Tear ducts
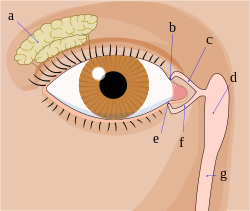
As tear ducts (Latin Viae lacrimales ) the anatomical structures of be lacrimal system referred to the derivative of the tear glands formed tear fluid for the nose are used. The tear ducts include the two tear points and tear ducts, the tear sac and the tear and nasal duct.
With normal tear production, the tear ducts drain the tear fluid into the nose, where it evaporates. Only with increased tear production or disruption of the drainage system does the tear fluid overflow over the edge of the eyelid , which is known as epiphora (Greek for "trickling tears").
Structure and functionality in humans
Skinny tear-way passage
The tear fluid is distributed over the cornea with the blink of an eye and keeps it moist. It is then derived from the conjunctival sac with the lacrimal lake ( Lacus lacrimalis ) through two punctiform openings on the corner of the eyelid on the nasal side, the upper and lower lacrimal point ( puncta lacrimalia ) . The tear points are equipped with a sphincter muscle that can close the opening of the tear points (0.34-0.64 mm).
A lacrimal tubule ( canaliculus lacrimalis ) leads from each of these points vertically 1.5–2 mm and then bends in a pointed arc into the 6–8 mm long horizontal part. As a rule, the upper and lower lacrimal tubules then unite to form a common horizontal lacrimal tubule ( ductus lacrimalis communis ), which is considered to be part of the lacrimal sac ( saccus lacrimalis ) and into which it opens. The tear sac is also located in the eye socket, on the lower part of the eye in a shallow pit ( fossa sacci lacrimalis ) in the tear bone ( os lacrimale ). In humans, it measures 12 mm vertically and about 4 mm horizontally and has an average volume of 20 µl. The slack and sagging skin of the lower eyelids is also popularly referred to as "bags under the eyes " ( dermatochalasis ), possibly in combination with eyelid swelling due to the fat tissue bulging into the eyelids. These have no relation to the tear system.
The eye ring muscle ( orbicularis oculi muscle ) can, mediated by a sinewy structure (eyelid ligament), compress the lacrimal sac and thereby generate a negative or positive pressure that sucks in the tear fluid or forwards it into the tear and nasal duct ( ductus nasolacrimalis ). The nasal tear duct is surrounded on all sides by bony structures and in humans it opens into the lower nasal passage after a maximum of 5 mm . The mouth of the tear-nasal duct behaves very differently when compared to animal species. Even within a species, the mouth can be in the middle of the lower nasal passage or first in the nasal vestibule, as in dogs. In the nose, the tear fluid serves to moisten the nasal mucosa and evaporates. A valve mechanism ( Hasner fold or flap ) prevents the tears from flowing back .
The membranous tear duct has a multitude of constrictions, folds and bays. The following structures are passed from top to bottom:
- Bochdalek fold
- Rosenmüller fold
- Arlt -sine
- Kraus or Berault fold
- Spiral fold according to Hyrtl
- Taillefer flap
- Hasner fold ( Plica lacrimalis ): Mucosal fold at the mouth of the lacrimal and nasal duct
The lacrimal tubules are lined with a multilayered squamous epithelium , the other lacrimal ducts with a multilayered columnar epithelium. Underneath is loose connective tissue in which an extensive venous network ( plexus ) is embedded. The pulsation of the blood vessels supports the drainage of tears.
Bony supporting skeleton of the tear ducts
The upper part of the bony lacrimal passage has its origin in the lacrimal pit ( Fossa sacci lacrimalis ), which is bounded to the front and back by a bony edge ( Crista lacrimalis ) of the tear bone ( Os lacrimale ). In the upper part they are adjacent to the ethmoid cells , in the lower part the middle nasal passage. The lacrimal canal joins down, the borders of which are formed on the side by a groove in the maxillary bone ( sulcus lacrimalis maxillae ) and on the nasal side by a protrusion of the nasal bone ( processus lacrimalis des os conchale ). The rear wall is formed in the lateral part by part of the maxillary bone and towards the nose by the middle nasal passage. The tear duct opens into the lower nasal passage.
Since the human facial skull can have a very variable shape, the dimensions of the bony passage also vary. The length of the tear pit is about 16 mm and 5–6 mm wide, the canal is between 12.4 and 15 mm long. It runs at an angle of 15-25 ° to the “back and to the side” downwards, so that the channels on both sides deviate from each other.
Development history
The tear trough can be detected from an embryo length of about 8 mm. It is located on the lateral nasal process and acts as a growth bar for the membranous tear ducts. These initially grow into the mesenchyme as solid epithelial strands .
At the rear end, two hollow cords sprout in the direction of the corner of the eyelid on the nasal side. Their adhesions with the eyelid margin epithelium represent the tear points. The distal part sprouts into the lower nasal passage. From the 3rd month the hollowing out of these solid strands begins, so that by the 5th – 6th Month of development both the tear points and access to the nose is opened. The latter step is absent in around 70% of cases until the time of birth (see congenital stenosis ).
Tear ducts in animals
The anatomical structures of the tear ducts of mammals are basically constructed in a similar way. However, there are also deviations: In some mammals (e.g. rabbits) only one tear point is formed on each side. In elephants and seals these are completely absent.
Investigation techniques
In the dye test , a dye is placed in the conjunctival sac. If the tear ducts function normally, the dye should be removed after a short time (approx. 5 minutes) and no longer be found in the conjunctival sac. The Jones test also involves putting a dye in the conjunctival sac. The test is said to be negative if no dye is found in the duct in the nose. This is an indication of the imperviousness of the tear ducts.
During the tear duct probing and irrigation , the tear ducts are examined with a special blunt tear duct cannula for passability and finally flushability. The bony portion of the tear duct can only be examined in this way in an anesthetized patient.
Of the imaging methods , the X-ray examinations with contrast media (dacryocystography, DCG ), possibly with digital subtraction technology, and computed tomography (CT dacryocystography) are of particular importance. Magnetic resonance tomography , scintigraphy , ultrasound examination and endoscopy can also be used for diagnosis in special cases.
Diseases and dysfunction
Overproduction of tear fluid
Only when there is an excess of tear production (for example due to inflammation of the conjunctiva or, in humans, also due to emotional factors), the transport capacity of this drainage system is insufficient and the tear lake runs over the edge of the eyelid, then the tears "roll" over the face. At the same time, there is also an increased volume of fluid in the nasal cavity (the nose drips).
Misalignment of the eyelids
If the eyelids are incorrectly positioned outwards ( ectropion ), the teardrop spots no longer submerge in the tear lake. As a result, the tear fluid cannot get into the tear ducts and tears appear. Surgical correction of the lid malposition is necessary in these cases.
Constipation and constriction
Even in the case of congenital (malformation) or acquired obstruction or narrowing ( stenosis ) of the tear drainage ducts, for example due to bacterial infections or inflammation of the nose ( rhinitis ) with swelling of the opening of the tear and nasal passage, tears flow over the edge of the eyelid. The constriction can occur both in the area of the lacrimal tubules (präsaccal) or in the area of the exit of the sac or the nasal passage (postsaccal). If a drug therapy is not sufficient, the natural lacrimal can be recovered surgically (z. B. means of lacrimal duct endoscopy, a further development of the method 1713 used by Dominique Anel opening of a laid lacrimal duct with syringe and the probe) or a bypass ( bypass ) of the constriction to be created for the nose. In individual cases the implantation of a tear duct prosthesis is necessary. Anesthesia is usually required for all surgical interventions on the tear ducts .
Congenital stenosis
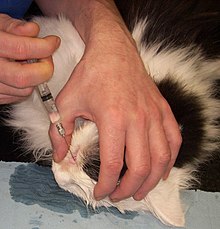
In children, a Hasner valve that does not open (see above) sometimes prevents the tears from being transported away (congenital tear duct stenosis). In these cases, a special blunt lacrimal cannula of the lacrimal be probed and rinsed. Since this procedure is painful, it should be performed under anesthesia. Some rare syndromes may have a stenosis, such as: B. in Branchio-oto-renal syndrome or Saethre-Chotzen syndrome .
Inflammation
An inflammation of the lacrimal sac is as Dakryozystitis referred. Pathologically, it is an empyema . This leads to a painful swelling in the area of the tear sac. Sometimes pus drains spontaneously through the skin, in individual cases the tear sac has to be relieved with a stab incision. An antibiotic treatment is usually required. The anatomical proximity to blood vessels that pull into the brain ( angular vein ) can result in life-threatening complications. Since the cause of the inflammation is mostly a drainage disorder, surgical rehabilitation is often necessary in the end.
The lacrimal tubules can also become inflamed ( canaliculitis ) and cause painful swelling. Often bacterial inflammation and / or tear duct stones (dacryolites) are the cause of this. Antibiotic therapy is often necessary, and if necessary, surgical removal of the tear duct stones.
Injuries
If the eyelids are injured in the nasal direction of the lacrimal points, the lacrimal tubules may become involved. An injury to the lacrimal ducts must be recognized in good time and the lacrimal tubules must be surgically restored, as otherwise scar healing and loss of function with tears may occur.
literature
- Theodor Axenfeld (founder), Hans Pau (ed.): Textbook and atlas of ophthalmology. With the collaboration of Rudolf Sachsenweger and others 12th, completely revised edition. Gustav Fischer, Stuttgart et al. 1980, ISBN 3-437-00255-4 .
- Holger Busse and Peter Kroll: History of the treatment of diseases of the lacrimal ducts. In: Historia ophthalmologica internationalis 1, 1979/80, pp. 241-258.
- Paul Simoens: organ of vision , organum visus. In: Franz-Viktor Salomon, Hans Geyer, Uwe Gille (Ed.): Anatomy for veterinary medicine. 2nd, revised and expanded edition. Enke, Stuttgart et al. 2008, ISBN 978-3-8304-1075-1 , pp. 579-612.
- Anton Waldeyer: Human anatomy. 17th, completely revised edition. Walter de Gruyter, Berlin et al. 2003, ISBN 3-11-016561-9 , pp. 587-588
Individual evidence
- ↑ Axel W. Bauer : Therapeutics, Therapy Methods. In: Werner E. Gerabek , Bernhard D. Haage, Gundolf Keil , Wolfgang Wegner (eds.): Enzyklopädie Medizingeschichte. De Gruyter, Berlin / New York 2005, ISBN 3-11-015714-4 , pp. 1388-1393; here: p. 1390.