Hives
| Classification according to ICD-10 | |
|---|---|
| L50 | Urticaria |
| ICD-10 online (WHO version 2019) | |
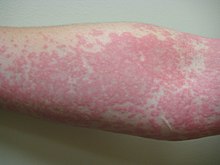
Hives or nettle rash , and urticaria ( latin urtica "nettle") is called, a pathological reaction of the skin with redness , hives and itching .
According to the course, a distinction is made between acute urticaria, which usually lasts only a few days, and a chronic form, which lasts longer than six weeks, often years.
The skin changes can be triggered in different ways. For example, they can represent a reaction to food, medication or toxins, to the effects of heat or cold , light or pressure , or to psychological stress . They can be signs of allergy , autoimmune diseases, and occur after infections . Often, however, a trigger cannot be determined ( idiopathic urticaria).
While between 10 and 25% of people experience an acute urticarial episode at least once in their life, chronic urticaria is less common, in Germany between 0.5 and 1% of the population is affected. In 2014, World Urticaria Day was proclaimed for the first time on October 1st .
overview
The disease begins with pale red to red bumps on the skin, similar to mosquito bites. The changes become larger, form wheals or erythema and itch - similar to the reaction when touching nettles ( Urtica ssp.), Hence the name. The wheals can only be a few millimeters in diameter or the size of a palm. With disseminated urticaria, large parts of the body surface are affected. A reddish reflex erythema often forms around the wheals .
Occasionally, the rash does not stay in the same place all the time but migrates across the body. He can change his position in a short time and be hardly recognizable at the place of origin. The regression usually takes 3 to 4 hours, in most cases no more appearance is visible after 12 hours.
Wheals are edematous protrusions on the dermis ; they can appear red (Urticaria rubra) , with pronounced edema also skin-colored or pale-white (Urticaria porcellanea ) . The trigger for the swelling is often the release of the messenger substance histamine from mast cells , which increases the permeability of the dermal blood vessels and thus leads to water retention in the dermis. The reasons for the release of this substance are various, only in one sixth of the cases an allergy is the cause. Rather, there are a large number of triggers and a number of possible causes:
- Auto-reactivity (endogenous substances are not tolerated; see autoimmune diseases )
- Generalized anxiety disorders (with accompanying panic attacks, after serious events, e.g. accident, death of a relative)
- Hypersensitivity to drugs or food additives (preservatives, colors and flavorings)
- chronic infections, which can be symptom-free except for urticaria (e.g. in the digestive tract)
- a histamine breakdown disorder that causes increased histamine release from mast cells
- Urticaria on pressure on the skin surface, called pressure urticaria
- Urticaria due to local exposure to heat or cold, as heat urticaria or cold urticaria
Possibly it may form a angioedema come; Swelling in the face, around the mucous membrane of the mouth and throat and on the larynx can lead to life-threatening shortness of breath. However, there are also forms of urticaria that are associated with no wheals and only painful stinging or burning of the skin.
Chronic urticaria can also have organic causes, e.g. B. Disorders in the adrenal cortex or the thyroid gland or hidden sources of inflammation in the body (e.g. in the mouth or ear, nose and throat area). A bacterium in the stomach, Helicobacter pylori , can cause hives. Other bacterial infections are also known to cause hives. Stress can make urticaria worse, but it is also discussed as a trigger.
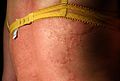
Physical urticaria
Physical urticaria are not triggered by chemical substances, but by external influences such as pressure, vibration, cold, heat or light. They belong to the pseudo- allergies , so they are not an allergy in the medical sense. Presumably due to a malfunction of the histaminergic system, the stimulus causes the release of histamine , an endogenous mediator substance , which in turn triggers the symptoms.
The individual forms are urticaria factitia or urticarial Dermographism (hives in the pattern of a mechanical action as, after scratching Press, painting or writing on the skin), heat urticaria , Sonnenurtikaria , Vibrationsurtikaria and the relatively frequent cold urticaria - colloquially also often referred to as "allergy to cold".
In some forms of the metabolic disorder erythropoietic protoporphyria (EPP), contact with (sunlight) light triggers an urticaria-like reaction (EPP of the urticaria type).
Other forms
Less common forms are cholinergic urticaria and adrenergic urticaria , whereby the terms express that activation of the autonomic nervous system (by acetylcholine or adrenaline ) plays a role. They can be triggered by psychological stimuli or primary organic diseases, for example of the thyroid gland (e.g. Hashimoto's thyroiditis ). Another form is the extremely rare aquagenic urticaria , in which itchy wheals and reddening of the skin are triggered even on contact with distilled water . There are only individual case descriptions in the literature. The pathomechanism of this disorder is still unknown; Speculations assume that soluble substances in the skin are washed into the pores with the water. As with the physical triggers, it is also incorrect here to speak of an allergy or even “water allergy”.
Treatment options
In acute urticaria, the therapy depends on the severity of the symptoms. The standard therapy is the administration of antihistamines , in the case of very severe disease treatment with intravenous cortisone in the hospital may be necessary.
For the treatment of chronic urticaria, according to the currently valid guidelines, a three-step procedure is recommended depending on the therapeutic response: First a modern antihistamine in standard dosage; If symptoms persist, the antihistamine is increased in the second stage up to four times the daily dose and, if symptoms persist, additional therapy with omalizumab , ciclosporin A or montelukast follows in the third stage . The only therapies approved for chronic urticaria are antihistamines in standard doses and, if this is insufficient, omalizumab.
Demarcation
Urticaria vasculitis is often confused with urticaria or hives . However, this is not a disease of the skin, but of the blood vessels. Both conditions cause itching, wheals, redness or swelling of the skin. H1 antihistamines, montelukast, danazol, H2 antihistamines, pentoxifylline, doxepin or tranexamic compounds prescribed for hives do not work in urticaria vasculitis - but cortisone, biologics and immunosuppressants.
Illustrations
literature
- S3- guideline urticaria, classification, diagnosis and therapy of the German Dermatological Society and the German Society for Allergology and Clinical Immunology. In: AWMF online (as of 2011)
Web links
- Website Urtikaria.net
- allum.de (allergy, environment and health): hives
Individual evidence
- ^ A b c Marcus Maurer, Jürgen Grabbe: Urticaria - specific anamnesis and cause-oriented therapy. In: Deutsches Ärzteblatt . Vol. 105, 2008, pp. 458-466, doi: 10.3238 / arztebl.2008.0458 .
- ↑ K. Weller, S. Altrichter, E. Ardelean, K. Krause, M. Magerl: Chronic Urticaria . In: The dermatologist . tape 61 , no. 9 , September 1, 2010, ISSN 0017-8470 , p. 750-757 , doi : 10.1007 / s00105-010-1933-8 .
- ↑ nesselsuchtinfo.de
- ^ Peter Fritsch: Dermatology and Venereology for Studies. Springer Medicine, Heidelberg 2009, ISBN 978-3-540-79302-1 .
- ↑ ECARF's allergy portal on the causes of urticaria accessed on February 3, 2018
- ↑ Bettina Wedi, Alexander Kapp: Evidence-based therapy of chronic urticaria. In: Journal of the German Dermatological Society . Vol. 5, No. 2, 2007, pp. 146-155, doi : 10.1111 / j.1610-0387.2007.06074_supp.x .
- ↑ Urtikaria.net ( Memento of the original from March 25, 2010 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice.
- ↑ Urticaria - Endless Suffering?
- ↑ Urticaria acute - P.Altmeyer - Encyclopedia of Dermatology, Venereology, Allergology, Environmental Medicine. Retrieved June 15, 2017 .
- ↑ a b Christian Termeer, Petra Staubach, Hjalmar Kurzen, Klaus Strömer, Rolf Ostendorf: Chronic spontaneous urticaria - a treatment path for diagnosis and therapy in practice . In: JDDG: Journal of the German Dermatological Society . tape 13 , no. 5 , May 1, 2015, ISSN 1610-0387 , p. 419-429 , doi : 10.1111 / ddg.12633_suppl .
- ↑ T. Zuberbier, W. Aberer, R. Asero, C. Bindslev-Jensen, Z. Brzoza: The EAACI / GA2LEN / EDF / WAO Guideline for the definition, classification, diagnosis, and management of urticaria: the 2013 revision and update . In: Allergy . tape 69 , no. 7 , July 1, 2014, ISSN 1398-9995 , p. 868-887 , doi : 10.1111 / all.12313 .
- ↑ P. Kolkhir, M. Grakhova u. a .: Treatment of urticarial vasculitis: A systematic review. In: The Journal of allergy and clinical immunology. [electronic publication before printing] September 2018, doi : 10.1016 / j.jaci.2018.09.007 , PMID 30268388 .