Asthma
| Asthma | |
|---|---|
| Specialty | Pulmonology, immunology |
Asthma is a chronic condition involving the respiratory system in which the airways occasionally constrict, become inflamed, and are lined with excessive amounts of mucus, often in response to one or more triggers.[1] These episodes may be triggered by such things as exposure to an environmental stimulant such as an allergen, environmental tobacco smoke, cold or warm air, perfume, pet dander, moist air, exercise or exertion, or emotional stress. In children, the most common triggers are viral illnesses such as those that cause the common cold.[2] This airway narrowing causes symptoms such as wheezing, shortness of breath, chest tightness, and coughing. The airway constriction responds to bronchodilators. Between episodes, most patients feel well but can have mild symptoms and they may remain short of breath after exercise for longer periods of time than the unaffected individual. The symptoms of asthma, which can range from mild to life threatening, can usually be controlled with a combination of drugs and environmental changes.
Public attention in the developed world has recently focused on asthma because of its rapidly increasing prevalence, affecting up to one in four urban children.[3]
Signs and symptoms
In some individuals asthma is characterized by chronic respiratory impairment. In others it is an intermittent illness marked by episodic symptoms that may result from a number of triggering events, including upper respiratory infection, stress, airborne allergens, air pollutants (such as smoke or traffic fumes), or exercise. Some or all of the following symptoms may be present in those with asthma: dyspnea, wheezing, stridor, coughing, an inability for physical exertion. Some asthmatics who have severe shortness of breath and tightening of the lungs never wheeze or have stridor and their symptoms may be confused with a COPD-type disease.
An acute exacerbation of asthma is commonly referred to as an asthma attack. The clinical hallmarks of an attack are shortness of breath (dyspnea) and either wheezing or stridor.[4] Although the former is "often regarded as the sine qua non of asthma",[4] some patients present primarily with coughing, and in the late stages of an attack, air motion may be so impaired that no wheezing may be heard. When present the cough may sometimes produce clear sputum. The onset may be sudden, with a sense of constriction in the chest, breathing becomes difficult, and wheezing occurs (primarily upon expiration, but can be in both respiratory phases).
Signs of an asthmatic episode include wheezing, prolonged expiration, a rapid heart rate (tachycardia), rhonchous lung sounds (audible through a stethoscope), the presence of a paradoxical pulse (a pulse that is weaker during inhalation and stronger during exhalation), and over-inflation of the chest. During a serious asthma attack, the accessory muscles of respiration (sternocleidomastoid and scalene muscles of the neck) may be used, shown as in-drawing of tissues between the ribs and above the sternum and clavicles.
During very severe attacks, an asthma sufferer can turn blue from lack of oxygen, and can experience chest pain or even loss of consciousness. Just before loss of consciousness, there is a chance that the patient will feel numbness in the limbs and palms may start to sweat. The person's feet may become icy cold. Severe asthma attacks, which may not be responsive to standard treatments (status asthmaticus), are life-threatening and may lead to respiratory arrest and death. Despite the severity of symptoms during an asthmatic episode, between attacks an asthmatic may show few or even no signs of the disease.[5]
Cause
Asthma is caused by a complex interaction of environmental and genetic factors that researchers do not fully understand yet.[6] These factors can also influence how severe a person’s asthma is and how well they respond to medication.[7] As with other complex diseases, many environmental and genetic factors have been suggested as causes of asthma, but not all of them have been replicated. In addition, as researchers detangle the complex causes of asthma, it is becoming more evident that certain environmental and genetic factors may only affect asthma when combined.
Environmental
Many environmental risk factors have been associated with asthma, but a few stand out as well-replicated or that have a meta-analysis of several studies to support their direct association:
- Poor air quality, from traffic pollution or high ozone levels, has been repeatedly associated with increased asthma morbidity and has a suggested association with asthma development that needs further research.[8][9]
- Environmental tobacco smoke, especially maternal cigarette smoking, is associated with high risk of asthma prevalence and asthma morbidity, wheeze, and respiratory infections.[8]
- Viral respiratory infections at an early age, along with siblings and day care exposure, may be protective against asthma, although there have been controversial results, and this protection may depend on genetic context.[8][10][11]
- Antibiotic use early in life has been linked to development of asthma in several examples; it is thought that antibiotics make one susceptible to development of asthma because they modify gut flora, and thus the immune system (as described by the hygiene hypothesis).[12]
- Caesarean sections have been associated with asthma when compared with vaginal birth; a meta-analysis found a 20% increase in asthma prevalence in children delivered by Caesarean section compared to those who were not. It was proposed that this is due to modified bacterial exposure during Caesarean section compared with vaginal birth, which modifies the immune system (as described by the hygiene hypothesis).[13]
- Psychological stress on the part of a child's caregiver has been associated with asthma, and is an area of active research. Stress can modify behaviors that affect asthma, like smoking, but research suggests that stress has other effects as well. There is growing evidence that stress may influence asthma and other diseases by influencing the immune system.[8]
The hygiene hypothesis is a theory about the cause of asthma and other allergic disease, and is supported by epidemiologic data for asthma. For example, asthma prevalence has been increasing in developed countries along with increased use of antibiotics, c-sections, and cleaning products.[12][13][14] All of these things may negatively affect exposure to beneficial bacteria and other immune system modulators that are important during development, and thus may cause increased risk for asthma and allergy.
Genetic
Over 100 genes have been associated with asthma in at least one genetic association study.[15] However, as with all association studies, replication is important before genetic variation (such as a single nucleotide polymorphism, or SNP) in a certain gene is thought to influence asthma. Through the end of 2005, 25 genes had been associated with asthma in six or more separate populations:[15]
Template:Multicol-break
Template:Multicol-break
Template:Multicol-break
Template:Multicol-break
Template:Multicol-end
Many of these genes are related to the immune system or to modulating inflammation. However, even among this list of highly replicated genes associated with asthma, the results have not been consistent among all of the populations that have been tested.[15] This indicates that these genes are not associated with asthma under every condition, and that researchers need to do further investigation to figure out the complex interactions that cause asthma.
Gene-environment Interactions
Research suggests that some genetic variants may only cause asthma when they are combined with specific environmental exposures, and otherwise may not be risk factors for asthma.[6]
The CD14 SNP C-159T and endotoxin exposure are a well-replicated example of a gene-environment interaction that is associated with asthma. Endotoxin exposure varies from person to person and can come from several environmental sources, including environmental tobacco smoke, dogs, and farms. Researchers have found that risk for asthma changes based on a person’s genotype at CD14 C-159T and level of endotoxin exposure.[16]
| Endotoxin levels | CC genotype | TT genotype |
|---|---|---|
| High exposure | Low risk | High risk |
| Low exposure | High risk | Low risk |
Pathophysiology
In asthma, constriction of the airways occurs due to bronchoconstriction and bronchial inflammation. Bronchoconstriction is the narrowing of the airways in the lungs due to the tightening of surrounding smooth muscle. Bronchial inflammation also causes narrowing due to oedema and swelling caused by an immune response to allergens.
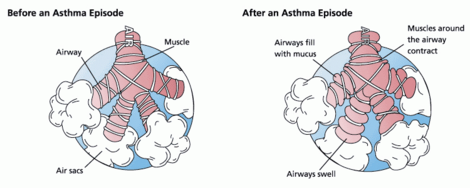
Bronchoconstriction
During an asthma episode, inflamed airways react to environmental triggers such as smoke, dust, or pollen. The airways narrow and produce excess mucus, making it difficult to breathe. In essence, asthma is the result of an immune response in the bronchial airways.[17]
The airways of asthmatics are "hypersensitive" to certain triggers, also known as stimuli (see below). In response to exposure to these triggers, the bronchi (large airways) contract into spasm (an "asthma attack"). Inflammation soon follows, leading to a further narrowing of the airways and excessive mucus production, which leads to coughing and other breathing difficulties.
The normal calibre of the bronchus is maintained by a balanced functioning of these systems, which both operate reflexively. The parasympathetic reflex loop consists of afferent nerve endings which originate under the inner lining of the bronchus. Whenever these afferent nerve endings are stimulated (for example, by dust, cold air or fumes) impulses travel to the brain-stem vagal centre, then down the vagal afferent pathway to again reach the bronchus. Acetylcholine is released from the afferent nerve endings. This acetylcholine results in the excessive formation of cyclic Guanine Mono phosphate (GMP). This initiates bronchoconstriction.
Bronchial inflammation
The mechanisms behind allergic asthma—i.e., asthma resulting from an immune response to inhaled allergens—are the best understood of the causal factors. In both asthmatics and non-asthmatics, inhaled allergens that find their way to the inner airways are ingested by a type of cell known as antigen presenting cells, or APCs. APCs then "present" pieces of the allergen to other immune system cells. In most people, these other immune cells (TH0 cells) "check" and usually ignore the allergen molecules. In asthmatics, however, these cells transform into a different type of cell (TH2), for reasons that are not well understood. The resultant TH2 cells activate an important arm of the immune system, known as the humoral immune system. The humoral immune system produces antibodies against the inhaled allergen. Later, when an asthmatic inhales the same allergen, these antibodies "recognize" it and activate a humoral response. Inflammation results: chemicals are produced that cause the airways to constrict and release more mucus, and the cell-mediated arm of the immune system is activated. The inflammatory response is responsible for the clinical manifestations of an asthma attack.
Stimuli
- Allergens from nature, typically inhaled, which include waste from common household pests, such as the house dust mite and cockroach, grass pollen, mould spores, and pet epithelial cells; [citation needed]
- Indoor air pollution from volatile organic compounds, including perfumes and perfumed products. Examples include soap, dishwashing liquid, laundry detergent, fabric softener, paper tissues, paper towels, toilet paper, shampoo, hairspray, hair gel, cosmetics, facial cream, sun cream, deodorant, cologne, shaving cream, aftershave lotion, air freshener and candles, and products such as oil-based paint.[citation needed]
- Medications, including aspirin,[18] β-adrenergic antagonists (beta blockers), and penicillin.[citation needed]
- Food allergies such as milk, peanuts, and eggs. However, asthma is rarely the only symptom, and not all people with food or other allergies have asthma. [citation needed]
- Use of fossil fuel related allergenic air pollution, such as ozone, smog, summer smog, nitrogen dioxide, and sulfur dioxide, which is thought to be one of the major reasons for the high prevalence of asthma in urban areas.[citation needed]
- Various industrial compounds and other chemicals, notably sulfites; chlorinated swimming pools generate chloramines—monochloramine (NH2Cl), dichloramine (NHCl2) and trichloramine (NCl3)—in the air around them, which are known to induce asthma.[19]
- Early childhood infections, especially viral respiratory infections. However, persons of any age can have asthma triggered by colds and other respiratory infections even though their normal stimuli might be from another category (e.g. pollen) and absent at the time of infection. In many cases, significant asthma may not even occur until the respiratory infection is in its waning stage, and the person is seemingly improving. Eighty percent of asthma attacks in adults and 60% in children are caused by respiratory viruses.[citation needed]
- Exercise or intense use of respiratory system. The effects of which differ somewhat from those of the other triggers, since they are brief. It is known that exercising regularly actually helps to cure asthma. [citation needed]
- Hormonal changes in adolescent girls and adult women associated with their menstrual cycle can lead to a worsening of asthma. Some women also experience a worsening of their asthma during pregnancy whereas others find no significant changes, and in other women their asthma improves during their pregnancy.[citation needed]
- Emotional stress which is poorly understood as a trigger.[citation needed] Emotional stress can affect breathing temporarily, however unlike something such as heart problems, it is unclear if it has any long-term effect.
- Cold weather can make it harder for asthmatics to breathe.[20] Whether high altitude helps or worsens asthma is debatable and may vary from person to person.[21]
Pathogenesis
The fundamental problem in asthma appears to be immunological: young children in the early stages of asthma show signs of excessive inflammation in their airways. Epidemiological findings give clues as to the pathogenesis: the incidence of asthma seems to be increasing worldwide, and asthma is now very much more common in affluent countries.
In 1968 Andor Szentivanyi first described The Beta Adrenergic Theory of Asthma; in which blockage of the Beta-2 receptors of pulmonary smooth muscle cells causes asthma.[22] Szentivanyi's Beta Adrenergic Theory is a citation classic[23] and has been cited more times than any other article in the history of the Journal of Allergy.
In 1995 Szentivanyi and colleagues demonstrated that IgE blocks beta-2 receptors.[24] Since overproduction of IgE is central to all atopic diseases, this was a watershed moment in the world of allergy.[25]
The Beta-Adrenergic Theory has been cited in the scholarship of such noted investigators as Richard F. Lockey (former President of the American Academy of Allergy, Asthma, and Immunology),[26] Charles Reed (Chief of Allergy at Mayo Medical School),[27] and Craig Venter (Human Genome Project).[28]
John P. McGovern, President of the American Association of Allergy nominated Szentivanyi for The 1968 Nobel Prize in Medicine in recognition of The Beta Adrenergic Theory.
In 2006, Researchers at Harvard Medical School found evidence that asthma is caused by over-proliferation of a special type of natural "killer" cell.[29]
Asthma and sleep apnea
It is recognized with increasing frequency, that patients who have both obstructive sleep apnea (OSA) and bronchial asthma, often improve tremendously when the sleep apnea is diagnosed and treated.[30] CPAP is not effective in patients with nocturnal asthma only.[31]
Asthma and gastro-esophageal reflux disease
If gastro-esophageal reflux disease is present, the patient may have repetitive episodes of acid aspiration, which results in airway inflammation and "irritant-induced" asthma.[citation needed] GERD may be common in difficult-to-control asthma, but according to one study, treating it does not seem to affect the asthma.[32]
Diagnosis
Asthma is defined simply as reversible airway obstruction. Reversibility occurs either spontaneously or with treatment. The basic measurement is peak flow rates and the following diagnostic criteria are used by the British Thoracic Society:[33]
- ≥20% difference on at least three days in a week for at least two weeks;
- ≥20% improvement of peak flow following treatment, for example:
- 10 minutes of inhaled β-agonist (e.g., salbutamol);
- six week of inhaled corticosteroid (e.g., beclometasone);
- 14 days of 30mg prednisolone.
- ≥20% decrease in peak flow following exposure to a trigger (e.g., exercise).
In many cases, a physician can diagnose asthma on the basis of typical findings in a patient's clinical history and examination. Asthma is strongly suspected if a patient suffers from eczema or other allergic conditions—suggesting a general atopic constitution—or has a family history of asthma. While measurement of airway function is possible for adults, most new cases are diagnosed in children who are unable to perform such tests. Diagnosis in children is based on a careful compilation and analysis of the patient's medical history and subsequent improvement with an inhaled bronchodilator medication. In adults, diagnosis can be made with a peak flow meter (which tests airway restriction), looking at both the diurnal variation and any reversibility following inhaled bronchodilator medication.
Testing peak flow at rest (or baseline) and after exercise can be helpful, especially in young asthmatics who may experience only exercise-induced asthma. If the diagnosis is in doubt, a more formal lung function test may be conducted. Once a diagnosis of asthma is made, a patient can use peak flow meter testing to monitor the severity of the disease.
Monitoring asthma with a peak flow meter on an ongoing basis assists with self monitoring of asthma. Peak flow readings can be charted on graph paper charts together with a record of symptoms or use peak flow charting software.[34] This allows patients to track their peak flow readings and pass information back to their doctor or nurse.[35]
In the Emergency Department doctors may use a capnography which measures the amount of exhaled carbon dioxide,[36] along with pulse oximetry which shows the amount of oxygen dissolved in the blood, to determine the severity of an asthma attack as well as the response to treatment.
Differential diagnosis
Before diagnosing someone as asthmatic, alternative possibilities should be considered. A clinician taking a history should check whether the patient is using any known bronchoconstrictors (substances that cause narrowing of the airways, e.g., certain anti-inflammatory agents or beta-blockers).
Chronic obstructive pulmonary disease, which closely resembles asthma, is correlated with more exposure to cigarette smoke, an older patient, less symptom reversibility after bronchodilator administration (as measured by spirometry), and decreased likelihood of family history of atopy.
Pulmonary aspiration, whether direct due to dysphagia (swallowing disorder) or indirect (due to acid reflux), can show similar symptoms to asthma. However, with aspiration, fevers might also indicate aspiration pneumonia. Direct aspiration (dysphagia) can be diagnosed by performing a Modified Barium Swallow test and treated with feeding therapy by a qualified speech therapist. If the aspiration is indirect (from acid reflux) then treatment directed at this is indicated.
A majority of children who are asthma sufferers have an identifiable allergy trigger. Specifically, in a 2004 study, 71% had positive test results for more than 1 allergen, and 42% had positive test results for more than 3 allergens.[37]
The majority of these triggers can often be identified from the history; for instance, asthmatics with hay fever or pollen allergy will have seasonal symptoms, those with allergies to pets may experience an abatement of symptoms when away from home, and those with occupational asthma may improve during leave from work. Allergy tests can help identify avoidable symptom triggers.
After a pulmonary function test has been carried out, radiological tests, such as a chest X-ray or CT scan, may be required to exclude the possibility of other lung diseases. In some people, asthma may be triggered by gastroesophageal reflux disease, which can be treated with suitable antacids. Very occasionally, specialized tests after inhalation of methacholine — or, even less commonly, histamine — may be performed.
Asthma is categorized by the United States National Heart, Lung and Blood Institute as falling into one of four categories: intermittent, mild persistent, moderate persistent and severe persistent. The diagnosis of "severe persistent asthma" occurs when symptoms are continual with frequent exacerbations and frequent night-time symptoms, result in limited physical activity and when lung function as measured by PEV or FEV1 tests is less than 60% predicted with PEF variability greater than 30%.
Prevention
Current treatment protocols recommend prevention medications such as an inhaled corticosteroid, which helps to suppress inflammation and reduces the swelling of the lining of the airways, in anyone who has frequent (greater than twice a week) need of relievers or who has severe symptoms. If symptoms persist, additional preventive drugs are added until the asthma is controlled. With the proper use of prevention drugs, asthmatics can avoid the complications that result from overuse of relief medications.
Asthmatics sometimes stop taking their preventive medication when they feel fine and have no problems breathing. This often results in further attacks, and no long-term improvement.
Preventive agents include the following.
- Inhaled glucocorticoids are the most widely used of the prevention medications and normally come as inhaler devices (ciclesonide, beclomethasone, budesonide, flunisolide, fluticasone, mometasone, and triamcinolone).
Long-term use of corticosteroids can have many side effects including a redistribution of fat, increased appetite, blood glucose problems and weight gain. In particular high doses of steroids may cause osteoporosis. For this reasons inhaled steroids are generally used for prevention, as their smaller doses are targeted to the lungs unlike the higher doses of oral preparations. Nevertheless, patients on high doses of inhaled steroids may still require prophylactic treatment to prevent osteoporosis.
Deposition of steroids in the mouth may cause a hoarse voice or oral thrush (due to decreased immunity). This may be minimised by rinsing the mouth with water after inhaler use, as well as by using a spacer which increases the amount of drug that reaches the lungs. - Leukotriene modifiers (montelukast, zafirlukast, pranlukast, and zileuton).
- Mast cell stabilizers (cromoglicate (cromolyn), and nedocromil).
- Antimuscarinics/anticholinergics (ipratropium, oxitropium, and tiotropium), which have a mixed reliever and preventer effect. (These are rarely used in preventive treatment of asthma, except in patients who do not tolerate beta-2-agonists.)
- Methylxanthines (theophylline and aminophylline), which are sometimes considered if sufficient control cannot be achieved with inhaled glucocorticoids and long-acting β-agonists alone.
- Antihistamines, often used to treat allergic symptoms that may underlie the chronic inflammation.
- Hyposensitization, (also known as immunodesensitisation therapy) may be recommended in some cases where allergy is the suspected cause or trigger of asthma. Depending on the allergen, it can be given orally or by injection.
- Omalizumab, an IgE blocker; this can help patients with severe allergic asthma that does not respond to other drugs. However, it is expensive and must be injected.
- Methotrexate is occasionally used in some difficult-to-treat patients.
- If chronic acid indigestion (GERD) contributes to a patient's asthma, it should also be treated, because it may prolong the respiratory problem.
Trigger avoidance
As is common with respiratory disease, smoking is believed to adversely affect asthmatics in several ways, including an increased severity of symptoms, a more rapid decline of lung function, and decreased response to preventive medications.[38] Automobile emissions are considered an even more significant cause and aggravating factor. [1] Asthmatics who smoke or who live near traffic [2] typically require additional medications to help control their disease. Furthermore, exposure of both non-smokers and smokers to wood smoke, gas stove fumes and second-hand smoke is detrimental, resulting in more severe asthma, more emergency room visits, and more asthma-related hospital admissions.[39] Smoking cessation and avoidance of second-hand smoke is strongly encouraged in asthmatics.[40]
For those in whom exercise can trigger an asthma attack (exercise-induced asthma), higher levels of ventilation and cold, dry air tend to exacerbate attacks. For this reason, activities in which a patient breathes large amounts of cold air, such as skiing and running, tend to be worse for asthmatics, whereas swimming in an indoor, heated pool, with warm, humid air, is less likely to provoke a response.[4]
Air Filters
If an asthmatic lives with a smoker, use of air filter or room air cleaner is likely to be helpful. Secondhand smoke can worsen the symptoms. The same is true for those with hay fever (allergic rhino sinusitis) or COPD (emphysema or chronic bronchitis). Room air cleaners remove small particles that are in the air near the air cleaner. However, room air cleaners do not remove small allergen particles that are caused by local disturbances, such as the microscopic house dust mite feces that surround a pillow when your head hits it or you turn over in bed. There are several types of air filters available.[41]
- Mechanical air filters use a fan to force air through a special screen that traps particles such as smoke, pollens, and other airborne allergens. The high-efficiency particulate air (HEPA) filter is the best-known air filter. HEPA (which is a type of filter, not a brand name) was developed during World War II to prevent radioactive particles from escaping from laboratories.
- Electronic air filters use electrical charges to attract and deposit allergens and irritants. If the device contains collecting plates, the particles are captured within the system; otherwise, they stick to room surfaces and have to be cleared away.
- Hybrid air filters contain elements of both mechanical and electrostatic filters.
- Gas phase air filters use activated carbon granules to remove odors (volatile organic compounds or VOCs) and non-particulate pollution such as cooking gas, gases emitted from paint or building materials (such as formaldehyde), and perfume.
- Germicidal air cleaners use ultraviolet (UV) lights to kill bacteria, viruses, and molds that pass through the area with the UV light. Such UV lights can be included with other air cleaner devices, which use a fan.
- Ozone generators are devices that intentionally produce high concentrations of ozone to clean the air in a room. They are often used to decontaminate rooms after smoke exposure following a fire.
Treatment
The most effective treatment for asthma is identifying triggers, such as pets or aspirin, and limiting or eliminating exposure to them. If trigger avoidance is insufficient, medical treatment is available. Desensitization is currently the only known "cure" to the disease.[42] Other forms of treatment include relief medication, prevention medication, long-acting β2-agonists, and emergency treatment.
Medical
The specific medical treatment recommended to patients with asthma depends on the severity of their illness and the frequency of their symptoms. Specific treatments for asthma are broadly classified as relievers, preventers and emergency treatment. The Expert Panel Report 2: Guidelines for the Diagnosis and Management of Asthma (EPR-2)[40] of the U.S. National Asthma Education and Prevention Program, and the British Guideline on the Management of Asthma[43] are broadly used and supported by many doctors. On August 29, 2007 the final Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma was officially released. Bronchodilators are recommended for short-term relief in all patients. For those who experience occasional attacks, no other medication is needed. For those with mild persistent disease (more than two attacks a week), low-dose inhaled glucocorticoids or alternatively, an oral leukotriene modifier, a mast-cell stabilizer, or theophylline may be administered. For those who suffer daily attacks, a higher dose of glucocorticoid in conjunction with a long-acting inhaled β-2 agonist may be prescribed; alternatively, a leukotriene modifier or theophylline may substitute for the β-2 agonist. In severe asthmatics, oral glucocorticoids may be added to these treatments during severe attacks.
The discovery in 2006 by researchers at Harvard Medical School that asthma may be caused by over-proliferation of a special type of natural "killer" cell may ultimately lead to the development of better and more targeted drugs. Natural killer T cells seem to be resistant to the corticosteroids, one of the mainstays of current treatment.[29] Other promising avenues of current research include using cholesterol-lowering drugs (statins) and fish oil supplementation to reduce airway inflammation [44].
Pharmaceutical
Symptomatic control of episodes of wheezing and shortness of breath is generally achieved with fast-acting bronchodilators. These are typically provided in pocket-sized, metered-dose inhalers (MDIs). In young sufferers, who may have difficulty with the coordination necessary to use inhalers, or those with a poor ability to hold their breath for 10 seconds after inhaler use (generally the elderly), an asthma spacer (see top image) is used. The spacer is a plastic cylinder that mixes the medication with air in a simple tube, making it easier for patients to receive a full dose of the drug and allows for the active agent to be dispersed into smaller, more fully inhaled bits.
A nebulizer which provides a larger, continuous dose can also be used. Nebulizers work by vaporizing a dose of medication in a saline solution into a steady stream of foggy vapour, which the patient inhales continuously until the full dosage is administered. There is no clear evidence, however, that they are more effective than inhalers used with a spacer. Nebulizers may be helpful to some patients experiencing a severe attack. Such patients may not be able to inhale deeply, so regular inhalers may not deliver medication deeply into the lungs, even on repeated attempts. Since a nebulizer delivers the medication continuously, it is thought that the first few inhalations may relax the airways enough to allow the following inhalations to draw in more medication.
Relievers include:
- Short-acting, selective beta2-adrenoceptor agonists, such as salbutamol (albuterol USAN), levalbuterol, terbutaline and bitolterol.
Tremors, the major side effect, have been greatly reduced by inhaled delivery, which allows the drug to target the lungs specifically; oral and injected medications are delivered throughout the body. There may also be cardiac side effects at higher doses (due to Beta-1 agonist activity), such as elevated heart rate or blood pressure; with the advent of selective agents, these side effects have become less common. Patients must be cautioned against using these medicines too frequently, as with such use their efficacy may decline, producing desensitization resulting in an exacerbation of symptoms which may lead to refractory asthma and death. - Older, less selective adrenergic agonists, such as inhaled epinephrine and ephedrine tablets, have also been used. Cardiac side effects occur with these agents at either similar or lesser rates to albuterol.[45] [46] When used solely as a relief medication, inhaled epinephrine has been shown to be an effective agent to terminate an acute asthmatic exacerbation.[45] In emergencies, these drugs were sometimes administered by injection. Their use via injection has declined due to related adverse effects.
- Anticholinergic medications, such as ipratropium bromide may be used instead. They have no cardiac side effects and thus can be used in patients with heart disease; however, they take up to an hour to achieve their full effect and are not as powerful as the β2-adrenoreceptor agonists.
- Inhaled glucocorticoids are usually considered preventive medications; however, a randomized controlled trial has demonstrated the benefit of 250 microg beclomethasone when taken as an as-needed combination inhaler with 100 microg of albuterol.[47]
Long-acting β2-agonists

Long-acting bronchodilators (LABD) are similar in structure to short-acting selective beta2-adrenoceptor agonists, but have much longer side chains resulting in a 12-hour effect, and are used to give a smoothed symptomatic relief (used morning and night). While patients report improved symptom control, these drugs do not replace the need for routine preventers, and their slow onset means the short-acting dilators may still be required. In November 2005, the American FDA released a health advisory alerting the public to findings that show the use of long-acting β2-agonists could lead to a worsening of symptoms, and in some cases death.[48]
Currently available long-acting beta2-adrenoceptor agonists include salmeterol, formoterol, bambuterol, and sustained-release oral albuterol. Combinations of inhaled steroids and long-acting bronchodilators are becoming more widespread; the most common combination currently in use is fluticasone/salmeterol (Advair in the United States, and Seretide in the United Kingdom). Another combination is budesonide/formoterol which is commercially known as Symbicort.
A recent meta-analysis of the roles of long-acting beta-agonists may indicate a danger to asthma patients. The study, published in the Annals of Internal Medicine in 2006, found that long-acting beta-agonists increased the risk for asthma hospitalizations and asthma deaths 2- to 4-fold, compared with placebo.[49] "These agents can improve symptoms through bronchodilation at the same time as increasing underlying inflammation and bronchial hyper-responsiveness, thus worsening asthma control without any warning of increased symptoms," said Shelley Salpeter in a press release after the publication of the study. The release goes on to say that "Three common asthma inhalers containing the drugs salmeterol or formoterol may be causing four out of five US asthma-related deaths per year and should be taken off the market".[50] This assertion has drawn criticism from many asthma specialists for being inaccurate. As Dr. Hal Nelson points out in a recent letter to the Annals of Internal Medicine, "Salpeter and colleagues also assert that salmeterol may be responsible for 4000 of the 5000 asthma-related deaths that occur in the United States annually. However, when salmeterol was introduced in 1994, more than 5000 asthma-related deaths occurred per year. Since the peak of asthma deaths in 1996, salmeterol sales have increased about 5-fold, while overall asthma mortality rates have decreased by about 25%, despite a continued increase in asthma diagnoses. In fact, according to the most recent data from the National Center for Health Statistics, U.S. asthma mortality rates peaked in 1996 (with 5667 deaths) and have decreased steadily since. The last available data, from 2004, indicate that 3780 deaths occurred. Thus, the suggestion that a vast majority of asthma deaths could be attributable to LABA use is inconsistent with the facts."
Dr. Shelley Salpeter, in a letter to the Annals of Internal Medicine, responds to the comments of Dr. Nelson, "It is true that the asthma death rate increased after salmeterol was introduced, then peaked and is now starting to decline despite continued use of the long-acting beta-agonists. This trend in death rates can best be explained by examining the ratio of beta-agonist use to inhaled corticosteroids... In the recent past, inhaled corticosteroid use has increased steadily while long-acting beta-agonist use has begun to stabilize and short-acting beta-agonist use has declined... Using this estimate, we can imagine that if long-acting beta-agonists were withdrawn from the market while maintaining high inhaled corticosteroid use, the death rate in the United States could be reduced significantly..."
Emergency
When an asthma attack is unresponsive to a patient's usual medication, other treatments are available to the physician or hospital:[51]
- Oxygen to alleviate the hypoxia (but not the asthma itself) that results from extreme asthma attacks.
- Nebulized salbutamol or terbutaline (short-acting beta-2-agonists), often combined with ipratropium (an anticholinergic).
- Systemic steroids, oral or intravenous (prednisone, prednisolone, methylprednisolone, dexamethasone, or hydrocortisone). Some research has looked into an alternative inhaled route.[52]
- Other bronchodilators that are occasionally effective when the usual drugs fail:
- Intravenous salbutamol
- Nonspecific beta-agonists, injected or inhaled (epinephrine, isoetharine, isoproterenol, metaproterenol)
- Anticholinergics, IV or nebulized, with systemic effects (glycopyrrolate, atropine, ipratropium)
- Methylxanthines (theophylline, aminophylline)
- Inhalation anesthetics that have a bronchodilatory effect (isoflurane, halothane, enflurane)
- The dissociative anaesthetic ketamine, often used in endotracheal tube induction
- Magnesium sulfate, intravenous
- Intubation and mechanical ventilation, for patients in or approaching respiratory arrest.
- Heliox, a mixture of helium and oxygen, may be used in a hospital setting. It has a more laminar flow than ambient air and moves more easily through constricted airways.
Non-medical treatments
Many asthmatics, like those who suffer from other chronic disorders, use alternative treatments; surveys show that roughly 50% of asthma patients use some form of unconventional therapy.[53][54] There is little data to support the effectiveness of most of these therapies. A Cochrane systematic review of acupuncture for asthma found no evidence of efficacy.[55] A similar review of air ionisers found no evidence that they improve asthma symptoms or benefit lung function; this applied equally to positive and negative ion generators.[56] A study of "manual therapies" for asthma, including osteopathic, chiropractic, physiotherapeutic and respiratory therapeutic manoeuvres, found there is insufficient evidence to support or refute their use in treating asthma;[57] these manoeuvers include various osteopathic and chiropractic techniques to "increase movement in the rib cage and the spine to try and improve the working of the lungs and circulation"; chest tapping, shaking, vibration, and the use of "postures to help shift and cough up phlegm." One meta-analysis finds that homeopathy may have a potentially mild benefit in reducing the intensity of symptoms.[58] However, the number of patients involved in the analysis was small, and subsequent studies have not supported this finding.[59] Several small trials have suggested some benefit from various yoga practices, ranging from integrated yoga programs,[60] yogasanas, Pranayama, meditation, and kriyas, to sahaja yoga,[61] a form of 'new religious' meditation.
Treatment controversies
In November 2007 The New York Times reported a review of more than 500 studies finding that independently backed studies on inhaled corticosteroids are up to four times more likely to find adverse effects than studies paid for by drug companies.[62][63]
Prognosis
The prognosis for asthmatics is good; especially for children with mild disease. For asthmatics diagnosed during childhood, 54% will no longer carry the diagnosis after a decade. The extent of permanent lung damage in asthmatics is unclear. Airway remodelling is observed, but it is unknown whether these represent harmful or beneficial changes.[17] Although conclusions from studies are mixed, most studies show that early treatment with glucocorticoids prevents or ameliorates decline in lung function as measured by several parameters.[64] For those who continue to suffer from mild symptoms, corticosteroids can help most to live their lives with few disabilities. The mortality rate for asthma is low, with around 6000 deaths per year in a population of some 10 million patients in the United States.[4] Better control of the condition may help prevent some of these deaths.

Epidemiology
More than 6% of children in the United States have been diagnosed with asthma, a 75% increase in recent decades. The rate soars to 40% among some populations of urban children.[citation needed]
Asthma is usually diagnosed in childhood. The risk factors for asthma include:[citation needed]
- A personal or family history of asthma or atopy
- Triggers (see Pathophysiology above)
- Premature birth or low birth weight
- Viral respiratory infection in early childhood
- Maternal smoking
- Being male, for asthma in prepubertal children
- Being female, for persistence of asthma into adulthood
Current research suggests that the prevalence of childhood asthma has been increasing. According to the Centers for Disease Control and Prevention's National Health Interview Surveys, some 9% of US children below 18 years of age had asthma in 2001, compared with just 3.6% in 1980 (see figure). The World Health Organization (WHO) reports that some 8% of the Swiss population suffers from asthma today, compared with just 2% some 25–30 years ago.[65] Although asthma is more common in affluent countries, it is by no means a problem restricted to the affluent; the WHO estimate that there are between 15 and 20 million asthmatics in India. In the U.S., urban residents, Hispanics, and African Americans are affected more than the population as a whole. Globally, asthma is responsible for around 180,000 deaths annually.[65]
Population disparities
Asthma prevalence, morbidity, mortality, and drug response vary greatly across populations. There is an almost 30-fold difference in asthma prevalence between some of the countries included in the International Study of Asthma and Allergy in Childhood[3], with a trend toward more developed and westernized countries having higher asthma prevalence. Westernization can’t explain the entire difference in asthma prevalence between countries, however, and the disparities may also be affected by differences in genetic, social and environmental risk factors.[8] There are also worldwide disparities in asthma mortality, which is most common in low to middle income countries.[66]
Asthma prevalence in the US is higher than in most other countries in the world, but varies drastically between diverse US populations.[8] In the US, asthma prevalence is highest in Puerto Ricans, African Americans, Filipinos and Native Hawaiians, and lowest in Mexicans and Koreans.[67][68][69] Mortality rates follow similar trends, and response to albuterol is lower in Puerto Ricans than in African Americans or Mexicans.[70][71] As with worldwide asthma disparities, differences in asthma prevalence, mortality, and drug response in the US may be explained by differences in genetic, social and environmental risk factors.
Asthma prevalence also differs between populations of the same ethnicity who are born and live in different places.[72] US-born Mexican populations, for example, have higher asthma rates than non-US born Mexican populations that are living in the US.[73] This probably reflects differences in social and environmental risk factors associated with acculturation to the US.
Asthma prevalence and asthma deaths also differ by gender. Males are more likely to be diagnosed with asthma as children, but asthma is more likely to persist into adulthood in females. Sixty five percent more adult women than men will die from asthma. This difference may be attributable to hormonal differences, among other things. In support of this, girls who reach puberty before age 12 were found to have a later diagnosis of asthma more than twice as much as girls who reach puberty after age 12. Asthma is also the number one cause of missed days from school.
Socioeconomic factors
The incidence of asthma is highest among low-income populations (asthma deaths are most common in low to middle income countries [4]), which in the western world are disproportionately ethnic minorities[74] and are more likely to live near industrial areas. Additionally, asthma has been strongly associated with the presence of cockroaches in living quarters, which is more likely in such neighborhoods.
Asthma incidence and quality of treatment varies among different racial groups, though this may be due to correlations with income (and thus affordability of health care) and geography. For example, Black Americans are less likely to receive outpatient treatment for asthma despite having a higher prevalence of the disease. They are much more likely to have emergency room visits or hospitalization for asthma, and are three times as likely to die from an asthma attack compared to whites. The prevalence of "severe persistent" asthma is also greater in low-income communities compared with communities with better access to treatment.[75][76]
Asthma and athletics
Asthma appears to be more prevalent in athletes than in the general population. One survey of participants in the 1996 Summer Olympic Games, in Atlanta, Georgia, U.S., showed that 15% had been diagnosed with asthma, and that 10% were on asthma medication.[77] These statistics have been questioned on at least two bases. Athletes with mild asthma may be more likely to be diagnosed with the condition than non-athletes, because even subtle symptoms may interfere with their performance and lead to pursuit of a diagnosis. It has also been suggested that some professional athletes who do not suffer from asthma claim to do so in order to obtain special permits to use certain performance-enhancing drugs.[citation needed]
There appears to be a relatively high incidence of asthma in sports such as cycling, mountain biking, and long-distance running, and a relatively lower incidence in weightlifting and diving. It is unclear how much of these disparities are from the effects of training in the sport, and from self-selection of sports that may appear to minimize the triggering of asthma.[77][78]
In addition, there exists a variant of asthma called exercise-induced asthma that shares many features with allergic asthma. It may occur either independently, or concurrent with the latter. Exercise studies may be helpful in diagnosing and assessing this condition.
History
Asthma was long considered a psychosomatic disease, and
- ... during the 1930s–50s, was even known as one of the 'holy seven' psychosomatic illnesses. At that time, psychoanalytic theories described the aetiology of asthma as psychological, with treatment often primarily involving psychoanalysis and other 'talking cures'. As the asthmatic wheeze was interpreted as the child's suppressed cry for his or her mother, psychoanalysts viewed the treatment of depression as especially important for individuals with asthma.[79]
See also
- Asthma and Allergy Foundation of America
- Atopy
- Global Initiative for Asthma (GINA)
- Hopkins syndrome
- Hygiene hypothesis
- Immune response
- Occupational asthma
- Reactive airway disease
- World Asthma Day
- Vocal cord dysfunction
References
- ^ "Asthma: What Causes Asthma". Asthma and Allergy Foundation of America. Retrieved 2008-01-03.
- ^ Zhao J, Takamura M, Yamaoka A, Odajima Y, Iikura Y (2002). "Altered eosinophil levels as a result of viral infection in asthma exacerbation in childhood". Pediatr Allergy Immunol. 13 (1): 47–50. doi:10.1034/j.1399-3038.2002.00051.x. PMID 12000498.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Lilly CM (2005). "Diversity of asthma: evolving concepts of pathophysiology and lessons from genetics". J. Allergy Clin. Immunol. 115 (4 Suppl): S526–31. doi:10.1016/j.jaci.2005.01.028. PMID 15806035.
- ^ a b c d McFadden ER, Jr (2004). "Asthma". Harrison's Principles of Internal Medicine (Kasper DL, Fauci AS, Longo DL, et al (eds)) (16th ed. ed.). New York: McGraw-Hill. pp. 1508–16.
{{cite book}}:|edition=has extra text (help) - ^ Longmore, Murray; et al. (2007). Oxford Handbook of Clinical Medicine (7th ed. ed.). Oxford University Press. ISBN 978-0198568377.
{{cite book}}:|edition=has extra text (help); Explicit use of et al. in:|first=(help) - ^ a b Martinez FD (2007). "Genes, environments, development and asthma: a reappraisal". Eur Respir J. 29 (1): 179–84. doi:10.1183/09031936.00087906. PMID 17197483.
- ^ Choudhry S, Seibold MA, Borrell LN; et al. (2007). "Dissecting complex diseases in complex populations: asthma in latino americans". Proc Am Thorac Soc. 4 (3): 226–33. doi:10.1513/pats.200701-029AW. PMID 17607004.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b c d e f Gold DR,Wright R (2005). "Population disparities in asthma". Annu Rev Public Health. 26: 89–113. doi:10.1146/annurev.publhealth.26.021304.144528. PMID 15760282.
- ^ "California Children's Health Study".
- ^ Harju TH, Leinonen M, Nokso-Koivisto J; et al. (2006). "Pathogenic bacteria and viruses in induced sputum or pharyngeal secretions of adults with stable asthma". Thorax. 61 (7): 579–84. doi:10.1136/thx.2005.056291. PMID 16517571.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Richeldi L, Ferrara G, Fabbri LM, Lasserson TJ, Gibson PG (2005). "Macrolides for chronic asthma". Cochrane Database Syst Rev (4): CD002997. doi:10.1002/14651858.CD002997.pub3. PMID 16235309.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Marra F, Lynd L, Coombes M; et al. (2006). "Does antibiotic exposure during infancy lead to development of asthma?: a systematic review and metaanalysis". Chest. 129 (3): 610–8. doi:10.1378/chest.129.3.610. PMID 16537858.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b Thavagnanam S, Fleming J, Bromley A, Shields MD, Cardwell, CR (2007). "A meta-analysis of the association between Caesarean section and childhood asthma". Clin. and Exper. Allergy. online ahead of print: 629. doi:10.1111/j.1365-2222.2007.02780.x.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Jeremy Laurance. "Asthma blamed on cleaning sprays and air fresheners".
- ^ a b c Ober C,Hoffjan S (2006). "Asthma genetics 2006: the long and winding road to gene discovery". Genes Immun. 7 (2): 95–100. doi:10.1038/sj.gene.6364284. PMID 16395390.
- ^ a b Martinez FD (2007). "CD14, endotoxin, and asthma risk: actions and interactions". Proc Am Thorac Soc. 4 (3): 221–5. doi:10.1513/pats.200702-035AW. PMID 17607003.
- ^ a b Maddox L, Schwartz DA (2002). "The pathophysiology of asthma". Annu. Rev. Med. 53: 477–98. doi:10.1146/annurev.med.53.082901.103921. PMID 11818486.
- ^ Jenkins C, Costello J, Hodge L (2004). "Systematic review of prevalence of aspirin induced asthma and its implications for clinical practice". BMJ. 328 (7437): 434. doi:10.1136/bmj.328.7437.434. PMID 14976098.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Nemery B, Hoet PH, Nowak D (2002). "Indoor swimming pools, water chlorination and respiratory health". Eur. Respir. J. 19 (5): 790–3. doi:10.1183/09031936.02.00308602. PMID 12030714.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ about.com article
- ^ Asthma and Altitude
- ^ Szentivanyi, Andor (1968). "The Beta Adrenergic Theory of the Atopic Abnormality in Asthma".
{{cite journal}}: Cite journal requires|journal=(help); Unknown parameter|jounal=ignored (help) - ^ Lockey, Richard, In lasting tribute: Andor Szentivanyi, MD. J. Allergy and Clinical Immunology, January, 2006
- ^ Szentivanyi A., Ali K., Calderon EG., Brooks SM., Coffey RG., Lockey RF. (1993). "The in vitro effect of Imunnoglobulin E {IgE} on cyclic AMP concentrations in A549 human pulmonary epithelial cells with or without beta adrenergic stimulation". J. Allergy Clin Immunol. 91: 379.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Part of Abstracts from:
"50th Anniversary of the American Academy of Allergy and Immunology. 49th Annual Meeting. Chicago, Illinois, March 12-17, 1993. Abstracts". J. Allergy Clin. Immunol. 91 (1 Pt 2): 141–379. 1993. PMID 8421135. - ^ Kowalak JP, Hughes AS et al (eds), ed. (2001). Professional Guide To Diseases (7th ed. ed.). Springhouse.
{{cite book}}:|edition=has extra text (help);|editor=has generic name (help) - ^ Lockey, Richard F. (2006-04-28). "Anaphylaxis: Synopsis". Allergic Diseases Resource Center. World Allergy Organization.
{{cite web}}: Unknown parameter|accessmonthday=ignored (help); Unknown parameter|accessyear=ignored (|access-date=suggested) (help) - ^ Ouellette JJ, Reed CE (1967). "The effect of partial beta adrenergic blockade on the bronchial response of hay fever subjects to ragweed aerosol". J Allergy. 39 (3): 160–6. doi:10.1016/0021-8707(67)90033-0. PMID 5227155.
- ^ Fraser CM, Venter JC (1980). "The synthesis of beta-adrenergic receptors in cultured human lung cells: induction by glucocorticoids". Biochem. Biophys. Res. Commun. 94 (1): 390–7. doi:10.1016/S0006-291X(80)80233-6. PMID 6248064.
- ^ a b Cromie, William J. (2006-03-16). "Researchers uncover cause of asthma". Harvard University Gazette. Harvard News Office. Retrieved 2006-09-23.
- ^ "Breathing disorders during sleep are common among asthmatics, may help predict severe asthma" (Press release). University of Michigan Health System. May 25, 2005. Retrieved 2006-09-23.
- ^ Basner, Robert C. (2006-07-25). "Asthma and OSA". ASAA Resources > Publications. American Sleep Apnea Association.
{{cite web}}: Unknown parameter|accessmonthday=ignored (help); Unknown parameter|accessyear=ignored (|access-date=suggested) (help) - ^ Leggett JJ, Johnston BT, Mills M, Gamble J, Heaney LG (2005). "Prevalence of gastroesophageal reflux in difficult asthma: relationship to asthma outcome". Chest. 127 (4): 1227–31. doi:10.1378/chest.127.4.1227. PMID 15821199.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Pinnock H, Shah R (2007). "Asthma". BMJ. 334 (7598): 847–50. doi:10.1136/bmj.39140.634896.BE. PMID 17446617.
- ^ "Peak flow charting software".
- ^ "'Be in control' pack" (PDF). Asthma UK. Retrieved 2007-11-19.
- ^ Corbo J, Bijur P, Lahn M, Gallagher EJ (2005). "Concordance between capnography and arterial blood gas measurements of carbon dioxide in acute asthma". Annals of emergency medicine. 46 (4): 323–7. doi:10.1016/j.annemergmed.2004.12.005. PMID 16187465.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Vargas PA, Simpson PM, Gary Wheeler J; et al. (2004). "Characteristics of children with asthma who are enrolled in a Head Start program". J. Allergy Clin. Immunol. 114 (3): 499–504. doi:10.1016/j.jaci.2004.05.025. PMID 15356547.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Thomson NC, Spears M (2005). "The influence of smoking on the treatment response in patients with asthma". Curr Opin Allergy Clin Immunol. 5 (1): 57–63. PMID 15643345.
- ^ Eisner MD, Yelin EH, Katz PP, Earnest G, Blanc PD (2002). "Exposure to indoor combustion and adult asthma outcomes: environmental tobacco smoke, gas stoves, and woodsmoke". Thorax. 57 (11): 973–8. doi:10.1136/thorax.57.11.973. PMID 12403881.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b National Asthma Education and Prevention Program. Expert Panel Report: Guidelines for the Diagnosis and Management of Asthma. National Institutes of Health pub no 97–4051. Bethesda, MD, 1997. (PDF)
- ^ Asthma and Air Filters Asthma and Air Filters
- ^ Abramson MJ, Puy RM, Weiner JM (1995). "Is allergen immunotherapy effective in asthma? A meta-analysis of randomized controlled trials". Am. J. Respir. Crit. Care Med. 151 (4): 969–74. PMID 7697274.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ British Thoracic Society & Scottish Intercollegiate Guidelines Network (SIGN). British Guideline on the Management of Asthma. Guideline No. 63. Edinburgh:SIGN; 2004. (HTML, Full PDF, Summary PDF)
- ^ K Baillie, "Asthma Trials", ClinicLog.com, accessed 05-07-2008.
- ^ a b Hendeles L, Marshik PL, Ahrens R, Kifle Y, Shuster J (2005). "Response to nonprescription epinephrine inhaler during nocturnal asthma". Ann. Allergy Asthma Immunol. 95 (6): 530–4. PMID 16400891.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Rodrigo GJ, Nannini LJ (2006). "Comparison between nebulized adrenaline and beta2 agonists for the treatment of acute asthma. A meta-analysis of randomized trials". Am J Emerg Med. 24 (2): 217–22. doi:10.1016/j.ajem.2005.10.008. PMID 16490653.
- ^ Papi A, Canonica GW, Maestrelli P; et al. (2007). "Rescue use of beclomethasone and albuterol in a single inhaler for mild asthma". N. Engl. J. Med. 356 (20): 2040–52. doi:10.1056/NEJMoa063861. PMID 17507703.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ "Serevent Diskus, Advair Diskus, and Foradil Information (Long Acting Beta Agonists) - Drug information". FDA. 2006-03-03.
{{cite web}}: Check date values in:|year=(help) - ^ Salpeter S, Buckley N, Ormiston T, Salpeter E (2006). "Meta-analysis: effect of long-acting beta-agonists on severe asthma exacerbations and asthma-related deaths". Ann Intern Med. 144 (12): 904–12. PMID 16754916.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Ramanujan, Krishna (2006-06-09). "Common asthma inhalers cause up to 80 percent of asthma-related deaths, Cornell and Stanford researchers assert". Cornell Chronicle Online. Cornell News Service. Retrieved 2006-09-23.
- ^ Rodrigo GJ, Rodrigo C, Hall JB (2004). "Acute asthma in adults: a review". Chest. 125 (3): 1081–102. doi:10.1378/chest.125.3.1081. PMID 15006973.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Rodrigo G (2005). "Comparison of inhaled fluticasone with intravenous hydrocortisone in the treatment of adult acute asthma". Am J Respir Crit Care Med. 171 (11): 1231–6. doi:10.1164/rccm.200410-1415OC. PMID 15764724.
- ^ Blanc PD, Trupin L, Earnest G, Katz PP, Yelin EH, Eisner MD (2001). "Alternative therapies among adults with a reported diagnosis of asthma or rhinosinusitis : data from a population-based survey". Chest. 120 (5): 1461–7. doi:10.1378/chest.120.5.1461. PMID 11713120.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Shenfield G, Lim E, Allen H (2002). "Survey of the use of complementary medicines and therapies in children with asthma". J Paediatr Child Health. 38 (3): 252–7. doi:10.1046/j.1440-1754.2002.00770.x. PMID 12047692.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ McCarney RW, Brinkhaus B, Lasserson TJ, Linde K (2004). "Acupuncture for chronic asthma". Cochrane Database Syst Rev (1): CD000008. doi:10.1002/14651858.CD000008.pub2. PMID 14973944.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Blackhall K, Appleton S, Cates CJ (2003). "Ionisers for chronic asthma". Cochrane Database Syst Rev (3): CD002986. doi:10.1002/14651858.CD002986. PMID 12917939.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Hondras MA, Linde K, Jones AP (2005). "Manual therapy for asthma". Cochrane Database Syst Rev (2): CD001002. doi:10.1002/14651858.CD001002.pub2. PMID 15846609.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Reilly D, Taylor MA, Beattie NG; et al. (1994). "Is evidence for homoeopathy reproducible?". Lancet. 344 (8937): 1601–6. doi:10.1016/S0140-6736(94)90407-3. PMID 7983994.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ White A, Slade P, Hunt C, Hart A, Ernst E (2003). "Individualised homeopathy as an adjunct in the treatment of childhood asthma: a randomised placebo controlled trial". Thorax. 58 (4): 317–21. doi:10.1136/thorax.58.4.317. PMID 12668794.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Nagendra HR, Nagarathna R (1986). "An integrated approach of yoga therapy for bronchial asthma: a 3-54-month prospective study". J Asthma. 23 (3): 123–37. doi:10.3109/02770908609077486. PMID 3745111.
- ^ Manocha R, Marks GB, Kenchington P, Peters D, Salome CM (2002). "Sahaja yoga in the management of moderate to severe asthma: a randomised controlled trial". Thorax. 57 (2): 110–5. doi:10.1136/thorax.57.2.110. PMID 11828038.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Nagourney E (2007-11-13). "For the Record: In Tests of Inhalers, Results May Depend on Who Pays". The New York Times. Retrieved 2007-12-02.
{{cite news}}: Italic or bold markup not allowed in:|publisher=(help) - ^ Nieto A, Mazon A, Pamies R; et al. (2007). "Adverse effects of inhaled corticosteroids in funded and nonfunded studies". Arch. Intern. Med. 167 (19): 2047–53. doi:10.1001/archinte.167.19.2047. PMID 17954797.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Beckett PA, Howarth PH (2003). "Pharmacotherapy and airway remodelling in asthma?". Thorax. 58 (2): 163–74. doi:10.1136/thorax.58.2.163. PMID 12554904.
- ^ a b World Health Organization. "Bronchial asthma: scope of the problem". Retrieved 2005-08-23.
- ^ World Health Organization. "WHO: Asthma". Retrieved 2007-12-29.
- ^ Lara M, Akinbami L, Flores G,Morgenstern H (2006). "Heterogeneity of childhood asthma among Hispanic children: Puerto Rican children bear a disproportionate burden". Pediatrics. 117 (1): 43–53. doi:10.1542/peds.2004-1714. PMID 16396859.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Davis AM, Kreutzer R, Lipsett M, King G,Shaikh N (2006). "Asthma prevalence in Hispanic and Asian American ethnic subgroups: results from the California Healthy Kids Survey". Pediatrics. 118 (2): e363–70. doi:10.1542/peds.2005-2687. PMID 16882779.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Johnson DB, Oyama N, LeMarchand L,Wilkens L (2004). "Native Hawaiians mortality, morbidity, and lifestyle: comparing data from 1982, 1990, and 2000". Pac Health Dialog. 11 (2): 120–30. PMID 16281689.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Naqvi M, Thyne S, Choudhry S; et al. (2007). "Ethnic-specific differences in bronchodilator responsiveness among african americans, puerto ricans, and mexicans with asthma". J Asthma. 44 (8): 639–48. doi:10.1080/02770900701554441. PMID 17943575.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Burchard EG, Avila PC, Nazario S; et al. (2004). "Lower bronchodilator responsiveness in Puerto Rican than in Mexican subjects with asthma". Am J Respir Crit Care Med. 169 (3): 386–92. doi:10.1164/rccm.200309-1293OC. PMID 14617512.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Gold DR,Acevedo-Garcia D (2005). "Immigration to the United States and acculturation as risk factors for asthma and allergy". J Allergy Clin Immunol. 116 (1): 38–41. doi:10.1016/j.jaci.2005.04.033. PMID 15990770.
- ^ Eldeirawi KM,Persky VW (2006). "Associations of acculturation and country of birth with asthma and wheezing in Mexican American youths". J Asthma. 43 (4): 279–86. doi:10.1080/0277090060022869. PMID 16809241.
- ^ "Patient/Public Education: Fast Facts - Asthma Demographics/Statistics". American Academy of Allergy Asthma & Immunology. Retrieved 2006-05-02.
- ^ National Heart, Lung, and Blood Institute (May 2004). "Morbidity & Mortality: 2004 Chart Book On Cardiovascular, Lung, and Blood Diseases". National Institutes of Health.
{{cite journal}}: Cite journal requires|journal=(help)CS1 maint: multiple names: authors list (link) - ^ National Center for Health Statistics (07 April 2006). "Asthma Prevalence, Health Care Use and Mortality, 2002". Centers for Disease Control and Prevention.
{{cite web}}: Check date values in:|year=(help) - ^ a b Weiler JM, Layton T, Hunt M (1998). "Asthma in United States Olympic athletes who participated in the 1996 Summer Games". J. Allergy Clin. Immunol. 102 (5): 722–6. doi:10.1016/S0091-6749(98)70010-7. PMID 9819287.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Helenius I, Haahtela T (2000). "Allergy and asthma in elite summer sport athletes". J. Allergy Clin. Immunol. 106 (3): 444–52. doi:10.1067/mai.2000.107749. PMID 10984362.
- ^ Asthma and depression: a pragmatic review of the literature and recommendations for future research Clin Pract Epidemol Ment Health. 2005; 1: 18. Published online 2005 September 27. doi: 10.1186/1745-0179-1-18. PMCID: PMC1253523 Copyright © 2005 Opolski and Wilson; licensee BioMed Central Ltd. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1253523
External links
- VIDEO Identifying Risk Factors for Childhood Asthma Presentation by James E. Gern, M.D., at the UW-Madison Health Sciences Learning Center.
- ATSDR Case Studies in Environmental Medicine: Environmental Triggers of Asthma U.S. Department of Health and Human Services
- World Health Organization site on asthma
- National Heart, Lung, and Blood Institute — Asthma – U.S. NHLBI Information for Patients and the Public page.
- MedLinePlus: Asthma – a U.S. National Library of Medicine page
- Neurogenic factors in mechanisms of bronchial asthma
- Asthma Helpline
- Free Asthma Forecasting and Educational Website
