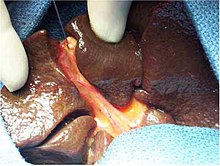
Biliary atresia
| Classification according to ICD-10 | |
|---|---|
| Q44.2 | Atresia of the bile ducts |
| ICD-10 online (WHO version 2019) | |
The Biliary atresia ( English : biliary atresia, BA) is a rare disease with closure ( atresia ) of the bile ducts exclusively in newborns (neonatal period) occurs. The cause is still unclear. In developed countries, biliary atresia is the leading cause of the need for liver transplantation in infancy.
Occurrence
The prevalence at birth varies worldwide between 1: 20,000 and 1: 3,100 live births, with an increase in the disease rate in Asia and the Pacific region . In Western Europe, around one child in 18,000 falls ill within the neonatal period. Girls are affected slightly more often than boys. About a tenth of the cases are associated with additional congenital malformations (e.g. heart defects, polysplenia) and are summarized as a syndromic form . The sole occurrence of obstruction of the biliary tract is called a nonsyndromic form . Internationally, it has become established that the distinction between extra- and intrahepatic forms is no longer made, since the disease affects the entire liver and all bile ducts.
root cause
The etiology (cause) of biliary atresia is largely unknown. Various indications - for example changes in the ultrasound structure of the liver in the womb - suggest that the narrowing of the biliary tract begins early in pregnancy. Extensive studies on the influence of viral infections have assumed a connection with cytomegaly , respiratory syncitial , Epstein-Barr and human papilloma viruses . In contrast, no connection to the hepatitis viruses A , B or C could be found. Even genetic factors appear to play a role: some studies report familial and ethnic (in the Pacific or parts of the US) clusters, as were certain HLA types (HLA-B12; haplotype A9-B5 haplotype A28-B35) common in affected Children found. A histopathological examination under the microscope reveals inflammatory damage to the bile ducts with an increase in the connective tissue (sclerosis) and narrowing up to the obstruction of the bile ducts.
Symptoms
After birth, the children develop prolonged jaundice ( jaundice ) which, in contrast to normal neonatal jaundice, is mainly caused by water-soluble "direct" bilirubin . They deposit discolored feces (so-called acholic stool) and the urine turns brown. An enlargement of the liver ( hepatomegaly ) can be observed as the third key symptom . There is very often an association with facial dysmorphism, eye malformations, cardiac vitia and skeletal malformations. The general condition of the children is initially good. Not even thriving is affected in the first few months. Only later does a weight loss and increasing hyperexcitability set in. As a sign of an increase in pressure in the portal vein of the liver ( portal hypertension ), an enlarged spleen and water accumulation in the abdomen ( ascites ) are added. Because too few bile acids get into the intestine with the disturbed flow of bile , fat digestion and thus also the absorption of fat-soluble vitamins , especially vitamin K, is disturbed, which can lead to a tendency to bleed.
diagnosis
In every child with neonatal jaundice that lasts longer than two weeks, biliary atresia must be actively excluded because of the particular prognostic importance of an early diagnosis. The first step is a laboratory differentiation of bilirubin into the water-soluble, conjugated (direct) and the water-insoluble, unconjugated (indirect) form. An ultrasound examination after a four to twelve hour fasting period confirms the suspicion that the gall bladder cannot be visualized or has shrunk, increased echogenicity of the hilum or a cyst in the hilum. If the gallbladder is normal on ultrasound and the suspicion persists, the anatomical structure and the patency of the biliary tract must be examined with an X-ray contrast agent image, a cholangiography . Any final diagnostic uncertainties can be clarified with a liver biopsy .
treatment
If left untreated, the disease leads to a gradual remodeling of connective tissue in the liver ( cirrhosis of the liver ) and death within the first few years of life. In order to temporarily restore the flow of bile, the affected children first undergo an operation according to Kasai , a hepatoporto enterostomy . The changed biliary tract including the connective tissue between the right and left portal vein branches in the hepatic porta are removed. Then a loop of intestine is sewn onto the open porta hepatica, so that the bile can, so to speak, drain out of the porta liver into the intestine. Additional drug treatment either with anti-inflammatory agents, which are supposed to slow down the progressive remodeling of the liver tissue, or with substances that can improve the flow of bile, is recommended on various occasions, but is controversial due to the lack of evidence of a long-term benefit.
If the bile flow recovers after the Kasai operation, this is reflected in a decrease in jaundice and an increasing brown coloration of the faeces. But even if this favorable situation occurs, two thirds of the patients develop cirrhosis of the liver caused by the biliary blockage. This, or a primary failure of the Kasai surgery, requires a liver transplant. The organ is usually transplanted in the second year of life, but this can also be necessary at the age of six months. Due to the development of new transplantation procedures (liver splitting, living donation), the availability of this treatment method has recently increased.
forecast
Survival with one's own liver into adulthood is only observed in around one tenth of patients. Nevertheless, today around 90% of all those affected can hope for survival with a largely normal quality of life. Bile duct atresia, which are associated with additional malformations of the spleen , generally have a poorer prognosis. Likewise, the further the changes in the biliary tract reach into the liver, the less likely it will be a successful treatment. The chances of success for the Kasai operation decrease with increasing age of the children, which is why an early diagnosis is of particular importance. Additionally, the overall prognosis improves with the availability of a liver transplant. In the Hamburg transplant center, the survival rate of children who received a liver transplant in infancy was 87% after two years.
Web links
Individual evidence
- ↑ a b E. F. Grabhorn et al.: Liver transplantation in infancy. In: Monthly Pediatrics. 2007, 155, pp. 381-389. doi: 10.1007 / s00112-007-1485-x .
- ↑ a b c d C. Chardot: Biliary atresia. Review In: Orphanet Journal of Rare Diseases. 2006; 1, p. 28. PMC 1560371 (free full text).