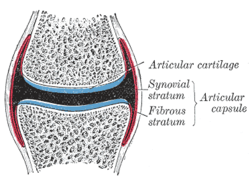
Joint capsule
The joint capsule ( Latin Capsula articularis ) is a connective tissue covering around real joints . It encloses the joint cavity filled with joint fluid ( synovia ).
Layout and function
The joint capsule is divided into two layers:
- Membrana fibrosa ( Stratum fibrosum )
- Membrana synovialis ( Stratum synoviale , synovial membrane)
Membrana fibrosa
The outer fibrous membrane consists of tight collagenous connective tissue. She goes in the neck area of the joint capsule into the periosteum over (periosteum). It determines the mechanical strength of the joint and releases the range of motion characteristic of the joint.
In most joints, the fibrous membrane is reinforced in stripes at certain points. These band-like capsular ligaments ( Ligamenta capsularia ) serve to further stabilize the joint ends and, as guide or inhibition bands, ensure that the mobility of the joint is limited to certain directions or degrees of movement. When loose connective tissue separates the joint ligaments from the fibrous membrane , one speaks of extracapsular ligaments.
There are various receptors in the fibrous membrane : Ruffini bodies , Vater-Pacini bodies and Golgi tendon organs . They register the position of the joint (so-called proprioceptive perception ). In addition, the membrana fibrosa has free nerve endings that act as nociceptors to absorb pain stimuli. They are responsible for the fact that capsule expansions and tears are extremely painful.
Synovial membrane
The synovial membrane (also briefly synovium called) or joint lining forming the inner lining of the joint cavity. It consists of several layers of so-called synovialocytes . This layer is not an epithelium - the typical cell contacts and a basement membrane are missing. Rather, it is a loose connective tissue in which the cells are spread out over a large area, as well as individual fat cells. There are two types of synovial cells:
- A synovialocytes:
The A synovialocytes are macrophages and are derived from the monocytes of the blood . They are used for resorption and phagocytosis , and to a lesser extent also for the synthesis of synovial components. - B synovialocytes:
B synovialocytes are similar to fibroblasts and make up most of the synovia .
The interplay between production and resorption of the synovia normally causes the joint to be cleaned of abrasion products. With osteoarthritis , however, so much occurs that this mechanism is overwhelmed. If an endoprosthesis has been inserted, the metal abrasion or abrasion of the bone cement can also accumulate in the A synovialocytes and then not be transported away from there.
Compound joints that involve more than two bones (e.g., knee , wrist , ankle ) share a common fibrous membrane . Several delimited internal spaces formed by the synovial membrane can lie within the common outer capsule. Here the inner skin forms several delimited partial joint cavities that either communicate with one another or can also be completely separated from one another.
Pathological changes in the joint capsule
Instabilities
In the event of a sprain or dislocation , the ligamentous apparatus, part of the joint capsule, is injured and often does not heal to the extent that the joint is sufficiently stable afterwards. This often happens on the ankle , the metatarsophalangeal joint of the thumb (“skier's thumb”) or the knee. The poor, less precise guidance of the joint leads to uneven loading of the cartilage layer. An injury-related post-traumatic osteoarthritis is the result.
Irritable states
Injuries, operations or inflammatory diseases can lead to swelling of the joint capsule. The swollen ligaments lose their suppleness, the joint loses its mobility to a greater or lesser extent.
Inflammatory diseases
An inflammation of the synovial membrane called synovitis . In rheumatoid arthritis , synovial cells change their function, become aggressive and overgrow the cartilage layer from the edges. The cartilage is then literally eaten up by these cells.
Capsule injury
In the event of an accident, the joint capsule can be injured or tear. If the capsule is damaged, there is bleeding into the joint ( hemarthrosis ). If the joint capsule is irritated, an irritant effusion occurs even without the involvement of blood vessels ( see section “Irritation” ). The capsule injury leads to pain, heating, swelling and restricted movement of the joint .
A hematoma indicates that the capsule has been injured, but an injury or a tear in the capsule can occur even without a hematoma. At the same time as a joint capsule injury, the affected joint is usually sprained or dislocated . Often, a torn capsule is also a torn ligament or a torn muscle fiber .
In the event of a capsule rupture, elevation and immediate cooling for 10–20 minutes are recommended, and in the further course of the disease, elevation and mechanical relief or immobilization, as well as compression to limit the physiological, inflammatory tendency to swell, are recommended. In the case of pronounced, long-lasting hemarthrosis, a joint puncture is an option in order to avoid damage to the joint.
The inner layer of the joint capsule (the synovial membrane) reacts to the injury with an inflammatory reaction called synovitis . The composition and the amount of synovial fluid change considerably ( see: Synovia: Pathological changes ). Treatment of the injured capsular tissue is therefore primarily about normalizing the function of the synovial membrane.
literature
- Theodor Heinrich Schiebler : Anatomy: histology, history of development, macroscopic and microscopic anatomy, topography . 9th edition. Springer, Berlin 2006, ISBN 978-3-540-26525-2 , pp. 174 .
Web links
- Entry on the joint capsule in the Flexikon , a Wiki of the DocCheck company
- Entry on joint capsule - Capsula articularis in the fitness lexicon of the Academy for Sport and Health.
Individual evidence
- ↑ Wolfgang Miehle: Joint and spinal rheumatism. Eular Verlag, Basel 1987, ISBN 3-7177-0133-9 , p. 175.
- ^ Pschyrembel Clinical Dictionary . Founded by Willibald Pschyrembel. Edited by the publisher's dictionary editor. 255th edition. De Gruyter, Berlin 1986, ISBN 978-3-11-018534-8 , p. 1630 f.
- ↑ a b Frans van den Berg: Applied Physiology , Georg Thieme Verlag, 2007, ISBN 978-3-13-117092-7 . P. 151 .
- ^ Frans van den Berg: Applied Physiology , Georg Thieme Verlag, 2007, ISBN 978-3-13-117092-7 . P. 152 .