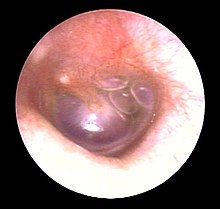
Timpani effusion
| Classification according to ICD-10 | |
|---|---|
| H65.0 | Acute serous otitis media |
| H65.1 | Other acute non- purulent otitis media |
| H65.2 | Chronic serous otitis media |
| H65.3 | Chronic mucous otitis media |
| ICD-10 online (WHO version 2019) | |
The effusion ( Engl. Secretory otitis media or serous otitis media ) is an accumulation of fluid in the tympanum - the part of the middle ear , where the ear drum ( lat. - Anat. Tympanic membrane ) is located.
The consistency of such an effusion, here: secretion , ranges from serous (= thinly fluid, watery; serotympanum ) to mucous (= viscous, slimy ; mucotympanum ) to glue-like (so-called glue ear , for example: 'sticky ear'). The time course can range from acute - especially in the context of a flu-like infection or after considerable pressure fluctuations ( tubular catarrh , barotrauma ) - to chronic dysfunction of the eustachian tube (e.g. due to tissue growth in the nasopharynx or in the nasal cavity ) vary.
causes
- Adenoids - the most common cause in children
- Rhinitis
- Sinusitis
- Nasal polyp
- Down syndrome , cleft lip and palate
- chronic obstructive tube ventilation disorder
- Mass in the nasopharynx such as nasopharyngeal carcinoma
- Metabolic disease with secretion disorders of the middle ear mucosa (rare)
Emergence
A middle ear catarrh and the resulting malfunction of the Eustachi tube form a thin (serous) secretion , which hinders the pressure equalization in the middle ear. The mucous membrane in the middle ear absorbs part of the secretion; a negative pressure builds up when the eardrum is intact. This can be recognized by the retraction of the eardrum. With the transition to a chronic form, the secretion becomes slimy (mucous), as the mucous membrane is transformed into a columnar epithelium with goblet cells that produce mucus due to the chronic negative pressure . Inflammatory episodes can lead to discoloration of the secretion (e.g. pus, bleeding). Eventually, overpressure can build up in the middle ear.
Symptoms
The symptoms usually occur with an infection and then persist.
- Hearing loss ( conductive hearing loss ) and a resulting speech delay in children
- Sensation of pressure and fullness in the ear
- Pain and dizziness
examination
- The ENT doctor will first use the otoscopy to get an idea of the condition of the middle ear. Based on the curvature of the eardrum, an initial statement about the pressure conditions is possible. The accumulation of fluid behind the eardrum is clearly visible. If the secretion is bloody, the liquid appears bluish shimmering ("blue drum").
- By measuring the mobility of the eardrum ( tympanometry ), the pressure conditions in the middle ear can be determined and the fluid accumulation behind the eardrum can be better assessed. If the tympanic cavity is completely filled, the eardrum can hardly vibrate (very high damping). This examination cannot be carried out in the case of a perforated eardrum.
- A hearing test shows the presence of conductive hearing loss .
- By mirroring the nasopharynx , enlarged tonsils may be found.
therapy
Acute tubular catarrh usually heals in two to three weeks. The chronic seromucotympanum can last for months or years.
The treatment depends on the cause of the tympanic effusion:
- Improvement or restoration of ventilation: use of decongestant nasal drops (not suitable as long-term therapy)
- Blasting the tube with a Politzerball
- Physiotherapy: inhalation therapy, steam baths, heat treatment, nasal rinsing
- Taking medication to liquefy secretions, e.g. B. Enzyme therapy with bromelain , papain
- A bacterial infection is treated with antibiotics
- If necessary, administration of painkillers
- Surgical removal of the enlarged pharynx : adenotomy (often incorrectly called polyp removal)
- Incision in the eardrum ( paracentesis ) and suction of the secretion
- Insertion of a ventilation tube into the eardrum in the case of chronic ventilation problems
- endoscopic balloon catheterization of the nasopharyngeal tube ostium
Complications
- Delayed speech development in children (due to prolonged hearing loss)
- Scarring or calcification of the lining of the middle ear
- Adhesion or destruction of the ossicles
- Spread of inflammation to neighboring structures, e.g. B. Labyrinthitis ( inflammation of the inner ear), meningitis (inflammation of the meninges), mastoiditis (inflammation in the mastoid process)
- Formation of atrophic retraction pockets of the eardrum with the risk of a later developing cholesteatoma
literature
Guidelines
- S2k guideline Seromukotympanum of the German Society for Ear, Nose and Throat Medicine, Head and Neck Surgery. In: AWMF online (as of 2018)