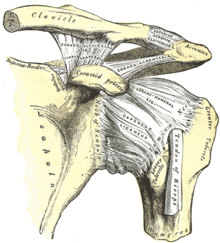
Shoulder joint

The shoulder joint ( lat. Articulatio humeri , also Articulatio glenohumeralis , glenohumeral joint , in veterinary anatomy and shoulder joint ) is the head of the humerus ( humeral head ) and the shoulder blade joint socket ( glenoid cavity , also briefly glenoid) of the scapula ( scapula ) is formed. Since this joint is mainly secured by muscles and movements are hardly restricted by bony structures, it is the most flexible ball joint in the human body. As a result, however, dislocations ( dislocations ) of the shoulder are relatively common, as well as muscle and tendon tears in the area of the rotator cuff .
The article mainly covers the shoulder joint in humans.
Bony structures and articular surfaces

The spherical head of the humerus ( humerus ) fits (separated by synovial fluid ) into the elongated oval joint surface of the shoulder blade ( glenoid cavity ).
The glenoid is flat and shaped like a plate. It is narrow at the top ( cranial ) and broader at the bottom ( caudal ). In three quarters of people it is tilted backwards ( retroverted ) by a mean 7.4 ° against the scapular levels . The diameter is 25 mm in the sagittal plane and 35 mm in the frontal plane. This joint surface is small compared to the humerus head (mean diameter 45-48 mm) and therefore does not completely surround it, as is the case, for example, in the hip joint , but only to a small extent. An enlargement of the contact area between the two joint partners creates a three to four millimeter wide fibrous cartilaginous lip ( labrum glenoidale ) attached to the joint surface, which increases the contact area with the humeral head and at the same time is the origin of the long biceps tendon and the glenohumeral ligaments.
The humerus head forms an angle of 130–150 ° with the humerus shaft and is rotated backwards (retroverted) by 20–30 ° against a line through the epicondyles at the elbow.
Joint capsule
The joint capsule of the shoulder joint is relatively large and flaccid. Towards the tail ( caudal ) there is an approximately one centimeter long reserve zone ( recessus axillaryis ), which offers a large range of movement.
The joint capsule sends a spur to the tendon of origin of the biceps and thus forms a so-called capsule tendon sheath .
Bursa
Several bursae ( bursae ) play an important role in the function of the shoulder joint, including:
- The bursa subtendinea musculi subscapularis lies under the tendon of the musculus subscapularis and reduces the friction that occurs between the tendon and shoulder blade. It communicates with the joint cavity through an oval opening ( foramen ovale , Weitbrecht ).
- The subcoracoid bursa is a reserve space of the joint located below the raven-bill-like extension of the roof of the shoulder ( coracoid process ). It also communicates with the joint cavity.
- The subacromial bursa and subdeltoid bursa are also known as the subacromial secondary joint. These two bursa ensure that the large humerus ( greater humerus humerus ) can be moved below the shoulder level ( acromion ) during the abduction of the arm .
Tapes
The shoulder joint is seen in relation to its load a very weak band trained apparatus which only four bands composed of: ligament coracohumeral , coracoglenoidale ligament , ligamentum coracoacromial and the ligaments glenohumeral . A guide by bands is therefore not given. The ligamentum transversum humeri stabilizes the biceps tendon in the sulcus intertubercularis of the humerus.
Musculature
The shoulder joint is guided and secured by cuff-like surrounding muscles, the so-called rotator cuff. It makes a much greater contribution to stability than the ligaments and thus takes over the main securing of the joint. In addition, the tendons of the long head of the biceps brachii muscle , the deltoideus muscle , the pectoralis major muscle and other muscles help stabilize and guide the shoulder.
The interaction of these muscles in connection with the freedom of movement of the shoulder joint means that the highest measured speed of the human body is achieved during the throw. The development of the biomechanical properties for this is dated to the time of Homo erectus about two million years ago.
Degrees of freedom
Due to the design as a ball joint, the arm can be moved in all three planes and axes. The two other partial joints of the shoulder girdle ( articulatio acromioclavicularis and articulatio sternoclavicularis ) as well as the sliding of the shoulder blade on the back of the thorax make a significant contribution to mobility in humans . Depending on the requirements, the mobility of these joints modifies the positions of the collarbone ( clavicle ) and shoulder blade.
In practice it can be assumed that hardly any movement of the arm is due to movement of the shoulder joint alone. The interaction of the joint group is therefore to be taken into account when evaluating movement restrictions. The standard values follow the information on the data sheets of the German Statutory Accident Insurance , which are used for medical assessments :
- Sagittal
- Anteversion up to 90 ° in the shoulder joint, an elevation beyond that up to 150–170 ° is only possible with the help of the shoulder girdle
- Retroversion up to 40 °
- Frontal
- Vertical axis
- Inward rotation ( internal rotation ) up to 95 ° with the arm resting against the body and up to 70 ° with the upper arm spread (abducted) by 90 °
- Outward rotation ( external rotation ) up to 40–60 ° with the upper arm resting against the body and up to 70 ° with the upper arm spread apart (abducted) by 90 °
Special features in animals
In the case of mammals , which perform more walking movements, the shoulder joint is likewise a ball joint, by the arrangement of the muscles but it is so far restricted in its movement, that only diffraction ( flexion ) and stretching ( extension ) are possible, so the joint only is moved in a directional axis (so-called change joint ).
Diseases
A relatively common injury to the joint is dislocation ( shoulder dislocation ), in which the head of the humerus jumps out of the socket of the shoulder blade. The repositioning (reduction) can usually be done non-operatively. Sometimes an initial traumatic dislocation can develop into a habitual dislocation if the joint has become unstable. A dislocation of the acromioclavicular joint is known as a shoulder dislocation .
For the treatment of osteoarthritis or after accidents there have also been artificial joint replacements ( endoprostheses ) in the shoulder joint since 1995 . The picture shows the X-ray of an inverse prosthesis of the shoulder joint - "inverse" because the joint head was attached to the shoulder blade and the socket was attached to the humerus.
See also: frozen shoulder , Bankart lesion , Hill-Sachs lesion , glenoid fracture, and SLAP lesion
literature
- Franz-Viktor Salomon: Bone Connections. In: F.-V. Salomon et al. (Ed.): Anatomy for veterinary medicine. 2nd ext. Edition. Enke-Verlag, Stuttgart 2008, ISBN 978-3-8304-1075-1 , pp. 110-147.
- John Strings, Michael L. Pretterklieber: musculoskeletal system . In: Friedrich Anderhuber, Franz Pera, Johannes Streicher (eds.): Waldeyer - Anatomie des Menschen. Textbook and atlas in one volume . 19th, completely revised and updated edition. Walter de Gruyter, Berlin / Boston 2012, ISBN 978-3-11-022863-2 , Section 4.3.2.4 Articulatio humeri, Articulatio glenohumeralis, shoulder joint , p. 209–212 ( pp. 209 , 211 and 212 in Google Book Search).
Web links
Individual evidence
- ^ Stephan Coenen, Frank Hoffmann, Bernhard Weigel: shoulder. In: Bernhard Weigel, Michael Nerlich (eds.): Praxisbuch Unfallchirurgie. Volume 1, Springer-Verlag, Berlin 2005, ISBN 3-540-41115-1 , p. 236 ff.
- ↑ Johannes Streicher, Michael L. Pretterklieber: musculoskeletal system . In: Friedrich Anderhuber, Franz Pera, Johannes Streicher (eds.): Waldeyer - Anatomie des Menschen. Textbook and atlas in one volume . 19th, completely revised and updated edition. Walter de Gruyter , Berlin / Boston 2012, ISBN 978-3-11-022863-2 , p. 211 ( limited preview in Google Book search).
- ↑ Jan Dönges: How humans came to their unique throwing talent. on: Spektrum.de from June 27, 2013, accessed on August 2, 2013.
- ↑ Stanley Hoppenfeld: Clinical examination of the spine and extremities . 3. Edition. People and Health, Berlin 1985, p. 2 .
- ↑ Measurement sheet for the upper extremities (PDF; 49 kB) from the German Social Accident Insurance