traumatic brain injury
| Classification according to ICD-10 | |
|---|---|
| S06 | Intracranial Injury |
| S06.0 | Concussion Commotio cerebri |
| S06.1 | Traumatic brain edema |
| S06.2 | Diffuse brain injury Compressio cerebri, traumatic, onA Brain contusion onA |
| S06.3 | Localized brain injury Localized brain contusion Traumatic intracerebral hemorrhage |
| S06.4 | Epidural bleeding |
| S06.5 | Traumatic subdural bleeding |
| S06.6 | Traumatic subarachnoid hemorrhage |
| S06.7 | Intracranial injury with prolonged coma [coma prolongé] |
| S06.8 | Other intracranial injuries |
| S06.9 | Intracranial injury, unspecified brain injury onA |
| ICD-10 online (WHO version 2019) | |
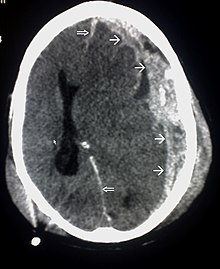
A traumatic brain injury ( ancient Greek τραύμα trauma , German 'wound' , abbreviation SHT or TBI for traumatic brain injury ) or traumatic brain injury is any injury to the brain due to an external cause (force). However, the term does not refer to any associated skull fractures or head laceration wounds. Often, hospital observation is recommended because of the possibility of cerebral hemorrhage or other complications from traumatic brain injury, even with minor traumatic brain injury, often referred to as a " concussion ".
causes
People suffer traumatic brain injuries in accidents , often in accidents at work , traffic accidents , household and sports accidents .
Helmets (e.g. protective helmets, bicycle helmets, sports helmets) can reduce the risk of injury.
Some sports carry a particularly high risk of traumatic brain injury, for example through the body check in ice hockey and American football . 42% of all injuries suffered by ice hockey players are directly attributable to a body check. Many professional ice hockey players had to end their athletic careers after head injuries. In 2012, the German Ice Hockey League stated that it would follow checks against the head and / or neck area harder than before. Former football players in the United States suffer from chronic brain disease.
Classifications
The SHT is divided using the Glasgow Coma Scale (GCS):
- light SHT : GCS 15-13
- moderate SHT : GCS 12–9
- severe TBI : GCS 8–3
One further distinguishes that
- covered SHT and that
- Open TBI: perforation of the scalp , cranial bones and tearing of the hard meninges ( dura mater ).
Previously, there was a division into three degrees of severity, based on the duration of the unconsciousness , the regression of the symptoms and the long-term effects:
- 1st degree TBI ( commotio cerebri or concussion ): slight, hidden brain injury with acute, temporary brain dysfunction. It is accompanied by an immediate short-term disturbance of consciousness of a few seconds up to a maximum of ten minutes. Other typical symptoms are retrograde amnesia (memory gap for the accident event and a period prior to the accident), nausea and / or vomiting . An anterograde amnesia (memory loss for the period after the accident) is rare (it is usually a sign of a higher grade brain injury). Neurological failures do not occur after the unconsciousness has subsided. Symptoms such as apathy , reduced performance, headaches , dizziness and nausea can persist for several weeks as part of a so-called post - commotional syndrome .
- 2nd degree TBI ( contusio cerebri , brain contusion or brain contusion ): The loss of consciousness lasts longer than ten minutes. Long-term effects depend on the location of the brain injury. No perforation of the dura mater .
- 3rd degree TBI ( Compressio cerebri or brain contusion ): The unconsciousness lasts longer than 60 minutes and is caused by entrapment of the brain due to bleeding, edema or similar processes. The brain is the only large part of the human body that is almost completely surrounded by bones. However, this special protection can become a danger in space-consuming processes, since the entire brain can suffer from the increase in pressure and the ensuing entrapment. The result is often a long-lasting coma (which is often artificially prolonged), a coma-like state or even death. Temporary removal of part of the skull (a few months) can be used to relieve pressure. Permanent brain injuries are to be expected, but not inevitable.
The division is very schematic. For example, a traumatic injury to the frontal lobe does not necessarily result in unconsciousness, but can lead to permanent brain injury ( frontal lobe syndrome ). Usually today a distinction is only made between mild, moderate and severe head trauma (according to the Glasgow Coma Scale ).
Pathophysiology
In TBI, neuronal structures are damaged in two phases. The first phase concerns the acute injury: The damage to neuronal structures can no longer be prevented here. The second phase of brain damage does not begin until later: Various pathophysiological processes result in delayed and non-mechanical neuronal damage, which can possibly be alleviated by adequate therapy.
Symptoms
The following symptoms could indicate a traumatic brain injury. Some of the symptoms mentioned may take some time to develop after the trauma. This is known as latency or latency (the amount of time between when the trauma occurs and the symptom occurs).
- Impairment of consciousness , possibly with increasing cloudiness, up to unconsciousness
- Headaches persist in up to 95% of patients and can also occur after a delay of up to seven days after the trauma. They can last for weeks to months; after three years, 13% of one case series still suffered from persistent headaches.
- Dizziness and imbalance
- CSF flow from the ear
- Brain mass leakage
- Squint ( Déviation conjuguée )
- Eye tremors
- Pupillary difference (different sized pupils)
- Rigid pupil
- Paralysis of the arms or legs
- Convulsions , seizures , rigidity
- Breathing disorder , for example from obstruction of the airway due to the tongue falling back
- Nausea and vomiting
- Word finding disorders ( amnestic or anomic aphasia )
- Gaps in memory ( amnesia )
- visual hallucinations ( photopsias )
The pupillary difference ( anisocoria ) and increasing disturbances in consciousness are special warning signs to be taken seriously, as they can be indications of bleeding within the skull . If, after an immediately post-traumatic, initially temporarily limited unconsciousness, a second phase of impaired consciousness occurs later, the phase in between of clearer consciousness is referred to as the free interval . Such a course is taken as a sign of epidural or subdural cerebral hemorrhage .
Diagnosis
TBI is a potentially life-threatening disease. Therefore, the patient must be examined immediately and thoroughly:
- Clinical-neurological examination: examination of the state of consciousness (including language and memory), the cranial nerves (eyes, ears, facial expressions, tongue and throat), the ability to move (strength, coordination) and sensitivity. Thereby assessment of the Glasgow coma scale and examination of the indication for a computed tomography . Since TBI often occurs as part of a multiple trauma, all other regions of the body must also be examined.
- Computed tomography ( CT ) of the head: The X-ray procedure can be used to determine whether and where there are bleeding spots, tissue damage or signs of intracranial pressure. In children, it should be checked whether CT can be replaced by magnetic resonance tomography because of the radiation exposure .
- In the case of flexion and / or extension synergisms at the scene of the accident, arterial hypotension and older people, there is an indication for the implementation of invasive intracranial pressure monitoring using an intraventricular ICP probe.
- The analysis of the protein S100 from the blood can be used to diagnose mild traumatic brain injury, but is hardly available.
Immediate (acute) therapy decisions must then be made: indication for surgery, intensive care medicine, further specialist examinations (ophthalmologist, ENT doctor, etc.), inpatient monitoring or discharge (e.g. in the case of bruised skull without TBI).
Further examinations are often useful in the interval:
- Magnetic resonance imaging (MRI): This is where electromagnetic pulses are measured. The images show even small damage to various areas of the brain. It is also possible to make an early statement about the prognosis for severe TBI. The prerequisite for this examination is the patient's resting position.
- The electroencephalogram ( EEG ): This measures the brain waves, i.e. the function of the brain (questions about epileptic seizures, testing of the reaction to external stimuli in severe TBI).
- Evoked potentials : nerve tracts are checked for their permeability. The eyes, ears and skin are electrically irritated. Reactions to this suggest malfunctions at certain switching points. SEP and AEP in particular often allow statements to be made about the prognosis for severe TBI.
- The ophthalmological findings: clarification of additional injuries to the eye (bleeding, perforation, detachment of the retina ).
- Post mortem plaques jaunes are found as evidence of severe TBI during an autopsy .
With the help of microRNAs from the saliva , indications of the severity of a concussion can be obtained, especially in children, as researchers working with Steven Hicks from Pennsylvania State University have found. About a third of children who experience a concussion develop prolonged concussion symptoms. The salivary microRNAs represent easily measurable, physiologically relevant and precise potential biomarkers for a traumatic brain injury, which allow a prediction of the symptoms.
treatment
Treatment of traumatic brain injury can vary depending on the severity and accompanying injuries. The immediate measures that are taken at the scene of the accident concentrate on stabilizing the cardiovascular function and eliminating all conditions associated with a drop in blood pressure ( hypotension ) and reduced oxygen concentration ( hypoxia ) in the blood. So measures must be taken to ensure the oxygen supply to the brain. Unconscious patients are therefore intubated , and associated respiratory injuries such as pneumothorax must also be treated.
In the case of TBI of the first degree (and if there are no accompanying injuries), only symptomatic treatment of nausea and vomiting, bed rest and inpatient monitoring for 12–24 hours are necessary.
In the case of TBI of the second or higher degree, further measures are required: Securing breathing by administering oxygen and intubation , fluid replacement depending on the loss, shock treatment (if necessary), combating intracranial pressure by elevating the upper body, intubation, mild hyperventilation, (strong) sedation using benzodiazepine and propofol and possibly barbiturate , as these substances simultaneously lower intracranial pressure and reduce cerebral metabolism. Surgical measures come immediately into consideration if bleeding has occurred that occupies space.
The patient must be transported to the nearest hospital that has a CT for further treatment and monitoring .
If the intracranial pressure rises too much despite maximum conservative therapy, a relief craniectomy is recommended . During this operation , parts of the skull are removed to give the swollen brain more space and thus help reduce intracranial pressure. The removed parts of the skull can be reinserted after the swelling has subsided, usually after 4 weeks to 6 months.
The resolution of symptoms with a concussion can take 10 to 25 days, in less severe cases as little as 3–7 days. It is supported by rest and avoidance of television, noise and stress.
If an affected person continues to exercise immediately after a concussion in contact sport, the time for their symptoms to resolve doubles.
Various complications can occur in the context of TBI, the treatment of which is described separately: unconsciousness , intracranial pressure , epidural haemorrhage , subdural haemorrhage and skull base fracture .
Hypothermia
In theory, hypothermia initiated shortly after the trauma, i.e. an artificial lowering of body temperature, should lower the brain's energy and oxygen requirements, reduce the inflammatory reaction ( encephalitis ) and the risk of permanent brain damage. The first observational experimental studies also showed marked neuroprotective results. The POLAR study from 2018 is now the fourth large multicenter randomized study that clearly shows that hypothermia does not have a protective effect. In this study with 466 patients after severe, traumatic brain damage, the hypothermia occurred on average 1.8 hours after the brain injury. Slow rewarming occurred after 22.5 hours. After 6 months, the result was checked using the Glasgow Outcome Scale . With hypothermia the result was favorable in 48.8%, without hypothermia in 49.1% ( relative risk RR = 0.99, not significant). Pneumonia (55% versus 51.3%) and intracranial bleeding (18.1% versus 15.4%) were more common under hypothermia.
Others
There is a consensus paper of the IOC and FIFA that contains specific guidelines for the diagnostic procedure after the occurrence of a minor head injury in sport as well as recommendations for the criteria for a gradual return to training and match events ( Sport Concussion Assessment Tool , SCAT).
In addition to the GCS , the following control questions are listed. a. the following are used for evaluation: headache, pressure in the head, neck pain, nausea or vomiting, dizziness, blurred vision, balance disorders, sensitivity to light or noise, the feeling “everything is slower”, one feels “like in a fog”, one does not feel "Together", difficulty concentrating, memory loss, tiredness or low energy, confusion, drowsiness, trouble falling asleep (if applicable), increased emotions / irritability / sadness, nervousness and anxiety.
A scientific longitudinal study of 235,110 patients revealed with a concussion that 667 of these later (median 9.3 years after) suicide committed. This corresponds to 31 suicides per 100,000 patients or 3 times more suicides than in the normal population.
See also
literature
- S2e guideline for traumatic brain injury in adulthood of the German Society for Neurosurgery . In: AWMF online (as of 07/2007)
- S1 guideline for mild traumatic brain injury of the German Society for Neurology . In: AWMF online (as of 10/2008)
- S1 guideline for severe traumatic brain injury of the German Society for Neurology. In: AWMF online (as of 10/2008)
- S1 guideline for assessment after covered head trauma of the German Society for Neuroscientific Assessment. In: AWMF online (as of 07/2013)
- Volker Schumpelick, Niels Bleese, Ulrich Mommsen (eds.): Short textbook surgery . 8th edition. Georg Thieme Verlag, Stuttgart / New York 2010, ISBN 978-3-13-127128-0 , p. 181, 182 .
- S2k guidelines for traumatic brain injury in childhood of the Society for Neonatology and Pediatric Intensive Care Medicine, the German Society for Pediatric Surgery, the Society for Neuropediatrics, the German Society for Neurosurgery, the German Society for Neuroradiology, the Society for Pediatric Radiology, the German Society for anesthesia and intensive care medicine, the German Society for Trauma Surgery and the German Interdisciplinary Association for Intensive Care and Emergency Medicine. In: AWMF online (as of 2011)
- Rainer Fritz Lick , Heinrich Schläfer: Accident rescue. Medicine and technology . Schattauer, Stuttgart / New York 1973, ISBN 978-3-7945-0326-1 ; 2nd, revised and expanded edition, ibid 1985, ISBN 3-7945-0626-X , pp. 188–190 ( traumatic brain injuries ).
Web links
- Underestimated finding. Researchers warn against playing down concussions. Spiegel Online , January 18, 2010.
- Advisor cranial brain trauma
- Project on "Minor head injuries in sport" in Germany. sportneuropsychologie.de
-
Heads Up: Concussion in Youth Sports
- Fact Sheet (PDF; 265 kB)
Individual evidence
- ↑ Ice Hockey Injuries ( Memento from March 20, 2012 in the Internet Archive )
- ↑ In ice hockey, the number of severe concussions increases dramatically. Many players are about to end their careers . In: Rheinische Post . December 8, 2012.
- ↑ del.org ( Memento of the original from December 28, 2012 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice.
- ↑ Super Bowl: Death is on the field. on: web.de , January 30, 2013.
- ^ Head Injuries in Football. In: New York Times ; Virginia Tech expands sports concussion-risk studies to include hockey and baseball , President Barack Obama And NFL Exchange Comments On Football And Concussions , Obama would think 'hard' before letting son play football, cites head-injury fears
- ↑ Heinz-Walter Delank: Neurology . 11th edition. Thieme , Stuttgart 2006, ISBN 3-13-129771-9 , pp. 277 ff .
- ↑ AG Mustafa, OA Alshboul: Pathophysiology of traumatic brain injury. In: Neurosciences (Riyadh, Saudi Arabia). Volume 18, Number 3, July 2013, pp. 222-234, ISSN 1319-6138 . PMID 23887212 . (Review).
- ↑ Felicitas Witte: Headache after brain trauma. In: Deutsches Ärzteblatt . 2018, volume 115, issue 6 of February 9, 2018, pages A244-A246
- ↑ Manio of Maravic: Neurological emergencies. In: Jörg Braun, Roland Preuss (Ed.): Clinic Guide Intensive Care Medicine. 9th edition. Elsevier, Munich 2016, ISBN 978-3-437-23763-8 , pp. 311–356, here: pp. 340–342 ( craniocerebral trauma ).
- ↑ Steffen Reissberg u. a .: Neuroradiological findings to assess the prognosis in patients after traumatic brain injuries. In: Clinical Neuroradiology. 13, No. 1, pp. 27-33, 2003, doi: 10.1007 / s00062-003-4348-4 .
- ^ Jeremiah J. Johnson, Andrea C. Loeffert, Jennifer Stokes, Robert P. Olympia, Harry Bramley, Steven D. Hicks: Association of Salivary MicroRNA Changes With Prolonged Concussion Symptoms. In: Journal of the American Medical Association - Pediatrics, November 20, 2017. doi : 10.1001 / jamapediatrics.2017.3884 .
- ↑ Traumatic brain injury . Heidelberg University Hospital
- ↑ Rachel Rabkin Peachman: Playing With a Concussion Doubles Recovery Time. In: The New York Times.com. August 29, 2016. Retrieved October 3, 2016 .
- ↑ RJ Elbin, Sufrinko A, Schatz P, French J, Henry L, Burkhart S, Collins MW, Kontos AP: Removal From Play After Concussion and Recovery Time . In: Pediatrics . 138: e20160910, 2016. PMID 27573089 .
- ↑ Kathrin Gießelmann: Neuroprotection after traumatic brain injury: early hypothermia is clinically of no use . Deutsches Ärzteblatt 2018, Volume 115, Issue 46 of November 16, 2018, Page A2128; [1]
- ↑ DJ Cooper, AD Nichol, M Bailey, and others: Effect of Early Sustained Prophylactic Hypothermia on Neurologic Outcomes Among Patients With Severe Traumatic Brain Injury. The POLAR Randomized Clinical Trial. In: Journal of the American Medical Association 2018; Volume 320 (Issue 21): pp. 2204-2206. doi: 10.1001 / jama.2018.17075
- ↑ questionnaire ( Memento of the original April 27, 2013 Internet Archive ) Info: The archive link is automatically inserted and not yet tested. Please check the original and archive link according to the instructions and then remove this notice. (English, PDF, 272 kB), app for the iPhone
- ↑ M. Fralick, D. Thiruchelvam, HC Tien, DA: Risk of suicide after a concussion . In: CMAJ . tape 188 , 2016, p. 497-504 , PMID 26858348 .