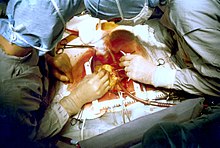
Coronary artery bypass
The coronary artery bypass is a blood vessel bridge that is intended to ensure blood flow to the downstream vascular segment by bypassing a narrowing or occlusion of a coronary artery .
history
The first coronary artery bypass surgery was performed on May 2, 1960 at Albert Einstein College of Medicine - Bronx Municipal Hospital Center , USA , by a team led by Robert Goetz and Michael Rohman and with the help of Jordan Haller and Ronald Dee.
Today arteries or veins are used to create the bypass . Since in the past only veins were used, the term aorto-coronary vein bypass (ACVB) was originally established in the German-speaking area . Nowadays, the English abbreviation CABG for coronary artery bypass graft is also in use.
execution
The standard access is by opening the chest through a median sternotomy , whereby no muscles have to be severed and an optimal representation of the heart is ensured. The rate of local complications is 0.4%, mainly wound healing disorders and wound infections. Rarely minimally invasive access paths ( minimally invasive direct coronary artery bypass , MIDCAB) or the "total endoscopic coronary artery bypass" ( totally endoscopic coronary artery bypass used TECAB).
After clamping off the ascending aorta and using a heart-lung machine , the heart is perfused with a cold, potassium- rich cardioplegic solution in order to induce the cardiac arrest that is necessary for one to two hours . The operation is rarely performed on the beating heart without a heart- lung machine , which is intended to reduce the frequency of postoperative stroke regardless of the patient's surgical risk, but is not a standard procedure.
The most difficult part is suturing the bypass end-to-side by hand below the clogged or blocked area on the coronary artery, usually with the help of magnifying glasses. The bypass is then sewn end-to-side via an aortotomy to the ascending aorta near the heart, except when using the left internal thoracic artery , the aortic branch of which is left.
The operation takes an average of three to four hours, followed by a five to seven day hospital stay (in the US), and full recovery takes six to twelve weeks.
Arterial bypass

In general, the left mammary artery is ( internal thoracic artery , engl. Left internal mammary artery LIMA) due to the spatial proximity to the supply of the left anterior descending artery (LAD engl. Left anterior descending artery ) were used. The advantage is, on the one hand, that the vascular outlet is preserved and only one side of the bypass has to be anastomized , and on the other hand, the longer service life of this bypass. The reason for the longer lifespan is not only the natural discharge of the vessel (only one anastomosis) but also the differences in the wall structure of arteries and veins.
In rare cases, especially in the case of second operations, the ( radial artery ), the internal thoracic artery on the opposite side or a gastric gastric artery can be used. The use of these arteries as bypasses is considered to be at least more promising than venous bypass, but it has not been a standard procedure to date and must be weighed up on a case-by-case basis.
Venous bypass
For a vein bypass one usually uses one of the veins of the leg ( vena saphena magna ), which runs from the inside of the ankle to the groin. Like the radial artery bypass, these are sutured to the ascending aorta and then connected to the diseased vessel. A so-called sequential bypass is also rarely used, in which a vein is first anastomosed with a vessel and then additionally, for example, with a side branch.
Common locations for venous bypass are the right coronary artery (RCA) and the circumflex branch (RCX).
Risks and Complications
According to data from the USA , the risk of dying during or as a result of the operation is around 2%. Stroke occurs in around 1–2% of patients . Predictors that increase the risk of stroke across the total patient population are old age, diabetes, past strokes and calcification of the aorta. Complications of the closure of the sternotomy wound, such as infections, are estimated at around 0.4%. Renal failure requiring permanent dialysis remains in around four percent of patients . Patients with pre-existing renal insufficiency are particularly at risk. This complication is less common in patients who have had a beating heart.
Another complication is postcardiotomy syndrome, an inflammatory reaction of the heart that is similar to Dressler's syndrome . One attempt to reduce the damage to the heart from ischemia during surgery is to precondition the heart. However, this is not clinical practice.
Coronary artery bypass or PTCA
There is a controversial discussion in professional circles whether the treatment of coronary artery disease with a coronary bypass is preferable to catheter-assisted percutaneous transluminal coronary angioplasty (PTCA). The current guidelines of the European Cardiological Society on revascularization recommend that patients with a low surgical risk and one or two affected coronary arteries without involvement of the left main trunk should be treated with PTCA. For all other patients, a higher-grade recommendation for surgical treatment with a coronary artery bypass applies.
Individual evidence
- ^ R. Dee: Who assisted whom? In: Tex Heart Inst J . tape 30 , no. 1 . Texas Heart Institute, Houston 2003, p. 90 , PMID 12638685 , PMC 152850 (free full text).
- ↑ JD Haller, AS Olearchyk: Cardiology's 10 greatest discoveries . In: Tex Heart Inst J . tape 29 , no. 4 . Texas Heart Institute, Houston 2002, p. 342-344 , PMID 12484626 , PMC 140304 (free full text).
- ↑ A. Haverich, G. Ziemer: Heart surgery: The interventions on the heart and on the vessels near the heart. 3. Edition. Springer Verlag, Berlin 2010.
- ↑ J. Afilalo: Off-pump vs. on-pump coronary artery bypass surgery: an updated meta-analysis and meta-regression of randomized trials. In: Eur Heart J . 2011. PMID 21987177
- ^ A b c John H. Alexander, Peter K. Smith: Coronary-Artery Bypass Grafting. In: New England Journal of Medicine . Volume 374, Issue 20, May 19, 2016, pp. 1954–1964, doi: 10.1056 / NEJMra1406944 - extensive review article.
- ↑ J. Bucerius, JF Gummert, T. Walther, DV Schmitt, N. Doll et al .: On-pump versus off-pump coronary artery bypass grafting: impact on postoperative renal failure requiring renal replacement therapy. In: Ann Thorac Surg. 77 (4), Apr 2004, pp. 1250-1256. PMID 15063246
- ↑ Database entries in Pubmed for the search query "CABG" (English for "coronary artery bypass") and "PCI" (English for " PTCA ")
- ↑ Wijns include: Guidelines on myocardial revascularization. In: European Heart Journal . 31, 2010, pp. 2501-2555.