Jaundice
| Classification according to ICD-10 | |
|---|---|
| R79.8 | Other specified abnormal blood chemistry findings |
| ICD-10 online (WHO version 2019) | |
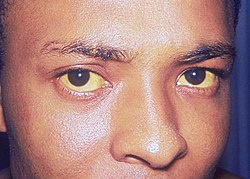
The jaundice (formerly and Latin jaundice ; from ancient Greek ἴκτερος , íkteros , "jaundice"), and jaundice (from Middle High German gëlsuht of batteries also Gallsucht ), is a yellowing of the skin , mucous membranes and the hides of the eyes by an increased concentration of bilirubin in blood. It is a symptom already described in ancient times in the Near East , which can occur in various diseases.
In linguistic usage, jaundice and liver inflammation are often equated ("jaundice epidemic" in the case of increased hepatitis diseases in the 1960s and 1970s). However, jaundice today is not a disease, but a symptom that occurs in many diseases, u. a. also with hepatitis (for example viral hepatitis, the sporadic form of which was previously known as icterus simplex or icterus catarrhalis ) and diseases of the biliary tract.
The jaundice is based on a disturbance in the bilirubin metabolism . Bilirubin is a breakdown product of the red blood pigment hemoglobin . The increased seizure or reduced excretion of bilirubin initially increases the serum concentration ( hyperbilirubinemia ) and then exits through the vascular endothelium with storage in body tissue.
From a serum level of more than 35 μ mol / l (= 2 mg / dl), the color change first appears on the (otherwise white) dermis of the eye (sclera) (scleric terus). As the values continue to increase, the yellowish changes can finally also be observed on the skin and mucous membranes. The body fluids and other organs are also affected. The urine can be dark brown ( bilirubinuria ), while the stool can be light or white.
Since the liver plays a central role in the underlying bilirubin metabolism, one can distinguish the following causes of jaundice, depending on the localization of the disorder:
- Prehepatic (with a cause "in front of the liver", usually associated with an increased attack of bilirubin due to hemolysis )
- intrahepatic (due to liver damage or liver dysfunction) as well
- posthepatic (if the bile duct system downstream of the liver is disturbed; usually a disturbance of the bile outflow)
Furthermore, the bilirubin uptake in the liver is slightly chronically reduced in around five percent of the population due to a genetic defect. This disorder is known as Gilbert syndrome . In these cases, mild forms of jaundice, particularly yellowing in the area of the conjunctiva, occur regularly. This type of jaundice is harmless and does not require treatment if no other physical abnormalities are observed.
Hemolytic jaundice (prehepatic)
In prehepatic jaundice, the increased breakdown of red blood cells ( erythrocytes ) during hemolysis leads to an increased attack of unconjugated bilirubin. Physiologically, the same mechanism occurs in neonatal icterus ( icterus haemolyticus neonatorum ). Shortly after birth, the erythrocytes loaded with fetal hemoglobin are increasingly broken down and replaced by newly formed red blood cells. The neonatal icterus is a sign of this ongoing reaction and is usually harmless. If the bilirubin levels are massively increased shortly after birth (e.g. due to an existing rhesus incompatibility ( erythroblastosis ) or in premature births ) there is a risk of kernicterus , damage to important centers of the central nervous system with a poor prognosis .
Prehepatic jaundice can also occur with blood transfusion complications (death of blood cells), as a result of a pulmonary infarction and with large bruises.
Hepatocellular jaundice (intrahepatic)
Since several steps of bilirubin metabolism take place in the liver, there are accordingly different possibilities for (intra) hepatic jaundice. Essentially, the following processes can be disrupted:
- Bilirubin uptake by liver cells
- Bilirubin conjugation (conversion of water-insoluble, unconjugated into water-soluble, conjugated bilirubin with the help of glucuronic acid )
- Transport of conjugated bilirubin out of the liver cell
- Drainage from the biliary tubules of the liver into the intrahepatic biliary tract
Disturbance of bilirubin uptake
Insufficient uptake of unconjugated bilirubin can be caused on the one hand by liver cell damage, for example in the context of viral hepatitis or acute liver failure , or on the other hand by overloading the cell's own transport system. Some drugs (some antibiotics, for example) have to be excreted through the same routes and can compete with bilirubin.
Disturbance of bilirubin conjugation
The trigger is mostly genetic defects in the enzymes involved (especially UDP-glucuronyltransferase ). The best known diseases in this context are the Gilbert-Meulengracht syndrome and the Crigler-Najjar syndrome .
Disturbance of bilirubin transport
In addition to liver cell damage of various causes, inherited disorders of the necessary structures can also be triggering. These include the Dubin-Johnson syndrome or the Rotor syndrome . When Inanitionsikterus mobilized fatty acids displace bilirubin from the transport proteins.
Disturbance of the bile outflow
Similar to posthepatic jaundice, in addition to bilirubin, a number of other substances are also affected by the lack of elimination. Therefore, it is referred to as intrahepatic cholestasis .
Cholestatic jaundice (posthepatic)
Here there is a disruption of the outflow of bile from the liver through the common bile duct into the duodenum . Since various other substances are excreted in the bile in addition to bilirubin, various other symptoms occur in addition to yellowing of the skin and mucous membranes. Together, all phenomena are subsumed under the term cholestasis . Most often it is gallstones that get stuck in the duct and obstruct it. But tumors (from pancreas , gallbladder , bile ducts or the duodenum ) can be sudden constriction of the duct and thus to an obstructive (or obstructive conduct). In contrast to gallstones, which often lead to biliary colic at the same time , tumorous changes are often painless at this stage. Therefore, every painless jaundice should be classified as suspicious of malignancy and medically clarified immediately (like all other forms, however). Bile duct atresia in newborns is a rare congenital cause of posthepatic jaundice .
treatment
Treatment for jaundice depends on the trigger. Gallstones, for example, can be removed using special endoscopes . In some cases, a diseased gallbladder must be surgically removed. If drugs have damaged the liver, the jaundice usually disappears when they are no longer taken. Antiviral agents can help against jaundice caused by viruses.
literature
- Pschyrembel: Clinical Dictionary 2011. 262nd edition. de Gruyter, Berlin 2010, ISBN 978-3-11-021152-8 .
- Böcker, Helmut Denk, Philipp Ulrich Heitz: Pathology . Urban & Schwarzenberg, Munich 1997 ISBN 3-541-15891-3 .
- Walter Siegenthaler, businessman, Hornbostel, Waller: textbook of internal medicine . Thieme, Stuttgart 1992 ISBN 3-13-624303-X .
Web links
- Hepatitis A. RKI guide for doctors. at the Robert Koch Institute
- Patient information from the German Association of Internists
Individual evidence
- ↑ List of historical disease names on bionity.com, accessed on October 22, 2016
- ↑ Franz Köcher : The Babylonian and Assyrian medicine in texts and studies. I-VI, Berlin 1963-1980, BAM 188: 1-2; 578: IV-26.
- ↑ Martha Haussperger : Did empirical medicine exist in the Near East before Hippocrates? In: Würzburger medical history reports 17, 1998, pp. 113–128; here p. 120 f.
- ↑ Hans Adolf Kühn: Diseases of the liver. In: Ludwig Heilmeyer (ed.): Textbook of internal medicine. Springer-Verlag, Berlin / Göttingen / Heidelberg 1955; 2nd edition ibid. 1961, pp. 847-875, here: pp. 854-861: Viral hepatitis (hepatitis epidemica and hematogenous [serum] hepatitis).
- ↑ Horst Kremling : On the development of clinical diagnostics. In: Würzburger medical history reports 23, 2004, pp. 233–261; here: p. 250 ( jaundice ).