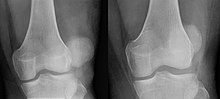
Patellar luxation
| Classification according to ICD-10 | |
|---|---|
| M22.0 | Habitual dislocation of the patella |
| M22.1 | Habitual subluxation of the patella |
| M22.2 | Diseases in the patellofemoral area |
| S83.0 | Dislocation of the patella (as a result of an external cause) |
| ICD-10 online (WHO version 2019) | |

Patellar dislocation is a knee joint injury in which the kneecap ( patella ) jumps out of its guide ( dislocation ). Usually the kneecap moves back spontaneously to its original position ( reduction ). It rarely remains in its dislocated position on the outside ( lateral ) of the knee joint.
With an incidence of 5.8 / 100,000 in the general population, patellar dislocation is one of the most common knee joint injuries. It also occurs in animals such as domestic dogs and cats.
predisposition
The most common causes of patellar dislocation are the following predisposing factors:
- congenital malformation of the kneecap and the plain bearing ( dysplasia of the femoral condyles )
- Axis or rotational misalignment of the knee joint ( genu valgum , " knock-kneed ")
- a raised kneecap (patella alta) and lateral attachment of the kneecap tendon to the shin. As a result, the kneecap tends not to slide centrally between the femoral condyles , but too far outside (laterally). With increasing flexion, a dislocation can occur. Rotational movements in the knee joint, for example during sport, have a beneficial effect, whereby the point of attachment of the kneecap tendon is shifted outwards and thus the direction of pull of the tendon is changed.
The following are also possible:
- Muscle imbalance
- Changes in the straps of the patella
- Band laxity also in Ehlers-Danlos syndrome , arachnodactyly , osteogenesis imperfecta , Turner syndrome , trisomy 21 , Kabuki syndrome
- in the context of (other) syndromes such as diastrophic dysplasia , Ellis-van-Creveld-Syndrome or Scholte-Syndrome (mental retardation - balding - patellar dislocation - acromicria)
Classification
Depending on the underlying cause, the following classification is common:
- acute traumatic dislocation (rare), due to adequate trauma such as the accident, which often leads to the rupture of the anterior cruciate ligament
- acute dispositional dislocation (more often) in the presence of predisposing factors, due to inadequate trauma, changes into recurrent form
- recurrent dislocation, occurring more and more frequently over time
- habitual dislocation, can be produced arbitrarily
- congenital dislocation, already present at birth, small, dysplastic or missing patella, e.g. B. in nail-patella syndrome , Prieto syndrome , arthrogryposis multiplex congenita
- neurogenic dislocation, due to abnormal pulling of the vastus lateralis muscle , in tetraspasticity
- Iatrogenic dislocation after inadequate operations on the patella or leg axis
effect
During the dislocation, the kneecap does not run in its regular patellar sliding bearing on the thigh roller between the femoral condyles, but always laterally along the lateral condyle. As the flexion increases, the kneecap becomes entrapped as the tendon tension increases. In this dislocated position, repositioning of the kneecap is only possible by applying force and causing cartilage-bone damage to both the kneecap and the lateral condylar cheek. This cartilage damage is the most damaging effect of patellar dislocation. In the case of patellar luxation, the medial holding apparatus of the kneecap (retinaculum) is usually torn, resulting in a bruise in the knee joint (hemarthrosis). If the retinaculum is torn or stretched, there is an increased risk of repeated dislocation ( relapse ) or even habitual dislocation (habitual dislocation).
treatment
In any case - if this has not happened by itself - the kneecap must be adjusted. Under the guidance of the doctor or an experienced sports trainer, the knee should be slowly and carefully straightened again, with the kneecap being held firmly with the hand so that it does not suddenly jump. If the kneecap is carefully brought into the starting position, it can be reduced again without any accompanying injury to the articular surfaces. There should not be a violent snap, which can cause cartilage damage. After the reduction, the affected person notices a clear reduction in pain. After the reduction, the knee should be x-rayed and an MRI scan should be performed to check the correct position of the kneecap and to rule out accompanying injuries.
Conservative treatment
- In general, any treatment of uncomplicated dislocation of the kneecap (without cartilage-bone lesion) is started with conservative therapy.
- If necessary, puncture of the knee joint under sterile conditions (today only performed in exceptional cases)
- Bandage, orthosis or plaster sleeve (plaster tutor)
- Physiotherapy (mobilization, strengthening of the vastus medialis musculi quadricipitis )
Operative treatment
Since conservative therapy leads to definitive success (no recurrence) in more than 50% of uncomplicated kneecap dislocations, every treatment should begin with a conservative concept. In the case of the first reluxation, the indication for surgery is given, unless there are important contraindications. In the so-called recurrent patellar dislocation, there are various surgical measures that lead to the fact that the patella no longer dislocates and can damage the cartilage in the process.
The aim of the operation is to stabilize the kneecap centrally between the femoral condyles in their plain bearing. To do this, the torn medial retinaculum is sutured at the site of the tear. Most of the time the crack is located exactly on the edge of the kneecap. In rare cases, the retinaculum can also be torn off at the epicondyle of the medial thigh roll. As a first measure of the operation, a knee joint arthroscopy is performed to show the retinacular lesion in its localization, to prove the integrity of the joint surfaces of the patella and femoral condyles or to confirm the extent and location of possible cartilage damage. All other joint structures ( menisci , cruciate ligaments ) must also be checked. The reconstruction of the retinaculum by suturing is carried out surgically because an exact anatomical adaptation under tension is not arthroscopically possible. Due to the unreliable stabilization by suturing the medial retinaculum, plastic reinforcement or plastic of the medial patellofemoral ligament (MPFL) is more common today (see below).
A number of interventions can be carried out in addition or as an alternative. Above all, this includes a so-called "lateral release", i.e. i.e., a limited arthroscopic or open transection of the lateral retinaculum of the kneecap. According to more recent studies, this part of the operation tends to lead to an even greater instability of the patella. In addition, the blood circulation is worsened because the kneecap receives its essential inflow via the lateral retinaculum. In special anatomical conditions such as B. in the case of lateralization of the attachment tendon of the kneecap, the shifting of the attachment point ( tibial tuberosity ) together with the tendon can take place medially. A large number of surgical procedures are described for this purpose:
- Operation according to Roux or Elmslie (tibial tuberosity is displaced medially and fixed with screws)
In the case of previously damaged retinaculum tissue and multiple dislocations, the medial reconstruction must be supplemented with ligament reinforcement (MPFL plastic):
- MPFL (mediales patello femoral ligament) reconstruction: A tendon from the knee region is used for this, which is also used in cruciate ligament surgery : it is the tendon of the semitendinosus or gracilis muscle . This is removed and guided along the medial retinaculum from the medial epicondyle to the edge of the patella, where it is fixed with implants (e.g. interference screws) or sutured to itself through a V-shaped canal. This ligament plasty creates a high degree of security against a relapse of dislocation. The most important thing in this operation is the correct insertion on the femur (thigh bone). This insertion is at the Schoettle point , a point that was described by the German orthopedic surgeon Philip Schöttle in 2007 and is now considered an international standard. If this point is too far forward (anterior) or too far up (proximal), this painfully restricts postoperative mobility.
The dysplastic plain bearing very rarely has to be tackled surgically. The effort here is very high, and the results usually leave something to be desired.
- Trochleaplastik, in this case the joint surface of the plain bearing is deepened in order to create an isosceles concave plain bearing and good guidance for the kneecap. This surgical technique is only performed in a few cases due to the considerable surgical effort involved.
Postoperatively, physiotherapeutic mobilization of the knee joint should take place at an early stage in order to avoid adhesions. Relief of the operated leg is not necessary. The free function can be expected to resume after approx. 6 weeks.
In dogs, the best results are achieved by relocating the tibia bulge (surgery according to Roux) while at the same time deepening the patella slide (trochleaplasty). One study showed a good result in 56%, a satisfactory result in 36% and an unsatisfactory result in 8%. A progressive osteoarthritis of the knee joint must be expected even with a successful operation.
Patellar luxation in the dog
Patellar luxation in dogs is particularly common in small dog breeds, especially the Chihuahua , but also in the Yorkshire Terrier , Jack Russell Terrier and other breeds . With the Chihuahua it is now relatively typical and often leads to the "three-legged walk" known among dog owners , in which the dog hops on only three legs every few meters before running again as if nothing had happened. In this case, the kneecap usually pops out, the dog tries not to put any further strain on the leg (which is why it hops on three legs), then the kneecap slides back into the groove on its own and the dog can walk completely normally again.
There are four general degrees of patellar dislocation in dogs.
In dog breeds in which the genetic disposition for patellar luxation is known, breeders are required to have a dog's kneecaps examined as part of a veterinary breeding suitability test before a decision is made as to whether it should be used for breeding.
Individual evidence
- ^ J. Dickschas, C. Roeder, F. Hennig, W. Strecker, V. Schoeffl: Ability to exercise after patellar luxation. In: Sports injury · Sports damage. 23, 2009, pp. 95-99, doi: 10.1055 / s-0028-1109451 .
- ↑ a b F. Hefti: Pediatric orthopedics in practice. Springer 1998, ISBN 3-540-61480-X
- ↑ Mental retardation - baldness - patellar luxation - acromicria. In: Orphanet (Rare Disease Database).
- ↑ Orthobullets
- ^ W. Petersen, P. Forkel, A. Achtnich: Chronic patellofemorale instability. In: The trauma surgeon. 115, 2012, pp. 397-409, doi: 10.1007 / s00113-012-2197-9 .
- ↑ M. Nelitz, J. Dreyhaupt, H. Reichel, J. Woelfle, p Lippacher: Anatomic Reconstruction of the Medial Patellofemoral Ligament in Children and Adolescents With Open Growth Plates: Surgical Technique and Clinical Outcome. In: The American journal of sports medicine. [electronic publication before printing] October 2012, ISSN 1552-3365 . doi: 10.1177 / 0363546512463683 . PMID 23111806 .
- ^ PB Schöttle, A. Schmeling , N. Rosenstiel, A. Weiler: Radiographic landmarks for femoral tunnel placement in medial patellofemoral ligament reconstruction. In: The American journal of sports medicine. Volume 35, Number 5, May 2007, ISSN 0363-5465 , pp. 801-804, doi: 10.1177 / 0363546506296415 , PMID 17267773 .
- ↑ B. Schmitz et al .: Luxatio patellae in dogs: Investigations into the success of therapy. In: Kleintierpraxis , Volume 61, No. 10, 2016, pp. 580-581.