Loop diuretics
Loop diuretics are a group of water pills ( diuretics ), which on the loop of Henle of the harnbildenden system, a portion of renal function. They are very effective over a short period of time and, since they show an almost linear concentration-effect relationship over a wide dose range, they are also referred to as "high ceiling" diuretics. With the appropriate fluid intake, it is possible to achieve a urine flow of 35 to 45 liters per day. Chemically, loop diuretics are different substances that all have the same mechanism of action. By inhibiting a transport protein in the kidney tubules , there is a reduced re- uptake of ions from the primary urine and, as a result of the change in the osmotic pressure, an increased excretion of water.
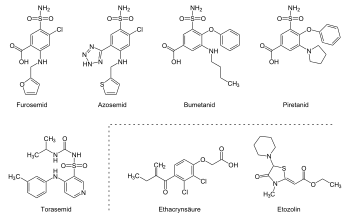
Representative and chemical structure
Loop diuretics can be chemically differentiated into sulfonamide derivatives and non-sulfonamide derivatives. The sulfonamide derivatives include the active ingredients furosemide , bumetanide and piretanide , all of which also have a carboxy group on the central benzene ring. Azosemide is also a sulfonamide, but without a carboxy group. Torasemid is a pyridinesulfonylurea derivative.
Etacrynic acid, on the other hand, is a halogenated phenoxyacetic acid with appended ketone and methylene groups . The methylene group bonds with cysteine to form the active form of the drug. Another representative is Etozolin .
Mercury diuretics are organic mercury compounds that are no longer used today due to their high toxicity .
pharmacology
Mechanism of action
In the kidney , metabolic end products are filtered out of the blood and excreted with the urine . At first, around 180 to 200 liters of primary urine are produced daily, which is then concentrated in the subsequent system of tubules , Henle loop (after Friedrich Gustav Jakob Henle ) and collecting tubes through the absorption of water until only around 1 to 1.5 liters of terminal urine are left or secondary urine left over. Important substances such as glucose , amino acids and electrolytes are also absorbed.
Loop diuretics work in the thick ascending part of Henle's loop, an important absorption site, in which up to 25% of the excreted sodium is taken up (reabsorbed) into the blood. This reuptake of the sodium ions takes place with the help of a transport protein , the Na + K + 2Cl - - symporter (cotransporter). It is located on the luminal side of the tubular cells (facing the urine) and, in addition to sodium, also transports chloride and potassium ions into the tubular cells. The driving force is the active transport of sodium out of the cell into the blood by the sodium-potassium pump , as this creates a concentration gradient between the tubular cell and the urine within the tubule. In addition, this transport causes the inside of the cell to be electrically negatively charged. This negative charge drives the absorption through the passive transport of magnesium (Mg 2+ ) and calcium ions (Ca 2+ ) into the spaces between the tubular cells. Since the wall of the tubule is only slightly permeable to water here, the urine is relatively diluted.
Loop diuretics now work by reversibly (reversibly) inhibiting the Na + K + 2Cl - symporter. Sodium can no longer be reabsorbed, which is why the urine remains concentrated. This leads to increased water excretion through osmosis . Since no negative membrane tension can be built up, calcium and magnesium ions remain in the urine and are lost to the body.
Loop diuretics also inhibit the Na + K + 2Cl - symporters of the macula densa, which leads to an increase in the glomerular filtration rate (GFR). (see: Glomerular Feedback )
After stopping the drug, it should be noted that the body tries to compensate for the loss of water and sodium ions by activating the natural counter-regulation mechanisms of the sympathetic adrenal and renin-angiotensin-aldosterone systems. As a result, the glomerular filtration rate and ultimately the urine volume are reduced . This process is known as post-diuretic sodium retention .
Indications
The indications for loop diuretics are similar to those of other diuretics. Mainly used in the treatment of acute pulmonary edema and other localized edema caused by cardiac , renal and hepatic insufficiency . Due to the high leaching of calcium , they are also used in the treatment of hypercalcaemia .
Further indications are acute kidney failure in order to be able to control the water balance for a certain period of time, hyperkalaemia and earlier for forced diuresis in case of poisoning e.g. B. with anions (especially bromide , fluoride and iodide ) or rhabdomyolysis . However, it is important to supply sufficient quantities of water, sodium and chloride in the form of electrolyte solutions at the same time .
Loop diuretics should be used cautiously because of their high effectiveness. The balance of the water balance and the adequate substitution of electrolytes are indicated above all in patients with disorders of the electrolyte or acid-base balance (e.g. cirrhosis of the liver ), since the ability to compensate is particularly poor.
Contraindications
The contraindications are the same as most other diuretics. These include sodium and potassium deficiency and hypercalcuria (increased excretion of calcium in the urine), as these are exacerbated, and hypovolemia , i.e. the lack of circulating water volume. Since too much calcium in the urine promotes the formation of kidney stones , loop diuretics should not be used for known kidney stones. Its use is also contraindicated in anuria , i.e. when there is no more urine flow.
However, if the use of loop diuretics is absolutely necessary despite existing contraindications, an exact balance, in particular of the electrolyte balance, is carried out. Representatives of the sulfonamide derivatives must not be used in the case of known allergies to other sulfonamides.
Pharmacokinetics
All loop diuretics can be administered either orally (in tablet form) or parenterally (as an injection or infusion ). Enteral uptake is almost as complete as parenteral (good oral bioavailability ). Loop diuretics work very quickly: depending on the dosage form, within five minutes (intravenous) to half an hour (orally). They reach their maximum effect after about two hours and last between six and eight hours. The half-life depends on the kidney function. Two thirds are excreted in the kidneys through both glomerular filtration and tubular secretion , the remaining third is released in the liver into the bile and ultimately excreted in the stool . There is little metabolism in the liver. Metabolic end products of furosemide and etacrynic acid have been identified. However, it is unknown whether they have any diuretic effects. Torasemide, on the other hand, has two active metabolic end products known as M1 and M3.
Since they work on the luminal side of the tubule, the loop diuretics must be in the primary urine to be effective. However, their strong binding to plasma proteins inhibits glomerular filtration. However, as weak organic acids, they are secreted in the proximal tubular cells. However, this can be reduced by other organic acids, such as nonsteroidal anti-inflammatory drugs (NSAID) or probenecid , or in some kidney diseases, which ultimately affects its effectiveness.
Side effects
Due to the strong effect of loop diuretics, regular control of the electrolyte concentration in the serum is necessary in order to prevent hypovolemia as a result of excessive dehydration with the resulting dizziness, headache, tendency to collapse and orthostatic hypotension , especially with long-term use . In severe cases, dehydration and desiccosis can occur.
The increased excretion of potassium ions (K + ) and protons (H + ) can lead to hypocalemic metabolic alkalosis , a condition that can be corrected by administering potassium and treating hypovolemia. Sodium deficiency is less common than with thiazide diuretics , but if patients ingest too much water as a result of hypovolaemia, it can lead to decreased levels of sodium in the blood. As a result of hypovolemia, uric acid is reabsorbed to a greater extent in the proximal tubule, which can lead to increased uric acid levels in the blood ( hyperuricemia ) and thus to gout attacks . Furthermore, long-term use often leads to reduced magnesium and calcium in the blood ( hypomagnesaemia or hypocalcaemia ).
With all loop diuretics, hearing damage in the high frequencies up to deafness can occur through inhibition of the Na + K + 2Cl - symporter, since no potassium concentration gradient (gradient) can be built up ( ototoxicity ). This effect occurs depending on the dose and generally only occurs during treatment; the damage can only be permanent when using etacrynic acid.
Sulphonamide derivatives can cause allergic reactions in patients with hypersensitivity to sulphonamides, characterized by skin rash, eosinophilia and, in rare cases, interstitial nephritis . After the substances are discontinued, these effects disappear again. In the case of etacrynic acid, this hypersensitivity does not occur due to the different chemical structure.
Interactions
The potassium and magnesium deficiency caused by loop diuretics intensifies the effect of cardiac glycosides . Since glucocorticoids and laxatives also increase potassium excretion, when used with loop diuretics, the development of potassium deficiency is favored. The effect of salicylates , theophylline , curare-like muscle relaxants and other antihypertensive drugs is increased, as is the toxic effect of lithium on the heart and nervous system , as the excretion is reduced and thus the lithium level in the blood is ultimately increased.
The blood sugar-lowering effect of anti- diabetic drugs is reduced. The blood pressure-increasing effect of adrenaline and noradrenaline is weakened because the reduced blood volume counteracts their effect. Other drugs that damage hearing ( ototoxic ), such as aminoglycosides and cisplatin , can increase the harmful effects on the hearing.
Since loop diuretics stimulate the kidneys to synthesize prostaglandins and this contributes to the diuretic effect, but this synthesis is hindered by nonsteroidal anti-inflammatory drugs , these weaken the diuretic and antihypertensive effects of the loop diuretics. This effect is only slight in otherwise healthy patients, but it is more pronounced in patients with kidney failure and those with liver cirrhosis .
history
The first loop diuretics used can be considered mercury compounds. Its diuretic effect was discovered by chance in 1919 as a side effect of the drug Novasurol , which was then used against syphilis . However, their frequent use has resulted in numerous cases of mercury poisoning. Even so, organic mercury compounds were the standard in the treatment of edema for the next forty years . However, their lack of oral availability, toxicity and the rapid development of tolerance severely restricted their usability. A less toxic alternative was Mersalyl developed by Hoechst in 1924 . Since it was much more effective than the chlorothiazide , which had been available since 1957 , it was still used despite its higher toxicity.
As the understanding of urine formation increased, the search for more effective and non-toxic drugs began. The researchers at MSD synthesized etacrynic acid from chlorothiazide. In 1959, Hoechst synthesized furosemide for the first time , based on the structure of sulfonamyl .
literature
- Bertram G. Katzung (Ed.): Basic & Clinical Pharmacology. 9th edition. Lange Medical Books / McGraw-Hill, New York, NY a. a. 2004, ISBN 0-07-141092-9 , Chapter 15: Diuretic agents .
- Donald Seldin, Gerhard Giebisch (Ed.): Diuretic Agents. Clinical Physiology and Pharmacology. Academic Press, San Diego CA et al. 1997, ISBN 0-12-635690-4 , pp. 3 ff .: Chapter 3: A history of diuretics .
- Charles R. Craig, Robert E. Stitzel (Eds.): Modern Pharmacology with Clinical Applications. 6th edition. Lippincott Williams & Wilkins, Philadelphia PA et al. 2004, ISBN 0-7817-3762-1 , pp. 249 ff .: Chapter 21: Diuretic Drugs .
Web links
Individual evidence
- ↑ Walther Schönfeld : About the one-time combined intravenous mercury salvarsan treatment of syphilis with special consideration of Novasurol silver salvarsan mixtures. In: Munich medical weekly. Volume 68, 1921, pp. 197-199.
- ^ Julius H. Comroe : Exploring the Heart. Discoveries in Heart Disease and High Blood Pressure. WW Norton & Co, New York NY 1983, ISBN 0-393-01708-7 .