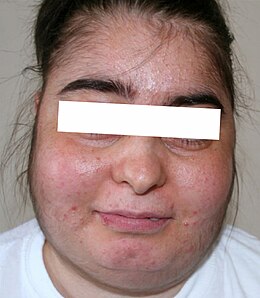
Cushing's Syndrome
| Classification according to ICD-10 | |
|---|---|
| E24 | Cushing's Syndrome |
| ICD-10 online (WHO version 2019) | |
The Cushing's syndrome [ ˈkʊʃɪŋ- ] is an excessive concentration of glucocorticoids ( cortisol ) in the blood, among other things with increased blood sugar level and with chronic form typical changes in body shape. It was named after the US neurosurgeon Harvey Williams Cushing , who first described it in 1910. The name after Cushing was proposed in 1942/43 by the American endocrinologist Fuller Albright . In addition to Cushing's syndrome I described below, other Cushing syndromes have also been described, which are sometimes referred to as Cushing's syndrome II and III.
Cushing's Syndrome I.
When Cushing's syndrome is physical changes caused by high cortisol levels in the blood (hypercortisolism) are caused. This is characterized by an increased blood sugar level and a partial suppression of the immune system . The disease can develop gradually over the years, with fatty tissue typically accumulating on the trunk of the body and the limbs becoming thinner due to muscle wasting.
A basic distinction is made between endogenous and exogenous Cushing's syndrome. The latter is much more common and is caused by external influences, especially the long-term use of glucocorticoids (mainly cortisone ).
Endogenous Cushing's syndrome affects women up to four times more often than men and can occur at all ages. The adrenal cortex produces too much cortisol without being stimulated (adrenal cortex autonomy). However, if the adrenal cortex is stimulated by the stimulation hormone ACTH because there is a tumor of the pituitary gland , the disease is called Cushing's disease .
causes
The causes of Cushing's syndrome can be:
- Central Cushing's syndrome (hypothalamic-pituitary): Increased production of ACTH (adrenocorticotropic hormone) in the anterior pituitary gland ( Cushing 's disease, Cushing's disease), less often increased production of CRH in the hypothalamus with subsequent increased corticosteroid release from the adrenal cortex .
- Adrenal or ACTH-dependent Cushing's syndrome (also known as ACTH cell hyperplasia or ACTH cell tumor): Increased secretion of glucocorticoids from the adrenal cortex in the course of neoplasias ( adenomas or carcinomas of the adrenal cortex) with subsequent suppressed release of ACTH from the anterior pituitary.
- Ectopic ( paraneoplastic ) Cushing's syndrome (also called ectopic ACTH syndrome): Formation of ACTH (or, very rarely, CRH) in ectopic tissue, usually in the context of small-cell lung cancer .
- Cushing's syndrome caused by medication: onset of symptoms after regular and prolonged systemic intake of high doses of ACTH or corticosteroids and other steroid hormones as part of the treatment of diseases such as autoimmune diseases , allergies or bronchial asthma .
- Pseudo-Cushing syndrome ( Cushingoid ): Temporary Cushing symptoms, for example in the course of severe skull injuries.
Symptoms
The symptoms of Cushing's syndrome are caused by the increased hormonal effect of the corticoids on the target tissues. Achard-Thiers syndrome is a special form of Cushing's syndrome with similar symptoms .
- " Full moon face " (round and with reddened cheeks)
- Weight gain due to trunk obesity
- stocky torso and thin legs
- " Bull neck ", also called "buffalo neck " and "buffalo hump", due to the accumulation of fat between the shoulders
- Metabolism as in diabetes mellitus with thirst and frequent urination
- Increased blood pressure , especially arterial hypertension
- Hypogonadism and Potency Reduction in Men
- Menstrual cycle disorders in women
- Increased tendency to fractures due to bone loss, see osteoporosis
- thinning skin and the formation of strips of tissue (so-called striae rubrae) due to the skin atrophy
- Muscle weakness , including heart weakness and muscle atrophy
- Acne and excessive hair ( hirsutism )
- Water retention in the tissue ( edema )
- Formation of kidney stones
- Back pain
- increased susceptibility to infection and slow healing of wounds
- Reduced growth and obesity in children
- occasional psychological changes such as anxiety attacks or psychosis
Diagnosis
If Cushing's syndrome is suspected, it must first be clarified whether medication containing cortisone has been taken. Corresponding hormone levels can be determined using blood, urine and saliva samples. Above all, the dexamethasone inhibition test and the CRH test can detect a disruption in the release of adrenal hormones. It also looks for tumors or adenomas that could cause endogenous Cushing's syndrome. Computer or magnetic resonance imaging is used to look for changes in the pituitary gland and adrenal glands.
- Physical examination:
- Skin inspection
- Blood pressure control
-
Endocrinological :
- Short dexamethasone test
- Cortisol excretion in the 24-hour urine
- Insulin hypoglycemia test
- CRH test
- Clarification of osteoporosis
-
Radiological :
- Depiction of the adrenal glands or the pituitary gland ( sonography , CT , MRI )
Differentiation of pituitary-adrenal-ectopic
1. CRH test : 100 µg corticotropin releasing hormone as an iv bolus; Measure ACTH and cortisol before CRH and after 30, 60, 90 and 120 minutes.
| ACTH mirror | CRH test | |
|---|---|---|
| normal | n | ACTH ↑ cortisone ↑ |
| Central | ↑ | ACTH ↑ cortisone ↑ |
| Adrenaline | ↓ | ACTH↔ Cortisone↔ |
| Ectopic | ↑ | ACTH↔ Cortisone↔ |
2. Liddle test : 0.5 mg dexamethasone po every 6 hours for 2 days, then 2 mg dexamethasone every 6 hours for 2 days. Daily cortisol excretion in the urine and in the serum cortisol concentration on days 3 and 5 at 8 a.m.
3. Sinus petrosus sampling : Catheters in the inferior petrosal sinus on both sides. ACTH, cortisol and possibly prolactin simultaneously from the petrosal sinus left and right and from the peripheral vein before and 2, 5 and 10 minutes after CRH.
The difficulties of finding a diagnosis are presented using a case study in the NDR broadcast Adventure Diagnosis .
Cushing threshold dose
In the specialist literature, the Cushing threshold dose is given with the strength of 7.5 mg prednisone or 30–40 mg (in men), 15–30 mg (in women) cortisol per day.
In children, the Cushing threshold dose is 6 mg / m² body surface area / day of prednisone equivalent (prednisone is about four times as effective as cortisol). This describes the daily maintenance dose that should not yet trigger Cushing's syndrome. However, this information is to be understood as a rough guideline, as there are considerable inter-individual differences. There is no absolute lower limit below which glucocorticoid therapy can be considered safe. Topically applied (on the skin) glucocorticoid preparations are most likely not to cause Cushing's syndrome, as they only penetrate the skin barrier to a very small extent. Nevertheless, it is recommended to limit the therapy to a maximum of 20% of the body surface and to be cautious when using it on the face or eyes.
therapy
Therapy depends on the cause of Cushing's syndrome: adenomas of the pituitary or adrenal glands are surgically removed; The treatment of choice for adrenal hyperplasia is adrenalectomy and subsequent lifelong hormone substitution to prevent Addison's disease . A Nelson tumor can then develop as a complication .
In January 2020, the EU Commission approved Osilodrostat (trade name: Isturisa , manufacturer: Novartis ) as an oral treatment for adult patients with endogenous Cushing's syndrome. Osilodrostat is an inhibitor of the body's own cortisol biosynthesis.
Cushing's Syndrome II
Cushing's syndrome II is a rare disease in which a tumor in the pons or cerebellum causes damage to the cranial nerves VI , VII and VIII on the same side . Deficiency symptoms of the cerebellum and signs of intracranial pressure are also described in the context of this disease. The current name is cerebellar bridge symptoms .
It was first described in 1917 by Harvey Williams Cushing .
Diagnostic criteria are:
- Gait disorder, possibly tinnitus
- Balance disorder
- later facial paralysis , failure of the trigeminal nerve
Cushing's syndrome in animals
In veterinary medicine , Cushing's syndrome occurs primarily in horses ( equines Cushing's syndrome ), in dogs ( canine Cushing's syndrome ) and rarely in cats (feline Cushing's syndrome ). Typical laboratory changes are a stress leukogram , elevated liver values ( ALT and ALP ), elevated blood sugar levels , high cholesterol levels and a low specific gravity of the urine . The treatment of the disease is usually carried out with drugs that lower the cortisol production in the adrenal cortex. The agent of choice for the dog is trilostane . Treatment with the DDT derivative mitotane and also with the antimycotic ketoconazole is possible.
See also
Web links
- The European Register on Cushing's Syndrome
- Patient information (PDF) [archived]
- What is Cushing's Syndrome? Internists on the net
Individual evidence
- ^ H. Cushing: The Pituitary Body and Its Disorders: Clinical States Produced by Disorders of the Hypophysis Cerebri. An Amplification of the Harvey Lecture for December, 1910. JB Lippincott, Philadelphia / London 1912.
- ^ F. Albright: Cushing's syndrome . In: Harvey Lectures . Series 38, 1943, pp. 123-186 .
- ↑ H. Nowakowski, H.-J. Breustedt: Diseases of the hypothalamus-pituitary system. In: Rudolf Gross , Paul Schölmerich , Wolfgang Gerok (Eds.): 1000 memoranda of internal medicine. Schattauer, Stuttgart / New York 1971; 4th, completely revised edition ibid 1989 (= UTB for Science / Uni-Taschenbücher. Volume 522), ISBN 3-7945-1282-0 , pp. 156–160, here: pp. 159 f.
- ^ Adventure Diagnosis NDR Cushing Syndrome Broadcast from December 6, 2016 . Retrieved December 13, 2016
- ↑ Summary of Product Characteristics. (PDF) EMA, accessed on February 12, 2020
- ^ HW Cushing: Tumors of the nervus acusticus and the syndrome of the cerebellopontine angle. Saunders, Philadelphia 1917.
- ^ B. Leiber: The clinical syndromes. Syndromes, sequences and symptom complexes. Edited by G. Burg, J. Kunze, D. Pongratz, PG Scheurlen, A. Schinzel, J. Spranger, 7th edition. Urban & Schwarzenberg 1990, ISBN 3-541-01727-9 .