Staphylococcal scalded skin syndrome
| Classification according to ICD-10 | |
|---|---|
| L00 |
Staphylococcal scalded skin syndrome (SSS syndrome)
|
| ICD-10 online (WHO version 2019) | |
The Staphylococcal scalded skin syndrome (abbreviation SSSS) ( English scalded skin [ skɔːldəd skɪn ], German 'scalded skin' ) - among many other synonyms also after the names of the first and second descriptions of dermatitis exfoliativa neonatorum Ritter von Rittershain (1878) or Staphylogenes Lyell Syndrome (1956) called - is a skin toxicosis in infants and small children caused by the haematogenic spread of highly specific staphylococcal exotoxins , which is characterized by extensive, burn-like erythema with blistering and subsequent skin detachment. The syndrome was formerly known as peeling blisters ( peeling blisters ). The potentially life-threatening disease is rare these days. If left untreated, the disease is still often fatal, but with early medical treatment the prognosis is favorable.
Epidemiology
Dermatitis exfoliativa neonatorum Ritter von Rittershain , Knight's disease for short , was an endemic and very feared infectious disease of newborns with a very high mortality rate, endemic in maternity wards and in orphanages , before the introduction of hospital hygiene and until the pre- antibiotic period .
Today the disease occurs only rarely and sporadically and mainly affects infants in the first three months of life and older toddlers with an age peak of up to four years. The incidence of the disease is higher in boys than in girls. The reason for this is the noticeably lower rate of breakdown of the bacterial toxins exfoliatin A and B in relation to adults as the triggering mechanism in the early childhood organism.
From the age of five, children become ill only extremely rarely and as a rule these are patients with immunodeficiency or impaired kidney function and the mortality in these cases is still very high despite antibiotic treatment. Cases of illness in adults are an extraordinary rarity; only around 50 cases (fewer than 40 cases) have been documented worldwide to date.
The rarity of the disease in adults is primarily attributed to an acquired immunity to the corresponding staphylococcal toxins, as well as to the fully efficient excretory function of the mature kidneys of healthy adults. The adult SSSS patients were almost exclusively patients with immunosuppression due to tumor disease, HIV , organ transplantation or alcoholism, as well as patients with renal insufficiency .
Pathogenesis

The extensive reddening of the skin with blistering is very reminiscent of scalding of the skin - "scalded skin syndrome" - and was sometimes confused with such in the past. The clinical picture is caused by toxic, hematogenous action at a distance, usually an extracutaneous infection with the strong toxin-forming agent Staphylococcus aureus of lysophage group II. The erythemato-bullous skin fluorescence is the direct consequence of a massive exfoliation in the bloodstream.
The staphylococcal toxins exfoliate A (ETA), exfoliate B (ETB) and exfoliate D (ETD) act as serine proteases and, due to their extremely targeted molecular specificity, lead to a breakdown of the adhesive protein desmoglein 1 within the desmosomes . The cell-cell contacts of the stratum granulosum of the epidermis dissolve and there is a non-inflammatory loosening of the cell structures with the formation of gaps (see image file 4 ), which causes the upper corneal layers of the epidermis to detach (subcorneal staphylococcal peeling syndrome) and as flaccid Blistering appears. This pronounced toxic specificity can also explain why the exfoliate-producing strains of Staphylococcus aureus develop their activity exclusively within the epidermis, although these toxins circulate equally throughout the entire organism.
At the time of the first description by the Prague pediatrician Gottfried Ritter von Rittershain (1878), purulent staphylococcal infections of the belly button were primarily responsible for this disease, which at that time was still spread like an epidemic in the maternity facilities of the time. Thanks to improved hygienic conditions, the incidence of the disease could be drastically reduced in the last century, so that today omphalitis is only rarely identified as the source of this skin toxicosis, but rather purulent infections of the conjunctiva and the upper respiratory tract.
More rarely, the disease is based on direct staphylococcal skin infections, such as B. Impetigo bullosa or cutaneous skin wounds, but in some cases it is also clinically inconspicuous staphylococcal niches. The SSS syndrome is a systemic disease and not, as previously assumed, the maximum variant of impetigo contagiosa staphylogenes. As a rule, therefore, no pathogens are detectable in the generalized subcorneal blisters.
Clinical course
Prodromal phase
The disease can be preceded by purulent staphylococcal infections of the nasopharynx ( rhinitis , tonsillitis ), ears ( otitis media ) and eyes ( conjunctivitis ) by a few days. The symptoms in the preliminary stage are often unspecific with impairment of the general condition and fever. Before the actual onset of the disease, a small speckled scarlet-like rash sometimes appears , which later changes into the SSSS-typical skin lesions in the acute phase. The periorifical onset of the rash around the eyes, nose and mouth is indicative of the differential diagnosis. Sometimes the so-called “staphylococcal scarlet fever” is also observed as a minimal variant of the SSSS. In these cases, the disease is mild without the full clinical picture developing.
Erythematosum stage
In the actual initial phase, bright red, fuzzy erythema develops on the face - preferably around the mouth, nose and eyes - which then quickly spread over the entire body via the large bends: neck, armpits and groin. The skin is extremely sensitive to any touch and the children are irritable and tearful because of the burning pain.
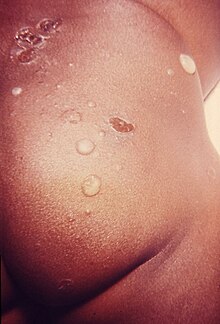
In the bullous impetigo shown here , the skin lesions remain localized. With staphylococcal scalded skin syndrome, however, there is a systemic toxicosis of the entire skin. Large-scale detachments of the top layers of the skin occur.
Exfoliative stage
After a few hours or days, the skin becomes wrinkled and large, flaccid blisters are formed which, due to their small thickness (it is only the top layers of the skin of the epidermis), tear open very easily and then erode as if "smacked" on the bright red Epidermis. This detachment can already be triggered by carefully brushing the erythematous skin (“indirect” Nikolski sign ), which is why it primarily affects the resting and rubbing areas at the beginning. But the Nikolski sign is also positive on apparently healthy skin: By firmly wiping your finger over it, the top layer of the skin can be pushed off tangentially “like a ripe peach” . In contrast to toxic epidermal necrolysis , the mucous membranes of the mouth, eyes and genitals are typically not or only rarely and slightly affected, which can be explained by the fact that the uppermost cornified skin layer, the stratum corneum, is physiologically non-existent in the mucous membranes.
Under the detachments, the skin is bright red and shiny, sometimes oozing but not purulent, since the detachment is not triggered directly by the staphylococci themselves, but by the remote action of their toxins . The detachment can take place in both small and large steps and extensive erosion occurs , especially on body parts subject to mechanical stress. The bright red eroded areas of skin are surrounded by a white border, which consists of contracted “shreds of skin”.
In this phase, significant losses of fluid and blood salts can occur, similar to a second-degree skin burn, and life-threatening conditions can quickly arise from hypovolemic shock or sepsis if therapeutic intervention is not timely.
Desquamativum stage
Correct medical treatment will bring the disease dynamics to a standstill within a few hours and the skin will begin to renew itself. The re-epithelialization of the erosions takes about 10 to 14 days and is followed by extensive, fine-lamellar peeling.
Differential diagnosis and diagnosis
The skin lesions are very similar to the clinical picture of a scald and can easily be confused with such. The Nikolski sign is positive and the pathogen Staphylococcus aureus can often be detected in the throat swab, depending on the focus of the infection, also from the eyes and ears. In the prodromal phase , a small-spotted rash, similar to scarlet fever , sometimes appears; the beginning of the face around the mouth, nose and eyes is indicative of the differential diagnosis. The signs of angina tonsillaris and “raspberry tongue” typical of scarlet fever are also missing . Sometimes there are also blisters that are reminiscent of the large-bubble impetigo contagiosa . In the case of the SSS syndrome, however, these are neither purulent nor can pathogens from them generally be detected. In certain cases, the staphylococcal scalded skin syndrome can also show extraordinary similarities to burn injuries in the context of child abuse and must therefore be diagnosed.
The distinction between staphylococcal scalded skin syndrome (staphylogenic Lyell's syndrome) and toxic epidermal necrolysis (drug-induced Lyell's syndrome ), two diseases that were previously not clearly differentiated or even equated, is of the greatest importance for the differential diagnosis . The patient's age, medication history and the Tzanck test provide initial clues. However, only a bladder lid histology provides diagnostic reliability. The histological examination shows the SSSS a acantholytic gap formation in the area of the granular layer and the formation of bubbles subcorneal. In TEN , however, specific epidermal necrosis can be found in all layers of the epidermis. Another typical feature of toxic epidermal necrolysis is the preferential infestation of the mucous membranes, which does not appear in the case of staphylococcal scalded skin syndrome , or only very discreetly. The DRESS syndrome must also be differentiated .
In addition to the formation of a gap in the stratum granulosum, evidence of SSSS is the detection of exfoliatins in the blood using enzyme-linked immunosorbent assays (ELISA), Western blots or polymerase chain reactions . A bacterial examination should be arranged to uncover sources of infection.
Complications and prognosis
It is a potentially serious disease that, if left untreated, can often lead to life-threatening complications such as hypovolemic shock , pneumonia and sepsis . With early and correct treatment, severe disease courses in small children are the exception and the prognosis for children up to the age of five is favorable (3%). For older patients, on the other hand, the SSS syndrome is very often fatal (40%) because of the underlying diseases, even with intensive care treatment.
therapy
The initial treatment includes high-dose administration of penicillinase-resistant penicillins ( e.g. flucloxacillin , oxacillin or methicillin ) and other antibiotics effective against Staphylococcus aureus ( e.g. cefalosporins , erythromycin or minocycline ). Phage type II staphylococci are rarely multi-resistant strains. In the case of extensive skin lesions, the loss of fluid and blood salts must be compensated for by infusion and adequate local treatment of the affected areas must be carried out. Particular attention should be paid to protection against infection. Intensive medical care and therapy that go beyond these medical measures, as in the case of burn injuries, is superfluous. Corticosteroids are contraindicated because their immunosuppressive effects increase the risk of infection.
History and synonyms
Alleged scalds by midwives and mothers
Due to the clinical picture, which even today can hardly be distinguished from a second-degree burn without laboratory diagnostics, these skin detachments were often mistaken for unintentional and deliberately concealed scalds in newborns. There have been trials in which mothers and midwives were sued for having bathed their infants suffering from SSSS too hot and thereby scalded them.
Dermatitis exfoliativa neonatorum Ritter von Rittershain (1878)
The pediatrician and director of the Prague foundling facility Gottfried Ritter von Rittershain was the first to examine this endemic infant disease. In a precisely defined time frame, he carried out systematic observations on symptoms, the course of the disease and mortality. During his ten-year case studies, which he wrote down from July 1, 1868 to June 30, 1878, he recorded a total of 297 cases of illness, of which 145 died. Describing the delicate, bright red erythema with which the disease first appears (see image file 4 ), he was initially called dermatitis erysipelatosa in 1870 . He later coined the term dermatitis exfoliativa neonatorum , which more accurately described the characteristic skin detachment and has now found its way into the specialist literature of the time and is still used today as a disease name for SSSS in newborns.
Pemphigus neonatorum and Pemphigus acutus neonatorum
After that, the disease was often simply called Ritter's disease after its supposed first person to describe it , in the English-speaking area Ritter Disease . However, the latest medical-historical research now suggests that with some probability the disease was already described 70 years earlier by other pediatricians in the specialist literature as Erisipelas (sic!) Neonatorum (1807) and Pemphigus infantilis analogous to Erysipelas of infants (1813), both of which were often observed in the children's hospitals of that time. In addition to the name dermatitis exfoliativa neonatorum Ritter von Rittershain, the synonyms pemphigus neonatorum and pemphigus acutus neonatorum were also used . In contrast to Ritter's disease, pemphigus neonatorum was, as some authors suspected, a much milder, self-limiting skin disease with only local blistering, which appears as a special form of bullous impetigo in newborns.
Staphylodermia superficialis diffusa exfoliativa
Later, after the causal significance of the staphylococci was discovered and the distinction between streptogenic and staphylogenic impetigo was soon made, Ritter’s dermatitis and other staphylogenic skin infections were grouped under the umbrella term staphyloderma . At that time, however, no distinction was made between systemic skin toxicosis (dermatitis exfoliativa) and local staphylococcal infection (bullous impetigo) , which is why Ritter’s disease was erroneously referred to as the maximum variant of bullous impetigo ( impetigo contagiosa staphylogenes ) In connection with this, "baroque" terms such as Staphylodermia superficialis bullosa pemphigoides neonatorum et infantum and Staphylodermia superficialis diffusa exfoliativa emerged , the latter of which is still currently used in German-speaking dermatological specialist circles.
Toxic epidermal necrolysis - "Lyell's syndrome" (1956)
With the increasing use of synthetic drugs , isolated dermatological side effects were observed as early as the mid-1930s, which largely corresponded to the clinical picture of a Ritter von Rittershain exfoliative dermatitis . After the Second World War, the British dermatologist Alan Lyell had made similar observations in adults and described them for the first time in 1956 as “Toxic epidermal necrolysis” “with the arrival of Anglisms (sic!) In continental terminology”.
In the course of his further investigations, however, he had to find out in retrospect that his original description was a mixture of two different clinical pictures. From now on he made a logical distinction between toxic epidermal necrolysis caused by staphylococci , which was already known to him as Ritter's disease , and the actual drug-induced TEN, which was unknown until recently and which he newly described . This differentiation was then referred to in the specialist literature of that time as staphylogenic Lyell syndrome (STEN) and drug-induced Lyell syndrome ( DTEN ) and these terms are still in use today in some cases.
Staphylococcal scalded skin syndrome (1970)
Lyell and his colleagues soon realized that a previously unknown staphylococcal toxin must be responsible for the staphylococcal-induced TEN and were actually able to isolate this toxin (exfoliate). The attempt in mice to produce a staphylococcal-induced TEN by inoculating these toxins, however, failed. A few years later, Melish and Glasgow (1970) carried out a similar experiment on newborn mice and this time actually triggered a staphylococcal-induced TEN.
literature
- Peter Fritsch: Dermatology, Venereology. 2nd Edition. Springer, Berlin / Heidelberg / New York 2004, ISBN 3-540-00332-0
- Otto Braun-Falco et al. (Ed.): Dermatology and Venereology. 5th edition. Springer, Berlin / Heidelberg / New York 2005, ISBN 3-540-40525-9
- Gernot Rassner: Dermatology - textbook and atlas. 8th edition. Urban & Fischer, Munich / Jena 2007, ISBN 3-437-42762-8
- Ingrid Moll, (Ernst G. Jung) (Ed.): Dermatology. 6th edition. Thieme, Stuttgart 2005, ISBN 3-13-126686-4
- Klaus Betke et al. (Ed.): Textbook of paediatrics - Keller / Wiskott. 6th edition. Thieme, Stuttgart 1991, ISBN 3-13-358906-7
- Manfred Dietel et al. (Ed.): Harrison's Internal Medicine. 15th edition. ABW, Berlin 2003, ISBN 3-936072-10-8
Web links
- "Staphylodermia superficialis diffusa exfoliativa" - DermIS: A cooperation between the University of Heidelberg and the University of Erlangen-Nuremberg.
- "Staphylococcal infections of the skin" - AWMF guidelines of the German Dermatological Society. ( "Staphylogenic Lyell Syndrome" see Chapter 2.3.1)
Individual evidence
The clinical observations and scientific findings that have found their way into this article originate primarily from the standard work of dermatology:
- Peter Fritsch: Dermatology, Venereology. 2nd Edition. Springer, Berlin / Heidelberg / New York (among others) 2004; Pp. 259f, ISBN 3-540-00332-0
Individual documents are only provided for disputed issues from this work. - The following sources are also cited:
- ↑ A. Müller, RW Schlecht, Alexander Früh, H. Still The way to health: A faithful and indispensable guide for the healthy and the sick. 2 volumes, (1901; 3rd edition 1906, 9th edition 1921) 31st to 44th edition. CA Weller, Berlin 1929 to 1931, Volume 1 (1931), p. 18 f.
- ↑ a b c d e f g h i j Dietrich Abeck: Staphylococcal scalded skin syndrome (SSSS) . In: Otto Braun-Falco , Gerd Plewig , Helmut H. Wolff, Walter HC Burgdorf, Michael Landthaler (eds.): Dermatology and Venerology . 5th edition. Springer, Berlin / Heidelberg / New York (among others) 2005, p. 110, ISBN 3-540-40525-9
- ^ A b Gottfried Ritter von Rittershain: Dermatitis exfoliativa neonatorum . In: Central newspaper for paediatrics. 2, 1878, pp. 3-23.
- ↑ SD Resnick, PM Elias: Staphylococcal scalded-skin syndrome . In: IM Freedberg, AZ Eisen, K. Wolff, KF Austen, LA Goldsmith, SI Katz, TB Fitzpatrick (eds.): Fitzpatrick's Dermatology in General Medicine. 5th ed. McGraw-Hill, New York 1999, ISBN 0-07-912938-2 , pp. 2207-2212
- ↑ a b Jessica H. Kim, Paul Benson: Staphylococcal Scalded Skin Syndrome . In: Leonard Sperling, Michael J. Wells, Edward F. Chan, Catherine Quirk, William D. James (Eds.): EMedicine Specialties - Dermatology - Bacterial Infections. Article Last Updated: May 16, 2007. URL: www.eMedicine.com - Full text. (accessed on August 28, 2007)
- ↑ a b Maja Mockenhaupt, Marco Idzko, Martine Grosber, Erwin Schöpf, John Norgauer: Epidemiology of staphylococcal scalded skin syndrome in Germany . In: Journal of Investigative Dermatology . 124, (4), April 2005; Pp. 700-703. doi: 10.1111 / j.0022-202X.2005.23642.x - Full text.
- ↑ Andrea C. Klucken, Martin Witzenrath, Norbert Suttorp: Staphylogenic Lyell syndrome (staphylococcol scalded skin syndrome; SSSS) . In: Manfred Dietel, Joachim Dudenhausen, Norbert Suttorp (eds.): Harrison's internal medicine - Volume 1 . 15th edition. ABW, Berlin 2003, ISBN 3-936072-10-8 , p. 984
- ↑ Peter Fritsch, Peter Elias, Janos Varga: The fate of Staphylococcal exfoliatin in newborn and adult mice. In: British Journal of Dermatology . Vol. 95, 3, September 1976, p. 275, doi: 10.1111 / j.1365-2133.1976.tb07015.x
- ↑ a b Gernot Rassner: Dermatology - textbook and atlas. 8th edition. Urban & Fischer, Munich / Jena 2007, ISBN 3-437-42762-8 , p. 87
- ↑ Takayuki Yamaguchi et al .: Identification of the Staphylococcus aureus etd Pathogenicity Island Which Encodes a Novel Exfoliative Toxin, ETD, and EDIN-B . In: Infection and Immunity . Vol. 70, No. 10, October 2002, pp. 5835-5845, doi: 10.1128 / IAI.70.10.5835-5845.2002 - abstract.
- ↑ G. Prevost, P. Couppie, H. Monteil: Staphylococcal epidermolysins . In: Current Opinion in Infectious Diseases . 16, (2) April 2003; Pp. 71-76, abstract. co-infectiousdiseases.com; Retrieved September 7, 2007
- ↑ Helmut Hahn: Staphylococci . In: Helmut Hahn, Dietrich Falke, Paul Klein (Eds.): Medical Microbiology . Springer, Berlin / Heidelberg / New York (among others) 1991, ISBN 3-540-19389-8 , p. 255
- ↑ a b c Peter Fritsch: Bacterial infections in childhood . In: Gerd Plewig, Peter Kaudewitz, Christian A. Sander (eds.): Advances in practical dermatology and venereology 2004. - Lectures and slide clinic of the 19th training week 2004: Training week for practical dermatology and venereology e. V. c / o Clinic and Polyclinic for Dermatology and Allergology at the Ludwig Maximilians University of Munich. Springer, Berlin / Heidelberg / New York (among others), 2005, ISBN 3-540-21055-5 , pp. 471-474
- ↑ a b c d Fritsch 2004
- ↑ a b c d e f g Regina Fölster-Holst: Bullous and vesicular skin diseases in childhood . In: CME Dermatology. Issue 5, No. 2, August 2007; P. 53 f., ISSN 1860-7268 , cme.akademos.de, accessed on August 31, 2007
- ↑ a b c d e f Helmut H. Wolff: Pyodermien . In: Klaus Betke, Wilhelm Künzer, Jürgen Schaub (Hrsg.): Textbook of Pediatrics - Keller / Wiskott. 6th edition. Thieme, Stuttgart / New York 1991, ISBN 3-13-358906-7 , p. 955
- ↑ Claus Simon and Michael Jänner: Color Atlas of Pediatrics with information on differential diagnosis. 3. Edition. Schattauer, Stuttgart / New York 1994, ISBN 3-7945-1640-0 , p. 158
- ↑ a b Marian E. Melish, Lowell A. Glasgow: "The staphylococcal scalded skin syndrome - Development of an experimental model." In: The New England Journal of Medicine . Vol. 287, no. 20; Pp. 1114-1119
- ↑ a b Marian E. Melish, Lowell A. Glasgow: Staphylococcal scalded skin syndrome: The expanded clinical syndrome . In: The Journal of Pediatrics . Vol. 78, No. June 6, 1971; Pp. 958-967
- ↑ Andrea Porzionatoa, Anna Aprile: Staphylococcal scalded skin syndrome mimicking child abuse by burning . In: Forensic Science International. Vol. 168, 1, 3 May 2007; S. e1-e4, doi: 10.1016 / j.forsciint.2007.01.014
- ↑ a b Maria Heckmann: Luminal disease under the picture of dermatitis exfoliativa with fatal outcome . In: European Journal of Pediatrics. Volume 57, No. 4, July 1935; Pp. 358-360, doi: 10.1007 / BF02249708
- ↑ a b D.M. Hitch et al .: Toxic late effects and exfoliative dermatitis according to 'Slim' (= dinitrophenol) . In: Fühner-Wieland's collection of poisoning cases . Volume 7, December 1936; P. 213f., Doi: 10.1007 / BF02452984
- ↑ a b Alan Lyell: Toxic epidermal Necrolysis: An Eruption resembling scalding of the skin . In: British Journal of Dermatology. 68, (11), 1956; Pp. 355-361
- ↑ Nicolaus Ostermayer: A case of Pemphigus neonatorum P. Richter (Dermatitis exfoliativa neonat. Ritter) with infection of the mother and death of the newborn . In: Archives for Dermatology and Syphilis . Vol. 67, No. 1, October 1903; Pp. 109-112, doi: 10.1007 / BF01951407
- ^ Gottfried Ritter von Rittershain In: Österreichisches Jahrbuch für Pädiatrik. Volume 1, 1870
- ↑ a b c d Karl Holubar : "The Rittersche Dermatitis exfoliativa neonatorum and the toxic epidermal necrolysis (TEN) - a medical historical consideration." In: Nova Acta Leopoldina. NF 89, No. 334, 2004; Pp. 119-124
- ↑ Joseph Jakob Plenck: Doctrine of the knowledge and healing of childhood diseases. JG Binz, Vienna 1807. Quoted from: Karl Holubar: The Rittersche Dermatitis exfoliativa neonatorum and the toxic epidermal necrolysis (TEN) - a medical historical consideration . In: Nova Acta Leopoldina. NF 89, No. 334, 2004; Pp. 119-124
- ↑ T. Bateman: Practical Synopsis of Cutaneous Disease According to the Arrangement of Dr. William. Longman Hurst Rees Orme and Brown, London 1813. Quoted from: Karl Holubar: The Rittersche Dermatitis exfoliativa neonatorum and the toxic epidermal necrolysis (TEN) - a medical historical consideration . In: Nova Acta Leopoldina. NF 89, No. 334, 2004; Pp. 119-124
- ↑ Julius Caspary: About Dermatitis exfoliativa neonatorum . In: Archives for Dermatology and Syphilis. Volume 11, number 1-2, March 1884, pp. 122-127, doi: 10.1007 / BF01968180
- ↑ Rudolf Winternitz: A contribution to the knowledge of the dermatitis exfoliativa neonatorum (Ritter) . In: Archives for Dermatology and Syphilis. Volume 44, Number 1, December 1898; Pp. 397-418, doi: 10.1007 / BF01990874
- ↑ Friedrich Luithlen: Dermatitis exfoliativa Ritter . In: Archives for Dermatology and Syphilis. Volume 47, Number 3, March 1899; Pp. 323-338, doi: 10.1007 / BF01950127
- ↑ Ernst Almquist: Pemphigus neonatorum, bacteriologically and epidemiologically illuminated . In: Journal of Hygiene and Infectious Diseases. Volume 10, April 1891, pp. 253-257, doi: 10.1007 / BF02188520
- ↑ K. Dohi: On the clinic and etiology of impetigo contagiosa . In: Archives for Dermatology and Syphilis. Volume 111, No. 2, March 1912, pp. 629-647, doi: 10.1007 / BF01960435 Abstract.
- ↑ DermIS A cooperation between the Department of Clinical Social Medicine (Heidelberg University) and the Erlangen Dermatology Clinic (Erlangen-Nuremberg University): "Staphylodermia superficialis diffusa exfoliativa". dermis.multimedica.de ( Memento of the original from September 27, 2007 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice. Retrieved August 31, 2007
- ^ Alan Lyell: Ritter's disease (Toxic epidermal necrolysis) . In: The Lancet . 2, 1962, p. 561
- ^ Alan Lyell: A review of toxic epidermal necrolysis in Britain . In: British Journal of Dermatology. 79, 1967; 662-671
- ^ Alan Lyell: Outbreak of toxic epidermal necrolysis associated with staphylococci . In: Lancet. 1, 1969; Pp. 787-790
- ^ Alan Lyell: The staphylococcal scalded skin syndrome in historical perspective: Emergence of dermopathic strains of Staphylococcus aureus and discovery of the epidermolytic toxin. A review of events up to 1970 . In: Journal of the American Academy of Dermatology . 9, (2), 1983; Pp. 285-294
- ↑ Alan Lyell (2000): "We had become certain ..." in a personal communication to Holubar. Quoted from: Rittersche Dermatitis exfoliativa neonatorum and toxic epidermal necrolysis (TEN) - a medical historical consideration . In: Nova Acta Leopoldina. NF 89, No. 334, 2004, pp. 119-124



