Echocardiography
Echocardiography or ultrasound cardiography (UKG) is the name given to the examination of the heart using ultrasound (see also sonography ).
In addition to the electrocardiogram (ECG), echocardiography is one of the most important technical non-invasive examination methods of the heart and an indispensable part of cardiological diagnostics. Echocardiography is also a valuable part of diagnostics for general practitioners and intensive care practitioners.
TTE
In TTE, or transthoracic echocardiography , the heart is first examined by placing the ultrasound head on the chest, parasternally, i.e. from an area next to the breastbone , and apically, i.e. from the apex of the heart. In the parasternal transducer position (usually above the third to fifth left intercostal space ), the longitudinal and transverse axes of the heart can be seen; in the apical one (usually above the seventh to ninth intercostal space in the anterior axillary line ) one obtains, among other things, a two-chamber view and four-chamber view of the heart cavities . The heart is also located subcostal , where the ultrasound beam first passes through the liver and shows, for example, the width of the hepatic veins before it joins the inferior vena cava before it joins the right atrium, as well as suprasternal . The acronym "echo" usually means transthoracic echocardiography.
The following can be examined in detail with the various techniques:
- With the 2-D image , you can watch the heart function in real time using a black and white sectional image . In particular, the size of the heart chambers, the valve function and the pumping function of the heart can be easily identified and, for example, the ejection fraction can be determined. The ascending aorta and the aortic arc can also be assessed in the parasternal longitudinal section and in the suprasternal section , e.g. For example with the question of an aortic dissection .
Aortic valve ( diastole ) in parasternal short axis
Left ventricle in HOCM in parasternal short axis
- With the M-mode , the aortic valve , the function of the left ventricle and the mitral valve are examined from the parasternal side .
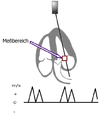
- The PW and CW Doppler are usually used to measure the blood flow velocity apically, especially in the valves, in order to quantify valve stenoses , but also to determine pulmonary artery pressure or to assess the diastolic function of the left ventricle.
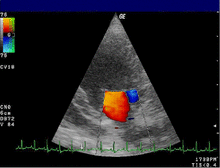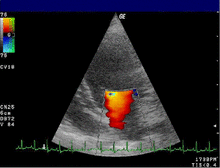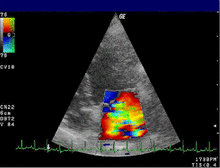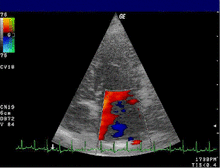
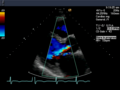
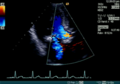
- The color Doppler helps to localize and quantify valve insufficiency and stenosis. In another device setting, the color Doppler is optimized for tissue and shows the movement of the heart wall. Applications of the tissue Doppler are the subject of research.
Tissue Doppler in the myocardium
TEA
The ultrasound examination of the heart introduced in 1976 by Leon J. Frazin from the esophagus (transesophageal echocardiography, TEE for short [derived from the American term transesophageal echocardiography, also called TOE]), is less necessary, especially in intensive care patients ventilated with PEEP . For this purpose, a tube with an ultrasound probe is inserted into the esophagus at the end of this tube. Adult patients are able to swallow the tube, hence the colloquial term "swallowing echo". In children and adolescents, it is usually necessary to carry out the examination under short anesthesia ( sedation ). Transesophageal echocardiography provides a better representation of certain parts of the heart and the thoracic aorta due to the close positional relationship between the esophagus and the heart . In addition, small thrombi , especially in the auricle of the left atrium , are better detected. This form of echocardiography may also be necessary in very obese patients if a transthoracic echo does not provide satisfactory imaging. As a rule, the tip of this tube, in which the ultrasound head, which works according to the piezoelectric effect, is located, is movable via small wheels on the "head" of the tube - similar to the structure of an endoscope - and can rotate around its own axis all possible sectional planes - ultrasound diagnostics generally belong to the sectional imaging method - of the heart. The fact that the left atrium and the esophagus (esophagus) have a close anatomical relationship is the rationale for a good assessment of important parts of the heart from transesophageally, for example if the transthoracic plumbing of the heart is not successful due to pulmonary emphysema.
Stress echocardiography
The " stress echo " ( stress echocardiography ) is an echocardiography that is performed under stress. The most common indication for a stress echo is suspected circulatory disorders in coronary artery disease .
There are two ways of exertion: In the case of a mechanical stress echo, the patient is lying on his left side on a bicycle ergometer. The patient steps on the pedals against a slowly increasing resistance while the doctor performs the ultrasound scan of the heart. In the event of a medicinal stress echo, however, the patient is given a drug (usually dobutamine or dipyridamole with atropine or adenosine ) intravenously.
Regardless of the type of stress, the examination is carried out in several stress levels. First, images of the left ventricle are taken at rest. The load is then increased over several stages until a termination criterion is met. Cancellation criteria are the achievement of the target heart rate , patient complaints about chest pain or the visibility of a wall movement disorder in the ultrasound. If the patient complains of chest pain or if a wall movement disorder is seen, then this reinforces the suspicion of coronary artery disease.
Specifically, an akinesia , hypokinesia , dyskinesia , hyperkinesia, asynergy, asynchrony or normokinesia (normal contraction) can be seen in the ultrasound image of contraction forms. In moderate stenoses of the coronary arteries , the stress usually triggers akinesia or hypokinesia. In severe stenoses, in which the wall is akinetic at rest because it suffers from hibernation , the load causes a temporary hypokinetic wall movement.
Technically, the systoles are usually recorded from four perspectives (apical 4-chamber view, apical 2-chamber view, parasternal long axis, parasternal short axis) in four different load levels. In a special view, the four stress levels of a glance are played synchronously side by side. This should make it easier to find changes in wall movement.
If the image quality is not optimal, recommends the European Society of Cardiology , ultrasound contrast agents use to the heart wall to better define. The presentation of myocardial perfusion with the same contrast media is the subject of research.
Opinions of echocardiography
Echocardiography allows a non-invasive, patient-friendly examination of the heart within a short period of time. The size of the individual heart chambers and atria, the pump function and the function of the individual heart valves can be easily assessed. Echocardiography is the basic imaging method in the diagnosis and follow-up of congenital heart defects . With echocardiography, heart defects in a child can be recorded in the womb.
The critical gap in echocardiography is the assessment of the coronary arteries. Due to their size and location, these can be assessed poorly or only indirectly through possible wall movement disorders. Since the ultrasound is almost completely reflected at the transition between media with a high density difference (e.g. muscle to bone or air), it cannot pass through the ribs or ventilated lungs in TTE, or through the left main bronchus to the aorta in TEE ascendens are "sounded".
Targeted use in an emergency (FEEL)
For emergency situations such as cardiac arrest or near cardiac arrest, extensive echocardiography cannot be performed due to lack of time and unfavorable conditions. The concept of Focused Echocardiographic Evaluation in Life Support (FEEL) therefore provides for the shortest possible targeted echocardiography in an emergency, which can be learned comparatively quickly and can therefore also be made available to doctors without cardiac specialization. The feel concept envisages being able to view all four heart cavities at the same time via a flat echocardiographic access under the ribs. Certain clinical pictures should then be recognized with the eye within a few seconds (with resuscitation a maximum of 10 seconds). The important clinical pictures that are important in the FEEL concept include:
Pseudopulsive electrical activity (PEA)
In the moving ultrasound image, it can be observed whether an electrical heart action in the EKG is also followed by a muscle response of the heart. If the muscle response is missing, one speaks of real pulseless electrical activity . If one sees muscle movements without feeling a pulse in the carotid artery at the same time, one speaks of pseudo- pulse-free electrical activity.
Dehydration
If there is a lack of fluid in the blood vessels, it can be observed how the heart cavities collapse so far during pumping that the walls touch (kissing trabecular muscles). Furthermore, if there is a lack of fluid, the superior vena cava , which leads directly to the right atrium , is usually narrowed (less than 15 mm).
Pericardium effusion
Too much fluid in the pericardium shows up as a black ( hypoechoic ) border around the heart cavities on ultrasound . In particular , if a pericardial effusion develops quickly, the heart can be life-threateningly compressed, so that it may be necessary to drain the effusion immediately with a hollow needle. On the other hand, larger amounts in the pericardium can be harmless as long as the fluid is created slowly and the pericardium can slowly expand.
Pulmonary embolism
In pulmonary embolism, the arteries leading from the heart to the lungs are blocked, which leads to a backlog of blood in front of the heart, which is noticeable in the ultrasound with enlarged right heart cavities. The heart valve between the right heart cavities is overcome by the back pressure in severe pulmonary embolism, so that blood can flow backwards, which can also be made visible in the ultrasound. Furthermore, the normally curved septum between the right and left halves of the heart is flattened. The heart septum is pressed towards the left heart because of the back pressure in the heart filling phase (paradoxical septum movement). In some cases, the blocked blood clots may even be visible as a fluttering foreign body. A life-threatening pulmonary embolism can be treated with thrombolytic medication if the pulmonary embolism is detected early enough, for example by ultrasound.
Pumping weakness of the left heart
If, for example, the heart is pumping weak due to a heart attack, this can be seen in the moving ultrasound image, as the left ventricle is no longer sufficiently emptied and too much blood remains in the ventricle. Usually this ejection fraction is determined by complex mathematical calculations. The ejection fraction can, however, also be estimated by the experienced examiner with the naked eye ( eye-balling ).
Collapsed Lung (Pneumothorax)
If the lungs collapse, the heart can be threateningly compressed ( tension pneumothorax ). With the ultrasound, the lungs and the lungs that normally slide over them can be visualized through the intercostal spaces (lung slide). The presence of a lung collapse can thus be determined or excluded with great certainty, even without X-raying the patient. In the case of tension pneumothorax, the excess pressure in the chest must be relieved through a hollow needle.
See also
- Intravascular / intravascular ultrasound examination ( IVUS ): In percutaneous transluminal angioplasty (PTA), a small ultrasound probe is also inserted into the artery, with which the change in the wall can be measured.
- Intracardiac Echocardiography ( ICE )
- Fetal echocardiography
literature
- Thomas Böhmeke: Checklist echocardiography. 3rd, revised and expanded edition. Thieme, Stuttgart et al. 2001, ISBN 3-13-129403-5 .
- Ekkehart Koehler, Mira-Christine Tataru: Clinical echocardiography. Textbook and video atlas. 5th, revised and expanded edition. Enke in Georg-Thieme-Verlag, Stuttgart et al. 2001, ISBN 3-13-124995-1 .
- Matthias Kunert , Ludger J. Ulbricht: Practical echocardiography. 2nd, completely revised and expanded edition. Deutscher Ärzte-Verlag, Cologne 2006, ISBN 3-7691-1210-5 .
- Stefan Pfleger, Franz Metzger, Karl K. Haase (Ed.): Compendium Echokardiographie. Guide to basic, advanced and advanced training. Wissenschaftliche Verlags-Gesellschaft, Stuttgart 2003, ISBN 3-8047-1964-3 .
Web links
- Echobasics - Guide to Echocardiography
- echocardia.com - echocardiography video and image database
- Quality guidelines in echocardiography
- Medlibrary
- Echocardiographic video clips
- Abbreviations and explanations Echocardiography (State Education Server Baden-Württemberg, archived version)
- VIRTUAL TEE - self-study and teaching - resource
- VIRTUAL Transthoracic Echocardiography - self-study and teaching - resource
- CT2TEE - transesophageal echocardiography simulator
Individual evidence
- ↑ Amitava Majumder, Anne Paschen: Medical working techniques. In: Jörg Braun, Roland Preuss (Ed.): Clinic Guide Intensive Care Medicine. 9th edition. Elsevier, Munich 2016, ISBN 978-3-437-23763-8 , pp. 29–93, here: pp. 85–89 ( echocardiography ).
- ↑ D. Scheidegger: Definition and parameters of acute respiratory insufficiency: pulmonary circulation, cardiac function. In: J. Kilian, H. Benzer, FW Ahnefeld (ed.): Basic principles of ventilation. Springer, Berlin a. a. 1991, ISBN 3-540-53078-9 , 2nd, unchanged edition, ibid. 1994, ISBN 3-540-57904-4 , pp. 109-120; here: p. 118 f.
- ↑ Reinhard Larsen: Anesthesia and intensive medicine in cardiac, thoracic and vascular surgery. (1st edition 1986) 5th edition. Springer, Berlin / Heidelberg / New York et al. 1999, ISBN 3-540-65024-5 , p. 173 f.
- ↑ Eugenio Picano: Stress Echocardiography . 4th edition. Springer, Berlin 2003, ISBN 3-540-00162-X (English).
- ↑ Rosa Sicari, et al .: Stress echocardiography expert consensus statement: European Association of Echocardiography (EAE) (a registered branch of the ESC) . In: European Journal of Echocardiography . tape 9 , 2008, p. 415–437 , doi : 10.1093 / ejechocard / jen175 (English, escardio.org [PDF; accessed on January 31, 2017]).
- ↑ M. Campo dell Orto, C. Hamm, A. Rolf, T. Dill, FH Seeger, F. Walcher, R. Breitkreutz: Echocardiography as a guide in peri-resuscitation . In: The cardiologist . tape 4 , no. 5 , October 2010, p. 407-424 , doi : 10.1007 / s12181-010-0289-8 .
- ↑ https://www.degum.de/fileadmin/dokumente/arbeitskreise/fetale-echokardiographie/literatur/9_US_Vier-Kammerblick.pdf