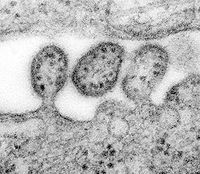
Lassa fever
| Classification according to ICD-10 | |
|---|---|
| A96.2 | Lassa fever |
| ICD-10 online (WHO version 2019) | |
The Lassa fever is a notifiable disease, is like the Marburg fever to viral hemorrhagic fevers .
history
Lassa fever was first described in 1969. At that time, an American missionary sister died in Nigeria , another fell ill and was flown to the USA for treatment . The virus was named after the city of Lassa, in what is now Borno state , where the first nurse worked. In New York City , two laboratory infections occurred among scientists who isolated the virus, and one of the infected died as a result of the disease.
Pathogen
The cause of Lassa fever is an enveloped single (-) - strand RNA virus = ss (-) RNA with high virulence and belongs to the genus Arena virus and thus to the family Arenaviridae . The pathogens of June fever and machupo fever also belong to the same virus family . They are all assigned the highest biological safety level 4. From Lassa virus so far four serological subtypes are known: Type Nigeria, Sierra Leone, Liberia and type Central African Republic.
The relatively high mortality rate of the disease caused by these viruses indicates that the Lassa viruses are not yet particularly well adapted to humans. A virus that has been adapted to its host has no interest in destroying it in the sense of selection pressure, because it needs it for its reproduction. Serological data suggest, however, that at least in West Africa around 90 to 95% of all infections could proceed without an outbreak of the disease. This would mean that local people in the natural range of the virus have already adapted to the local population or the virus.
The natal multi-teat mouse ( Mastomys natalensis ) has been identified as the natural reservoir host for the Lassa virus, along with other small rodents .
Epidemiology
The Lassa virus is found constantly present (endemic) in the West African countries Senegal , Gambia , Mali , Guinea , Liberia , Sierra Leone , Ivory Coast , Ghana , Burkina Faso and Nigeria . It has also been found in other tropical countries such as the Central African Republic and Namibia . There are related viruses all over the African continent, but they do not cause any disease in humans. Up to 15 percent of the multi-teat mice in these areas are infected with the virus.
It is estimated that about 100,000-300,000 cases of Lassa fever occur in West Africa each year, and about 70% are subclinical. The mortality rate ranges between 2% in the villages, 15–16% in the hospitals and 30–50% in pregnant women. In West Africa, there have been multiple outbreaks in hospitals, particularly in Nigeria , Liberia and Sierra Leone , often with deaths among medical staff. In the past, sporadic cases were observed in Germany. In March 2016, an undertaker in Alzey (Rhineland-Palatinate) was possibly infected with the Lassa virus after coming into contact with the body of a man who died at the Cologne University Hospital at the end of February . He had previously worked as a nurse in Togo and was infected with the virus there, but this was only discovered several days after his death. It is the first infection outside of Africa and the first case of transmission within Germany. Since the man was admitted to the special isolation ward of the University Clinic in Frankfurt am Main at an early stage , there were good prospects of recovery. After five weeks in the clinic, the patient was discharged as cured.
transmission
The Lassa virus is transmitted by the natal multi-teat mouse ( Mastomys natalensis ), which is widespread in African houses, via contact infection or smear infection via the excretions of the animals to food subsequently consumed by humans. In addition, the pathogen viruses can also be transmitted directly from person to person as well as through sexual intercourse via droplet infection , wound infection and secretions . Before the outbreak of the disease - i.e. during the incubation period - the only possibility of transmission by infected people was determined via the blood.
Previously, a seasonal increase in incidence was assumed during the dry season from January to March. In Sierra Leone, however, an epidemic peak was observed in the transition to the rainy season (May to November).
Clinical picture
Course of disease
The incubation period of Lassa fever is between 6 and 21 days, but mostly 7 to 10 days.
After a gradual onset of illness with exhaustion, flu-like muscle and limb pain, nausea and headache, a permanent fever ( continuous fever ) of 40 ° C develops . From the 3rd to the 7th day, symptoms of inflammation appear in the throat, then later whitish plaques and ulcerations . The patients are very generally reduced and apathetic. The cervical lymph nodes (cervical lymph nodes) are enlarged and tender (pain when pressure is applied to the lymph nodes).
From the 7th day onwards, a maculo-papular rash (blotchy skin rash with small, raised nodules) often develops on the face, neck and arms, which then spreads to the whole body. At the same time, colicky abdominal pain occurs, the stool is from a pulpy consistency to diarrhea. Vomiting is possible due to the poor general condition. Occasionally, there is generalized swelling of the lymph nodes. The crisis occurs between the 7th and 14th day. Food intake is difficult because of the ulcerations and swellings; breathing can also be impaired. Most patients have a hepato- splenomegaly on (liver and spleen). Hemorrhagic diathesis (tendency to bleeding) occurs due to the reduced coagulation factors with a normal platelet count and increased permeability of the capillaries due to wall damage. Proteinuria and microhematuria indicate kidney involvement . After a short defervation after the 5th – 7th On the 2nd day, the fever may rise again after another three to five days. The prognosis is grave and the mortality rate for hospitalized patients is about 15-16%, but about 30-50% for pregnant women.
Complications
Between the 5th and 8th day of the onset of Lassa fever, the tendency to hemorrhagic bleeding ( diathesis ) is a dreaded complication, as is pneumonia , possibly with accompanying pleuritis and effusion. It often occurs in the second week and has been the cause of death in some cases. They include still meningism , confusion and dizziness. The recovery is significantly delayed, and circulatory problems may persist after the disease for a long time.
diagnosis
Test for pathogens in the pharynx, the pleural or ascites punctate, or through an increase in the titer in the complement fixation reaction. These tests can only be carried out in laboratories with special safety equipment.
Malaria , influenza , typhoid and septic fever are possible differential diagnoses .
therapy
No specific therapy is known. The antiviral agent ribavirin (oral, intravenous or as immune plasma) was successful within the first six days of the disease . Convalescent serum was given in 6 other cases and was also successful in 5 of these 6 cases. Antipyretic drugs are given and the most careful care is a matter of course. Constant monitoring of the fluid balance and the circulation is necessary.
prevention
There is currently no preventive vaccination against Lassa fever , but work is underway on the development of a vaccine .
Sick people and people suspected of having an illness must be strictly isolated. The patient's excrement must be disinfected prior to disposal. Protective clothing is necessary in contact with patients.
Reporting requirement
In Switzerland, the disease is Lassa fever notifiable and that after the Epidemics Act (EpG) in connection with the epidemic Regulation and Annex 1 of the Regulation of EDI on the reporting of observations of communicable diseases of man . Doctors, hospitals etc. are required to report. Criteria for reporting are clinical suspicion and consultation with a specialist in infectious diseases and the initiation of a pathogen-specific laboratory diagnosis.
In Germany, the Infection Protection Act (IfSG) prescribes in Section 6 IfSG a general obligation to report by name in the event of suspected diseases or deaths from viral hemorrhagic fevers . In addition, according to this law, direct or indirect evidence of other pathogens causing haemorrhagic fever is subject to notification in accordance with Section 7 IfSG if the evidence indicates an acute infection. In contrast to almost all other infections in the case of hemorrhagic fevers that can be transmitted from person to person, immediate isolation is mandatory for the sick person ( Section 30 (1) sentence 1 IfSG [quarantine], together with pulmonary plague).
In Austria, virus-related hemorrhagic fever is notifiable in the event of suspicion, illness or death in accordance with Section 1 Paragraph 1 Number 1 of the 1950 Epidemic Act . Doctors and laboratories, among others, are obliged to report this ( Section 3 Epidemics Act).
literature
- Joseph B. McCormick: Death Zone 4. The Fight Against the Killer Viruses; a factual thriller (= Econ & List. Vol. 26555). Econ-und-List-Taschenbuch-Verlag, Munich 1998, ISBN 3-612-26555-5 .
Web links
- RKI : Lassa fever . As of April 1, 2014, last accessed on August 19, 2014.
- Peter Roese: Researchers capitulate to a virus . In: Die Zeit , No. 8/1970; On: zeit.de , updated on February 20, 1970, last accessed on August 19, 2014.
- WHO: Fact sheet No. 179: Lassa fever. (English) ( Memento from 23 August 2011 in the Internet Archive )
Individual evidence
- ↑ Nigeria: Lassa Fieber - News 3080 . On: tropenmedicus.de of March 21, 2008, last accessed on August 19, 2014.
- ^ Lassa fever in West Africa. On: infografikdienst.de ( Memento from September 29, 2007 in the Internet Archive )
- ↑ Infected on a corpse in Alzeyer funeral parlor / Lassa patient not in critical condition . On: swr.de from March 17, 2016.
- ↑ Ali Reza Houshami: Lassa patient from Alzey shows signs of severe virus infection - doctors are nevertheless optimistic . In: Allgemeine Zeitung (Mainz) . of March 18, 2016, p. 36.
- ↑ RP ONLINE: Lassa virus: Undertaker may be infected by corpse. In: RP ONLINE. Retrieved March 16, 2016 .
- ^ Ingrid Karb: Frankfurt Lassa patient seriously ill . In: Frankfurter Allgemeine . 17th March 2016.
- ↑ Dpa of 20 April 2016: cured Lassa Patient: Frankfurt University Clinic . On: pharmische-zeitung.de ; last accessed on April 8, 2017.