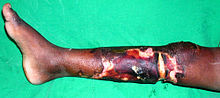
necrosis
| Classification according to ICD-10 | |
|---|---|
| R02 | Gangrene, not elsewhere classified |
| ICD-10 online (WHO version 2019) | |
| Parent |
| Cell death |
| Gene Ontology |
|---|
| QuickGO |
Under a necrosis (also necrobiosis ) ( ancient Greek νέκρωσις nékrosis "killing", also "the death of individual limbs", to νεκρόω nekróō "I kill") is understood in biology and medicine the dying or death of single or multiple cells . The necrosis is pathological - that is, the process is pathological and is triggered by damaging influences on the cell: nutrient and oxygen deficiency, toxins, radioactivity and others. As a result, the cells in the tissue die and usually lead to an inflammatory reaction . Depending on the type of tissue and extent of damage, the necrosis heals completely through regrowth of surviving cells, or the dead tissue is replaced by a connective tissue scar (example: myocardium after a heart attack - with corresponding functional restrictions).
Apoptosis must be differentiated from necrosis : It describes the "normal" ( physiological ) and controlled death of individual cells in the sense of the entire organism.
Necrosis is observed not only in humans and animals, but also in plants.
Forms of necrosis
Coagulation necrosis
This form of necrosis occurs when protein-rich tissues, such as muscles, die. A prime example is the heart muscles after a heart attack. First, the cells swell and become acidic. This leads to the precipitation and "coagulation" of the proteins and to increased eosinophilia of the cytoplasm. The histological tissue drawing becomes more indistinct and the cell nucleus dissolves in several steps: Initially, the nucleus shrinks ( pycnosis ) and then the nucleus breaks ( karyorrhexis ). Ultimately, the nucleus loses its chromatin and fades ( karyolysis ). Macroscopically (with the naked eye), the necrotic tissue appears clay-yellow and dry (after six hours at the earliest).
Inflammatory substances are released from the destroyed cells, so that granulocytes are attracted. These migrate into the tissue and, via the release of proteases, lead to the dissolution of the necrotic tissue. Cell and tissue residues are phagocytosed by macrophages . Macroscopically, there is a red border. However, the necrotic area loses its strength in the course of the process and can tear. For example, the heart wall can rupture after an extensive infarct. At the end there is the scarred healing of the tissue.
Colliquational necrosis
It is typical for tissues with a high percentage of fat and a low percentage of protein, for example in the brain with insufficient oxygen supply , or for tissues with a high percentage of proteases such as the pancreas . Chemical burns from the action of lye or abscess formation also lead to colliquation necrosis. The proteases of the body's own immune cells are decisive for abscesses. In contrast to coagulation necrosis, after initial cell swelling, the tissue liquefies ( colliquation ) and then an inflammatory reaction (except in the nervous system). Macroscopically, the tissue appears mushy, greasy and softened.
Special forms
In tuberculosis , the peculiarities of the triggering bacteria cause a cheesy necrosis (also known as cheese formation ). Gangrene is a special form of necrosis that is black and looks like it has been burned. The gangrene is dry ( dry gangrene ), unless it is attacked by putrefactive bacteria and becomes inflamed ( wet gangrene ). When fat necrosis is the death of fat cells, for example, a calcified necrosis in the adipose tissue around the pancreas around. It arises traumatically or enzymatically as a result of lipases released from the pancreas in the context of pancreatitis . Other special forms are gummatous necrosis , which occurs in syphilis , and fibrinoid necrosis , which is typical of rheumatoid arthritis , polyarthritis nodosa or peptic gastric ulcers .
Under a Panzernekrose refers absterbendes tanks tissue in turtles , for example by wet or fungi.
So-called phosphorus necrosis occurred as an occupational disease among matchmakers in the 19th century .
In rare cases, necrosis occurs as an adverse drug reaction. Sub-therapeutic concentrations of antibiotics of the fluoroquinolone group can lead to necrosis of adult chondrocytes in healthy adult human cartilage . Histologically, necrosis has also been documented in connection with fluoroquinolone-related tendon and kidney damage. Necrosis of hepatocytes of the liver can with poisoning by paracetamol be associated. In 2011, about half of all acute liver failure cases in the US and UK were attributed to acetaminophen. Necroses are caused by reactive metabolites and the subsequent oxidative stress, the loss of the mitochondrial membrane potential and the loss of the ability of the mitochondria to synthesize ATP. Likewise, the broad spectrum anti-epileptic valproic acid can cause fatal liver dysfunction in which extensive confluent lytic necrosis of liver acini has been observed. Liver necrosis has also been documented with diclofenac , methyldopa , and halothane .
See also
- Vasculopathy
- mummification
- Burn (medicine)
- Frostbite
- atrophy
- Necrotizing fasciitis
- Infarct
- Chlorosis
Web links
Individual evidence
- ^ Matthias Krams et al .: Short textbook pathology , 2nd edition. Georg Thieme Verlag, Stuttgart 2013, ISBN 978-3-13-143252-0 , pp. 17–31.
- ↑ Ursus-Nikolaus Riede and Martin Werner (eds.): General and Special Pathology , 2nd edition. Springer Verlag, Berlin - Heidelberg, 2017, ISBN 978-3-662-48725-9 , pp. 55f.
- ^ A b c Matthias Krams et al .: Short textbook Pathology , 2nd edition. Georg Thieme Verlag, Stuttgart 2013, ISBN 978-3-13-143252-0 , p. 31
- ^ A b Matthias Krams et al .: Short textbook pathology , 2nd edition. Georg Thieme Verlag, Stuttgart 2013, ISBN 978-3-13-143252-0 , p. 30
- ↑ a b Ursus-Nikolaus Riede and Martin Werner (eds.): General and Special Pathology , 2nd edition. Springer Verlag, Berlin - Heidelberg, 2017, ISBN 978-3-662-48725-9 , pp. 56f.
- ↑ a b tissue death (PDF) pp. 9–13
- ↑ Ursus-Nikolaus Riede and Martin Werner (eds.): General and Special Pathology , 2nd edition. Springer Verlag, Berlin - Heidelberg, 2017, ISBN 978-3-662-48725-9 , p. 57f.
- ^ P. Kölle: Panzernekrosen . In: Die Schildkröte - Heimtier und Patient , Georg Thieme Verlag, Stuttgart 2008, ISBN 978-3-8304-1066-9 , pp. 157-160. Available at: thieme.de (last accessed on October 26, 2017)
- ↑ Phosphorous necrosis
- ↑ On the rejection of compensation for phosphorus necrosis in the statutory accident insurance in the 19th century, cf. Collection of sources on the history of German social policy from 1867 to 1914 , Section II: From the Imperial Social Message to the February decrees of Wilhelm II (1881–1890), Volume 2, Part 2: The expansion legislation and the practice of accident insurance, edited by Wolfgang Ayaß , Darmstadt 2001, No. 306.
- ↑ M Menschik, J Neumüller, CW Steiner, L Erlacher, M Köller: Effects of ciprofloxacin and ofloxacin on adult human cartilage in vitro. In: Antimicrobial Agents and Chemotherapy . tape 41 , no. November 11 , 1997, ISSN 0066-4804 , pp. 2562-2565 , PMID 9371369 , PMC 164164 (free full text).
- ^ W. Petersen, H. Laprell: The "insidious" rupture of the achilles tendon after ciprofloxacin induced tendinopathy. A case report . In: The trauma surgeon . tape 101 , no. 9 , September 1, 1998, pp. 731-734 , doi : 10.1007 / s001130050330 .
- Jump up ↑ Jc Le Huec, T. Schaeverbeke, D. Chauveaux, J. Rivel, J. Dehais: Epicondylitis after treatment with fluoroquinolone antibiotics . In: The Journal of Bone and Joint Surgery. British volume . 77-B, no. 2 , March 1, 1995, p. 293-295 , doi : 10.1302 / 0301-620x.77b2.7706350 .
- ↑ AJ Dichiara, M. Atkinson, Z. Goodman, KE Sherman: Ciprofloxacin-induced acute cholestatic liver injury and associated renal failure. Case report and review . In: Minerva Gastroenterologica E Dietologica . tape 54 , no. 3 , September 2008, p. 307-315 , PMID 18614979 .
- ^ Nada N. Al-Shawi, Possible Histological Changes Induced by Therapeutic Doses of Ciprofloxacin in Liver and Kidney of Juvenile Rats . In: Pharmacologia . tape 3 , no. 9 , p. 477-480 , doi : 10.5567 / pharmacologia.2012.477.480 .
- ^ Jack A. Hinson, corresponding author Dean W. Roberts, Laura P. James: Mechanisms of Acetaminophen-Induced Liver Necrosis . January 2011, doi : 10.1007 / 978-3-642-00663-0_12 , PMC 2836803 (free full text).
- ↑ Tough W, Rengeling M, G Rühl, Hackenberg K .: Acute liver necrosis Caused by valproate . Ed .: Dtsch Med Wochenschr. June 1985, doi : 10.1055 / s-2008-1068939 , PMID 3922731 .
- ↑ Grit Barthel: Hepatotoxicity of valproic acid in isolated rat hepatocytes: Influence of prooxidants and starvation . Ed .: Federal Institute for Consumer Health Protection and Veterinary Medicine. Berlin 1997 ( gwdg.de [PDF]).
- ↑ Nilesh Mehta, Lisa Anne Ozick and Emmanuel Gbadehan: Drug-Induced Hepatotoxicity. In: medscape.com. MedScape, December 8, 2016, accessed October 12, 2018 .