hernia
| Classification according to ICD-10 | |
|---|---|
| K40 | Inguinal hernia (inguinal hernia) |
| K41 | Femoral hernia (femoral hernia) |
| K42 | Umbilical hernia (umbilical hernia) |
| K43 | Ventral hernia (epigastric, scar) |
| K44 | Diaphragmatic hernia (diaphragmatic hernia) |
| K45 | Other abdominal hernias |
| K46 | Unspecified abdominal hernia |
| ICD-10 online (WHO version 2019) | |
A hernia (pronunciation: [ ˈhɛʁni̯ə ]; from Latin hernia , 'break', from Greek ἔρνος érnos "bud, sprout"), German break , is the exit ("breakthrough", "breakthrough") of viscera from the abdominal cavity ( Intestinal hernia , abdominal hernia ) through a congenital or acquired gap ( hernial opening ) in the supporting or delimiting tissue layers. If parts of the brain leave their normal position, one speaks of a brain hernia .
features
Each hernia has three characteristics:
- Breach gate
- A prerequisite for the development of a hernia is a weak point in the wall of the abdominal cavity . Mostly this is already established in the embryonic development . The weak point can also arise later, for example from a scar after an abdominal operation. Due to the constant intra-abdominal pressure and a slight overstrain (coughing blow), the supporting layers of the abdominal wall can diverge so far that a bag-like bulging of the remaining layers of the abdominal wall results as a hernial sac.
- Hernial sac
- Its inner lining usually consists of sliding peritoneum with hernia. Its narrowest point, trapped in the hernial port, is called the hernial sac neck.
- Fractional content
- Due to inflammatory reactions, a break can contain broken water , but it can also be temporarily empty. Often, however, it contains a corner of the large network or even a loop of the small intestine. Freely movable organs such as the ovary , wall parts of the urinary bladder or the large intestine can also be included. With a diaphragmatic hernia, it is often the stomach that slides through a slit in the chest.
Organs (stomach, large intestine, bladder) that are only partially located within the abdominal cavity lined with peritoneum, so-called retro- or extraperitoneal organs , can slide through a hernial opening and then take a peritoneal pocket on the outside with them as a hernial sac. These hernias are called sliding fractures .
Malnutrition, cachexia (with tumor disease) and ascites cause an increase in abdominal pressure and weakening of the abdominal wall and thus promote the development of abdominal wall hernias, which are then referred to as symptomatic hernias .
Fresh hernias are usually reponible (from the Latin reponere = to restore ), i.e. This means that the contents can be returned to the abdominal cavity by applying gentle pressure from the outside. This maneuver is called taxis and can mask complications if used uncritically and there is no subsequent monitoring.
Types of hernias
A distinction is made between internal and external hernias according to the location of their appearance. If the hernia can be recognized from the outside or if the hernial portal leads from the inside of the body towards the skin, it is called an external hernia . If the hernia lies within the trunk (e.g. directed from the abdomen into the chest) and therefore cannot be recognized without aids, then it is an internal hernia .
Internal hernias
Diaphragmatic hernia
In the case of diaphragmatic hernia (Latin hernia diaphragmatica ), abdominal organs enter the chest cavity.
- Their congenital diaphragmatic hernia (abbreviation CDH) is caused by an incomplete diaphragm.
- In adulthood, however, anatomical weaknesses in the diaphragm promote hernia formation:
- the slit-shaped passage of the esophagus, called the hiatus oesophageus, as a passage for a hiatal hernia
- a herniation through the gap between the sternum and the rib (diaphragm sternocostalis / parasternalis) is called Morgagni hernia on the right and Larrey hernia on the left
- the passage of soft tissues through the pars lumbocostalis, especially on the left, where the liver does not cover this gap (only shown on the right of the graphic), is called Bochdalek's hernia.
Treitz's hernia
In Treitz's hernia, parts of the intestine are pinched in the superior duodenal recess, a very narrow peritoneum pocket behind the so-called Treitz's ligament ( ligamentum suspensorium duodeni ), which fixes the duodenum and contains intestinal vessels.
External hernias
Inguinal hernia
The inguinal hernia or inguinal hernia (Latin hernia inguinalis ) is the most common form of hernia (80%). It appears above the inguinal ligament at an anatomically predetermined point, the outer inguinal ring. One distinguishes the
- direct inguinal hernia (Latin hernia inguinalis directa / medialis )
- Here the break emerges through a weak point in the inner layer of the abdominal wall, the medial inguinal fossa , which projects onto the outer inguinal ring. This type of fracture, as well as the following, emerges externally on the outer inguinal ring (annulus inguinalis superficialis). But since there is no favorable embryonic structure as a guide rail, this form is rarely innate.
- indirect inguinal hernia ( lat.Hernia inguinalis indirecta / lateralis )
- It enters the abdominal wall on the inner inguinal ring , runs in the spermatic cord in men and accompanies the vas deferens and, like the aforementioned break on the outer inguinal ring, comes to the surface of the body. In women, only the uterine ligament runs in the inguinal canal . Since it is significantly smaller than the spermatic cord, the lateral inguinal hernia is rare in women, but the medial shape is not common in women either.
The majority of the child's inguinal hernia develops from an open peritoneal vaginal process and thus corresponds to the definition of a so-called “indirect inguinal hernia”. It is usually diagnosed in infancy and is more common in premature babies. Boys and the right side are more often affected. The inguinal hernia must be surgically corrected shortly after the diagnosis. The risk of incarceration (entrapment of the intestine) exists especially in the first year of life. In female babies, the ovaries and fallopian tubes can slide into the fracture, which is known as an "ovarian hernia". If the appendix is found in the inguinal hernia, it is called an Amyand hernia.
Femoral hernia
The femoral hernia (syn. Femoral fracture, Latin hernia femoralis ) occurs predominantly in older women. It also occurs in men after an inguinal hernia operation according to Shouldice or Bassini (2–3%).
The femoral hernia emerges below the inguinal ligament through the lacuna vasorum , more precisely on the inside (medial) of the vena femoralis through the so-called lacuna lymphatica . Femoral hernias are more painful than inguinal hernias and often pinch or cannot be repositioned. Often only the greater omentum and no bowel is trapped in them. But mobile ovaries are also possible as hernial sac contents. A femoral hernia should be excluded for any swelling palpable below the inguinal ligament. Because of the more frequent risk of entrapment with circulatory disorders (incarceration), urgent surgery is desirable.
As with an inguinal hernia, swollen lymph nodes, among other things, can be used as a differential diagnosis .
Umbilical cord break
In the case of an omphalocele (umbilical cord break), the umbilical cord is inflated like a sack due to a malformation of the abdominal wall, and abdominal organs protrude through the navel.
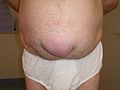
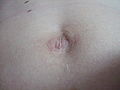
Umbilical hernia
Umbilical hernias ( Latin hernia umbilicalis et paraumbilicalis ) often occur immediately after birth in infancy. The cause is the incomplete formation of the abdominal wall on the navel . As a rule, these infant umbilical hernias do not tend to become trapped and usually regress spontaneously, so they are not treated surgically, but with bandages. In rare cases, e.g. If, for example, the hernia does not want to slide back into the abdominal cavity immediately when the infant screams loudly, the doctor can administer sedatives so that the child can relax and the fracture can slide back ( repositioning ).
Umbilical hernias are relatively common in adults. Often those affected have no symptoms and have also come to terms with the bulging appearance of the navel. In umbilical hernias with a small hernial port, abdominal organs can become trapped and cause considerable discomfort. The large network is found most frequently . Especially for small hernia is incarcerated feared.
Many techniques exist for the surgical treatment of umbilical hernias. The choice of the "right" surgical technique depends on the size of the hernia, the patient's activity, general health and the like. a. dependent.
Obturator hernia
A hernia obturatoria emerges through the hip bone hole ( foramen obturatum ), a point of passage in the hip bone that is closed with connective tissue, and the contents of the hernia can squeeze the vessels running in the hip hole canal (canalis obturatorius) and the nervus obturatorius in such a way that sensory disturbances on the inner thigh (ramus cutaneus) are caused obturator nerve). However, this form of hernia is very rare and, as it is not externally visible or palpable, is often only recognized by the intestinal obstruction due to entrapment. Diagnostics by means of ultrasound is possible, the mobile break content can be recognized during the pressing test and the diagnosis can be made.
Epigastric hernia
In the case of epigastric hernia (Latin hernia epigastrica ; epi (Greek) = on, over; gaster (Greek) = stomach), a painful swelling can be felt in the linea alba between the xiphoid and the navel in the abdominal wall consists of preperitoneal fatty tissue, but later of a real hernial sac, which often contains a corner of the large network .
Spieghel's hernia
The Spieghel hernia (Latin hernia spigeli or H. lineae semilunaris, English Spigelian hernia) is a hernia that extends into the abdominal wall in the area of the posterior leaf of the rectus sheath (linea semilunaris). It too is rare and often misunderstood.
Incisional hernia
In incisional hernias (Latin: Hernia cicatrica ), an all-layered abdominal wall scar forms the hernial port due to its lack of elasticity. Such scars are almost exclusively the result of previous laparotomies (open abdominal surgery). Due to adhesions , the preparation is demanding and the long-term success of an operation is by no means certain. However, surgery is recommended, as the hernia enlarges the chances of recovery from getting worse over time. Fascia doublings
according to Mayo or a butt-to-butt suture were standard recurrent therapy . Plastic nets are currently used for reinforcement, the methods often being named after the position of the netting in relation to the supporting abdominal wall layers, mostly in English (sublay, inlay, onlay plastic).
Diastasis recti
As diastasis recti is defined as the moving apart of the straight abdominal muscles (the rectus abdominis ). An operation indication exists only in case of complaints. It is not a hernia in the classic sense.
Littré - Richter hernia
It describes a type in which only part of the intestinal wall is trapped in a very small hernia like a blister. Since this hernia can easily be loosened again and can easily be overlooked intraoperatively, a thorough inspection of all intestinal sections is essential during the operation. Because of its non-obstructive nature (i.e., passage through the small intestine is never completely prevented), abdominal pain is easily misunderstood.
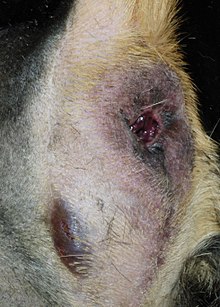
Perineal hernia
A perineal hernia is a hernia of the pelvic floor with a protrusion of the perineum . It is relatively common in uncastrated male domestic dogs .
Muscle hernia
A muscle hernia is the bulging of skeletal muscle tissue through a tear in the fascia .
Symptoms
Depending on its location, a hernia can be noticed by swelling or go unnoticed. This can also cause pain. With external hernias, increased intra-abdominal pressure, e.g. B. by coughing or abdominal pressure, the hernia protrude.
Some hernias no longer slip back due to inflammatory adhesions (they are called irreposible ) and cause variable pain.
Usually, patients first notice occasional pulling pain in the groin area, later see or notice a bulge, but sometimes the bulge appears without pain. The swelling often disappears spontaneously when the load ceases, but will occur more frequently and become larger in the further course until it is perceived as annoying.
The cause of the bulging often occurs due to an increase in pressure in the abdomen (intra-abdominal pressure) when coughing and laughing, when pressing, when exercising or when carrying heavy loads. Particularly susceptible are people who have to carry heavy loads inexperienced or who practice extreme sports (due to excessive strain), but constant loads can also promote this disease if the stabilizing body tissue is fatigued.
If the contents of the hernia (tip of the large mesh, intestine ) are trapped in the hernia gap, severe permanent pain occurs at the location of the protrusion with pain radiation, e.g. B. in the scrotum with inguinal hernias or in the pubic region with inguinal and femoral hernias. If, in addition to the swelling, there is reddening as an expression of severe inflammation, urgent surgery can hardly be avoided. In the case of inguinal and femoral hernias, a restriction of movement is often indicated.
In principle, any abnormal protrusion in the groin area should be examined by a doctor. In addition to hernias, there may also be enlarged lymph nodes or vascular changes.
Only in cases of uncomplicated, slight fractures may the protrusion be pushed back by the doctor without exception. However, this is not a cure, and an operation that can be planned (weeks to months) cannot be avoided. As long as there is no fracture entrapment or other complications, there is no need for immediate surgery.
Complications
In the case of untreated hernias in particular, there is a fear of complications, which in the older German surgical literature were also referred to as incidental fractures .
The accumulation of intestinal contents in the worn intestinal loops causes a fecal entrapment with damage to the intestinal wall. Even more feared, however, is the clamping of the blood supply to the intestinal loops, known as incarceration . It is obvious that these complications occur particularly with narrow and by no means large hernial openings. These last two complications are extremely painful and require surgical therapy within six hours.
Another complication is the maceration of the skin over a mostly monstrous hernial sac. Because of the associated increase in the risk of surgical infection, such wounds often cause the unavoidably necessary operation to be postponed.
Therapy options
Treating an inguinal hernia with a truss , rupture gymnastics, or injecting drugs are historical methods. Since only one operation ensures lasting success, it is now the rule. In acute cases, a reduction can be attempted using taxis in order to gain time for the surgical treatment. Various surgical procedures are available for surgical care. Because of the risk of life-threatening incarceration (see above), there is an indication for early fracture surgery , especially with small fractures .
Because soft tissue fractures do not recede, they get larger over time. If, for example, the diagnosis of an inguinal hernia has been confirmed and the patient is in an operable condition, then nowadays there is no doubt about the operation. Depending on the symptoms, only the most suitable time for the operation can be determined. A hernia ligament can only be used in patients who are inoperable or who have refused to operate . A truss is an unwieldy tool with dubious success. It consists of a padded, elastic metal clasp that is placed around the hips and a small ball-shaped leather sack that presses on the hernia. Since inguinal hernias can be operated under general anesthesia , spinal anesthesia or local anesthesia , the truss is only of historical importance these days.
Operating principles and procedures
"Open" surgery using an abdominal incision
The hernial sac is exposed via an incision and, with a few exceptions, opened. The contents are shifted back into the abdominal cavity, the hernial sac prepared up to the hernial sac neck, shortened and closed. The hernial port is then closed by a:
- direct suture: This closure is often only possible with very small breaks.
- Fascia doubling: The edges of the coarse layers of the abdominal wall ( fascia ) are doubled (Mayo operation for hernia ventralis, Inguinal hernia operation according to Shouldice for hernia inguinalis), that is, sutured overlapping in order to achieve greater stability. The recurrence rate is to be classified with 1% as relatively low.
- Stabilization of the hernial port closure through artificial materials. In the case of larger breaks, the seam is strengthened by stitching the body's own tissue (rarely) or with plastic nets. Both non-absorbable and absorbable, and recently even special hybrid materials are used. The individual methods also differ in the layer of the abdominal wall in which the mesh is implanted. So far , the Lichtenstein operation , developed by the American surgeon Irving L. Lichtenstein , has often been used for inguinal hernias , in which a non-absorbable plastic mesh is fixed to (over) the transversal fascia (= onlay technique) after the hernial sac reduction. According to recent findings, the recurrence rate is higher than expected, which is why the mesh is now increasingly placed preperitoneally (= sublay technique). The pressure in the abdominal cavity is absorbed by the network in the right place, so to speak. With a good surgical technique (see Shouldice Clinic), the recurrence rates are roughly the same as with the Shouldice duplication (open sublay techniques according to Wantz [unilateral] or Stoppa [bilateral]). The long-term results are better, long-term side effects with abrasion and others are unpredictable. Surgeons who have mastered several methods, which should be the rule, therefore generally recommend doubling the fascia in the case of good fascia material, but in the case of a very large fracture, recurrence or, if the connective tissue does not promise a secure seam, mesh implantation in this way.
"Closed" surgery using a laparoscopy
This access through the abdominal wall ( laparoscopic surgery ) has also become increasingly established in hernia surgery. The principle here is basically the introduction of a (plastic) mesh into the abdominal wall in methodically different depths. A general superiority over conventional technology has not yet been proven because the long-term results are still pending.
Aftercare
Healing to a firm scar takes up to three months. Tensile and compressive loads that z. B. when lifting heavy objects, when coughing violently or by abrupt movements should be avoided if possible. Depending on the size of the fracture, this stress should be avoided for up to two years in order to ensure the success of the treatment. Any excess weight should be reduced if possible.
history
Early publications on hernia surgery come from Caspar Stromayr (1559) and Pierre Franco (1561).
literature
- Ch. Neubert, L. Faupel and U. Katzenmeier: Abdominal wall hernias. In: Surgery historically: beginning - development - differentiation. Edited by FX Sailer and FW Gierhake, Dustri-Verlag, Deisenhofen near Munich 1973, ISBN 3-87185-021-7 , pp. 139–152.
- A [rpad] Gyergyai: Critical Comments on the History of the Doctrine of Fractions . In: German Archive for the History of Medicin u. medicinische Geographie 3, 1880 (reprint Hildesheim 1971), pp. 321–331 and 381–393.
- Alfred H. Iason (Ed.): Hernia. Philadelphia 1941, particularly pp. 3-152 (Alfred H. Iason: The evolution of hernial surgery ).
- Ernst Kern: hernias. In: Karl Vossschulte , Hanns Gotthard Lasch , F. Heinrich (Ed.): Internal medicine and surgery. An integrated textbook. Stuttgart and New York 1979; 2nd edition, ibid. 1982, pp. 588-597.
Web links
- MedlinePlus: hernia (English)
- Hernia Guide from the German Publishing House for Health Information GmbH
Individual evidence
- ↑ spectrum: brain hernia .
- ↑ Spectrum: tentorial hernia .
- ↑ Alexander M. Rokitansky; Hernia surgery in pediatric surgery ; Schweinitz and Ure; Springer Verlag, 2009; ISBN 978-3-540-89031-7 ; here online , accessed on December 3, 2015.
- ^ R. Hutchinson: Amyand's hernia. In: Journal of the Royal Society of Medicine. Volume 86, Number 2, February 1993, pp. 104-105, PMID 8433290 , PMC 1293861 (free full text).
- ↑ Pierre Franco: Traité des hernies. Lyon 1561.