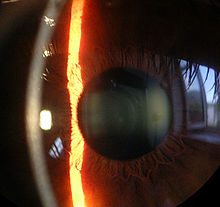
Cornea
The cornea ( Latin cornea , Germanized also cornea , Greek keras = horn, keratoeides chitōn = cornea) is the crystal-clear , arched front part of the outer eye skin, wetted by tear fluid , and provides a large part of the light refraction . It is the frontal closure of the eyeball .

1. sclera ( sclera )
2. choroid ( choroid )
3. Schlemm's canal ( sinus venosus sclerae / venous plexus sclera )
4. orris root ( Radix iris )
5. cornea ( cornea )
6. iris ( Iris )
7. Pupil ( Pupilla )
8. Anterior chamber of the eye ( Camera anterior bulbi )
9. Posterior chamber of the eye ( Camera posterior bulbi )
10. Ciliary body ( Corpus ciliare )
11. Lens ( Lens )
12. Vitreous body ( Corpus vitreum )
13. Retina ( Retina )
14. Optic nerve ( Nervus opticus )
15. Zonula fibers ( Fibrae zonulares )
Outer eye skin ( Tunica externa bulbi ): 1. + 5.
Middle eye skin ( Tunica media bulbi / uvea ): 2. + 6. + 10.
Inner eye skin ( Tunica interna bulbi ): 13.
function
A clear and downright wet cornea is a necessary condition for sharp vision, as it as a "window" of the eyeball with a power of +43 diopters the bulk of the refraction of light for image focusing accepts (the entire human eye has a refractive power diopter of about 60, Emmetropauge according to Gullstrand 58.635 dpt). The refractive power of +43 D is only achieved because there is aqueous humor behind the cornea . If there were air in the eye chambers , the cornea would be a minus lens ( diverging lens ), since it is thinner in the center than at the edge.
anatomy
shape
The cornea is a clear disc, circularly demarcated from the sclera (dermis) by the limbus . The normal human cornea is mostly horizontally elliptical (diameter 11.7 mm × 10.6 mm) and is spherically arched. The radius of this bulge is about 7.7 mm. The cornea is thinner in the center (0.52 mm) than at the edge (0.67 mm). If the horizontal radius differs from the vertical radius, one speaks of a corneal curvature ( astigmatism ). The cornea can be deformed by pressure exerted from the outside, for example by dimensionally stable contact lenses , and it then takes minutes to days to return to its original shape . This effect is even used in orthokeratology to compensate for myopia. Lid pressure also influences the shape and thus the refractive power of the cornea. To test this fact, you can look sideways "out of the corner of the eye" for 2 to 3 minutes, which temporarily severely deforms the cornea. As a result, when you look straight ahead, your visual acuity will have changed significantly for a few minutes.
Microscopic layer structure

The human cornea consists of six layers: the epithelial layer (1 in the figure), the Bowman membrane (2), the stroma (3), the Descemet membrane (4) and the endothelial cell layer (5). In a study from 2013, the sixth layer defined between the stroma and Descemet's membrane is a 15 µm thick layer (Dua layer), which consists of 5 to 8 lamellae of collagen type 1 bundles.
Epithelial layer
The surface of the cornea consists of five to six layers of multilayered epithelial cells. The epithelium is on average 40–60 µm thick, with its thickness increasing towards the limbus . From the inside out, the corneal epithelium consists of three different cell types, the basal, wing and squamous cells. The basal cells, which are highly prismatic in shape with a vertically standing nucleus and make up 35–45% of the total thickness of the epithelium, adhere to the basement membrane . These basal cells in the limbal region are able to divide and form the germinal layer epithelium of the cornea. Outside the basal cells are the two- or three-layer wing cells , which consist of former basal cells and become flat as they migrate to the outside. After the wing cells have advanced further to the surface, they finally become the squamous cells. These are again arranged in two to three layers and contain fewer organelles and desmosomes (adhesive plates) than the basal and wing cells.
The superficial cells that border the tear film are covered with many micro-villi or microvilli . Their height is about 0.5 µm, their width is 0.3 µm and their spacing is about 0.5 µm. These cells presumably stabilize the tear film and are involved in the absorption of nutrients. If you look at the squamous cells with the micro villi under the electron microscope , two different cell types become visible: long, dark cells and small, light cells. The dark cells are characterized by a high density of micro-villi. They are the older and more mature cells that are shed into the tear film. The small, light cells have significantly fewer micro-villi and are the younger cells. They are therefore not immediately peeled off into the tear film. The structure of the epithelial layer adjacent to the tear film is therefore irregular. Since the cornea is vascular, it is unable to initiate its own immune response . For this reason the Langerhans cells are found in the epithelium near the limbus . These are activated on contact with foreign antigens , migrate from the limbal region to the nearest lymph nodes and trigger an immune reaction against the antigen there.
The interwoven basal cells, which form the lowest cell layer of the epithelium, are on average around 24 μm high and 12 μm wide. The desmosomes on the front and side walls and basal hemidesmosome anchors to the basement membrane make the corneal epithelium resistant to mechanical stress (e.g. eye rubbing).
Bowman membrane
The Bowman membrane, also called Bowman's layer or lamina limitans anterior , lies between the stroma and the basement membrane and is about 12 µm thick. It is less of a membrane than a collection of collagen fibrils and proteoglycans . The collagen fibrils have a diameter of about 20-30 nm, which is about two thirds the thickness of those in the stroma. Since the collagen fibrils are arranged at random and are composed of separate keratinocytes from the stroma, one can assume that Bowman's membrane and stroma are closely interrelated. The front surface of Bowman's membrane is smooth and forms the basement membrane. Furthermore, the Bowman membrane is essential for maintaining the epithelial structure. Once injured, it only heals with scarring because it has no regenerative capacity. Only primates have a distinct Bowman membrane.
Stroma
The stroma makes up about 90% of the total corneal thickness. It is the middle layer of the cornea and with 400–500 µm the thickest of all corneal layers. The corneal stroma - also known as the substantia propria ( own layer ) - consists of fibers, intermediate substances and cells (keratocytes) and is basically a connective tissue in its entirety . The stroma also contains nerve fibers. Cellular components exist in the stroma only in the order of 2–3%. The rest is filled by various components of the extracellular matrix - collagen fibrils , proteoglycans and glycosaminoglycans . When viewed under an electron microscope, the collagen fibrils do not appear fully developed, but retain an embryonic character throughout their life. They are all similarly thick (25–30 nm) and, in contrast to the sclerafibrils, are evenly arranged, parallel within a lamella. With 10% collagen type III and 90% collagen type I, the collagen fibrils have a collagen pattern typical of connective tissue. Every collagen molecule consists of α-protein chains. It is believed that the stroma has about 100–150 lamellae with fibrils that are 5–6 µm thick. The lamellas each intersect at an angle of 90 °, run parallel to the other layers and in this way form a regular grid of particularly high stability. In addition to the swelling equilibrium, this arrangement is one of the prerequisites for the transparency of the cornea. The lamellae are connected to one another with a cement or base substance, which chemically consists of proteoglycans, a mixture of keratin sulfate and chondroitin sulfate. Glycosaminoglycans have numerous surface charges and are therefore able to bind large amounts of water. In this way, the refractive index between the cement substance and the collagen lamellae is kept at the same level in order to ensure the transparency of the cornea. If the equilibrium is disturbed by water absorption or water withdrawal, the refractive index changes and reflections and scattering occur at the interfaces. In the event of excessive water intake, the cement substance swells and pushes the fibrils apart so that congestion in the stroma occurs. Clouds arise. Only potential gap spaces can be found between the lamellae B. expand with hydrogen peroxide to the finest tubular juice columns (Bowman tubes). There are also some corneal cells here.
The keratocytes are fixed cells that resemble the fibrocytes of the connective tissue. They have an elongated shape and have long, branched processes. These cells are connected to one another by protoplasmic bridges and form a syncytium . It is a cell association in which the cells are cytoplasmic. This means that there are no longer any boundaries between them. This arrangement of the cells means that in the event of an irritation, not only the affected cells but also the surrounding cells react. Under normal circumstances, the keratocytes rarely divide. The turnover rate is around 2–3 years. If the cornea is injured right into the stroma, the keratocytes multiply and migrate into the damaged tissue. There they transform into fibroblasts and produce collagens and proteoglycans. Thus the wound is closed with scarring. There are also fibrocytes, which are constantly making collagen. They secure the basic substance of the stroma.
The wandering cells can appear in various forms ( reticulocytes , macrophages , lymphocytes , etc.). In the event of inflammation, these cells migrate to the affected area and provide a good defense. In the limbus area, the lamellae intertwine and merge into the opaque, white dermis (sclera).
Dua layer
The Dua layer is a fine, at the same time very resilient, approximately 15 µm thick membrane that is located between the stroma and Descemet's membrane. Despite its small thickness, it is very tear-resistant and can withstand a pressure load of up to 2 bar. It was only discovered in June 2013 by the English ophthalmologist Harminder Dua , after whom it is also named.
Descemet membrane
The Descemet membrane - also known as Demours membrane, lamina limitans posterior or also rear basement membrane - is the thickest basement membrane in the human body. It is about 3 µm thick at birth and 8-10 µm thick in adulthood. The Descemet membrane increases in thickness over the course of life.
The Descemet membrane is divided into different layers: an unbound, about 0.3 µm thick layer that directly adjoins the stroma, a 2-4 µm thick front layer and a rear shapeless, unbound layer more than 4 µm thick. It is the back layer that increases in thickness in life due to the accumulation of endothelial collagens. It is believed that Descemet's membrane is a product of excretion from the endothelium. However, it compensates for the decreasing pumping capacity of the endothelium with increasing age. Descemet's membrane is transparent, homogeneous, and consists mainly of type VIII collagen fibers and laminin . The collagen fibrils form a regular, two-dimensional hexagonal grid. This makes the Descemet membrane the toughest, elastic membrane in the entire cornea. As a protective layer for the endothelium, the Descemet membrane effectively counteracts infections, mechanical and chemical injuries and enzymatic destruction. Injuries only heal with scarring.
Endothelial cell layer
The endothelium consists of a single layer of hexagonal cells. These are around 5 µm thick and have a diameter of around 20 µm. Usually the cells are regular in shape and similar in size. The cell density in young, adult humans is approximately 3500 cells / mm². However, this number is steadily decreasing with advancing age and regardless of diseases, until it still shows about 2000 cells / mm² in old age. In the first few months of life, cell divisions occasionally occur in the periphery of the endothelium. In adults, however, no such processes have been observed. The division or regeneration of the cells takes place from the trabecular structure of the chamber angle. In the transition area between the cornea and the trabecular structure, there are cell nests that lie in small depressions in Descemet's membrane and that can have cell divisions. Endothelial cells have large nuclei and abundant cytoplasmic organelles such as mitochondria, endoplasmic reticulum, free ribosomes, and Golgi apparatus. The endothelial cells are thus actively involved in the metabolism. The anterior side of the cells is flat against Descemet's membrane, the posterior side against the anterior chamber of the eye. Here the cells are no longer flat, but have micro-villi and folds towards the edge, creating a larger surface area facing the aqueous humor. The endothelial cells are closely connected to one another by complex connection points. But there are no desmosomes. Molecules and electrolytes can pass between the endothelial cells through cleft connections. The mutual connection of the endothelial cell layer creates a barrier that is permeable to the aqueous humor. In comparison, the endothelium is 7 times more permeable to water and 400 times more permeable to ions than the epithelium. Dying or failing cells are replaced by polymorphism and polymegatism . The cells lose their hexagonal shape and cells of different shapes and sizes are created. This process ensures that the Descemet membrane is always completely covered by endothelial cells. A cell density of at least 300-800 cells / mm² is necessary to maintain the endothelial pumping capacity, otherwise the stroma will decompress and the cornea will become cloudy.
One of the most important tasks of the endothelium is to maintain the state of hydration and thus the transparency of the cornea. Another task consists in the synthesis of certain components of the Descemet membrane and the regulation of the exchange of metabolic products between aqueous humor and stroma. The water that penetrates through the metabolic process must be pumped out of the cornea by the endothelial cells using metabolic energy.
embryology
Only the epithelium comes from the embryonic ectoderm , the other corneal layers develop from the mesoderm . The endothelial cells arise from the neural crest . The average corneal diameter of a newborn is 9.5 mm. Corneal growth stops at the end of the second year of life. An adult has an average corneal diameter of 11.5 mm (<10 = microcornea ,> 13 = macrocornea)
physiology
transparency
The transparency of the cornea is due to a regular ultrastructural arrangement of its protein components ( collagens and proteoglycans ) and a strictly defined water content of the stroma. If the water content of the corneal stroma is disturbed, for example due to swelling, the regular arrangement is lost and the light scattering increases. In the extreme case, the light scattering causes the cornea to become completely white. The water content is actively regulated by the endothelial cell layer while consuming oxygen.
Polarization properties
Due to its structured structure (fibrils), the cornea is highly birefringent, i. H. the polarization of light passing through is significantly changed. The birefringence of the cornea generally has a linear as well as a circular component. It depends on the location, the angle of incidence and the light wavelength. In addition, the strength of the corneal birefringence is individually very variable.
Tear film
- → Main article tear film
The tear fluid is largely produced in the lacrimal gland and runs down the corner of the eye and the tear duct into the nasal cavity . The entire tear film consists of two different types of tear films, the pre-ocular and the precorneal tear film. The preocular tear film covers the cornea and conjunctiva located within the fissure of the eyelids. The precorneal tear film, on the other hand, only covers the exposed cornea. The precorneal tear fluid forms a three-layer tear film on the surface of the eye.
When you blink, microscopic vesicles appear that temporarily reduce visual performance. After about 0.5 to 1.5 seconds, they dissolve (depending on the consistency of the film) and the thickening caused by blinking the eye is evened out. After about 5 seconds, the film breaks open and again creates irregularities, as a result of which the visual performance deteriorates again.
metabolism
The outer layers of the cornea are supplied with nutrients and oxygen by the tear fluid , the inner ones by the aqueous humor and the peripheral loop network . From an energetic point of view, the cornea is in the same state as the whole organism is after a 1000 meter run. Deficits in the energy metabolism immediately lead to edema in the cornea and reduced epithelial regeneration. The cornea is therefore dependent on a constant and good supply of nutrients and on a complete elimination of metabolic end products. For the metabolism , glucose (grape sugar) and oxygen , which have to be supplied from the outside , are primarily required. The main metabolic end products are water, carbon dioxide and lactate (lactic acid). Substances from the tear film and the aqueous humor required for metabolism must be introduced into the cornea by diffusion , since it is vascular. Likewise, the metabolic end products must be removed from the cornea by diffusion. Only the peripheral loop network as the peripheral vascular system in the limbus area is able to directly supply the periphery of the cornea with glucose and oxygen. Furthermore, the substances only get into the cornea by diffusion. In the event of any damage to the peripheral loop network and its complete failure to participate in the nutritional involvement of the cornea, the cornea does not become inoperative. It is believed that the contribution to the nutrition of the cornea is extremely small. The tear fluid supplies the largest proportion of oxygen, whereby it reaches the tear film from the atmosphere when the lids are open and diffuses from the vessels of the peripheral loop network and the conjunctiva into the tear film when the lids are closed. While there is very little glucose in the tear film (about 0.2 µmol / g water), there is little dissolved oxygen in the aqueous humor. This is just enough to supply the rearmost area of the cornea. On the other hand, the aqueous humor contains the largest proportion of glucose (about 6.5 µmol / g water). For the cornea, the breakdown of glucose is of crucial importance for the energy supply. The degradation takes place with the participation of numerous enzymes in three ways. One path runs in the absence of oxygen, i.e. anaerobic , two paths require the presence of oxygen, they are aerobic :
- Without oxygen, glucose is broken down by means of anaerobic glycolysis . The process is also called the Embden-Meyerhof cycle . This process leads in several stages via pyruvic acid to lactate or lactic acid. The lactic acid is then removed via the aqueous humor. In the event of a glucose deficiency, the glycogen stored in the epithelium is used . It is estimated that around 55% of the glucose available in the cornea is broken down in this way. However, only 2 mol of high-energy ATP are produced per mole of glucose . The energy yield is therefore relatively low.
- The hexose monophosphate route provides different amounts of energy in the yield, which is stored in the form of ATP. With one mole of high-energy ATP per mole of glucose, the hexose monophosphate route is probably the least productive, but around 35% of all glucose is converted via it.
- In the presence of oxygen, the lactate produced, which is produced via aerobic glycolysis, is completely converted into carbon dioxide and water. This process is known as the citric acid cycle . During the aerobic breakdown of glucose (citric acid cycle), 36 moles of ATP are produced per mole of glucose. However, only about 15% of the metabolized glucose takes this route.
It can therefore be seen that the oxygen supply is decisive for energy use. In the event of a lack of oxygen, the glucose is only partially broken down into lactate. This then accumulates in the cornea and inhibits or interrupts the conversion into water and carbon dioxide. This leads to swelling of the cornea, a disruption of the regular arrangement of the fibrils in the stroma and ultimately a clouding of the cornea. Less tear fluid is formed during the night and less oxygen can be absorbed by the cornea through the closed eyelids. This fact explains that the symptoms of many corneal diseases are more pronounced in the morning than in the evening. The clouding caused by corneal swelling is also considered an "uncertain sign of death " that is observed around 24 hours after the endothelial cell function has lost.
Innervation
The cornea is innervated by sensitive nerve branches of the ophthalmic nerve that are not myelinated in the cornea. About 70 to 80 nerve trunks radiate into the cornea. The epithelial axons that are not accompanied by Schwann cells are located parallel to the basement membrane in an indentation of the basal plasmalemma of the basal cells. Most axons end here. However, some nerves extend further into the epithelium almost to the surface. Interestingly, the fewer nerve fibers in the stroma also respond to external stimuli, like the nerves in the epithelium. Thus, the nerves in the stroma are able to replace the protective function of the nerves in the epithelium when it is lost. Since there is a symbiosis between the nerves and the corneal epithelium, epithelial loads or trauma cause changes in the corneal neurology. Damage to the nerves triggers an epithelial response known as neuroparalytical keratitis . With this type of keratitis, the affected person does not notice the lack of moisture in their eyes due to the lack of sensitivity of the nerves. First superficial lesions are formed, followed by larger epithelial defects. Corneal ulcers can then form as a result of bacterial superinfections . Any damage to the nerves carries an increased risk because they act as a vital warning system for the cornea. Therefore, a reduction in the sensitivity of the cornea by wearing contact lenses is an undesirable side effect.
The innervation is a prerequisite for the corneal reflex , the involuntary closing of the eyelids with increased production of tear fluid, after mechanical corneal irritation . The corneal nerves also release growth factors that, like an intact tear film, are essential for the regular renewal of the epithelial layer.
Investigation methods
- The examination by the ophthalmologist or master optician is usually done with a slit lamp microscope . The slit of light projected onto the cornea creates an optical section through the cornea, which can be viewed with different magnification levels (6–40 ×, mostly 16 ×).
- The endothelial cell layer can be viewed in isolation with a mirror microscope .
- The corneal topography can be measured with a topometer (also known as a “video keratograph” or “topography device”) .
- The corneal curvature radii are measured in keratometry using an ophthalmometer .
- An esthesiometer measures the corneal sensitivity.
- A pachymeter measures the corneal thickness.
- Tear production can be measured using the Schirmer test .
- The tear-open time (break-up time) measures the quality of the tear film when fluorescein is given and is measured on the slit lamp .
- The Seidel test is also carried out on the slit lamp with the addition of fluorescein .
- The intraocular pressure is measured with the tonometer . These are used as contact and non-contact tonometers, the gold mantonometer (contact tonometer) being the most accurate.
- The Heidelberg Retina Tomograph creates detailed images of the cell tissue at different depths of the cornea.
Diseases and Treatment Options
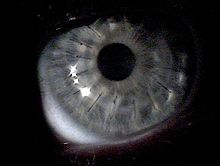
In many patients, ametropia can be corrected within certain limits by changing the corneal refractive power using refractive surgery , for example LASIK or photorefractive keratectomy .
Diseases can be divided into degenerations (acquired), dystrophies (inherited, see corneal dystrophy ) and inflammation (acquired, e.g. herpetic keratitis , acanthamoeic keratitis , corneal ulcer ). In appropriately indicated cases, a transplant ( keratoplasty ) can replace a diseased cornea.
A deficiency in vitamin A can lead to softening of the cornea, keratomalacia .
Foreign body injuries of varying degrees are also common .
In keratoconus, the most common curvature anomaly of the cornea, a cone-shaped protrusion occurs as a result of thinning. In Fuchs endothelial dystrophy , the destruction of the endothelial cells leads to the swelling of the cornea. A Sjogren's syndrome , however leads to dehydration.
Further corneal deformities are descemetoceles and staphylomas of various causes.
A number of infections can also affect the cornea . The keratitis occurs in corneal injury (or immunodeficiency ) by bacteria ( pneumococci , Pseudomonas , Moraxella ), viruses ( herpes simplex virus , varicella zoster virus ) or fungi ( Candida , Aspergillus ).
In some cases of corneal lesions , monocular diplopia may occur.
In congenital syndromes there may be an enlargement of the cornea, a megalocornea , e.g. B. Neuhauser syndrome .
literature
- Theodor Axenfeld (founder), Hans Pau (ed.): Textbook and atlas of ophthalmology. With the collaboration of Rudolf Sachsenweger and others 12th, completely revised edition. Gustav Fischer, Stuttgart et al. 1980, ISBN 3-437-00255-4 .
- Albert J. Augustin: Ophthalmology. 3rd, completely revised and expanded edition. Springer, Berlin et al. 2007, ISBN 978-3-540-30454-8 .
- Pschyrembel clinical dictionary. With clinical syndromes and nouns anatomica. = Clinical Dictionary. Edited by the publisher's dictionary editor under the direction of Christoph Zink. 256th, revised edition. de Gruyter, Berlin et al. 1990, ISBN 3-11-010881-X .
Web links
Individual evidence
- ↑ Harminder S. Dua, Lana A. Faraj, Dalia Said G., Trevor Gray, James Lowe: Human Corneal Anatomy Redefined: A Novel Pre-Descemet's Layer (Dua's layer). In: Ophthalmology. May 2013, ISSN 1549-4713 , (electronic publication before printing), PMID 23714320 , doi: 10.1016 / j.ophtha.2013.01.018 , abstract .
- ↑ UPI.com - Scientists discover new layer of human cornea
- ↑ Harminder S. Dua, Lana A. Faraj, Dalia Said G., Trevor Gray, James Lowe: Human Corneal Anatomy Redefined: A Novel Pre-Descemet's Layer (Dua's layer). In: Ophthalmology. May 2013, ISSN 1549-4713 , (electronic publication before printing), PMID 23714320 , doi: 10.1016 / j.ophtha.2013.01.018 , abstract .
- ^ Peter Westphal, Johannes-Maria Kaltenbach, and Kai Wicker, “Corneal birefringence measured by spectrally resolved Mueller matrix ellipsometry and implications for non-invasive glucose monitoring,” Biomed. Opt. Express 7, 1160-1174 (2016) [1] .
- ↑ It is estimated that around 65% of the glucose available in the cornea is broken down via glycolysis. Starting from this, about 85% are degraded via the anaerobic route (Embden-Meyerhof cycle).