Intraocular pressure
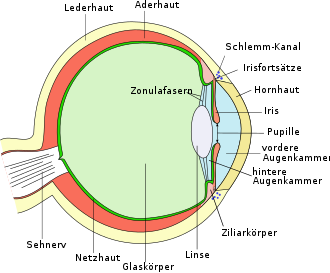
As intraocular pressure (Synonyms: intraocular pressure , medical: Tensio ) refers to the physical pressure put on inside the eye. It causes a consistently smooth curvature of the corneal surface, a constant distance between the cornea , lens and retina of the eye as well as an even alignment of the photoreceptors on the retina. In addition, it maintains the stable spherical shape of the eyeball. The intraocular pressure is regulated by the aqueous humor . It is formed by the epithelium of the ciliary body and passes between the iris and the lens of the eye through the pupil into the anterior chamber of the eye. From there it flows for the most part via the trabecular structure of the chamber angle through Schlemm's canal into the episcleral venous system . The intraocular pressure depends on the aqueous humor production and the drainage resistance of the trabecular network.
Measurement

The normal intraocular pressure is between 10 and 21 mmHg . There are different methods for measuring it, which are summarized under the term tonometry . Ophthalmologists examine the intraocular pressure manually by gently pressing ( palpatory ) on the half-closed eye. Experienced examiners can estimate the intraocular pressure within certain limits to an accuracy of about 2 mmHg. Of apparatus it is usually a so-called tonometer by Goldmann determined. The force is measured that is required for a defined mechanical flattening of the cornea , which has previously been anesthetized by drugs . Alternatively, a non-contact measurement using non-contact tonometry (flattening of the cornea with an air blast) can be carried out. Further methods are impression tonometry and dynamic contour tonometry . Although applanation tonometry has so far been the method of choice, all measurement methods also have their disadvantages. Since the intraocular pressure can fluctuate during the day, several measurements spread over the day can be displayed (daily pressure profile).
pathology
If less aqueous humor flows out than is produced, the intraocular pressure increases. A permanent increase above about 21 mmHg is usually not tolerated and can lead to damage to the optic nerve , glaucoma (glaucoma). Within certain individual limits, the eye can withstand an increase in intraocular pressure without damage ( tension tolerance ), but the higher the pressure rises and the longer this situation lasts, the more likely damage is to be expected. On the other hand, with reduced tolerance of tension, glaucoma can also occur without an increase in intraocular pressure ( normal pressure glaucoma ). Increased intraocular pressure is a very important, but not the only key symptom for glaucoma. If an increase in pressure were used as a diagnostic criterion, half of the glaucomas would be overlooked. Increased intraocular pressure without any damage to the eye, optic nerve, visual field, papilla or retina is called ocular hypertension .
The explicit examination of the chamber angle is carried out with a so-called contact lens and called gonioscopy .
There are a number of risk groups that are particularly prone to a pathological rise in pressure. This is another reason why ophthalmologists recommend a preventive examination.
A permanently too low intraocular pressure can lead to glaucoma ( low pressure glaucoma ), in extreme cases to massive symptoms up to retinal detachment and / or shrinkage of the eyeball ( phthisis bulbi ). An acute loss of pressure, for example due to a traumatic outflow of aqueous humor or vitreous humor, can also be a possible trigger for this.
Treatment of pathological increase in pressure
There are conservative and surgical options for treating increased intraocular pressure with the aim of either improving or normalizing the outflow of aqueous humor, or reducing aqueous humor production. Drug therapy is carried out with eye drops, so-called anti - glaucoma . In addition to the beta blockers , which have been used successfully for a long time, prostaglandins and alpha agonists have been increasingly used to lower pressure in recent years . Also include carbonic anhydrase inhibitors to the active preparations.
Ophthalmic surgical procedures come into question when the drug therapy does not lead to the treatment goal or does not lead to it alone. In addition to the conventional methods such as trabeculotomy or iridectomy, there are a number of laser surgical interventions such as argon laser trabeculoplasty (ALT) or selective laser trabeculoplasty (SLT) .
literature
- Theodor Axenfeld (founder), Hans Pau (ed.): Textbook and atlas of ophthalmology. 12th, completely revised edition. With the collaboration of Rudolf Sachsenweger and others Gustav Fischer, Stuttgart and others 1980, ISBN 3-437-00255-4 .
Web links
Individual evidence
- ^ Pschyrembel clinical dictionary. With clinical syndromes and nouns anatomica. = Clinical Dictionary. Edited by the publisher's dictionary editor under the direction of Christoph Zink. 256th, revised edition. de Gruyter, Berlin et al. 1990, ISBN 3-11-010881-X .
- ^ Albert J. Augustin: Physiology for the Oral Examination: Questions and Answers . 2nd Edition. Springer-Verlag, 2013, ISBN 978-3-642-97698-8 , pp. 191 ( limited preview in Google Book search).
- ^ Franz Grehn: Ophthalmology. Springer Verlag 2013, page 334, ISBN 978-3-662-05918-0 .
- ↑ a b c Patient information from the Professional Association of Ophthalmologists in Germany (BVA) and the German Ophthalmological Society (DOG) (PDF; 121 kB).
- ^ EM Hoffmann, J. Lamparter: Delimitation of ocular hypertension , in: "Der Ophthalmologe", edition 8/2016