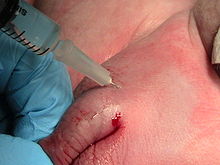
Regional anesthesia
The regional anesthesia called umbrella term a number of anesthesia methods that have a pain elimination of certain areas of the body to the target without affecting consciousness. These regional anesthesia procedures, through the targeted application of anesthetics , mostly local anesthetics , cause the temporary, reversible functional inhibition of nerves and lead to insensitivity and freedom from pain, and sometimes also to inhibition of active mobility in parts of the body. Such “ partial anesthesia ” is carried out as a single injection or by placing a pain catheter, which can be used to continue effective pain therapy even after the operation. The combination of regional and general anesthesia (general anesthesia ) is known as combination anesthesia .
Systematics
For historical and pharmacological reasons, the term regional anesthesia is mostly subordinate to local anesthesia . The nomenclature of the classification is not uniform, however, sometimes the regional anesthesia is carried out separately. A distinction is made between peripheral, spinal cord, intravenous and infiltrating regional anesthesia.
Conduction anesthesia
As nerve blocks is called method by the injection of anesthetics in the immediate proximity of nerves which transmission of pain impulses in the afferent nerve fibers inhibit. These are further divided into peripheral and spinal cord-related procedures.
Peripheral regional anesthesia procedures
In peripheral regional anesthesia procedures , the targeted blockade of individual nerves or nerve plexuses that supply a specific area of the body is called. These are located with the aid of technology based on anatomical landmarks, a nerve stimulator or under ultrasound control and anesthetized by injecting a local anesthetic through a cannula. The ultrasound-controlled technology, which has been established as the standard for several years, can reduce the failure rates of blockages, extend the duration of action and reduce the risk of injuring a blood vessel. Frequent procedures are blockages of the brachial plexus on the arm (upper extremity) ( interscalene blockade , infraclavicular plexus blockade , axillary blockade ) as well as blockages of individual nerves of the arm or the fingers ( Oberst block ). On the leg, blockages of the lumbar plexus ( psoas compartment blockade , blockages of the femoral nerve , blockages of the obturator nerve ) and the sacral plexus ( sciatic nerve blockages ) are used in addition to the blockade of individual nerves (foot block, etc.). In ophthalmology , peri- and retrobulbar anesthesia, especially in intraocular interventions , are common, sometimes in combination with a so-called facial block for temporary paralysis of the orbicularis oculi muscle . Circuit anesthesia is most commonly used in dentistry , mostly to block the mandibular nerve , but also other peripheral nerves.
In order to effectively numb the nerve or the nerve bundle, it is necessary to inject the anesthetic as close as possible to the nerve with the tip of the needle so that it can spread around the nerve. The needle must not cause internal injuries such as the lungs and the needle tip should not get into blood vessels in order to avoid life-threatening poisoning (systemic local anesthetic toxicity ). The needle must not come too close to the nerve in order to avoid injection into the nerve and the associated nerve damage. According to the guideline of the German Society for Anesthesia and Intensive Care Medicine, ultrasound or nerve stimulation or both at the same time can be used to locate the nerves. When using ultrasound, it should always be possible to reliably represent the position of the needle tip. To make this easier, needles are available that are better represented in the ultrasound image thanks to a roughened or notched surface. If the nerve is visited with electrical nerve stimulation, current pulses with 2 Hz, 0.1 ms pulse width and a current strength of 2.0 to 0.5 mA should be used so that the needle tip near the nerve can trigger muscle activity. If muscle activity can be triggered below 0.5 mA, the needle may be too close to the nerve, so that the needle tip should be withdrawn a little. In the case of purely sensitive nerves, a wider impulse (1.0 ms) should be used to get a sensitive reaction. Likewise, diabetes, polyneuropathy or renal insufficiency can reduce the excitability of nerves. Either the pulse width can then be increased to 1.0 ms or the current intensity can be increased.
Regional anesthesia procedures close to the spinal cord
When neuraxial , central or neuroaxial regional anesthesia procedures (the Austrian, particularly in obstetrics, including cross stitch called) spinal anesthesia and epidural (synonym epidural ) are summarized. In these, the local anesthetics act on the nerve roots that extend from the spinal cord. In spinal anesthesia, the liquor space is punctured at the level of the lumbar spine and the injection of the medication causes a rapid, complete anesthesia of the lower half of the body. Usually a single injection is given. With epidural anesthesia, on the other hand, the catheter, which is usually inserted, comes to rest in the epidural space , so that the local anesthetic mainly acts on the spinal nerves extending from the spinal cord outside the meninges. While in spinal anesthesia all the nerve fibers below the puncture site and thereby the entire lower half of the body are numbed through the distribution of the medication, in epidural anesthesia the anesthesia is emphasized in the puncture height. The combined spinal and epidural anesthesia combines both procedures, whereby the rapid and complete onset of action of the spinal anesthesia interacts with the long-lasting effectiveness of the epidural catheter.
Intravenous regional anesthesia
In the case of intravenous regional anesthesia after beer , on the other hand, the local anesthetics are not injected into the vicinity of nerves, but into previously emptied veins of a previously tied limb, usually the arm. From there, the active ingredients diffuse into the sensitive nerve endings and nerve tracts.
Infiltration anesthesia
In infiltration anesthesia, the local anesthetic is infiltrated into the tissue of the target area to be anesthetized. Infiltration anesthesia is often used in dentistry for all interventions that do not involve central anesthesia. To reduce toxicity (by delaying resorption ) and to extend the duration of action, a local anesthetic is used to which a vasoconstrictor ( adrenaline , noradrenaline ) is added in small doses.
history
As the first regional anesthesia method , August Bier (1861–1949) introduced spinal anesthesia in 1898 and intravenous regional anesthesia in 1908. 1901 published Cathelin. and Sicard. independent first experiences with epidural anesthesia.
application areas
Regional anesthetic procedures have been increasingly used in recent years. Above all, the very good effectiveness against postoperative pain in relation to low side effects and the resulting shorter length of stay in the recovery room and possibly in the hospital in general speak in favor of this procedure. In addition, there is less stress on the cardiovascular system and therefore also less morbidity .
Regional anesthetic procedures are often performed for:
- Dental treatments
- Operations on the extremities, shoulder and hip joint
- Operations on the lower abdomen
- Interventions in obstetrics and gynecology
- Vascular surgery (carotid artery)
- Urological interventions ( prostate , bladder , genital organs )
- Post-operative pain management
- Patients with chronic analgesic use / drug abuse
- Fast track surgery
The procedures may not be used for:
- Rejection by the patient
- non-cooperative patient
- Infection in the puncture area or distal to it
- Allergy to the local anesthetic
- Allergy to additional components of the local anesthetic (e.g. preservatives )
- Intolerance to vasoconstrictors with certain LA combination products
- shock
- sepsis
- Immunosuppression
- Coagulation disorder or therapeutic anticoagulation
See also
Individual evidence
- ↑ a b H. A. Adams, E. Kochs, C. Krier: Today's anesthesia methods - attempting a system. In: Anästhesiol Intensivmed Emergency Med Schmerzther. 36, 2001, pp. 262-267. doi: 10.1055 / s-2001-14470 , PMID 11413694 .
- ↑ P. Marhofer, M. Greher, S. Kapral: Ultrasound guidance in regional anesthesia. In: Br J Anaesth. 94 (1), Jan 2005, pp. 7-17. Epub 2004 Jul 26th Review. PMID 15277302
- ↑ MS Abrahams, MF Aziz, RF Fu, JL Horn: Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block: a systematic review and meta-analysis of randomized controlled trials. In: Br J Anaesth. 102 (3), Mar 2009, pp. 408-417. Review. PMID 19174373
- ↑ Volker Hessemer: Peribulbar anesthesia versus retrobulbar anesthesia with facial block - techniques, local anesthetics and additives, akinesia and sensitive blocks, complications. Thieme eJournal. In: Clinical Monthly Ophthalmology. 204 (2), 1994, pp. 75-89, doi: 10.1055 / s-2008-1035503 .
- ↑ S1 guideline recommendation: Thorsten Steinfeldt: nerve localization for peripheral regional anesthesia. In: Anaesthesiology and Intensive Care Medicine. 12, 2013, pp. 662-666.
- ↑ A. Bier: Experiments on the cocainization of the spinal cord. In: Dtsch Z Chir. 51, 1899, pp. 361-368.
- ↑ A. Bier: About a new way of producing local anesthesia on the limbs. In: Arch. Klin. Chir. 86, 1908, pp. 1007-1016.
- ↑ R. Schäfer, P. Söding: Clinical Guide Anesthesia. Urban & Fischer, Munich 2010.