency - Find medicine - Altargo. Retrieved February 8, 2012 .
- ↑ a b § 24 Treatment of Communicable Diseases. Retrieved February 8, 2012 .
- ↑ Streptococcus pyogenes infections. In: RKI-Ratgeber. Robert Koch Institute, May 2, 2018, accessed on March 21, 2020 (notification obligation according to IfSG).
literature
- ML O'Dell: Skin and wound infections: an overview. In: Am Fam Physician. 1998 May 15; 57 (10), pp. 2424-2432. Review. PMID 9614412
- DL Stulberg, MA Penrod, RA Blatny: Common bacterial skin infections. In: Am Fam Physician. 2002 Jul 1; 66 (1), pp. 119-124. Review. PMID 12126026