Diabetes mellitus
| Classification according to ICD-10 | |
|---|---|
| E10 | Primarily insulin-dependent diabetes mellitus (type 1 diabetes) |
| E11 | Non-primarily insulin-dependent diabetes mellitus (type 2 diabetes) |
| E12 | Diabetes mellitus in connection with malnutrition or malnutrition (malnutrition) |
| E13 | Other specified diabetes mellitus |
| E14 | Unspecified diabetes mellitus |
| ICD-10 online (WHO version 2019) | |
The diabetes mellitus (honey-sweet flow ', Honigharnruhr'; from ancient Greek διαβήτης diabetes [to διαβαίνειν diabainein , German , pass' , flow through '] and Latin mellitus , honeyed' ), commonly known as just diabetes , German diabetes (formerly Zuckerharnruhr ) or, more rarely, blood sugar disease , describes a group of metabolic disorders of the carbohydrate metabolism, which are based on an (absolute or relative) lack of insulin and lead to chronic hypoglycaemia . The hallmarks of this complex disorder include hyperglycemia , glucosuria , acidosis, and ketosis .
The word describes their main symptom , excessive excretion of sugar in the urine . Thomas Willis diagnosed the disease in 1675, as did doctors of antiquity in India, Alexandria and Rome, on the basis of a taste test of the urine, because the urine of people with diabetes has a sweet taste when the blood sugar level is high .
Mechanisms that lead to excess sugar in the blood (hyperglycemia), set mainly on insulin, the main control hormone of glucose metabolism in the human body, to: absolute insulin deficiency, relative insulin deficiency due to a weakened effectiveness of insulin ( insulin resistance ) or both. The main consequences of diabetes mellitus are changes in the nervous system and the blood vessel system, including diabetic foot syndrome .
For the history of diabetology and in particular the history of the active ingredient insulin see History of Diabetology .
Physiological basics
The digestive system breaks down the carbohydrates ingested with food (from fruits, grain products, potatoes, corn, rice) into glucose (grape sugar), which is then absorbed into the blood through the intestinal wall and distributed throughout the body.
The pancreas produces the hormone insulin in the β cells of the islets of Langerhans . As a messenger substance , insulin effects the transport of glucose into the cell interior, where the glucose is then used to generate energy ( glycolysis ). In addition, insulin also causes the storage of glucose in the form of glycogen in the liver and in the muscle cells, which means that the blood sugar level after eating is within narrow limits (approx. 80–120 mg / dl or 4.5–6.7 mmol / l ) is kept constant.
Even with long periods of sobriety, the blood sugar level remains at a normal level, which in turn is mainly provided by the liver , on the one hand by the fact that the previously formed glycogen is split back into glucose and released back into the blood, on the other hand by the fact that the liver is biochemical constantly produces new glucose ( gluconeogenesis ).
If the insulin-producing β-cells no longer produce enough or no insulin at all or B. due to inflammation or surgery are no longer present, so both the glucose uptake in the body cells and the inhibition of glucose formation in the liver (which can produce up to 500 grams of glucose daily in humans) are missing. This new formation explains the rise in blood sugar levels in diabetics. B. in the early morning in the sober state (see also dawn phenomenon ).
In the case of diabetes mellitus, the glucose ingested remains in the blood, or the body's own formation of new glucose in the liver continues unchecked and constantly supplies glucose, which offsets or even exceeds the continuous consumption and, as a result, causes the blood sugar to rise. It is a very complex and dynamic biochemical process in which inflows, outflows, new formation and degradation of glucose have to be constantly balanced, i.e. offset. In order to understand these relationships - and thus the disease and how to deal with the disease - affected patients must be carefully informed and advised and, if necessary, trained, for example in drawing up suitable nutrition plans.
In addition, insulin has another, third effect. It is the only hormone in the human body that builds up body fat and also ensures that this fat remains in the depots (so-called adipogenic effect).
An essential characteristic of the severe, persistent insulin deficiency is therefore also an extreme weight loss due to the loss of the adipogenic effect, in particular through the breakdown of body fat and (muscle) protein for energy production.
Classification of diabetes mellitus into types
In 1965 the World Health Organization (WHO) published a distinction between different types of diabetes in its "Recommendations for Classification and Diagnostics".
In 1997 the American Diabetes Society (ADA) changed the criteria for classification and diagnosis, which were adopted by the WHO in 1998 and the German Diabetes Society (DDG) in 2000 . The model no longer differentiated between insulin-dependent diabetes mellitus (IDDM) and non-insulin-dependent diabetes mellitus (NIDDM), since this classification only relates to the treatment and not to the cause of the disease. Since 2009, the definition no longer distinguishes between subgroups a and b. The ranking of diabetes types from A to H was also abandoned.
Classification until 1997
Up to this date, diabetes mellitus was divided into four groups according to the type of treatment, the fifth denoting that the disease was absent:
- NIR : (non-insulin-requiring) treatment without external insulin supply, e.g. B. only with diet and / or oral antidiabetic drugs.
- IRC : (insulin requiring for control) In addition to the body's own insulin, external insulin is also required in order to lower elevated blood sugar levels.
- IRS : (insulin requiring for survival) External insulin supply is required for survival. According to the new classification, these are type 1 diabetes and type 2 diabetes with greatly reduced or discontinued own insulin production.
- IGT : (impaired glucose tolerance) impaired glucose tolerance .
- ND : (non diabetic) Not suffering from diabetes.
Types of diabetes since 1998
As of that date, all organizations have divided the disease into four types based on its cause:
-
Type 1 diabetes mellitus: destruction of the beta cells in particular in the islets of Langerhans in the pancreas usually leads to an absolute insulin deficiency
- Type 1a : immune-mediated ( autoimmune disease )
- Type 1b : idiopathic (unknown cause)
-
Type 2 diabetes mellitus: different combinations of insulin resistance , hyperinsulinism , relative insulin deficiency, secretion
disorders
- Type 2a : without obesity (obesity)
- Type 2b : with obesity
-
Other specific types of diabetes
- A : genetic defects in the beta cells of the islets of Langerhans (impaired insulin secretion)
- B : rare genetic defects in the action of insulin
- C : Diseased or destroyed pancreas
- D : diabetes due to hormonal disorders (endocrinopathies)
- E : Diabetes from drugs or chemicals (drugs, poisons)
- Q : Diabetes mellitus due to infections
- G : unusual forms of immune-mediated diabetes
- H : other genetic syndromes associated with diabetes
- Gestational diabetes (gestational diabetes)
Diabetes types according to the guidelines of the DDG 2009
Based on the report of the WHO commission from 1999, the following criteria are used in accordance with the guidelines of the DDG 2009:
- Type 1 diabetes mellitus: Destruction of the beta cells in the islets of Langerhans in the pancreas leads to an absolute insulin deficiency.
- Type 2 diabetes mellitus: Can range from (genetically determined) insulin resistance with a relative insulin deficiency to an absolute insulin deficiency in the later course of the disease. It is often associated with other metabolic syndrome problems .
- Other specific types of diabetes
- Exocrine pancreatic disorders (e.g., pancreatitis , cystic fibrosis , hemochromatosis )
- Endocrinopathies (e.g., Cushing's syndrome , acromegaly , pheochromocytoma )
- Drug-chemically induced (e.g. glucocorticoids , neuroleptics , alpha interferon , pentamidine )
- Genetic defects in β-cell function (e.g. MODY forms)
- Genetic defects in the action of insulin
- Other genetic syndromes that may be associated with diabetes
- Rare forms of autoimmune-mediated diabetes.
- Gestational diabetes : Glucose tolerance disorder that appeared or was diagnosed for the first time during pregnancy. This includes:
- First manifestation of type 1 diabetes
- First manifestation of type 2 diabetes
- Initial onset of other specific types of diabetes
- Preconceptionally manifest, but undiagnosed diabetes mellitus (type 2), especially to be assumed in the case of glucose tolerance disorders already in the 1st trimester .
This classification was confirmed in 2011 as part of an update of the guidelines by the DDG.
More terms
- Adolescent diabetes (English: juvenile diabetes mellitus ) or "juvenile diabetes mellitus" is the outdated term for type 1 diabetes.
- Age diabetes (English: Adult-Onset Diabetes mellitus ) or "adult diabetes" used to be called type 2 diabetes. Both terms are still widely used, but do not reflect the state of the art and are therefore no longer included in the current classifications.
- LADA : LADA ( latent autoimmune diabetes with onset in adults ) also belongs to type 1 diabetes mellitus . This form affects the autoimmune diabetes that develops in later adulthood, which after a relatively short time no longer reacts to oral medication and requires insulin. The detection of the GAD (= glutamate decarboxylase ) antibody is typical .
- MODY : MODY ( maturity onset diabetes of the young ) corresponds to the course of type 2 diabetes, but without the occurrence of obesity and insulin resistance; it already occurs in children and adolescents.
- IDDM : Abbreviation for insulin dependent diabetes mellitus . Conventional but still widespread classification according to the necessary form of therapy.
- NIDDM : Abbreviation for non insulin dependent diabetes mellitus . Conventional but still widespread classification according to the necessary form of therapy.
Epidemiology
Around 56 million people in Europe live with diabetes, corresponding to an (increasing) prevalence of around 8.5 percent. Over 90 percent of all diabetics are type 2 diabetics.
Frequency in Germany
Diabetes prevalence in the general population by type
According to estimates from care data , the diabetes prevalence (i.e. the proportion of patients treated for diabetes in the total population) in Germany in 2007 was 8.9%. In absolute numbers, this is over 7 million people in Germany who were treated for diabetes mellitus. Approx. 5–10% of those suffering from diabetes have type 1 and approx. 90% type 2.
Development of the prevalence of diabetes
The prevalence of diabetes has been growing since the earliest surveys in the early 1960s.
According to estimates from health insurance data, the proportion of people with diabetes in the total population increased from 5.9 to 8.9% between 1989 and 2007. This increase is mainly caused by an increased prevalence of type 2 diabetes.
An increase was also observed on the basis of the representative survey and examination data from the 1998 Federal Health Survey (GNHIES98) and the DEGS study from 2008 to 2011 (DEGS1): in 1998, 4.7% of men and 5.7% of women knew that they suffer from diabetes; in 2008/11 this was the case for 7.0% of men and 7.4% of women. Overall, there was an increase in known diabetes from 5.2 to 7.2% between these two studies. A good third of this increase results from the aging of the population.
For unknown reasons, the rate of children newly diagnosed with type 1 diabetes is increasing by three to four percent annually. Every year around 3000 children in Germany are diagnosed.
Prevalence by age group
Diabetes mellitus is more common among older people than among younger people: While among those insured with the AOK in Hesse in 2004 in the 40–59 year old age group only approx. 4–10% suffered from diabetes mellitus, the proportion was in the 60 age group Years or older between 18 and 28%.
In the Germany-wide representative DEGS study 2008/11, there were 2% men and 4.5% women among 40 to 49 year olds who were known to have diabetes; in the age group of 70 to 79 year olds it was around 22%.
Prevalence and incidence of type 1 diabetes in children and adolescents
Approx. In 2007, 15,000 children and adolescents up to 14 years of age in Germany suffered from type 1 diabetes. Between 2100 and 2300 new cases are registered in this age group every year. Several studies have shown an increase in the incidence of type 1 diabetes by 3–4% per year. In 2010 there were around 32,000 patients under the age of 20 living with type 1 diabetes in Germany.
Worldwide development for type 1 diabetes
Type 1 can appear for the first time at any age, and an aged person can still develop type 1 LADA . In 2003 , the International Diabetes Federation (IDF) estimated the worldwide prevalence of the child population at around 430,000 of the total of 1.8 billion children, which is slightly more than 0.02%
The incidence - that is the rate of new cases - is increasing worldwide. Worldwide, 65,000 new cases are known each year, the annual rate of increase is estimated at 3%.
The country with the highest known incidence of type 1 diabetes to date is Finland . However, the rate of new cases among those under 15 has not increased further, at least in the last 15 years. Researchers associate this with vitamin D fortification in milk.
Distribution, socio-medical and economic importance
Diabetes mellitus - mainly related to type 2 - has become a widespread disease worldwide. The IDF speaks of the "epidemic of the 21st century". The worldwide numbers (projections) are increasing rapidly and the forecast estimates are constantly being revised upwards.
| year | People with diabetes worldwide (estimate interval) |
Share of the world population | estimate | source |
|---|---|---|---|---|
| 1980 | 153 million (127–182) | Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group | ||
| 1994 | 110 million | 2010: 239 million | International Diabetes Institute | |
| 1995 | 135 million | 2025: 299 million | WHO | |
| 2000 | 150 million | 2025: 300 million | ||
| 2003 | 194 million | 5.1% | 2025: 333 million (6.6%) | IDF Diabetes Atlas 2003 |
| 2006 | 246 million | 6.0% | 2025: 380 million (7.3%) | IDF Diabetes Atlas 2006 |
| 2008 | 347 million (314-382) | Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group | ||
| 2010 | 285 million | 6.4% | 2030: 439 million (7.7%) | IDF Diabetes Atlas 2009 |
| 2013 | 382 million | 8.3% | 2035: 592 million | IDF Diabetes Atlas 2013 |
| 2019 | 463 million | 9.3% | 2045: 700 million | IDF Diabetes Atlas 2019 |
The island state of Nauru in the Pacific has the largest proportion of diabetics in the world . The highest number of type 1 diabetics in children has (as of 2013) Europe.
Diabetes is not equally common in different social classes. Diabetes is more common in the lower class than in the middle or upper class.
In Germany in 2007, 20% of the expenditures of the statutory health insurance were used for the treatment of diabetes and its accompanying and secondary diseases. The expenditure for the treatment of diabetes and its consequences in 2005 amounted to around 25 billion euros. Diabetes (types 1 and 2) is one of the most frequent consultation occasions in general medical practices.
The cost situation for type 2 diabetics is as follows: According to the CODE 2 study in Germany in 1998, the total economic costs resulting from type 2 diabetes amounted to 16.05 billion euros (31.4 billion DM ) . Of these, carrying statutory and private health insurance companies the lion's share with 61%.
A patient with type 2 diabetes caused depending on its complication status (through the secondary diabetes diseases caused) 1,3- ( no complications) to 4.1-fold ( macro- and microvascular complications) higher cost than average for statutory health insurance output becomes. Half of the total costs are caused by inpatient treatment, a further 27% of the expenses are attributable to drug treatment (of which insulin and oral antidiabetic drugs: 7%) and finally 13% to outpatient treatment.
A significant proportion of the diabetes-related complications and the associated health care expenditure could be avoided by offering early detection and prevention of type 2 diabetes. A current health economic analysis based on a Monte Carlo microsimulation model shows that such an offer could not only be implemented cost-effectively within the framework of the German statutory health insurance . Rather, absolute savings for the health system can be expected on average for all diabetics. The diabetics supported in this way benefit from an improved quality of life, a lower frequency of complications and a higher life expectancy compared to the status quo of diabetes diagnosis and therapy in Germany.
A more recent study on the same topic shows that starting from a fasting blood sugar of 105 mg / dl, according to an economic cost-benefit calculation, inclusion in a prevention program with lifestyle intervention is cost-effective.
Diagnosis
criteria
| classification | Fasting blood sugar (venous / plasma-referenced) | Blood sugar in the oGTT after 2 hours (venous) |
|---|---|---|
| normal | <110 mg / dl <6.1 mmol / l |
<140 mg / dl <7.8 mmol / l |
| Abnormal Fasting Glucose (IFG) |
≥110– <126 mg / dl ≥ 6.1– <7.0 mmol / l |
<140 mg / dl <7.8 mmol / l |
| Impaired glucose tolerance (IGT) |
<126 mg / dl <7.0 mmol / l |
≥140– <200 mg / dl ≥7.8– <11.1 mmol / l |
| Diabetes mellitus | ≥126 mg / dl ≥7.0 mmol / l |
≥200 mg / dl ≥11.1 mmol / l |
| Blood sugar control | Metabolism healthy |
Well | moderate (measures recommended) |
Bad (action required) |
|---|---|---|---|---|
| BG before meals or on an empty stomach in mmol / l (mg / dl) |
3.6-5.6 (65-100) |
5-8 (90-145) |
> 8 (> 145) |
> 9 (> 162) |
| BG after eating in mmol / l (mg / dl) |
4.5-7.0 (80-126) |
5-10 (90-180) |
10-14 (180-250) |
> 14 (> 250) |
| BG at night in mmol / l (mg / dl) | 3.6-5.6 (65-100) |
4.5-9 (80-162) |
<4.2 or> 9 (<75 or> 162) |
<4.0 or> 11 (<70 or> 200) |
| HbA 1c value (standardized value according to DCC trials) |
<6.05 | <7.5 | 7.5-9.0 | > 9.0 |
According to the definition of the World Health Organization (WHO) from 1999, diabetes mellitus is present if one of the following criteria is met ( glucose measured in the blood plasma, venous):
- Fasting blood sugar ≥ 126 mg / dl (7 mmol / l)
- Blood sugar ≥ 200 mg / dl (11.2 mmol / l) two hours after the administration of 75 g glucose in the oral glucose tolerance test ( oGTT )
- Blood sugar ≥ 200 mg / dL (11.2 mmol / L) in a random blood sample.
To make a diagnosis, either a defined elevated blood sugar value must be present at least twice (on an empty stomach above 126 mg / dl or after a meal (= postprandial) above 200 mg / dl for random checks) or a pathological oral glucose tolerance test .
It should be noted that different limit values apply to the various materials (capillary blood or venous blood, measurement in plasma or whole blood ). The measurement should be made as soon as the blood is taken. Only quality-assured measuring systems may be used. Blood glucose meters for self-monitoring of blood glucose must not be used for diagnostic purposes. In the case of serum glucose, due to in-vitro glycolysis, the possibility of incorrectly low measured values must be expected. Serum samples for determining blood sugar without the addition of glycolysis inhibitors must therefore not be used (see practical guidelines of the German Diabetes Society ). Finally, clinical pictures that can temporarily lead to increased blood sugar levels as a side effect must be ruled out.
Both the German Diabetes Society and the US Diabetes Association regard glycated hemoglobin as a relevant diagnostic marker, provided that it has been determined according to an internationally standardized procedure:
- Glycated hemoglobin (HbA 1c ) ≥ 6.5% or ≥ 47.5 mmol / mol.
Laboratory diagnostics
HbA 1c
The HbA 1c value is a long-term blood sugar value that can be used to determine the average blood sugar level over the last six to ten weeks. This is the portion of the red blood pigment ( hemoglobin ) that is associated with glucose. The HbA 1c value was previously given in percent, now in mmol / mol (see below). The more glucose there is in the blood, the more blood pigment is saccharified. This initially creates an unstable intermediate product, which is converted into an irreversible end product after a few hours. Short-term blood sugar peaks are therefore hardly reflected in the HbA 1c . In healthy people, the value is around 4–6%. Since the normal ranges for the HbA 1c value differ from laboratory to laboratory, the respective standard range of the laboratory must also be specified with the value. In diabetes therapy, the goal is to achieve an HbA 1c value that is as close as possible to the normal range (target value: 6.5–7.5% or 48–58 mmol / mol), since then there is extensive protection against consequential damage .
- Measurement method and unit
The international diabetes organizations have agreed on a new standard that is supposed to be more precise and will be introduced worldwide. The HbA 1c values must be given in mmol / mol instead of in percent as before. This regulation has been in effect since 2009 and had a transitional period until March 31, 2010. In practical implementation there are two values: the HbA 1c value in% and the mmol / mol value.
Fructosamines
Sustained high blood sugar levels lead to an accumulation of glucose on proteins (mainly albumin ) - the concentration of fructosamines (also fructosamines ) is proportional to the average glucose concentration during the lifetime of the proteins - with albumin approx. 14 days. It makes sense to determine the fructosamines if the HbA 1c values are inexplicably high or if hemoglobin formation is impaired, e.g. B. after blood loss or kidney disease (since 2009 this value can no longer be determined at the expense of the statutory health insurance).
C-peptide
The so-called C-peptide is a measure of insulin production . The C-peptide is part of proinsulin and is released from the pancreas in the same amount as insulin. Since the C-peptide molecule is much more stable than the insulin molecule (the half-life of the latter is a few minutes), it is easier to determine in the laboratory. The measurement of the C-peptide helps to a limited extent in the differentiation of type 1 (C-peptide less due to increasing loss of β-cells until no longer present after months or years) from type 2 (C-peptide initially increased due to hyperinsulinism or also normal, however, with a long duration of illness, also decreased or no longer detectable).
insulin
The level of the insulin hormone can also be determined directly; the shorter half-life (compared to the C-peptide) makes it suitable for detecting shorter peaks. Together with the determination of the C-peptide it is useful for the clarification of hypoglycaemia factitia . Indirectly, with the help of the fasting insulin level and the fasting blood sugar, insulin resistance can be determined even with normal blood sugar values by calculating the HOMA -IR (Homeostasis Model Assessment for Insulin Resistance). The HOMA-Beta is based on the same calculation model to determine the beta cell function in manifest diabetes.
Urine sugar
Glucosuria : A symptom of the increased blood sugar is the eponymous (see above) "honey-sweet flowing through". This means the excretion of glucose in the urine , which occurs in many people at blood sugar levels around 180 mg / dl (10.1 mmol / l). At these values ( kidney threshold ), the kidneys can no longer keep up with their absorption capacity, and glucose passes into the urine (glucosuria). Likewise, the reabsorption of water is impaired, which leads to increased urine excretion ( polyuria ) with correspondingly high water loss and increased thirst . Since the kidney threshold is relatively different from person to person and also z. B. is changed in acute illnesses or during pregnancy , this measurement method is increasingly abandoned. The costs for the measuring strips are also similar to those for determining blood sugar.
Glucosuria with blood sugar levels below 180 mg / dl (10.1 mmol / l) is called diabetes renalis . This kidney dysfunction, either congenital or acquired, must be differentiated from diabetes mellitus in the differential diagnosis. In particular, diabetes mellitus must not be diagnosed on the basis of a single finding of glucosuria.
Ketones in urine
Ketonuria : When insulin levels are low, the energy reserves of adipose tissue are mobilized. This increases not only the glucose concentration in the blood, but also three even smaller molecules, the so-called ketone bodies . These are also energy sources. Two of them are weak acids. If there is a drastic insulin deficiency, its concentration can rise so much that it leads to dangerous over-acidification of the blood, known as ketoacidosis . Test strips are available to measure one of these ketone bodies, acetone , in the urine. Serious derailments can thus be recognized and treated by those concerned themselves (e.g. in the case of insulin pump wearers, if an unnoticed pump defect has led to a severe metabolic derailment). Third parties can often smell acetone in their breath. The determination - and thus also the prescription and provision of corresponding test strips - is only relevant for type 1 diabetes, since such a pronounced insulin deficiency in type 2 diabetics can only occur after decades of disease and then only very rarely.
Autoantibodies
In type 1 diabetes, autoantibodies against islet cells (ICA = islet cell autoantibodies) can be detected in 80% of cases. These are differentiated into different autoantibodies depending on the target antigen:
- Antibodies against glutamate decarboxylase isoform 65 (GADA): These antibodies are specifically directed against an enzyme in the beta cells and are evidence of type 1 diabetes mellitus, but are only present in 50 to 70 percent of cases when the disease breaks out, and later increasingly less. GADA are typical of type 1 diabetes mellitus in adults.
- Insulin autoantibodies (IAA)
- Antibodies against tyrosine phosphatase IA-2 (IA-2A)
- Antibodies against zinc transporter 8 (ZnT8A)
Diagnostic classification
In the International Statistical Classification of Diseases and Related Health Problems (ICD 10-GM (German Modification)) of the World Health Organization (WHO) there are five categories of diabetes mellitus, namely E10, E11, E12, E13 and E14 .
Type 1 diabetes
When type 1 diabetes is a chronic autoimmune disease with absolute insulin deficiency. The body's own immune system destroys the insulin-producing β-cells in the pancreas as part of an inflammatory reaction known as insulitis . This loss of the β-cells leads to an increasing insulin deficiency. Type 1 diabetes only manifests itself when about 80–90% of the β cells are destroyed. In the initial phase of the disease, there may still be a small residual production of insulin - measurable via the C-peptide .
The insulin deficiency causes the following:
- Glucose can no longer be absorbed into the insulin-dependent tissue or cells. The glucose is lacking in the cells as a source of energy and accumulates in the blood.
- The formation of new glucose in the liver proceeds unchecked. Up to 500 g of glucose are released into the blood per day. Since this cannot be used by the cells (see 1.), it remains in the blood and the blood sugar level rises.
- The body fat can no longer be kept in its depots and is released into the blood. The blood becomes flooded with free fatty acids. Since substrates from the carbohydrate metabolism are necessary for the metabolism of fatty acids , these fatty acids cannot be broken down in the normal way, but are converted into ketone bodies via a secondary route (acetone, beta-hydroxybutyric acid, acetoacetic acid). Since both the free fatty acids and these ketone bodies (with the exception of acetone) are acids, the blood becomes excessively acidic ( ketoacidosis ), which affects all metabolic processes in the body.
- Assuming healthy kidney function, reabsorption in the tubules is impaired after the kidney threshold is exceeded, so that glucose is excreted in the urine ( glucosuria ). In order to be able to excrete the accumulating glucose, it has to be removed from the body via the increased diuresis . There is constant urination (= polyuria ) and as a result dehydration (dehydration state) with constant compulsion to drink ( polydipsia ), otherwise (terminally) desiccosis (dehydration) occurs.
In summary, a lack of insulin results in a lack of substrate in the cells, a rise in blood sugar, a loss of water and nutrients, an overacidification of the blood and weight loss. In extreme cases, it can lead to a life-threatening clinical picture - the ketoacidotic coma .
For type 1 diabetics, treatment with insulin is essential (ketoacidosis can start to develop after just eight hours without insulin).
causes
The development of type 1 diabetes mellitus is understood today as a multifactorial event in which both genetic and environmental factors are involved. Epidemiologically, an increase in the disease can be determined worldwide: According to the EURODIAB registry data (2018), the incidence of type 1 diabetes in Europe is increasing by 3.4% per year, especially in Poland (6.6%). An increase of 1.8% was recently reported for the USA and an increase of 1.3% for Canada. The increase in China is particularly dramatic at 12% / year.
There are indications that the rotavirus vaccination , which has been recommended for small children since 2013, could also have a protective effect against the autoimmunologically mediated development of type 1 diabetes. Evidence for this emerges from a time series analysis of an Australian study from the period 2000–2015, which documents a downward trend in type 1 diabetes since the introduction of rotavirus vaccination in 2007. A similar study carried out in the USA of the health data of almost 1.5 million privately insured children and adolescents (observation period 1 to 16 years) between 2001 and 2017: the mean incidence rate for type 1 diabetes was 0.122 over the period 2006-2017 (per 1000 person-years) with complete multiple vaccination - but not with incomplete vaccination series (0.205) - significantly lower than without vaccination (0.206). There was also a decrease in the incidence rate among unvaccinated persons, which was 0.370 over the period 2001–2005 without rotavirus vaccination. A reduced rate from 0.20 to 0.12 means eight fewer cases of type 1 diabetes per year for 100,000 fully vaccinated children in absolute terms.
In children with type 1 diabetes, the immunological response of known antibodies against the islet cells of Langerhans in the pancreas (GAD65 / anti-IA-2) correlates with the IgG titre against rotaviruses. A similar mechanism of action is also used with other enteroviruses and their vaccination, such as. B. the Coxsackie B viruses, suspected.
Genetic causes
To date, more than 50 genes have been identified that have been shown to be associated with the development of type 1 diabetes. Most of the genetic changes described result in a polygenetic origin, i. H. several genetic changes must be present for type 1 diabetes to develop. A monogenic disease is only present in rare cases .
In particular, genetic changes in the short arm of chromosome 6 , the so-called MHC region , were responsible for the development of type 1 diabetes mellitus. The HLA-A and HLA-B genes in this region contain the genetic information for proteins on the surface of body cells, which the body's immune system also uses as a basis for differentiating it from non-body cells. Genes outside the HLA complex probably play a much smaller role in the genesis of type 1 diabetes. These include the gene for insulin (INS) and the gene CTLA4, which is responsible for T-lymphocyte regulation. Type 1 diabetes occurs most between the ages of 11 and 13 and is therefore also called juvenile diabetes .
Environmental factors
An autoimmune reaction occurs when the immune system is exposed to an antigen that is foreign to the body and resembles or resembles an endogenous surface protein. The resulting immune response is directed both against the foreign antigen and against the body's own proteins on the islet cells of the pancreas ( cross-reactivity , molecular mimicry ). In addition, it is assumed that exposure to foreign antigens, especially in the first few months of life, has an immunomodulating effect that can promote the development of type 1 diabetes. Correlations could be proven for the following environmental factors:
- Caesarean section : Scientists from the Diabetes Research Group at the Institute for Diabetes Research at the Helmholtz Center in Munich under the direction of Anette-Gabriele Ziegler investigated the influence of environmental factors on the development of the disease in 1,650 children from risk families in a long-term study. According to this, the risk for children of diabetic parents of developing diabetes up to the age of 12 after a caesarean section is twice as high at 4.8 percent as after a natural birth (2.2 percent). Study participants were followed for an average of 11 years from birth. The researchers see one explanation in the fact that delivery by caesarean section changes the composition of the child's intestinal flora and thus promotes the development of autoimmunity. Caesarean section was identified as the greatest known extra-genetic individual risk for diabetes-1, but it must always be seen in connection with other simultaneously occurring factors.
- Diabetogenic (diabetes-causing) viruses : Coxsackie B viruses (especially B4), intrauterine rubella infection ( occurring in the uterus during pregnancy ) with rubella virus (leads to diabetes in 50%), echoviruses , cytomegalovirus (CMV), herpes viruses . According to the results of the international TEDDY study (The Environmental Determinants of Diabetes in the Young) , however, a causal virus infection has proven to be relatively unlikely.
- Insulin-like structures on antigens . They trigger the immune system's attack on the pancreas. Lymphocytes of type 1 diabetics have been shown to react to a certain part of the insulin protein.
- Bafilomycins, which are formed by streptomycetes in the rotten areas of root vegetables (potatoes, carrots) in particular: in animal experiments, bafilomycin A1 causes glucose intolerance even in nanogram quantities and damages the islets of Langerhans in the pancreas. Bafilomycin B1 also disturbed the development of the islets of Langerhans in a minimal amount in pregnant mice and led to an increase in type 1 diabetes in the offspring.
- Vitamin D deficiency: Vitamin D supplementation in young children not only prevents rickets , but can also reduce the risk of diabetes later on. Children who received high doses had the lowest risk of developing the disease. The incidence of type 1 diabetes in industrialized countries has almost doubled since 1990 . Countries with low UVB solar radiation have a high rate of new cases.
- A German study showed that especially respiratory infections in infancy can be associated with later type 1 diabetes mellitus. While the diabetes manifestation occurs much later, the autoantibodies responsible for it can often be detected at an age of 6 months to 3 years.
The following environmental factors are discussed:
- The consumption of cow's milk in the first three months of life in children with only a short period of breastfeeding. The background to this is the hypothesis that early exposure to foreign dietary proteins could interfere with the development of normal oral tolerance and promote antibody production to dietary proteins, which then cross-react with β-cell antigens.
- The very early exposure to the protein gluten found in various types of grain. A special intestinal flora resulting from gluten consumption is suspected to be the cause of the development of hyperglycaemia and type 1 diabetes in mice.
In large cohort studies , no statistical relationship was found between the length of breastfeeding and the risk of islet cell autoimmunity or type 1 diabetes. According to current knowledge, the age at which cow's milk is introduced into infant nutrition is not associated with the risk of islet cell autoimmunity or type 1 diabetes. The international, double-blind, randomized TRIGR study found no effect of delaying cow milk feeding on the risk of type 1 diabetes.
Symptoms
Characteristic of the manifestation of type 1 diabetes is the pronounced weight loss within days to a few weeks, combined with dehydration ( desiccosis ), constant feeling of thirst ( polydipsia ), frequent urination ( polyuria ), vomiting and occasionally also cramps in the calves and abdominal pain. There are also general symptoms such as tiredness , lack of drive and powerlessness, reduced performance, erectile dysfunction, depressive moods, cravings, sweating, visual disturbances and poor concentration. Headaches are also not uncommon.
therapy
In type 1 diabetes, the missing hormone insulin has to be supplied artificially in the form of insulin preparations , see insulin therapy . The aim of this insulin therapy is not to cure type 1 diabetes, but to replace the body's missing insulin. Therefore, the therapy must be carried out continuously until the end of life. Therapy for healing is not yet available.
- See also: Blood Glucose Awareness Training
New approaches to research
Continuously measuring glucose sensors alone or in combination with an insulin pump as an artificial pancreas make it possible to apply insulin and, if necessary, carbohydrates for therapy control by the patient himself or via an automatic control algorithm using an insulin pump. The latter is still in the experimental stage. Continuous blood sugar measurement is technically mature. In Germany, it is currently paid for by statutory health insurances under certain conditions.
Heredity
The above mentioned mutation of the 6th chromosome can be inherited over several generations. The likelihood of developing type 1 diabetes depends on the type of inheritance (see table below).
| collective | Risk [%] |
|---|---|
| General population | 0.4 |
| Relatives of a patient with type 1 diabetes | |
| parents | |
|
8th |
|
3 |
| siblings | |
|
33 |
|
15th |
|
5 |
|
1 |
Type 2 diabetes
This is a disorder in which insulin is present at its target location, the cell membrane, but cannot work properly ( insulin resistance ). In the first few years of the disease, the pancreas can compensate for this by producing high amounts of insulin. At some point, however, the pancreas can no longer maintain the excessive production of insulin. The amount of insulin produced is then no longer sufficient to control the blood sugar level , and type 2 diabetes mellitus becomes manifest. A type 2 diabetic produces much more insulin in the body than a person with healthy metabolism (hyperinsulinism), but due to a high level of insulin resistance, the blood sugar still rises; later on, a relative deficiency leads to an absolute insulin deficiency in some cases. The Selfish Brain Theory provides a possible explanation of the complex regulation of blood sugar and lipid metabolism by the hypothalamus , with the aim of always making enough glucose available to the brain.
In the 1990s, type 2 diabetes was still playing down the nickname of old- age diabetes because it usually only appeared in older people. However, type 2 diabetes is also being diagnosed in more and more younger people. MODY diabetes is becoming increasingly common in children and adolescents . Due to the occurrence in younger years and the risk of developing massive damage to health in the course of life, the term “adult diabetes” is no longer appropriate.
Type 2 diabetes is often diagnosed late, not taken seriously, or inadequately treated, and doctors can sometimes be unsure about treatment. Even the patients often tend to repress themselves, despite education and training, since noticeable health impairments often only occur when acute, sometimes irreversible damage manifests itself. In order to achieve consistent quality, the statutory health insurance companies in Germany have been promoting uniform diagnosis and therapy guidelines as part of the Disease Management Program (DMP) since 2003 .
The German Medical Association , the National Association of Statutory Health Insurance Physicians and the Association of the Scientific Medical Societies give national supply guidelines u. a. for type 2 diabetes mellitus. These guidelines are evidence-based medical decision-making aids for structured medical care (disease management, integrated care).
causes
Type 2 diabetes is also a multifactorial disease. The most important factors in the development of this type of diabetes are insulin resistance with secondary hyperinsulinemia and impaired insulin secretion. The main cause is obesity. Its influence is changed by the genes and other possible factors.
Obesity
Obesity is considered to be one of the main causes of this type of disease. In particular, excessive belly fat around internal organs such as the liver or pancreas, caused by a diet that is high in fat and sugar, is a risk factor. In addition to the innate insulin insensitivity, the excess weight results in an additional insulin resistance of the insulin-dependent body cells. If such a cell is stimulated with insulin in healthy people, an increased number of glucose transport proteins of type 4 ( GLUT-4 ) are inserted into the cell membrane. In type 2 diabetics, this mechanism is disrupted, among other things. GLUT-4 is downregulated in your muscle and fat tissue. The exact mechanism of insulin resistance is so far unclear; however, it is not a defect in the GLUT-4. There is a connection between the concentration of the messenger substance Retinol Binding Protein 4 (RBP-4) and the extent of insulin resistance. RBP-4 is produced in excessive quantities in the adipose tissue of overweight people. This messenger substance seems to lead to the fact that muscle and liver cells hardly react to the blood sugar regulating hormone insulin. If the insulin resistance improves after physical training, lower RBP-4 plasma levels should also be measured (for the therapeutic consequences, see Therapy - New Research Approaches ).
However, diet plays a role in the risk of developing diabetes mellitus II not only in terms of body weight. For example, a study from 2013 indicated that the consumption of fruit juices increases the risk of developing diabetes, while the consumption of fresh fruit - especially blueberries , grapes and apples - has a reduced rate of diabetes-type 2 diseases. Mediterranean diets are recommended for diabetes. In a complex analysis, the researchers evaluated the data from 4,937 study participants from 56 nutrition studies.
Genetic factors
70 to 80 percent of the children of parents who both have type 2 diabetes also develop diabetes as adults. Genetic predisposition is a decisive factor, and many genes are likely to be involved (polygenic disease). The different genetics are probably the reason for the different course forms. In 2004, researchers at the Baptist Medical Center at Wake Forest University ( USA ) succeeded in identifying one of the genes involved: PTPN1. The on human chromosome localized 20 gene encodes for a P rotein t yrosine P hosphatase (N1). There are several variants of the PTPN1 gene: the risky variant is found in around 35% of all individuals in the white (American) population, while the protective (protective) form occurs in around 45%. The neutral variant of PTPN1 is found in around 20% of individuals. If the protein of the risky variant is in abundance in the body, it suppresses the body's insulin reaction, so that more glucose (sugar) remains in the bloodstream and type 2 diabetes manifests itself .
The existence of other genes responsible for type 2 diabetes is considered certain. The researchers estimate that the PTPN1 gene is responsible in around 20% of the fair-skinned population. In African-Americans, on the other hand, the gene does not seem to play a role, further evidence that several genes are involved in the development of type 2 diabetes.
In a study in which the genome of 2,000 people was sequenced, however, it could be ruled out that rare mutations in a few genes are responsible for the majority of diabetes 2 diseases. It follows that either significantly more than 20 genes are involved or that rare mutations play a subordinate role.
Lifestyle factors
Another factor in the disease process is an increased body's own gluconeogenesis (sugar formation) in the liver (see above). The hormone insulin inhibits and the hormone glucagon increases gluconeogenesis in the liver. Glucagon, which raises the blood sugar level by increasing the production of sugar, is increasingly produced in the body's cells in response to the need for sugar. Stress hormones such as catecholamines and glucocorticoids also increase gluconeogenesis physiologically. In addition, the innate insulin resistance also affects the liver cells, which hardly react to the inhibitory effects of insulin and release too much sugar into the blood. In mice, the offspring of stressed fathers often have high blood sugar levels. Stress hormones cause additional methyl groups to attach to a gene in the sperm. This epigenetic mutation leads to uncontrolled sugar production in the offspring's liver.
A high vitamin D level is associated with a halved risk of diabetes, according to a systematic review with 28 studies and a total of almost 100,000 participants. The metabolic syndrome was also only half as common in subjects with high vitamin D levels as in subjects with little vitamin D in their blood. A deficiency in melatonin, which is mainly released at night, appears to increase the risk of type 2 diabetes.
With regard to the risk of developing type 2 diabetes, a cohort study showed that with each year of breastfeeding, the risk of these women developing this form of diabetes decreased by around 15 percent. After weaning, the protective effect lasts for a few years.
The enzyme heme oxygenase -1 (HO-1) has attracted attention in research on type 2 diabetes. With regard to wound healing , stressed bodies or illness in connection with lack of exercise, it is suspected to cause excessive levels of HO-1, which further worsens the state of health. As a result, HO-1 leads to an increased production of HO-1. It has not been researched whether HO-1 is a consequence or the possible cause of type 2 diabetes.
Symptoms
Many type 2 diabetics have had no tangible symptoms for years. In contrast to type 1 diabetes, type 2 diabetes is rarely associated with weight loss and only with massively increased blood sugar levels with increased urination and a feeling of thirst. At the beginning there are often unspecific symptoms such as tiredness, weakness, visual disturbances and a tendency to infection (bacterial infections and fungal infections) such as B. frequent bladder infections, genitoanal pruritus , in men recurring inflammation of the glans and / or the foreskin with possible development of a secondary phimosis .
Since these symptoms are very unspecific, the diagnosis is often made by chance only after years. A so-called hyperosmolar syndrome up to hyperosmolar coma is rare but possible . This happens when the kidneys excrete so much water when the blood sugar level is extremely high that the fluid loss can no longer be compensated for by drinking.
Therapy and prevention
In type 2 diabetes, the increased insulin resistance can u. a. can be reduced through weight loss and increased exercise. Until 2009, the German Diabetes Society demanded in its guidelines that drug therapy should only take place after these measures have been exhausted. In every patient who loses excess weight, the percentage of blood sugar decreases more significantly than the blood pressure. About half of all newly diagnosed diabetics achieve remission by losing 10 kg (normal fasting blood sugar). These findings suggest a comprehensive lifestyle change for overweight diabetics, which, however, requires a high level of motivation and is difficult to realize for many patients.
There are numerous studies on the effectiveness of lifestyle changes in preventing type 2 diabetes mellitus. However, these also show that patients are more likely to accept medication than a change in lifestyle (and thus do not differ from people with other chronic diseases - see, for example, the lung disease COPD and smoking ).
According to current studies, lightly strenuous exercise for at least 30 minutes at least three times a week is necessary to avoid metabolic disorders such as B. to prevent or sustainably influence diabetes.
New studies for metformin show that early drug initiation delays the development of the disease because the underlying insulin resistance is reduced from the time the diagnosis is made. For the new DPP4 inhibitors , too , initial studies show that the functionality of the B cells in the pancreas may be preserved for longer if treatment is started early (from symposia at the 45th German Annual Meeting of the German Diabetes Association in Stuttgart 2010).
A study with an active ingredient from the group of glitazones showed that this active ingredient significantly reduced the risk of the disease progressing in people with a preliminary stage of type 2 diabetes mellitus . In a group treated with rosiglitazone for three years, less than half as many participants fell ill as in a comparison group that received only a dummy drug . However, heart failure was significantly more common with rosiglitazone . The approval is currently suspended.
There are various therapeutic approaches for drug therapy (see below). The better it is possible to normalize blood sugar levels (before a meal below 120 mg / dl, then below 180 mg / dl), the lower the risk of complications.
Since type 2 diabetes, as part of the metabolic syndrome, is often associated with high blood pressure and the high blood pressure further exacerbates the long-term effects, especially in the eyes, kidneys and large blood vessels, high blood pressure must be recognized and treated in good time. With regard to macrovascular risks such as heart attack or stroke, in particular, optimal blood pressure adjustment is even more important than optimization of the sugar metabolism. For the microvascular risks to the eyes and nerves, however, optimizing blood sugar is considered more important.
Even with type 2 diabetics, regular self-monitoring of blood sugar levels helps to sustainably adhere to a change in lifestyle. The ROSSO study has shown that there is a significant decrease in secondary diseases and a significant reduction in the death rate.
A surgical removal or bypass of the stomach and the upper part of the small intestine ( anti-diabetic intestinal bypass , ADIB) can lead to improved metabolic levels in obese diabetic type 2nd The operation is fraught with various risks, the mortality rate during the operation is one percent (see also bariatric surgery ).
Step-by-step plan of drug therapy for type 2 diabetes in accordance with the 2013 National Care Guideline
| DEGAM / AkdÄ | DDG / DGIM | |
|---|---|---|
| Level 1 basic therapy |
|
|
| Stage 2 monotherapy |
If, after three to six months, the basic therapy alone does not reach an HbA1c value in the target range, therapy begins with metformin . |
|
|
subordinate meaning:
|
|
| Level 3 insulin or two combinations |
If after three to six months with basic measures and monotherapy an HbA1c value in the target range is not achieved, the combination therapy consisting of metformin and |
|
Alternatively insulin alone |
(alphabetical order) |
|
| Level 4 Intensified (re) insulin and combination therapy |
If after three to six months the combination therapy alone does not reach an HbA1c value in the target range, intensified (more) insulin and combination therapy is used. |
|
|
In addition to oral therapy, especially with metformin, possibly DPP4 inhibitor, SGLT-2 inhibitor
|
|
Oral anti-diabetic drugs
- Acarbose : A special sugar that reduces the absorption of glucose from the intestine by inhibiting enzymes.
- Biguanide : first choice. Functional mechanism, including inhibition of the formation of new glucose in the liver, has not yet been clearly clarified. The only authorized representative is metformin .
- Glinide : Increases the insulin secretion from the pancreas ( nateglinide and repaglinide ) independent of food intake .
- DPP-IV inhibitors : inhibition of the breakdown of glucagon-like peptide 1 (GLP-1) and thus increased secretion of insulin from the pancreas depending on food intake (including linagliptin , sitagliptin ).
- Insulin sensitizer or glitazone: Increasing the sensitivity of the cells of the liver, muscles and adipose tissue to insulin ( pioglitazone , rosiglitazone ).
- SGLT-2 inhibitor : Promotion of glucose excretion via the kidneys by inhibiting the return of sugar from the primary urine ( dapagliflozin , canagliflozin , empagliflozin ) and (still in clinical testing ) ertugliflozin . In type 2 diabetics, canagliflozin was able to significantly slow the progression of chronic kidney disease in a CREDENCE study. Nephrologists speak of a milestone. In addition to standard therapy (RAAS blockade with ACE inhibitors), it can significantly slow the progression of chronic kidney disease (CKD).
- Sulphonylureas : Increase in food intake-independent insulin release from the pancreas via mechanisms other than glinides (including glibenclamide , glimepiride ).
Non-oral anti-diabetic drugs
- Incretin mimetics : The active ingredients exenatide , liraglutide, albiglutide and dulaglutide are polypeptides that act in humans like the intestinal hormone glucagon-like peptide 1 (GLP-1). GLP-1 lowers the blood sugar level by stimulating the release of insulin and inhibiting glucagon secretion. Incretin mimetics are injected subcutaneously . In a randomized, placebo-controlled endpoint study, a reduction in cardiovascular events ( stroke and myocardial infarction ) and a slight improvement in prognosis could be demonstrated for liraglutide .
New approaches to research
- Fenretinide , an active ingredient originally created for cancer therapy, led in animal experiments with mice to the fact that the excess enzyme RBP4 was excreted in the urine. The treated animals then lost their insulin resistance.
- Nasal insulins should improve cognitive performance in diabetics without affecting blood sugar. (at least according to an American study).
Heredity
Children of one parent with type 2 diabetes are up to 50% likely to develop type 2 diabetes later. The probability that an identical twin sibling of someone who is already suffering from type 2 diabetes will also develop the disease is approximately 100%.
Comparison of type 1 and type 2 (table)
| Type 1 | Type 2 | |
|---|---|---|
| Frequency in Germany | about 300,000 | Adults (18–79 years): around 4.6 million known (2012), around 1.3 million undetected (2012) |
| Age of manifestation (age) | Children and adolescents, less often adults, but no age limit | Adults (from around 40 years of age), in recent years increasingly also young adults, even adolescents |
| Main causes |
Genetic predisposition , autoimmune process Organic: Destruction of beta cells |
Disturbances of insulin action ( insulin resistance ) and insulin secretion of varying degrees of severity - starting with hyperinsulinism up to secretion failure based on a genetic predisposition . Beta cells only moderately decreased |
| Occurrence / beginning | acute to subacute | mostly creeping |
| Symptoms | Insulin deficiency syndrome : polydipsia (hyper osmolarity increases thirst), polyuria (osmotic diuresis when the glucose kidney threshold is exceeded), weight loss, fatigue, ketoacidosis | often no complaints, there are less severe metabolic imbalances, but more frequent macro and microangiopathies and neuropathies |
| body weight | normal weight or weight loss (if there is a lack of insulin, the build-up of fat and glycogen is limited) | often overweight |
| Insulin secretion | diminished to absent | subnormal to high, qualitatively always disturbed |
| Insulin resistance | none or only little | often pronounced |
| Family accumulation | low | high (over 90% in identical twins) |
| HLA association | available | unavailable |
| Diabetes-associated antibodies | at manifestation 90-95% | no |
| metabolism | unstable | initially stable, unstable if insulin secretion fails |
| treatment | Training and motivation, lifelong insulin therapy | Training and motivation, regular exercise, adapted diet, oral anti-diabetic drugs if required, additional insulin therapy if required |
Other specific types of diabetes (type 3 diabetes)
The 1999 WHO classification lists eight categories under “Other specific types of diabetes”. Unofficially, they are sometimes also referred to as type 3 diabetes.
A: genetic defects of the beta cell
- MODY , 11 known forms so far
- Mutation of mitochondrial DNA 3243 (point mutation A3243G), mitochondrial diabetes (MIDM)
- neonatal diabetes mellitus (NDM, homozygous MODY forms and mutations of KCNJ11 or ABCC8)
- other
B: genetic defects in the action of insulin
- Type A insulin resistance
- Leprechaunism
- Rabson-Mendenhall Syndrome
- Lipathrophic diabetes
- other
C: pancreas is diseased or destroyed ( pankreopriver diabetes)
- Fibrocalcular pancreatopathy
- Pancreatitis
- Trauma , see pancreatic rupture and duodenopancreatectomy
- Neoplasia
- Cystic fibrosis
- Hemochromatosis
- other
D: diabetes due to hormonal disorders (endocrinopathies)
- Cushing's Syndrome
- Acromegaly
- Pheochromocytoma
- Glucagonoma
- Hyperthyroidism
- Somatostatin
- Aldosterone
- other
E: Diabetes from drugs or chemicals
- Nicotinic acid
- Glucocorticoids
- Antipsychotics
- Thyroid hormones
- Sympathomimetics
- Thiazides
- Dilantin
- Pentamidine
- Streptozocin
- Vacor
- Interferon alpha therapy
- other
Q: Infections as a cause of diabetes mellitus
- Congenital rubella
- Cytomegalovirus
- other
G: unusual forms of immune-mediated diabetes
- Insulin autoimmune syndrome (insulin antibodies)
- Antiinsulin receptor antibody syndrome
- other
H: other genetic syndromes associated with diabetes
- Down syndrom
- Friedreich's ataxia
- Chorea huntington
- Klinefelter Syndrome
- Laurence-Moon-Biedl-Bardet syndrome
- Type 1 myotonic dystrophy
- Porphyria
- Prader-Willi Syndrome
- Turner Syndrome
- Wolfram syndrome or DIDMOAD syndrome
- other
Diabetes mellitus and pregnancy (type 4 diabetes)
to form
A distinction is made between diabetes mellitus in the mother, which existed before the start of pregnancy, and diabetes, which is first diagnosed during pregnancy (see also gestational diabetes ).
With the previously known diabetes mellitus, an optimal metabolic control should be aimed for before the start of pregnancy in order to prevent child complications in particular. Diabetes-related diseases in women should be identified and treated beforehand (e.g. laser therapy for proliferative diabetic retinopathy ). Pre-existing damage to the eye may increase during pregnancy.
In the case of gestational or gestational diabetes (also known as type 4 diabetes ), early diagnosis is important, as excessively high blood sugar levels can lead to serious diseases of the embryo or fetus .
Macrosomia (oversized fetus) is characteristic of insufficient diabetes control during pregnancy . Therefore, the attending gynecologist regularly performs an ultrasound of the fetus, whereby the child's abdominal circumference in particular can provide an indication of pathological weight gain.
therapy
In the case of diabetes during pregnancy, blood sugar regulation must be particularly strict, especially in the interests of the child. The maternal blood glucose values to be achieved during pregnancy are well below the values outside of pregnancy (target: below 90 mg / dl on an empty stomach, below 140 mg / dl 2 hours after a meal). In pregnancy, during the phase of organogenesis of the embryo, it should be noted that in this phase, even in a non-diabetic woman, a fundamentally lower blood sugar level will be measured than during the other phases of life and pregnancy. One possible reason is the vessel size of the developing organs of the embryo. If the daily mean blood sugar value is more than 110 mg / dl (6.2 mmol / l), a disordered organ formation or immature organs, especially the child's lungs, are to be expected. If this cannot be achieved through diet, insulin therapy is necessary. Oral antidiabetic drugs are not approved for pregnant women in Germany.
Depending on the child's abdominal circumference measured sonographically, the mother's diabetes therapy can be relaxed (lack of or insufficient growth) or intensified (too rapid increase in abdominal circumference).
Pre-existing hypertension must be treated further with medication. To protect the child, the medication should be checked and changed if necessary. As a first-line drug is considered alpha-methyldopa , then metoprolol or hydralazine .
Diabetes diet
Diet for Type 1 Diabetes
According to the German Nutrition Society, a balanced diet should cover the energy needs of around 52–53% from carbohydrates, 16–17% from protein and 28–31% from fat and is recommended by them for all people, including diabetics. The normal weight type 1 diabetic can in principle eat normally if he has his blood sugar level under control (including sweets), but an adjustment of the insulin therapy is always necessary. The amounts recommended by the GMA are around 4 grams of carbohydrates per day and kilogram of body weight. Bread units are usually used as the basis of calculation (one BE = 12 g carbohydrates). The term carbohydrate units is also used less frequently (one KE = 10 g carbohydrates). This is intended for faster predictability, but has not caught on because the manufacturers continue to specify BE. The fat and protein content of the food has a clear influence on the rate of increase and the duration of the increase in blood glucose. The diabetic who injects insulin must therefore learn to estimate the effect of insulin on the blood sugar level in relation to the food consumed.
Type 1 diabetics treated with intensive insulin therapy have the opportunity to decide for themselves about the composition of their diet. The bread unit or KE is therefore used today by trained type 1 diabetics only to calculate the carbohydrates consumed and thus the correct insulin dose, instead of - as in the past - the calculation of the meal with regard to the total energy intake. Even in type 1 diabetics with well-adjusted therapy, the excessive supply of energy (see: physiological calorific value ) leads to obesity. Example: A pretzel has 2 units with a calorific value of approx. 540 kJ (= 130 kcal ). A butter pretzel only has 2 BU, but a calorific value of approx. 1,250 kJ (= 300 kcal). An excess in the energy balance leads to overweight in the long term.
Diet for Type 2 Diabetes
The general principles of a healthy diet apply to type 2 diabetics : adapted to the actual calorie requirement, high in fiber, wholesome, plenty of fresh fruit and vegetables, alcohol in moderation. Whole grain products and fiber-rich light carbohydrate components such as beta-glucan barley and beta-glucan-rich barley baked goods, barley flakes or barley muesli are suitable for a high-fiber diet. Beta-glucans from barley may significantly reduce the rise in blood sugar after meals, associated with a decreased insulin secretion when the meal 4 g beta-glucan from barley or oats per 30-80 g carbohydrates. A Scandinavian study shows a possible preventive effect of beta-glucan from barley against diabetes via the microbiome when consuming barley bread. Only depending on complications ( hyperglycemic metabolic imbalances , obesity , significant lipid metabolism disorders , significantly increased uric acid , additional diseases such as hypertension , circulatory disorders , advanced renal insufficiency , liver diseases, etc.) are appropriately adapted diet recommendations.
Dietetic foods
Special diabetic foods can negatively affect the development of the disease. The advantage of the reduced carbohydrate content is canceled out by the increased content of fats, which can have a negative effect on weight control. The replacement of granulated sugar ( sucrose ) by fruit sugar (fructose) with the advantage of insulin-independent metabolism is not considered a sensible measure due to health risks. The professional associations have been trying for years to ban food for diabetics. In September 2010 the German Federal Council decided to abolish labeling as dietetic food . The transition period for the sale of dietetic foods was two years.
Acute complications
Diabetic coma
The diabetic coma (Latin coma diabeticum ) is the most severe hyperglycemic derailment of diabetes and life-threatening. In the case of a diabetic coma, blood sugar levels can reach over 1000 mg / dl (56.0 mmol / l), especially in type 2 diabetics. In type 1 diabetes, blood sugar levels of over 400 mg / dl for several hours lead to severe over-acidification of the blood (metabolic acidosis ). Such a coma can e.g. B. from infections or, in the case of insulin-injecting diabetics, from defective insulin (e.g. storage below freezing point or above 40 ° C) or technical defects such as B. Failure of the insulin pump can be caused.
Low blood sugar (hypoglycaemia)
Blood sugar lowering drugs such as sulfonylureas and insulin lead to low blood sugar levels if overdosed or if food is not consumed enough.
The symptoms of hypoglycemia arise from the insufficient supply of glucose and from the hormonal and neural reactions to it. They can vary very individually, both between people and depending on the situation. The blood sugar levels at which symptoms are felt also vary greatly between individuals. Depending on the severity of the hypoglycaemia, the symptoms range from mild impairment to unconsciousness ( shock ).
Repeated severe hypoglycaemia has shown in an observational study in type 2 diabetics an increased risk of later development of dementia . With severe hypoglycemia, the dementia rate increases by 26 percent, with two episodes by 80 percent and with three hypoglycemia the dementia rate almost doubles.
Liver disease ( liver failure ) increases the risk and extent of hypoglycaemia. The gluconeogenesis and glucose uptake in peripheral tissues may be disrupted. In addition, these patients develop higher levels of insulin resistance.
Hypoglycaemia is eliminated through the intake of quickly absorbable carbohydrates, e.g. B. Dextrose (1-2 BU) or fruit juice (200 ml). Sugar that is wrapped in fat (e.g. chocolate) or slowly absorbable carbohydrates (whole grain bread) are unsuitable. In the event of severe hypoglycaemia with unconsciousness, the emergency services should be alerted immediately.
Some type 1 diabetics carry an emergency kit with them in the event of severe hypoglycaemia with unconsciousness, which enables admitted laypersons to inject glucagon. However, the emergency services should be informed, as the time until recovery is uncertain.
Misunderstanding symptoms
Both hypoglycaemia and hypoglycaemia can be misinterpreted by other people in everyday life.
- In the case of ketoacidosis , the exhaled air may contain acetone. This can be confused with the smell of alcohol.
- Symptoms of hypoglycemia such as staggering, drowsiness, speech impairment and aggressiveness can be misinterpreted as alcoholism or the influence of drugs.
Because of these misunderstandings, vital aid measures can be omitted.
Concomitant and secondary illnesses
overview

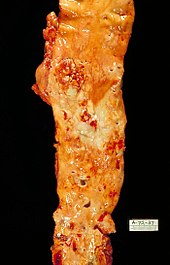

Diabetes mellitus promotes other diseases that can occur as a result of diabetes. The reason for these diseases is often due to the following causes:
- Quality of metabolic control, prolonged high blood sugar levels or frequent severe hypoglycaemia .
- Long-term increased insulin level.
In addition to type 1 diabetes, other autoimmune diseases often occur.
The Diabetes Health Report 2010 gives an overview of the frequency of the occurrence of accompanying and secondary diseases (after 11 or more years) in cared for type 2 diabetics:
- 80.1% hypertension
- 24.1% diabetic retinopathy
- 23% neuropathy
- 12.1% peripheral arterial occlusive disease (PAD)
- 11.1% heart attack
- 9.7% diabetic nephropathy (renal insufficiency)
- 7.4% stroke
- 4.9% diabetic foot syndrome
- 1.7% amputation
- 0.6% blindness
The basis are permanent changes in structure-forming proteins and negative effects of repair processes, e.g. B. the disordered formation of new blood vessels or suppression of the formation of replacement blood vessels in the event of damage. An (infected) pressure ulcer can also be favored by diabetes mellitus.
Even tuberculosis seems to manifest itself more frequently from diabetes. A rare short stature occurs in Mauriac syndrome .
Damage to blood vessels
Damage to small blood vessels
In the microangiopathy leads to circulatory disorders of the small arterial blood vessels can be damaged causing various organs. In particular, these are the eyes, especially the retina ( diabetic retinal disease with rubeosis diabetica ), the kidneys (diabetic nephropathy) and the peripheral nerves (neuropathy).
Damage to large blood vessels
When Macroangiopathy the major arteries are affected, in particular: the Mönckeberg media calcification , the coronary heart disease and peripheral arterial occlusive disease (PAOD).
The formation of deposits and calcification in the vascular walls of the large blood vessels leads to circulatory disorders and stiffening of the vascular wall. With simultaneous polyneuropathy, pain may be absent despite critical blood flow. The possible consequences of circulatory disorders are intermittent claudication , heart attack and stroke .
Women with type 2 diabetes are at higher risk of heart attacks and strokes than men of the same age with type 2 diabetes.
Nerve damage (diabetic neuropathy)
Diabetes is the leading cause of neuropathy . and can damage the nerve pathways called diabetic neuropathy . Sensitive, motor and vegetative nerve fibers can be affected by this. If the vegetative nerves are damaged, one speaks of diabetic, autonomic neuropathy. This leads to an impairment of automatic processes that cannot be deliberately influenced, such as vasodilation, heart rate, bladder and rectal function or sexual functions. This type of neuropathy is often overlooked or misinterpreted in diagnostics.
The pathogenesis of diabetic neuropathy is largely unexplained and probably multifactorial.
Peripheral polyneuropathy
Extensive nerve damage such as polyneuropathy affects around half of diabetics. In particular, long and fine peripheral nerve fibers are destroyed here. This often leads to numbness or tingling in the limbs, especially the feet. However, diabetic polyneuropathy can not only manifest itself in a loss of sensitivity, but also cause abnormal sensations such as pain, burning sensation or over-sensitivity to pain . Around every fifth diabetic is affected by painful diabetic neuropathy (PDN painful diabetic neuropathy), which is often treated symptomatically at the neurotransmitter level. Here, the chronic painful neuropathy is more common than the acutely painful neuropathy. Furthermore, the nerve damage can lead to muscle spasms and loss of reflexes. In advanced disease, nerve-related muscle weakness and muscle wasting as well as the associated motor impairments also occur. Most of the time, the loss of muscle strength begins in the feet and typically manifests itself first as a weakness in the toe lifting and lowering and later in a weakness in the lifting and lowering of the feet. With the help of the Ipswich touch test, those affected can identify nerve damage themselves.
In the drug treatment of painful polyneuropathy, selective serotonin-norepinephrine reuptake inhibitors (SSNRIs), calcium channel blockers , anticonvulsants , antidepressants , metamizole ( novaminsulfon ), paracetamol and topical pain relievers are used.
Along with circulatory disorders, diabetic polyneuropathy is the main cause of diabetic foot syndrome. It is responsible for 50–75% of non-traumatic foot amputations.
Diabetic foot syndrome
The main symptom of diabetic foot syndrome is poorly healing wounds on the lower leg or foot. Since polyneuropathy prevents adequate pain, the smallest injuries are often not noticed. The risk is particularly high with simultaneous circulatory disorders. Daily foot inspection and good foot care are very important and can help prevent damage. Medical foot care ( podiatry ) is indicated in the case of pronounced misalignments of the feet, severe nerve disorders and, above all, if injuries have already occurred . If it is prescribed by a doctor, the statutory health insurance pays the costs. For infections related to diabetic foot syndrome, which can range from a slight superficial infection with intact skin to ulcers and gangrenous wounds to life-threatening infections, oral or parenteral antibiotic therapy is required, depending on the severity.
Amputations
In Germany, over 60,000 amputations are performed every year. This puts Germany in the top third across Europe. About 70% of these amputations are performed on diabetics. Diabetes mellitus is the main cause of amputation in around 30,000 patients.
According to the President of the German Society for Angiology , Karl-Ludwig Schulte, every second amputation due to diabetes in Germany is superfluous. In 2008, Germany had a significantly higher amputation rate than countries such as Finland, Denmark, the Netherlands and Great Britain. In addition, Germany is the only country in which this rate has increased in recent years, while the rate is falling in other countries.
Cause of the high risk of amputation: In poorly controlled diabetes mellitus, sugar molecules accumulate on all structures of the body in the long term. In the legs, this leads to damage to the large and small blood vessels - macro and microangiopathy - and to the nerves, known as neuropathy. Those affected do not recognize injuries to the feet until late, which also heal slowly due to the circulatory disorders.
Diabetic neuropathic osteoarthropathy (DNOAP)
This disease, also known as Charcot's foot , is a non-infectious, inflammatory destruction of bones and joints. It is a special form of diabetic foot syndrome.
Frozen shoulder
Primary stiff shoulder (adhesive capsulitis) is diagnosed in 10–20% of people with diabetes, and 36% if insulin is required. A reason for the increased incidence in diabetes is not known. The incidence of frozen shoulder in people without diabetes is two to five percent.
Eye damage
Eye damage caused by diabetes mainly affects the retina and the cornea . Around 70% of diabetics are affected by keratitis , damage to the cornea that is associated with signs of wear and tear and impaired wound healing processes. The fluid content of the eye lens fluctuates with the blood sugar level , which can aggravate or accelerate a cataract . In diabetic retinopathy there are changes in the small retinal vessels. The consequences range from visual acuity reduction on visual field to blindness . In Germany around 17% of all cases of acquired blindness are due to diabetes.
Kidney damage
The spectrum of diabetic nephropathy ranges from slight protein excretion to kidney failure with dialysis dependence. The risk of nephropathy increases significantly with an increase in blood pressure. Nephropathy in turn can increase "high blood pressure" ( arterial hypertension ). About 30-40% of all diabetics develop nephropathies. The risk increases with the duration and age of diabetes. Men are more often affected than women. Since the kidneys are involved in gluconeogenesis , an important mechanism for regulating blood sugar is disrupted in the event of kidney damage. In patients with impaired kidney function, the need for insulin may be reduced due to reduced insulin excretion and resistance. Most oral anti-diabetic drugs are contraindicated in end-stage renal disease. SGLT-2 inhibitors lose their effectiveness with increasing renal insufficiency.
Lipid metabolism disorders
The type of dyslipidemia (or lipid metabolism disorder) in type 2 diabetes mellitus ( hyperlipidemia , hypercholesterolemia ) is characterized by a particularly high risk of atherosclerotic complications. The impairment of lipid metabolism leads to an increased breakdown of the body's own fat stocks (increased lipolysis ) and new formation of triglycerides in the liver cells (and hypertriglyceridaemia ). This leads to fatty liver disease (steatosis hepatis).
Mouth and gum problems
Diabetics have an up to 3.5 times higher risk of developing periodontitis than healthy people. A preliminary stage is gingivitis , which also occurs more frequently in diabetics, as well as abscesses of the gums , angular mouth ulcers and wound healing disorders after dental treatment. The cause of these problems lies in the different metabolic status and in circulatory disorders in the gums.
cancer
The analysis of six large studies involving 549,944 people revealed that diabetes sufferers versus non-diabetics have an increased risk to cancer becoming ill or die. The risk of cancer increases with the level of blood sugar levels, in men by around 20%, in women by around 30%. The liver , gall bladder and airways, as well as the thyroid and intestines , were particularly often affected in men, and the pancreas , urinary bladder , uterus and stomach in women .
Hearing loss
Studies show a link between diabetes mellitus (DM) and damage to the inner ear. Damage to the small blood vessels ( microangiopathy ) in the inner ear is suspected to be the cause of the reduction in hearing . The symptoms of a slight hearing loss can appear in the otherwise asymptomatic early stage of DM. The prognosis for a sudden hearing loss in DM patients with regard to a complete restoration of hearing is probably due to a microangiopathy of the inner ear, whereby only the factors age and postprandial blood sugar values (postprandial: after the meal) were relevant, but not the current metabolic setting or the duration of diabetes .
osteoporosis
Type 1 diabetes is also responsible for an increased risk of osteoporosis . Among other things, the diabetes disrupts the development and activity of osteoblasts , the cells that are responsible for building bone substance. This leads to a decrease in bone density and thus an increased risk of fractures.
forecast
A significant improvement in the prognosis by reducing the likelihood of secondary diseases (see above) has been proven and confirmed. a. through the DCCT study for type 1 diabetics and the UKPDS study for type 2 diabetics - by lowering blood sugar - and HbA1c values. However, in type 2 diabetes mellitus, the optimal extent of lowering blood sugar is controversial.
People who do not change their lifestyle in accordance with the recommendations (see UKPDS study, Steno-2 study) have an increased risk of secondary diseases.
The saccharification of the cells (measurable on the basis of the non-enzymatic glycation of the red blood cells by the HbA1c value) already forms an irreversible chemical bond with the cell membranes after 2 hours of increased blood sugar value ( Amadori rearrangement ), which is not compensated or reversed by a low metabolism , but can only be stopped in order to avoid secondary diseases. The primary goal of diabetes therapy is therefore to minimize this irreversible chemical reaction of the glucose deposits (AGE- "RAGE" formation process).
The lower the glycation, the greater the chance of a long life free from secondary diseases. Large fluctuations in blood sugar levels reduce this chance. Too low a blood sugar level and too high a level of insulin damages the intima media (inner wall of the blood vessels) just like a too high blood sugar level. It must be determined individually for each affected person how the lowest blood sugar values can be achieved with the lowest number of hypoglycaemia.
For the affected diabetic it is therefore important that he himself become a specialist in his illness and should take responsibility. He has to do the fine-tuning and, if possible, the basal rate determination in everyday life himself, because only he knows and can assess the exact reaction of his body due to the framework conditions (food, exercise, insulin, illness, sport ...). In this respect, the prognosis improves if those affected make an effort about their illness by changing their lifestyle, acquiring and implementing knowledge. The central instrument for this form of " empowerment " is blood sugar self-control .
Prominent examples of successful athletes such as B. Sir Steven Redgrave from Great Britain, who won five Olympic gold medals in rowing, Kris Freeman , the 2006 cross-country skiing champion from the USA, the triathlete and Ironman Jay Hewitt and Matthias Steiner , the 2008 German Olympic champion in weightlifting, prove that despite the illness for many a life with relatively few restrictions is possible. The mountaineers Josu Feijoo (E), Geri Winkler (A; started at the Dead Sea ) and Will Cross (USA) were the first diabetics to reach the summit of Mount Everest within a few days in May 2006 . Nicole Johnson, type 1 diabetic, was Miss America in 1999.
Organs and companies
A number of organs, societies and foundations have set themselves the goal of fighting the spread of diabetes mellitus nationally and internationally and supporting those affected, including:
- WHO
- International Diabetes Federation
- European Association for the Study of Diabetes and European Foundation for the Study of Diabetes
- German Diabetes Society
- German Diabetes Foundation
- German Diabetics Association
- German Center for Diabetes Research
- diabetesDE
- American Diabetes Association
In order to increase awareness of this clinical picture, November 14th has been celebrated as World Diabetes Day since 1991 .
Diabetes mellitus in animals
Diabetes mellitus also occurs in other mammals. The disease is more important in dogs (→ canine diabetes mellitus ) and cats (→ feline diabetes mellitus ).
literature
An overview of the keywords in Wikipedia that deal with topics related to diabetes mellitus can be found in Diabetology .
Overview works
- Society for Rehabilitation for Digestive and Metabolic Diseases e. V. (Ed.): Diabetes Reading Book. Interesting facts for everyday life with diabetes. Pabst Science Publishers, Lengerich 2011, ISBN 978-3-89967-695-2 .
- Burkhard Göke / Klaus G. Parhofer / Carsten Otto: The practice book Diabetes mellitus . Urban & Fischer, Munich a. a. 2002, ISBN 3-437-22930-3 .
- Helmut Schatz , Andreas FH Pfeiffer (ed.): Diabetology compact. Basics and practice. 5th edition. Springer, Heidelberg 2014, ISBN 978-3-642-41358-2 .
- Viviane Scherenberg: patient orientation. Compliance and Disease Management Programs. Practical example of type 2 diabetes mellitus . Publishing house for science and culture, Stuttgart u. a. 2003, ISBN 3-936749-43-4 .
- Matthias B. Schulze, Kurt Hoffmann u. a .: An Accurate Risk Score Based on Anthropometric, Dietary, and Lifestyle Factors to Predict the Development of Type 2 Diabetes. In: Diabetes Care Volume 30, 2007, pp. 510-515, doi: 10.2337 / dc06-2089 (on the German Diabetes Risk Score ) .
- Andreas Thomas: The Diabetes Research Book. New drugs, devices, visions . 2nd revised and expanded edition. Kirchheim + Co, Mainz 2006, ISBN 3-87409-411-1 .
- Hellmut Mehnert, Eberhard Standl, Klaus-Henning Usadel, Hans-Ulrich Häring (eds.): Diabetology in clinic and practice . Thieme, Stuttgart a. a. 2003, ISBN 3-13-512805-9 , also as a Google Book
- Renate Jäckle, Axel Hirsch, Manfred Dreyer : Living well with type 1 diabetes. Workbook for basic bolus therapy. 7th edition. Elsevier / Urban & Fischer, Munich 2010, ISBN 978-3-437-45756-2 .
- Richard Daikeler, Götz Use, Sylke Waibel: Diabetes. Evidence-based diagnosis and therapy. 10th edition. Kitteltaschenbuch, Sinsheim 2015, ISBN 978-3-00-050903-2 .
History of diabetes
- Dietrich von Engelhardt (Ed.): Diabetes: Its Medical and Cultural History. Outlines - Texts - Bibliography. Springer-Verlag, Berlin / Heidelberg / New York 1989, ISBN 3-540-50950-X .
- N. Spyros Papaspyros: The history of Diabetes mellitus. etc. Papaspyros, London 1952.
- Johannes Steudel : The History of Diabetes. In: Diabetics. No. 3, 1953, pp. 45 f., 61 f. and 71 f.
Guidelines
- S3 guideline National care guideline for type 2 diabetes: Training by the German Diabetes Society (DDG). In: AWMF online (as of 2013)
- S3 guideline therapy of diabetes mellitus type 1 of the German Diabetes Society (DDG). In: AWMF online (as of 2011)
- S3 guideline for diagnosis, therapy and follow-up of diabetes mellitus in children and adolescents of the German Diabetes Society (DDG). In: AWMF online (as of 2009)
- S2 guideline nutritional recommendations for the treatment and prevention of diabetes mellitus of the German Diabetes Society (DDG). In: AWMF online (as of 2010)
- S3 guideline on physical activity and diabetes mellitus of the German Diabetes Society (DDG). In: AWMF online (as of 2008)
- S3- guideline drug antihyperglycaemic therapy of diabetes mellitus type 2 of the German Diabetes Society (DDG). In: AWMF online (as of 2008)
- S3 guideline National care guideline type 2 diabetes: Prevention and treatment of retinal complications of the BÄK, KBV, AWMF. In: AWMF online (as of 2010)
- S3 guideline National care guideline for type 2 diabetes: Neuropathy of the BÄK, KBV, AWMF. In: AWMF online (as of 2011)
- S3 guideline National care guideline for type 2 diabetes: prevention and treatment strategies for foot complications of the BÄK, KBV, AWMF. In: AWMF online (as of 2010)
- S3 guidelines on diabetes and pregnancy of the German Diabetes Society (DDG). In: AWMF online (as of 2008)
- S2k guidelines for the care of newborns from diabetic mothers of the German Diabetes Society (DDG), German Society for Gynecology and Obstetrics (DGGG), German Society for Child and Adolescent Psychiatry, Psychosomatics and Psychotherapy (DGKJP), Society for Neonatology and Pediatric Intensive Care Medicine (GNPI) . In: AWMF online (as of 2010)
- S2 guideline in inpatient rehabilitation for diabetes mellitus of the German Society for Child and Adolescent Medicine (DGKJ). In: AWMF online (as of 2007)
Web links
- Type 1 diabetes - information at Gesundheitsinformation.de (online offer from the Institute for Quality and Efficiency in Healthcare )
- Type 2 diabetes - information at Gesundheitsinformation.de (online offer of the Institute for Quality and Efficiency in Healthcare )
- Homepage of the German Center for Diabetes Research e. V.
- German diabetes risk test by the German Institute for Nutritional Research Potsdam-Rehbrücke
- Diabetes information portal
Individual evidence
- ↑ Hermann Orth: The ancient diabetes synonyms and their word history. In: Janus. Volume 51, 1964, pp. 193-201.
- ↑ Horst Kremling : Historical considerations on preventive medicine. In: Würzburg medical history reports. Volume 24, 2005, pp. 222-260, here p. 240 f.
- ^ Mark E. Daly: Acute effects on insulin sensitivity and diurnal metabolic profiles of a high-sucrose compared with a high starch diet . In: Am J Clin Nutr 1998 . No. 67 . American Society for Clinical Nutrition, 1998, pp. 1186–1196 (English, ajcn.org [PDF]).
- ^ Report of the expert committee on the diagnosis and classification of diabetes mellitus. In: Diabetes care. Volume 26 Suppl 1, January 2003, pp. S5-20, PMID 12502614 .
- ↑ a b Classification according to the German Diabetes Society (PDF) Evidence-based guideline DDG, update 2004.
- ↑ a b c World Health Organization Department of Noncommunicable Disease Surveillance: Definition, Diagnosis and Classification of Diabetes Mellitus and its Complications. (PDF; 1.8 MB) In: WHO / NCD / NCS / 99.2. 1999, accessed February 23, 2011 .
- ↑ a b Practice guidelines of the German Diabetes Association 2011 ( Memento of the original from February 28, 2013 in the Internet Archive ) Info: The archive link was automatically inserted and not yet checked. Please check the original and archive link according to the instructions and then remove this notice. (PDF; 1.1 MB)
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 10th edition. Kitteltaschenbuch, Sinsheim 2015, ISBN 978-3-00-050903-2 , p. 8.
- ↑ a b c d e German Diabetes Health Report 2010, diabetesDE 2009.
- ↑ a b c Robert Koch Institute (ed.): DEGS Symposium “Measured and asked - the health of Germans under the microscope”: How high is the number of adults with diabetes in Germany? June 14, 2012, slide 12–13 ( rki.de [PDF]).
- ↑ Veronika Hackenbroch: Caught early . In: Der Spiegel . No. 11 , 2019, pp. 98-100 ( online ).
- ↑ Ralph Ziegler, Andreas Neu: Diabetes in childhood and adolescence . In: Deutsches Aerzteblatt Online . 2018, doi : 10.3238 / arztebl.2018.0146 ( aerzteblatt.de [accessed on March 6, 2018]).
- ^ A b IDF: Diabetes Atlas, 3rd edition. 2006, eatlas.idf.org ( Memento of the original dated August 30, 2009 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice.
- ↑ V. Harjutsalo, R. Sund u. a .: Incidence of type 1 diabetes in Finland. In: JAMA. Volume 310, number 4, July 2013, pp. 427-428, doi: 10.1001 / jama.2013.8399 . PMID 23917294 .
- ↑ M. Knip, O. Simell: Environmental triggers of type 1 diabetes. In: Cold Spring Harbor perspectives in medicine. Volume 2, Number 7, July 2012, p. A007690, doi: 10.1101 / cshperspect.a007690 . PMID 22762021 . PMC 3385937 (free full text). (Review).
- ↑ a b Diabetes epidemic out of control. Press release December 4, 2006 ( Memento of November 20, 2009 in the Internet Archive ) IDF
- ↑ a b G. Danaei, MM Finucane u. a .: National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 27 million participants. In: Lancet. Volume 378, Number 9785, July 2011, pp. 31-40, doi: 10.1016 / S0140-6736 (11) 60679-X . PMID 21705069 . (Review).
- ↑ a b c IDF Diabetes Atlas - Prevalence ( Memento of March 3, 2007 in the Internet Archive )
- ↑ a b Helmut Schatz: Diabetology compact. 4th edition. 2006, ISBN 3-13-137724-0 .
- ^ IDF Diabetes Atlas 4th edition, IDF 2009 diabetesatlas.org
- ^ IDF Diabetes Atlas 6th edition, IDF 2013 diabetesatlas.org
- ↑ IDF Diabetes Atlas 9th edition, IDF 2019 diabetesatlas.org
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 2015, p. 8.
- ^ White Book Diabetes in Germany, Supply of a Widespread Disease .
- ^ A. Icks, W. Rathmann, B. Haastert, A. Mielck, R. Holle, H. Lowel et al.: Quality of care research and extent of complications in a population-based sample of type 2 diabetes patients . The KORA Survey 2000. In: German Medical Weekly. 2006, Vol. 131, H. 3, pp. 73-78.
- ^ German Health Report ( Memento from July 4, 2007 in the Internet Archive ) German Diabetes Union: Health Report 2007
- ↑ According to W. Fink, G. Haidinger: The frequency of health disorders in 10 years of general practice. In: Z. Allg. Med. 83, 200, pp. 102-108. Quoted from What family doctors mainly deal with . MMW update Med. No. 16/2007 (149th year)
- ↑ a b Thilo Schaufler: Economic benefits of medical early diagnosis. Economic evaluation using the example of a screening for type 2 diabetes mellitus . 2007, ISBN 978-3-8300-3308-0 .
- ↑ X. Zhuo, P. Zhang et al. a .: Cost-effectiveness of alternative thresholds of the fasting plasma glucose test to identify the target population for type 2 diabetes prevention in adults aged> = 45 years. In: Diabetes care. Volume 36, Number 12, December 2013, pp. 3992-3998, doi: 10.2337 / dc13-0497 . PMID 24135386 . PMC 3836092 (free full text).
- ↑ a b Definition and Diagnosis of Diabetes Mellitus and Intermediate Hyperglycemia. (PDF; 1.6 MB) In: World Health Organization . www.who.int, 2006, p. 36 , accessed on February 20, 2011 (English).
- ↑ PM Holterhus ao: diagnostics, therapy, progress control of diabetes mellitus in childhood and adolescence . 2010, p. 18 ( deutsche-diabetes-gesellschaft.de [PDF]).
- ↑ "Diabetology and Metabolism" 2016. (PDF; 0.2 MB) (No longer available online.) In: Deutsche Diabetes-Gesellschaft. Archived from the original on December 1, 2017 ; accessed on November 20, 2017 . Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice.
- ^ "Diabetes Care" January 2010. In: American Diabetes Association. Retrieved January 29, 2010 .
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 10th edition. Kitteltaschenbuch, Sinsheim 2015, ISBN 978-3-00-050903-2 , p. 40.
- ↑ diabetes-news.de Diabetes Network Germany
- ↑ Hans Reinauer, Werner A. Scherbaum: Diabetes mellitus: New reference standard for HbA1c . In: Deutsches Ärzteblatt . tape 106 , no. 17 . Deutscher Ärzte-Verlag, April 24, 2009, p. A-805 / B-686 / C-670 ( aerzteblatt.de ).
- ↑ RC Turner, RR Holman, D. Matthews, TD Hockaday, J. Peto: Insulin deficiency and insulin resistance interaction in diabetes: estimation of their relative contribution by feedback analysis from basal plasma insulin and glucose concentrations . In: Metabolism . tape 28 , no. 11 , 1979, pp. 1086-1096 , doi : 10.1016 / 0026-0495 (79) 90146-X , PMID 386029 ( ncbi.nlm.nih.gov ).
- ↑ Gerd Herold: Internal Medicine . aerztekunst.de (PDF; 237 kB)
- ↑ Position paper of the German Diabetes Society on the therapy of diabetes mellitus in hospitals. DDG 2016. ( PDF ).
- ↑ Herbert Renz-Polster , Steffen Krautzig (Ed.): Basic textbook internal medicine. Munich 2008, ISBN 978-3-437-41053-6 , p. 813.
- ↑ Kirsten P. Perrett et al .: Association of Rotavirus Vaccination With the Incidence of Type 1 Diabetes in Children . In: JAMA pediatrics . tape 173 , no. 3 , March 1, 2019, p. 280–282 , doi : 10.1001 / jamapediatrics.2018.4578 , PMID 30667473 , PMC 6439878 (free full text).
- ↑ Mary Rogers, Tanima Basu, Catherine Kim: Lower Incidence Rate of Type 1 diabetes after Receipt of the rotavirus vaccine in the United States, 2001-2017. In: Scientific Reports. Volume 6, No. 7727, June 2019; doi: 10.1038 / s41598-019-44193-4 , PMID 31197227 , PMC 6565744 (free full text).
- ↑ Risk of type 1 diabetes , report dated July 19, 2019 by the professional association of paediatricians; accessed on October 23, 2019.
- ↑ Stone VM et al .: A Coxsackievirus-B vaccine protects against virus induced diabetes in an experimental mouse model of type 1 diabetes. Ed .: Diabetologia. tape 61 , no. 2 , 2018, p. 475-481 .
- ^ P. Concannon, SS Rich, GT Nepom: Genetics of type 1A diabetes. In: The New England Journal of Medicine . Volume 360, Number 16, April 2009, pp. 1646-1654, doi: 10.1056 / NEJMra0808284 . PMID 19369670 . (Review).
- ↑ S. Nejentsev, JM Howson u. a .: Localization of type 1 diabetes susceptibility to the MHC class I genes HLA-B and HLA-A. In: Nature. Volume 450, number 7171, December 2007, pp. 887-892, doi: 10.1038 / nature06406 . PMID 18004301 . PMC 2703779 (free full text).
- ↑ Caesarean section increases the risk of type 1 diabetes: results from the BABYDIAB study DZKF 9 / 10-2012. MAIN TOPIC: GYNECOLOGY
- ↑ U. Kraft: On the trail of diabetes. Origin of type 1 diabetes. Diabetes No. 2, 2016, pp. 42-50.
- ↑ HS Lee, T. Briese et al. a .: Next-generation sequencing for viruses in children with rapid-onset type 1 diabetes. In: Diabetologia. Volume 56, Number 8, August 2013, pp. 1705-1711, doi: 10.1007 / s00125-013-2924-y . PMID 23657799 . PMC 4019381 (free full text).
- ↑ KD Hettiarachchi, PZ Zimmet, MA Myers: The effects of repeated exposure to sub-toxic doses of plecomacrolide antibiotics on the endocrine pancreas. In: Food and chemical toxicology. Volume 44, Number 12, December 2006, pp. 1966–1977, doi: 10.1016 / j.fct.2006.06.023 . PMID 16905235 .
- ^ Arch Dis Child , 93, 2008, 512, quoted in Ärzte Zeitung , March 3, 2010, p. 1.
- ↑ A. Beyerlein, F. Wehweck a. a .: Respiratory infections in early life and the development of islet autoimmunity in children at increased type 1 diabetes risk: evidence from the BABYDIET study. In: JAMA pediatrics. Volume 167, number 9, September 2013, pp. 800-807, doi: 10.1001 / jamapediatrics.2013.158 . PMID 23818010 .
- ↑ H. Kolb: Cow's Milk and Diabetes. In: Monthly Pediatrics . (2001) 149 (13), pp. S62-S65. doi : 10.1007 / s001120170010 .
- ^ Sabine Marienfeld, Sandra Hummel, Anette-Gabriele Ziegler, Michael Hummel: Early childhood nutrition and type 1 diabetes . In: Deutsches Ärzteblatt . tape 104 , no. 9 . Deutscher Ärzte-Verlag, March 2, 2007, p. A-570 / B-501 / C-482 ( aerzteblatt.de ).
- ^ EV Marietta, AM Gomez u. a .: Low incidence of spontaneous type 1 diabetes in non-obese diabetic mice raised on gluten-free diets is associated with changes in the intestinal microbiome. In: PloS one. Volume 8, number 11, 2013, p. E78687, doi: 10.1371 / journal.pone.0078687 . PMID 24236037 . PMC 3827256 (free full text).
- ↑ Jill M. Norris, Randi K. Johnson, Lars C. Stene: Type 1 diabetes — early life origins and changing epidemiology In: Lancet Diabetes & Endocrinology , 2020 Mar; 8 (3), pp. 226-238. PMID 31999944 . PMC 7332108 (free full text). doi : 10.1016 / S2213-8587 (19) 30412-7 .
- ^ Diabetes Information Service Munich: Type 1 Diabetes Risk Factors
- ↑ versorgungsleitlinien.de
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 2015, p. 10.
- ↑ It's all about belly fat , aerzte-zeitung.de, June 26, 2008
- ↑ Belly fat: cause of diabetes and atherosclerosis? , ugb.de, April 2013
- ↑ Abdominal circumference ( Memento of the original from December 11, 2015 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice. , diabetesstiftung.de, accessed: December 13, 2015
- ^ Q. Yang, TE Graham et al. a .: Serum retinol binding protein 4 contributes to insulin resistance in obesity and type 2 diabetes. In: Nature. Volume 436, number 7049, July 2005, pp. 356-362, doi: 10.1038 / nature03711 . PMID 16034410 .
- ^ TE Graham, Q. Yang et al. a .: Retinol-binding protein 4 and insulin resistance in lean, obese, and diabetic subjects. In: The New England Journal of Medicine . Volume 354, Number 24, June 2006, pp. 2552-2563, doi: 10.1056 / NEJMoa054862 . PMID 16775236 .
- ^ I. Muraki, F. Imamura et al. a .: Fruit consumption and risk of type 2 diabetes: results from three prospective longitudinal cohort studies. In: BMJ (Clinical research ed.). Volume 347, 2013, p. F5001, PMID 23990623 . PMC 3978819 (free full text).
- ↑ Study on nutritional approaches in type 2 diabetes. Accessed on January 21, 2018 (English).
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 2015, p. 9 f.
- ↑ KE Lohmueller, T. Sparsø u. a .: Whole-exome sequencing of 2,000 Danish individuals and the role of rare coding variants in type 2 diabetes. In: American Journal of Human Genetics . Volume 93, number 6, December 2013, pp. 1072-1086, doi: 10.1016 / j.ajhg.2013.11.005 . PMID 24290377 . PMC 3852935 (free full text).
- ↑ Stress in the father also affects the offspring , Deutschlandfunk - research aktuell from February 19, 2016
- ↑ Ling Wu, Yan Lu, Yang Jiao, Bin Liu, Shangang Li, Yao Li1, Fengying Xing, Dongbao Chen, Xing Liu, Jiejie Zhao, Xuelian Xiong, Yanyun Gu, Jieli Lu, Xuejin Chen, Xiaoying Li: Paternal Psychological Stress Reprograms Hepatic Gluconeogenesis in Offspring , Cell Metabolism , doi: 10.1016 / j.cmet.2016.01.014 .
- ↑ quoted in Ärzte Zeitung , February 24, 2010, p. 4: J. Parker, O. Hashmi u. a .: Levels of vitamin D and cardiometabolic disorders: systematic review and meta-analysis. In: Maturitas. Volume 65, number 3, March 2010, pp. 225-236, doi: 10.1016 / j.maturitas.2009.12.013 . PMID 20031348 . (Review).
- ^ CJ McMullan, ES Schernhammer, EB Rimm, FB Hu, JP Forman: Melatonin secretion and the incidence of type 2 diabetes. In: JAMA: the journal of the American Medical Association. Volume 309, Number 13, April 2013, pp. 1388-1396, doi: 10.1001 / jama.2013.2710 , PMID 23549584 .
- ↑ AM Stuebe, JW Rich-Edwards and a .: Duration of lactation and incidence of type 2 diabetes. In: JAMA. Volume 294, Number 20, November 2005, pp. 2601-2610, doi: 10.1001 / jama.294.20.2601 . PMID 16304074 .
- ↑ Ursula Biermann: MEDICINE - An enzyme as a possible trigger of diabetes , in Deutschlandfunk " Forschung aktuell " from July 9, 2014.
- ↑ Karin Janke, Claudia Krallmann, Arne Tiemann: Phimosis (foreskin narrowing) . On: urologenportal.de of November 23, 2006, updated August 8, 2016; last accessed on August 13, 2016.
- ↑ J. Tuomilehto, J. Lindström u. a .: Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. In: The New England Journal of Medicine . Volume 344, Number 18, May 2001, pp. 1343-1350, doi: 10.1056 / NEJM200105033441801 . PMID 11333990 .
- ↑ toilet Knowler, E. Barrett-Connor, SE Fowler and others; Diabetes Prevention Program Research Group .: Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. In: N Engl J Med. Band 346 , no. 6 , 2002, pp. 393-403 , PMID 11832527 . (Full text; English)
- ↑ HC Gerstein u. a .: Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomized controlled trial. In: Lancet. Volume 368, Number 9541, September 2006, pp. 1096-1105, doi: 10.1016 / S0140-6736 (06) 69420-8 . PMID 16997664 .
- ↑ DAZ online, Drugs Commission: BfArM orders sales to be discontinued ( memento of the original from September 28, 2010 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice. , September 23, 2010.
- ↑ diabetes.uni-duesseldorf.de ( Memento of the original from September 29, 2007 in the Internet Archive ) Info: The archive link was inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice. ROSSO study by the German Diabetes Center leads to a general recommendation for blood glucose self-monitoring in type 2 diabetes in new global diabetes guidelines
- ↑ Opinion of BdSN to ADIB operation
- ↑ National Care Guideline Therapy of Type 2 Diabetes ( Memento of April 8, 2014 in the Internet Archive ) (PDF); Ed .: German Medical Association , National Association of Statutory Health Insurance Physicians , Association of the Scientific Medical Societies in Germany ; As of 09/2013.
- ↑ Merck and Pfizer Announce That Investigational SGLT-2 Inhibitor Ertugliflozin Met Primary Endpoint in Two Phase 3 Studies , Merck PM, June 10, 2017, accessed June 11, 2017
- ↑ Vlado Perkovic, Meg J. Jardine a. a .: Canagliflozin and Renal Outcomes in Type 2 Diabetes and Nephropathy. In: New England Journal of Medicine. April 14, 2019, doi: 10.1056 / NEJMoa1811744 .
- ↑ Steven P. Marso, Gilbert H. Daniels et al. a .: Liraglutide and Cardiovascular Outcomes in Type 2 Diabetes. In: New England Journal of Medicine. 375, 2016, p. 311, doi: 10.1056 / NEJMoa1603827 .
- ^ V. Novak, W. Milberg et al. a .: Enhancement of vasoreactivity and cognition by intranasal insulin in type 2 diabetes. In: Diabetes care. Volume 37, Number 3, March 2014, pp. 751-759, doi: 10.2337 / dc13-1672 . PMID 24101698 . PMC 3931384 (free full text).
- ↑ Rare forms - "Type 3 diabetes"
- ↑ deutsche-diabetes-gesellschaft.de (PDF; 357 kB) Diabetes and Pregnancy, guidelines of the German Diabetes Society, as of 04/2008.
- ↑ deutsche-diabetes-gesellschaft.de (PDF; 1.1 MB) Guideline gestational diabetes mellitus, evidence-based guideline for diagnostics, therapy and aftercare, DDG and DDDG, as of 08/2011.
- ^ Susan Tosh: Review of human studies investigating the post-prandial blood-glucose lowering ability of oat and barley food products. In: European Journal of Clinical Nutrition. No. 67, 2013, pp. 310-317.
- ↑ European Food Safety Authority (EFSA): Scientific Opinion on the substantiation of health claims related to beta-glucans from oats and barley and maintenance of normal blood LDL-cholesterol concentrations (ID 1236, 1299), increase in satiety leading to a reduction in energy intake (ID 851, 852), reduction of post-prandial glycaemic responses (ID 821, 824), and “digestive function” (ID 850) pursuant to Article 13 (1) of Regulation (EC) No 1924/2006. In: EFSA Journal. No. 9 (6): 2207, 2011.
- ↑ Petia, Kovatcheva-Datchary et al .: Dietary fiber-induced improvement in glucose metabolism is associated with increased abundance of prevotella. In: Cell metabolism. No. 22, 2015, pp. 971-982.
- ↑ Practical recommendations of the German Diabetes Society Ed .: M. Kellerer, S. Matthaei on behalf of the DDG Updated version 2011 ( Memento from March 31, 2015 in the Internet Archive ) (PDF)
- ↑ Expensive and harmful - food for diabetics ( memento of the original from January 3, 2015 in the Internet Archive ) Info: The archive link has been inserted automatically and has not yet been checked. Please check the original and archive link according to the instructions and then remove this notice. In: Frontal21
- ↑ An increased intake of fructose is not recommended for diabetics. (PDF; 52 kB) In: Opinion No. 041/2009. Federal Institute for Risk Assessment , March 6, 2009, accessed on April 13, 2012 .
- ↑ The labeling of food for diabetics must change ( Memento from January 21, 2010 in the Internet Archive ) DDG, 2006.
- ↑ a b Sixteenth ordinance amending the Diet Ordinance ( Memento of November 16, 2011 in the Internet Archive ) Federal Council
- ^ RA Whitmer, AJ Karter, K. Yaffe, CP Quesenberry, JV Selby: Hypoglycemic episodes and risk of dementia in older patients with type 2 diabetes mellitus . In: JAMA . tape 301 , no. 15 , April 2009, p. 1565-1572 , doi : 10.1001 / jama.2009.460 , PMID 19366776 .
- ↑ P. Schweikert-Wehner: Diabetes in hepatic insufficiency: Targeted selection and dosage of antidiabetic drugs . In: Deutsches Ärzteblatt (Ed.): Perspektiven der Diabetologie . No. 115/41 . Doctors Verlag, Berlin 2018.
- ↑ Every third type 1 diabetic also has thyroid problems. Jena University Hospital, April 12, 2010, accessed on May 14, 2011 .
- ↑ DiabetesDE: German Diabetes Health Report 2010. (PDF) on diabetesde.org (PDF; 1.5 MB) Kirchheim Verlag, 2009.
- ^ Marianne Abele-Horn: Antimicrobial Therapy. Decision support for the treatment and prophylaxis of infectious diseases. With the collaboration of Werner Heinz, Hartwig Klinker, Johann Schurz and August Stich, 2nd, revised and expanded edition. Peter Wiehl, Marburg 2009, ISBN 978-3-927219-14-4 , p. 152 f. (Infections in diabetes mellitus) .
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 2015, p. 21.
- ↑ Gender influences the long-term effects of diabetes: Women with diabetes are more likely to suffer heart attacks and strokes. German Diabetes Society, January 11, 2016, accessed on August 31, 2016 .
- ↑ G. Said: Diabetic neuropathy. In: Handbook of clinical neurology. Volume 115, 2013, pp. 579-589, doi: 10.1016 / B978-0-444-52902-2.00033-3 , PMID 23931803 (review).
- ↑ a b Alberto Verrotti, Giovanni Prezioso, Raffaella Scattoni, Francesco Chiarelli: Autonomic neuropathy in diabetes mellitus. In: Frontiers in Endocrinology. 5, 2014, doi: 10.3389 / fendo.2014.00205 .
- ^ S. Javed, IN Petropoulos, U. Alam, RA Malik: Treatment of painful diabetic neuropathy. In: Therapeutic Advances in Chronic Disease. 6, 2014, p. 15, doi: 10.1177 / 2040622314552071 .
- ↑ Richard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 10th edition. Kitteltaschenbuch, Sinsheim 2015, ISBN 978-3-00-050903-2 , p. 171.
- ↑ Mayo Clinic, Jacksonville Florida: mayoclinic.org .
- ↑ Ipswich touch test: This is how diabetics recognize sensory disorders in the foot , test.de , February 25, 2015, accessed on February 27, 2015.
- ↑ ichard Daikeler, idols Use, Sylke Waibel: diabetes. Evidence-based diagnosis and therapy. 2015, p. 174 f.
- ^ Marianne Abele-Horn: Antimicrobial Therapy. Decision support for the treatment and prophylaxis of infectious diseases. With the collaboration of Werner Heinz, Hartwig Klinker, Johann Schurz and August Stich, 2nd, revised and expanded edition. Peter Wiehl, Marburg 2009, ISBN 978-3-927219-14-4 , pp. 152-155.
- ↑ Diabetics: Every second amputation superfluous. In: Focus Online . September 21, 2008, accessed December 26, 2014 .
- ↑ Leaflet: Stiff shoulder (adhesive capsulitis). (No longer available online.) Institute for Quality and Efficiency in Health Care (IQWiG), September 19, 2008, archived from the original on November 12, 2013 ; Retrieved May 13, 2011 .
- ^ Carl J. Wirth, Ludwig Zichner, Frank Golke, Achim Hedtmann: Handbook Orthopädie, shoulder . Thieme, Stuttgart, 2002, p. 341 ( full text in Google Book Search).
- ↑ Nicholas Shah, Mark Levis: Shoulder adhesive capsulitis: systematic review of randomized trials using multiple corticosteroid injections. In: The British journal of general practice: the journal of the Royal College of General Practitioners . tape 57 , no. 541 , August 2007, PMID 17688763 .
- ↑ Gerard A. Lutty: Effects of Diabetes on the eye. In: Investigative Opthalmology & Visual Science. 54, 2013, S. ORSF81, doi: 10.1167 / iovs.13-12979 .
- ^ P. Schweikert-Wehner: Antidiabetic drugs for renal insufficiency . In: Mediengruppe Oberfranken-Fachverlag GmbH & Co KG (ed.): Heart medicine . No. 1 . Mediengruppe Oberfranken-Fachverlag GmbH & Co KG, Kulmbach 2018, p. 30-31 .
- ^ Rainer F. Mausberg: Diabetes and Parodontitis - an unsympathetic team . (PDF; 322 kB) University of Göttingen
- ^ Diabetes and Teeth , Diabetes Information Service Munich
- ↑ T. Stocks, K. Rapp et al. a .: Blood glucose and risk of incident and fatal cancer in the metabolic syndrome and cancer project (me-can): analysis of six prospective cohorts. In: PLoS medicine. Volume 6, number 12, December 2009, p. E1000201, doi: 10.1371 / journal.pmed.1000201 . PMID 20027213 . PMC 2791167 (free full text).
- ↑ V. Kakarlapudi, R. Sawyer, H. Staecker: The effect of diabetes on sensorineural hearing loss. In: Otology & neurotology. Volume 24, Number 3, May 2003, pp. 382-386, PMID 12806288 . (Review).
- ↑ V. Misra, CG Agarwal, N. Bhatia, GK Shukla: Sensorineural deafness in patients of type 2 diabetes mellitus in uttar pradesh: a pilot study. In: Indian J Otolaryngol Head Neck Surg. 2013 Dec, 65 (Suppl 3), pp. 532-536, doi: 10.1007 / s12070-011-0442-0 . Epub 2012 Jan 6
- ↑ SF Weng, YS Chen et al. a .: Clinical features of sudden sensorineural hearing loss in diabetic patients. In: The Laryngoscope. Volume 115, Number 9, September 2005, pp. 1676-1680, doi: 10.1097 / 01.mlg.0000184790.91675.e3 . PMID 16148716 .
- ↑ Tayyab S. Khan, Lisa-Ann Fraser: Type 1 Diabetes and Osteoporosis: From Molecular Pathways to Bone Phenotype. In: Journal of Osteoporosis. 2015, 2015, p. 1, doi: 10.1155 / 2015/174186 .
- ↑ DM Nathan, PA Cleary, JY Backlund et al .: Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes . In: N. Engl. J. Med. Band 353 , no. 25 , December 2005, p. 2643-2653 , doi : 10.1056 / NEJMoa052187 , PMID 16371630 , PMC 2637991 (free full text).
- ^ RR Holman, SK Paul, MA Bethel, DR Matthews, HA Neil: 10-year follow-up of intensive glucose control in type 2 diabetes . In: N. Engl. J. Med. Band 359 , no. October 15 , 2008, p. 1577-1589 , doi : 10.1056 / NEJMoa0806470 , PMID 18784090 .
- ↑ Hellmut Mehnert: UKPDS and DCCT - is a good diabetes control worthwhile? In: diabetes-deutschland.de
- ^ HC Gerstein, ME Miller, RP Byington et al.: Effects of intensive glucose lowering in type 2 diabetes . In: N. Engl. J. Med. Band 358 , no. June 24 , 2008, p. 2545-2559 , doi : 10.1056 / NEJMoa0802743 , PMID 18539917 .
- ↑ Hellmut Mehnert, Thomas Haak: Type 2 Diabetes Mellitus - New Findings on a Widespread Disease. 1st edition. Diabetes Academy, Bad-Mergentheim 2003, p. 40, 1st paragraph.
- ↑ Hellmut Mehnert: Diabetology in clinic and practice. Thieme, Stuttgart a. a. 2003, ISBN 3-13-512805-9 . limited preview in Google Book search


