typhus
| Classification according to ICD-10 | |
|---|---|
| A01.0 | Typhus abdominalis |
| ICD-10 online (WHO version 2019) | |
Typhus or typhoid fever (including typhoid fever , German typhoid fever , and typhoid fever , typhoid fever or enteric fever called formerly also "brain fever ') is a systemic infectious disease caused by the bacterium Salmonella enterica ssp. enterica Serovar Typhi . For convenience, the old name Salmonella Typhi is often used. The second name Typhi is capitalized because it is not a species name , but aSerovar .
The course of the disease is mainly characterized by a high fever. If left untreated, the disease can be dangerous and lead to death. Typhus is notifiable in Germany , Austria and Switzerland .
As paratyphoid , however, refers to a typhoid fever resembling attenuated disease whose causative agent is not Salmonella Typhi , but Salmonella Paratyphi is.
In older texts and English called typhoid fever , the typhus .
Word origin and terms
The name typhus is derived from the ancient Greek τῦφος typhos , which means' haze ',' fog ',' smoke ',' steam ', but also figuratively means' fogging of the senses' or dizziness ' or' foggy state of mind '. This refers to the neurological symptoms of the disease, particularly the drowsiness as "fogged consciousness".
In international usage, such as B. in English, the disease is known under the name typhoid fever , while the word typhus (cf. Greek typho , "burn slowly") describes the disease caused by rickettsia in German spotted fever , but occasionally also "typhoid fever ". Typhus was previously also known as Typhus levissimus or Typhus ambulatorius . The German Institute for Medical Documentation and Information (DIMDI) follows the international nomenclature and describes the disease described here as "typhoid fever".
story
Typhus (abdominal typhus) has been common since ancient times and was also known to Hippocrates of Kos . In 1546 Girolamo Fracastoro announced the disease under the name morbus lenticularis , who also recognized the risk of transmission from person to person. This assumption was confirmed by epidemics in Naples and Hungary in 1556. A more detailed description of the clinical picture was given in 1659 by Thomas Willis . It was not until 1760 that Boissier de Sauvages proposed the name typhus . In 1847, William Jenner established the distinction between typhus and typhus , which he published in 1850. The bacillus was first detected microscopically in 1880 by Carl Joseph Eberth in the spleen and mesenteric glands ( mesenteric glands, glandulae mesentericae) and cultivated in pure form in 1884 by Georg August Gaffky , but its distribution path initially remained unknown. Almroth Wright introduced vaccination in 1897 .
Germany
For a long time it was unclear about the sources of infection for typhoid. After the devastating cholera epidemic in Hamburg in 1892 and the typhus epidemic in Gelsenkirchen in 1901 , however, increased attention was paid to drinking water as a means of spreading contagious diseases.
The south-west of Germany , in which typhus was widespread above average, became an experimental area for medicine towards the end of the 19th century. Malstatt-Burbach , Ottweiler and Hülzweiler, for example, were the scenes of major epidemics in the 1880s and 1890s, in which numerous people died. In addition to the people employed in the mining industry, who mostly lived in overcrowded quarters under unsanitary conditions, the military was also at risk. In 1898, 40 soldiers of the 8th Rhenish Infantry Regiment No. 70 died in Saarbrücken from typhus spread by a team chef. He had a potato salad prepared, having previously a cesspool cleaned and then his hands had not been cleaned thoroughly enough. During the typhus epidemic in Lebach in Saarland, more than 50 people fell ill in the winter of 1902/1903.
Since it was assumed that the district doctors alone would not be able to carry out comprehensive investigations into these epidemics, the investigation commission was set up, which consisted of experts from the Reich Health Office and the Institute for Infectious Diseases in Berlin . Initially active in the Trier area, this commission was expanded in 1902. Parts of the Koblenz administrative district were examined alongside the Trier district, and a second examination station was set up in Saarbrücken. The apparatus was later expanded significantly. The main task was to examine suspicious material and to understand the path of spread of the epidemics. This work was supported by the Prussian Epidemic Protection Act of August 28, 1905, a special instruction regarding typhus from 1906 and financial support from the Reich government. In 1914 the State Institute for Hygiene and Infectious Diseases in Saarbrücken emerged from the bacteriological examination stations.
While the hygienic conditions in the cities initially gave cause for concern, at the turn of the century rural towns such as in the Lebach area came to the fore of the authorities' interest. The main focus of the medical professionals was on water and wastewater treatment in the affected areas. Medizinalrat Schlecht from Trier complained: “The number of abortions is low, defecation takes place in the cattle shed, on the fertilizer in front of the house, in the garden behind the house, in the courtyard or even in the cellar. A proper drainage pit can hardly be found; the pits are seldom emptied; the lavatory and the cesspool are often in a condition that does not permit use. ”The water supply also gave cause for complaint, since not only numerous wells were often contaminated, but also, as in the case of the Lebach typhoid epidemic, many people drinking their water - and had to take service water from open watercourses.
In the period under study between 1903 and 1914, an additional 39 hospitals, 34 of them with isolation wards, were set up and 132 disinfectants were purchased and disinfectors and community nurses trained in south-west Germany . In 1900 the district administrators were made aware that a decree existed that enabled the police to compulsorily order the construction of water pipes. In 1904 the district doctors were also obliged to make regular site visits. Finally, the decree of April 23, 1907 came into force regarding the requirements for the procurement of usable, hygienically perfect water .
But in the administrative district of Trier , for example, there was still no nationwide central water supply even after the state campaign to combat typhus; conditions improved primarily in the larger towns with more than 1000 inhabitants. Smaller towns mostly had to rely on financial support from the province or the Prussian government for the implementation. Many communities therefore had to wait for a central water supply for decades.
Tradition-conscious supporters of the old well system were also often negative about the planning of a central water supply; Others agreed in principle to have their property connected to a central water supply, but at the same time did not want to give up the use of their previous well. The case of the widow Wacht-Thiel from Söst near Saarburg , who wanted to continue to water her cattle with well water, went as far as the Royal Prussian Higher Administrative Court in Trier. Some large farmers from Berschweiler also opposed the compulsory supply of safe drinking water. They were actually able to largely defend themselves against the collection of the fees in court. The dispute over the collection of fees for the abstraction of drinking water led in some municipalities to the fact that flat-rate regulations were not lifted until the 1950s and water meters were installed in the individual houses. In Schwemlingen, for example, this did not happen until 1956.
Switzerland
There were probably several epidemics in Switzerland in the early modern period. The number of typhoid cases fluctuated considerably until 1905, after which it decreased continuously. During the Second World War, many cases of typhoid occurred again. In 1987 a person died of typhus for the last time in Switzerland. The incidence rate in 2008 was less than one per 100,000 people. In March 1963, a typhus epidemic raged in Zermatt with over 400 sick people and three dead.
Pathogen and transmission
The causative agent is the typhoid bacterium ( Salmonella enterica subsp. Enterica Serovar Typhi), a gram-negative , flagellated bacterium. It is transmitted faecal - orally , for example through contaminated food or polluted water. It is an intracellular pathogen.
During the incubation period of six to 30 days, the pathogens penetrate the intestinal wall cells, especially the cells of the Peyer's plaques, and migrate into the bloodstream via the lymphatic and reticulohistiocytic systems . Only when the pathogens have got there does the disease break out, especially with a high fever.
distribution
Nowadays, typhoid fever is mainly a problem in developing countries with inadequate hygienic conditions. Central and South America, the Caribbean, Africa and Asia are affected, especially South Asia. According to a more recent estimate from 2014, around 11.9 million people develop typhoid fever each year, and 129,000 people die.
Typhoid fever is rare in North America and Europe, with a few hundred reported annually in the United States. Of these, around 90% were brought in by long-distance travelers, the majority from India, Pakistan and Bangladesh. There are also high rates of antibiotic resistance there. Resistance or intermediate sensitivity to ciprofloxazine has been demonstrated in more than 90% of infected returning Americans . In 2016 there were 60 proven cases in Germany, 78 in 2017, 58 diseases were recorded in 2018 and the number rose to 84 in 2019.
Clinical picture
Disease stages
The incubation period is usually 1–3 weeks, depending on the amount of ingested pathogens, but extreme values can also be between 3 and 60 days.
1st week (stage incrementi): At first there are unspecific general symptoms such as fatigue, headache , constipation and a step-like rise in fever.
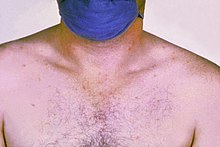
2-3 Week (stage fastigii): After approx. 8 days, a stage of persistent high fever is reached (fever continuum with 40 to 41 ° C), which can last for weeks. In some patients only the high fever is found, but more often it is accompanied by unspecific, slowly developing general symptoms. However, typical changes are less common. Possible symptoms are:
- Fatigue and exhaustion, headache, unproductive cough, general abdominal discomfort.
- Diarrhea and constipation can occasionally occur.
- Relative bradycardia , a heartbeat that is unusually slow for a fever. Otherwise, fever is often associated with a faster heartbeat (tachycardia).
- Lack of white blood cells ( leukopenia ). This is also the exception in the case of a bacterial infection. But leukocytosis , an increased concentration of white blood cells , can also occur. In addition, thrombocytopenia and anemia may be present.
- In addition, there are sometimes disorders of consciousness (hence the name)
- In rare cases, hepatomegaly (swelling of the liver) with slightly increased liver values in the laboratory (increased transaminases ) and splenomegaly (swelling of the spleen, formerly also called "spleen tumor").
- A pinkish-reddish blotchy rash ( roseoles ) on the trunk and arms and legs is rare, only visible for a short time, but typical. This typhus exanthematicus , which appeared all over Europe in the 16th century, was first described by Girolamo Fracastoro in 1546.
- Typical and rare is the so-called typhoid tongue, which is clearly gray-white in the middle, but shows free red edges on the edges and the tip of the tongue.
If the disease progresses, serious complications can occur if left untreated:
- The destruction of the Peyer's plaques in the small intestine , through which the pathogens enter the bloodstream, can lead to characteristic pea-like diarrhea , which only occurs after about 14 days, but can also be completely absent. This can cause severe pain in the kidney area and lower abdomen.
- Gastrointestinal bleeding can also be triggered by the destruction of Peyer's plaques
- Intestinal perforations can result from necrotizing lymphadenitis and have a very high mortality rate , which is why immediate surgical intervention is necessary if perforation is suspected.
Abscesses, bronchopneumonia, and meningitis can also occur.
Permanent eliminators
As a result, about 10% of untreated patients excrete typhoid bacteria in their stool or urine for up to 3 months; 5% of untreated patients become so-called permanent excretors (excretion> 1 year) of Salmonella, as the pathogens can persist in the gall bladder and biliary tract (see: Mary Mallon ). This is favored by abnormalities in the biliary tract, e.g. B. Gallstones . The permanent eliminators can infect other people without showing signs of illness themselves. Treated patients also excrete pathogens permanently (> 6 months) after surviving typhoid fever in around 2 to 5 percent of cases.
Persons suffering from or suspected of having typhus abdominalis or paratyphoid fever are not allowed to work or be employed in the production, handling or marketing of food if they come into contact with it, or in the kitchens of restaurants and other establishments with or for communal catering will.
diagnosis
The diagnosis is based on the typical clinic, the anamnesis (travel to tropical regions, especially India, Nepal and Indonesia) and laboratory and bacteriological findings.
Bacteriological pathogen detection is only possible in 40% of cases with the help of blood cultures in the first two weeks of the disease; the sensitivity is even lower with stool and urine cultures. Stool samples can only be positive in the earliest stage of the disease and after two weeks, but they have a low sensitivity.
The antibodies formed by the organism's immune system , which are directed against specific bacterial antigens (antibodies against O / h antigen), can be detected serologically from around the end of the first week of illness using the Gruber-Widal reaction . High antibody titers are only reached from the third week of the disease (1: 400–800). If antibiotics therapy is started initially, the detection of antibodies may fail. In addition, false-positive values can be found because, for example, an infection was previously present in endemic areas .
Therefore, if there is sufficient clinical suspicion, therapy must be carried out immediately and empirically even without evidence of pathogens.
treatment
The treatment of typhoid infection, to be started as early as possible, takes place with antibiotics . Before the start of therapy, blood and stool samples are taken in order to identify the pathogen and - once the pathogen has been successfully cultivated - to determine the resistance to common antibiotics. The antibiotics of choice in adults are newer quinolone antibiotics like ciprofloxacin or ofloxacin for seven to ten days. Since Salmonella Typhi is an intracellular pathogen, there is usually no immediate reduction in fever and symptom improvement; the fever can last for several days, but this does not indicate a wrong choice of antibiotics.
Alternatively, amoxicillin or cotrimoxazole can also be used for fully sensitive strains and azithromycin should be used if there is concern about resistance to quinolone antibiotics, such as those returning from India, Pakistan or Bangladesh .
If the disease is severe, intravenous antibiotics with a 3rd generation cephalosporin , e.g. B. be carried out with ceftriaxone for one to two weeks.
If the substances mentioned cannot be used due to contraindications or if the pathogens are resistant, therapy with cefixime , ampicillin , cotrimoxazole or chloramphenicol can be carried out. However, there is also often resistance to the last three active substances mentioned.
In the case of severe illness and impaired consciousness or encephalopathy , high-dose dexamethasone administration can reduce mortality.
prophylaxis
Hygiene is the best protection. This also includes frequent hand washing. The usual measures on trips to the tropics, such as avoiding insufficiently cooked food, juices, ice cubes and tap water , should be observed in any case (" cook it, peel it or leave it ") .
A vaccination prophylaxis against typhus can be carried out with both dead and live vaccines . The live vaccine (Vivotif; in Germany Typhoral) contains non-pathogenic (non-pathogenic) Salmonella Typhi bacteria, which stimulate the immune system to produce protective antibodies. The live vaccine is administered orally in enteric capsules, is well tolerated and protects around 60 percent of those vaccinated in endemic areas for at least one year. In the case of multiple travelers, a booster vaccination is recommended after one year. The inactivated vaccine contains a polysaccharide from the Salmonella Typhi capsule, which also leads to the formation of antibodies in the person being vaccinated. The vaccine is administered intramuscularly or subcutaneously , is well tolerated and offers about 60 percent of those vaccinated a protection for a maximum of three years.
Reporting requirement
In Germany, typhus is a reportable disease according to Section 6 (1) of the Infection Protection Act . You are required to report by name in the event of suspicion, illness or death.
In Austria, typhus is also a notifiable disease in accordance with Section 1 (1) of the 1950 Epidemic Act . The reporting obligation relates to suspected illnesses and deaths.
In Switzerland, typhoid is also a notifiable disease and that after the Epidemics Act (EpG) in connection with the epidemic Regulation and Annex 1 of the Regulation of EDI on the reporting of observations of communicable diseases of man . A positive laboratory analysis result is required to be reported.
literature
- Marianne Abele-Horn: Antimicrobial Therapy. Decision support for the treatment and prophylaxis of infectious diseases. With the collaboration of Werner Heinz, Hartwig Klinker, Johann Schurz and August Stich, 2nd, revised and expanded edition. Peter Wiehl, Marburg 2009, ISBN 978-3-927219-14-4 , p. 252 f.
- Karl Wurm, AM Walter: Infectious Diseases. In: Ludwig Heilmeyer (Hrsg.): Textbook of internal medicine. Springer-Verlag, Berlin / Göttingen / Heidelberg 1955; 2nd edition ibid. 1961, pp. 9-223, here: pp. 124-134.
Web links
- Typhus - information from the Robert Koch Institute
- Leaflet (PDF; 31 kB; 1 page), Federal Foreign Office
Individual evidence
- ↑ Uwe Groß: Short textbook on medical microbiology and infectiology . 3rd Edition. Georg Thieme Verlag, Stuttgart 2013, p. 64
- ↑ Karl Wurm, AM Walter: Infectious Diseases. In: Ludwig Heilmeyer (Hrsg.): Textbook of internal medicine. 1961, p. 124.
- ^ Dictionary and Lexicon Ancient Greek - Latin . Retrieved on September 12, 2011. ( Page no longer available , search in web archives )
- ↑ Manfred Vasold: The mortality in Nuremberg in the 19th century. Living circumstances, illness and death (around 1800 to 1913). In: Würzburg medical history reports. Volume 25, 2006, pp. 241-338, here: pp. 275 f.
- ↑ Typhoid . In: The word information system for the German language in the past and present
- ↑ Friedrich Kluge , Alfred Götze : Etymological dictionary of the German language . 20th ed., Ed. by Walther Mitzka , De Gruyter, Berlin / New York 1967; Reprint (“21st unchanged edition”) ibid 1975, ISBN 3-11-005709-3 , p. 799.
- ↑ International Statistical Classification of Diseases and Related Health Problems , English version
- ↑ typhoid fever: MedlinePlus Medical Encyclopedia . Retrieved September 12, 2011.
- ↑ Georg Sticker : Hippokrates: The common diseases first and third book (around the year 434-430 BC). Translated, introduced and explained from the Greek. Johann Ambrosius Barth, Leipzig 1923 (= Classics of Medicine. Volume 29); Unchanged reprint: Central antiquariat of the German Democratic Republic, Leipzig 1968, pp. 96 f. and 106.
- ↑ Horst Kremling : Historical considerations on preventive medicine. In: Würzburg medical history reports. Volume 24, 2005, pp. 222-260; here p. 230.
- ↑ Karl Wurm, AM Walter: Infectious Diseases. In: Ludwig Heilmeyer (Hrsg.): Textbook of internal medicine. 1961, p. 124.
- ↑ quoted from Hans-Henning Krämer, Vom Dorfbrunnen zum Wasserwerk. History of drinking water supply on the Saar , Gollenstein Verlag 1999, ISBN 3-933389-07-0 , p. 139
- ↑ Krämer 1999, p. 145
- ↑ Krämer 1999, p. 170
- ↑ Krämer 1999, p. 171 f.
- ↑ Krämer 1999, p. 179
- ↑ Iris Ritzmann: Typhus. In: Historical Lexicon of Switzerland . 2010 .
- ↑ Marc Tribelhorn: Deadly bacteria on the Matterhorn. In: Neue Zürcher Zeitung , March 11, 2019.
- ↑ a b c d e Maralyssa Bann, Daniel R. Kaul, Mahri Z. Haider, Sanjay Saint, Zachary D. Goldberger: Home Sweet Home . In: New England Journal of Medicine , 2018, Volume 378, Issue 5 February 1, 2018, pp. 461-466, doi: 10.1056 / NEJMcps1704731 .
- ↑ V. Mogasale, B. Maskery, RL Ochiai et al .: Burden of typhoid fever in: a systematic, literature-based update with risk-factor adjustment . Lancet Global Health 2014: Volume 2, Issue 10, Pages e570-e580
- ↑ KA Date, A. E Newton, F. Medalla: Changing patterns in enteric fever incidence and increasing antibiotic resistane of enteric fever isolates in the United States, 2008-2012 . Clinical Infectious Diseases 2016, Volume 63, Pages 322-329
- ↑ Gerd Herold : Internal Medicine . Cologne 2009, p. 808 .
- ↑ IMPP State Examination in Medicine, Spring 2007: Case Study 3.1, Question 3.48
- ↑ Walther Schönfeld : Introduction. In: Girolamo Fracastoro: Syphilidis sive morbi gallici libri tres in the translation by Ernst Alfred Seckendorf (1892–1941), introduced by Walther Schönfeld, Lipsius & Tischer, Kiel 1960 (= series of publications by the North-West German Dermatological Society. Issue 6), p. 5 –20, here: p. 6.
- ↑ Hahn, Kaufmann, Schulz, Suerbaum: Medical Microbiology and Infectiology. 6th edition. Springer Verlag, Heidelberg, 2009.
- ↑ Marianne Abele-Horn (2009), p. 252.
- ↑ Law for the prevention and control of infectious diseases in humans (Infection Protection Law - IfSG), § 42
- ↑ M. Classen, V. Diehl, K. Kochsiek (eds.): Internal medicine. 5th edition. Urban & Fischer Verlag, Munich, 2004. p. 966.
- ^ W. Caspary, M. Kist, J. Stein (Ed.): Infectiology of the gastrointestinal tract. 1st edition. Springer, Heidelberg 2006. p. 212.
- ^ E. Hohmann, S. Calderwood, E. Baron: Treatment and prevention of typhoid fever. In: UpToDate, Rose, BD (Ed), UpToDate, Waltham MA 2008.
- ^ W. Caspary, M. Kist, J. Stein (Ed.): Infectiology of the gastrointestinal tract. 1st edition. Springer, Heidelberg 2006. p. 437.
- ^ Typhoid and paratyphoid. RKI guide for doctors, as of August 2011; Retrieved June 24, 2014
- ↑ Notifiable communicable diseases and pathogens. (PDF; 114 kB) Overview of mandatory reporting in 2020. Federal Office of Public Health FOPH, Communicable Diseases Department, January 23, 2020, accessed on March 8, 2020 (Swiss Standard German, flyer with tabular overview).

