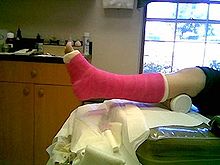
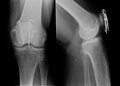
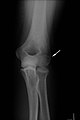
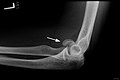
Fracture treatment
The treatment of a bone fracture (a fracture ) comprises the method for supporting the natural bone healing . It is part of human medicine and veterinary medicine .
Diagnosis
Clinical diagnostics
The symptoms found on physical exam are detailed in the article broken bones .
X-ray diagnostics

As a rule, X-rays are made of the suspected fracture skeleton section in 2 mutually perpendicular planes. If the clinical suspicion of a fracture persists despite inconspicuous X-ray images, special projections (oblique images, target images, slice images, special images such as the base of the skull, sinus images) or image converter images must often be made. If these do not lead to success, the following methods are used to search further:
Computed Tomography
The computed tomography allows not only the detection does not yet visible fractures, but also the three-dimensional representation of complex fractures (z. B. tibial, humeral head, spine, heel bone), which are then called upon to select the required treatment process. A special feature is the use of modern spiral CTs in the diagnosis of multiple trauma, a complete "trauma scan" can be performed and initially the individual representation of minor fractures can be dispensed with.
Magnetic resonance imaging
The magnetic resonance imaging (MRI) is also a suitable method for the preparation of fractures and can be used in contrast to the radiological procedures also in pregnant women. In addition, the MRI reliably depicts injuries to the fracture area such as tendons, ligaments and joint capsules.
Sonography
In some parts of the body (examples: wrist, elbow, upper arm, sternum) fractures can also be documented or excluded using fracture ultrasound. Can also be carried out on pregnant women.
Skeletal scintigraphy
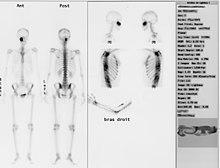
A recent fracture can be confirmed or excluded with the help of skeletal scintigraphy in bones that are difficult to assess radiologically, such as the vertebral bodies or the scaphoid . In the case of a fresh fracture, there are hot spots over the affected region.
Fracture healing
Secondary fracture healing takes place in five phases, some of which overlap in time:
| Fracture phase: | This short phase encompasses the period from the beginning of the force applied to the bone to the point at which forces no longer act on the bone and the surrounding tissue. During this time, the cortex , bone marrow, periosteum and, to varying degrees, surrounding tissue are severed. A bruise occurs in the fracture gap. |
| Inflammatory phase: | After the fracture occurs, an excessive sprouting of the finest blood vessels ( capillaries ) begins , accompanied by the rapid formation of various inflammatory cells (white blood cells, mast cells, scavenger cells ( macrophages )). Among other things, this leads to a rapid increase in blood supply, which can be increased by 6 times the normal after about 2 weeks. The inflammatory phase itself usually subsides after 2-3 days. |
| Granulation phase: | After the inflammatory phase has subsided, the bruise, in which a network of fibrin and collagen has already formed, is replaced by granulation tissue with fibroblasts , additional collagen and numerous capillaries. This so-called "soft callus " brings about the first bridging of the fracture ends. Osteoclasts begin to break down dead bone that is not supplied with blood, while osteoblasts begin to form new bone in the periosteum. This is called the "primary callus response". At the end of this phase, after 3–4 weeks, the fracture ends are softly connected to one another partly by connective tissue and partly by bone. In the X-ray you can now see a blurring of the fracture gap and still faint shadows in and around the fracture gap. |
| Callus hardening phase: | The callus is then “hardened” by mineralization. This essentially happens through the storage of calcium , which is released by chondrocytes . This initially creates a “braided bone” that spreads like a network along the newly formed capillaries. |
| "Modeling" and "Remodeling" phase: | The callus is gradually replaced by lamellar bone. ("Modeling"). With the at least partial restoration of the normal bone structure through slow dismantling, building up and remodeling (“remodeling”), fracture healing is complete. |
Under "primary fracture healing" is meant the fracture healing without callus radiographically visible by exaktester reduction and retention by means of suitable stable osteosynthesis . Histologically, it is not clear whether this is actually an independent, different healing process or whether the remodeling processes only take place on a much smaller scale.
“Primary fracture healing” had a high, almost mythical value in the early years of the AO , until it was established that micro-movements in the fracture gap accelerated rather than hindered fracture healing. On the occasion of the AO basic course in 1984, Weller first spoke of “optimal minimal instability” instead of “absolute stability”.
Treatment principles
From the process of fracture healing described above and the clear fact that the function of the injured system is restored the better the more precisely it corresponds to the intact anatomy in terms of length, rotation and axis bend, the three basic principles of fracture treatment result almost automatically:
Reduction
The fracture must first be brought into a position that is as precise as possible for the anatomy using suitable measures (so-called reduction ). As a rule, this should be done as early as possible, since in the case of grossly misaligned fractures the accompanying damage can quickly worsen (hematoma, tension blisters, circulatory disorders, etc.). The suitable reduction method depends very much on the type of fracture: Sometimes a simple pull in the longitudinal axis is sufficient, even in exceptional cases without anesthesia , often the closed reduction must be carried out under anesthesia under X-ray control, and in many cases the reduction is only successful surgically as an "open" reduction. If, depending on the current situation, immediate surgical treatment of the fracture is necessary, roughly aligned positioning on an appropriate rail or vacuum mattress is sufficient until then . The final reduction should be as exact as possible in all three planes (length, axis bend and lateral shift). Exceptions are described in the corresponding subsections. Completely unshifted fractures naturally do not require repositioning.
Retention
Appropriate measures must be taken to prevent the reduced fracture from subsequently deviating from the desired anatomical position ("secondary correction loss"). This retention can mean completely different efforts depending on the type of fracture. For example, if the head of the humerus is slightly displaced or “compressed”, it is sufficient to wrap the arm on the body ( Desault or Gilchrist bandage ), broken toes are simply “tied” to the neighbor with a strip of plaster. Often, rigid casts ( plaster of paris or plastic cast ) can be used, but in many cases retention must be achieved through surgical treatment using a wide variety of methods. The details are discussed in the following chapters.
rehabilitation
The rehabilitation of a fracture injured person does not begin after the fracture has healed, but immediately after a suitable retention has been achieved. The early mobilization of the injured person is an essential part of rehabilitation in order to avoid consequential damage, especially to the neighboring joints. If bed rest is necessary due to the injury or other factors (internal illnesses, accompanying injuries such as craniocerebral trauma, etc.), the mobility of the extremities should be maintained through intensive physiotherapy exercises in bed. In this way, an inactivity atrophy of the muscles can also be partially averted. Mobile injured persons are encouraged to use all joints that have not been immobilized as normally as possible. The immobilized extremity is treated with isometric muscle training to prevent atrophy and to quickly return to normal strength levels after the immobilization has ended. In the case of fractures of the lower extremities, it is necessary to learn to walk with crutches as quickly as possible ; for weaker patients, strength training (based on the principle of medical training therapy (MTT) ) is also required. After serious injuries, follow-up treatment ( BGSW in the case of work- related accidents ) is initiated in a suitable rehabilitation clinic.
Treatment concepts
The choice of a suitable treatment concept and its professional implementation is the real challenge for the trauma surgeon when treating fractures. It is by no means based solely on the X-ray or the AO classification of the fracture, but is significantly influenced by a number of other factors. The most important in brief:
- Compliance : The patient should be physically, psychologically and intellectually able to support the selected treatment concept. Reduced compliance can mean that necessary rules of conduct (e.g. discharge) are not observed. These problems occur regularly in small children, elderly, psychotic or mentally disabled patients. Also, alcoholism or drug addiction may significantly affect compliance.
- Concomitant illnesses : Does the general health of the injured person even allow the ideal treatment concept? Severe osteoporosis can lead to the failure of good osteosynthetic care. Derailed diabetes mellitus conjures up wound healing disorders. Treatment with anticoagulants and platelet aggregation inhibitors often requires postponing or even omitting surgical treatment. Severe consuming underlying diseases (e.g. advanced tumor diseases) and their therapy ( radiation , cytostatics ) can greatly delay the healing of the bone fracture.
- Multiple Injury: If there is more than one injury, the interaction of these injuries should be considered. The relief of a leg on crutches z. B. may not be possible if the upper extremity is severely injured at the same time. In polytrauma patients, the definitive treatment of fractures of the extremities has to be avoided in favor of the treatment of further life-threatening injuries.In these cases, fractures are primarily secured by quickly applied external fixation and, after the stabilization phase, finally treated according to the situation.
No treatment
Various fractures do not require any or only unspecific / symptomatic ( analgesics / anti-inflammatory drugs , mobilization) treatment due to the lack of functional impairment after spontaneous healing . This concerns, for example, unshifted skull fractures, simple rib fractures, isolated sitting or pubic bone fractures without instability, coccyx fractures, avulsion fractures of the spinous or transverse processes and also vertebral body fractures without loss of stability. However, the intensive pain treatment occasionally requires inpatient treatment. This can also be necessary to reliably exclude or prevent indirect consequences of fractures ( head and brain trauma , pneumonia in rib fractures, etc.).
Conservative treatment
Conservative treatment means treating a fracture without surgery in or around the fracture area. Naturally, only closed fractures and open fractures grade I with only minimal skin lesions are available for conservative treatment. Conservative treatment does not mean treatment without anesthesia: This is often already used for very painful repositioning and e.g. B. required for the insertion of an extension wire (see below). The fracture gap anesthesia (frowned upon by many surgeons because of the possible bacterial contamination ), local anesthesia , conduction anesthesia (e.g. Oberst conduction anesthesia ), regional anesthesia ( plexus anesthesia ), spinal anesthesia or general anesthesia come into question .
Functional treatment
“The basic idea of non-surgical functional fracture treatment is based on the belief that function is beneficial for tissue healing, rehabilitation and the prevention of restricted use of joints and limbs; and renouncing anatomically accurate reduction of fractures is a small price to pay for regaining function and for rapid healing without compromising the cosmetic appearance of the limb. (...) Non-operative functional fracture treatment is primarily aimed at the Make the best possible use of biological parameters associated with fracture healing and restoration of function. It approximates the natural reparative processes and the rehabilitation schemes that the body has developed through the normal feedback mechanism ( pain ) that the biological system has developed. The development of these treatment methods significantly shortens the duration of the inability to function during and after the treatment. "
Shaft fractures of the long tubular bones and, less often, joint fractures or joint fractures are essentially suitable for functional fracture treatment. Functional fracture treatment begins with immobilization in the plaster of paris or in the plaster splint with simultaneous correction of the axial and rotational malalignment. The exact correction of a shortening or a lateral misalignment is usually not done. As early as possible, usually after the acute fracture pain and swelling have subsided, the plaster immobilization is ended and an individual fracture splint is put on, which leaves the range of motion of the adjacent joints free or only to a small extent. The released function of the affected extremity promotes new bone formation by creating a physiological environment and promoting blood circulation. The load is controlled by the injured person depending on the pain that occurs. If the fracture splint is correctly applied, there is no need to fear any loss of correction with regard to the axis and rotational position; smaller losses in length are accepted. After radiological consolidation of the fracture, the fracture splint is removed if there are no symptoms. If necessary, a further physiotherapy rehabilitation treatment follows .
Functional fracture treatment can be used for both closed and open fractures. The combination of operative and functional fracture treatment is also possible and often useful.
The purely functional treatment of fractures - despite its undisputed advantages and successes - has only established itself for a small range of indications in Central Europe . Uncomplicated collarbone fractures are usually treated in a backpack bandage (see below), suitable humerus shaft fractures are often treated in a so-called brace . Occasionally this Sarmiento plaster is used in the treatment of lower leg fractures in children and adolescents.
The main reasons for the low prevalence of functional fracture treatment are:
- The personnel and time required for functional fracture treatment hardly differ from that of surgical treatment.
- The required qualification and experience of the practitioner is to be assessed just as highly as with surgical treatment.
- The requirements for patient compliance are just as high as for surgical fracture treatment.
- The cost of materials for the individually adapted fracture splints is significantly higher than that of a conservative plaster treatment; the production of the splints requires specially qualified orthopedic technicians . The costs of such an individual fitting are often not reimbursed or not sufficiently reimbursed by the health insurers with reference to ready-made orthoses .
- The current remuneration system ( DRG ) favors surgical treatment and makes the conservative or functional treatment of inpatients unattractive for hospitals.
- The radiological treatment result often does not look satisfactory for laypeople, but also for experts and doctors providing further treatment : there are often extensive callus masses in the fracture area and lateral displacement of the fragments. Even if a good function could be achieved again, this can lead to accusation of malpractice .
Immobilization in a simple bandage
For some fractures, immobilization with a simple bandage is sufficient. A typical example is a simple fracture of the proximal upper arm that is not or only slightly displaced : immobilization in the Gilchrist or Desault bandage is sufficient for about 14 days, and then functional therapy is quickly adopted. Another example are the fractures of the toes II – V: A so-called plaster rein bandage ties the injured toe to its healthy neighbor. Simple finger fractures can also be treated in this way. A slightly different example is the treatment of a collarbone fracture in a rucksack bandage: Here the bandage's “reminder function” ensures that the injured person pulls his shoulder backwards and thus counteracts a shortening of the fracture.
Immobilization in a cast
The classic cast is the plaster cast , it has been used to immobilize fractures since 1851. Lorenz Böhler systematized the bandage technique and presented it comprehensively in his standard work. “The guidelines for conservative fracture treatment propagated by Böhler are still valid today, with some variations.” The application of a plaster bandage is an original medical activity, but its implementation in reality often delegated to experienced nurses. Large outpatient clinics even employ experienced “plaster nurses” or “plaster nurses”, whose skills often create artistic associations. However, the doctor placing the order is always responsible for the correct application of the plaster cast, informing the patient about rules of conduct and possible complications, as well as monitoring the course of treatment.
The plaster cast is still very important in bone fracture treatment, although more and more fractures are treated surgically. The particularly complicated special casts such as the thoracic abduction cast (in the vernacular earlier " Stuka "), the pelvic and leg cast, the Minerva cast or the Böhler cast corset have largely disappeared. They have either been replaced by modern orthoses or are no longer common because the underlying injury is regularly treated surgically.
Plastic casts are used on a large scale as an alternative to classic white plaster ; since the differences in application are marginal, everything else also relates to these.
Basically, during treatment in a plaster cast, both joints adjacent to the broken bone are immobilized, with the exception of the fractures near the joints on the distal forearm and lower leg.
The following fractures are still mainly or often treated in a plaster cast, especially in children:
- Forearm fractures in the upper arm cast.
- Fractures of the distal radius (most common of all fractures!) In a forearm cast.
- Scaphoid fractures of the hand, especially upper arm scaphoid plaster, including the base of the thumb and the base of fingers II and III (" Rehbein " cast)
- Lower leg fractures in the child in a thigh cast
- Uncomplicated outer ankle fractures, tarsal and metatarsal fractures in the lower leg cast.
The prerequisite for the plaster treatment is always the correct reduction or the primary lack of a fragment displacement ( dislocation ).
In the context of operative fracture treatment, plaster casts, mostly as plaster splints, are used for preoperative temporary immobilization, for postoperative immobilization as a decongestant or long-term postoperatively after treatment without achieving movement stability. (see there ).
The pure plaster treatment is by no means easier or less risky than the surgical treatment. Specific complications are:
- Pressure sores with insufficient padding.
- complete or partial disturbance of the blood circulation due to too tight bandages or subsequent swelling. If the partial circulatory disorder is not recognized, there is a risk of a Volkmann contracture .
- Pressure damage to nerves, e.g. B. Peroneal paralysis by pressing the upper edge of a lower leg cast on the fibula head.
- Muscle atrophy due to long immobilization .
- Deep vein thrombosis and pulmonary embolism
Extension treatment
The principle of extension treatment (from Latin 'extendere': to pull apart) consists in the application of a continuous longitudinal pull on the injured extremity. Depending on the fracture to be treated, a drill wire is inserted across the bone under local anesthesia on the lower extremity and tensioned using a metal bracket. A variable weight is hung on this bracket via a deflected cable, which means that the leg, which is mounted on a rail, is subjected to longitudinal tension.
For the treatment of fractures close to the hip joint ( acetabular fracture , femoral neck fracture , pertrochanteric fracture), the drill wire is driven across the distal thigh roller; this is called a condyle extension.
Fractures of the femoral shaft are treated with tibial head extension, here the drill wire is passed through the tibial head.
For lower leg fractures, the drill wire is driven through the heel bone, i.e. as a calcaneus extension. As an alternative to the drill wire, an extension shoe can also be used here.
The fingers are held on the upper extremity with girl's catchers and the weight is hung on the upper arm with a cuff close to the elbow.
The wire-tensioning technique, first used by Otto Borchgrevink in 1912 and implemented with the procedure developed by Martin Kirschner until 1940, is no longer used as the sole treatment, as it is associated with numerous serious risks ( thrombosis , pulmonary embolism , pneumonia , decubitus ) due to the extreme immobilization . It is only used as a temporary measure if an immediate, definitive surgical treatment is not yet possible.
On the upper extremity, the extension is regularly used to facilitate the reduction (establishment) of a closed fracture of the distal radius or forearm.
The extension treatment of child thigh fractures occupies a special position; For children between 3 and 6 years of age, it was carried out on the "Weber Bock", with the lower leg being positioned at right angles to the thigh on a height-adjustable plate that is set so that the pelvis floats freely and thus forms the extension weight. With smaller children, the "overhead extension" was used, whereby the legs are pulled vertically upwards over plaster reins. Since children tolerate such a treatment with surprisingly few problems, this type of treatment was used until a few years ago and has only recently faded into the background in favor of surgical procedures. Here, the fault-tolerant and safe minimally invasive osteosynthesis with ESIN nails has created a major change and significantly improved the results.
Operative treatment
Not all surgical procedures are osteosynthesis, but all osteosynthesis procedures are surgical interventions.
An exception is the treatment of the femoral neck fracture with complete joint replacement ( total hip joint prosthesis or femoral head prosthesis).
Osteosynthesis is divided into open (with surgical exposure of the fracture) and closed (without exposure of the fracture) procedures.
A distinction is made between five biomechanical principles in surgical fracture treatment:
- Interfragmentary compression (lag screws, special implants such as the dynamic hip screw DHS or the proximal femoral nail PFN, compression over a plate DCP or LC-DCP)
- Splinting: intramedullary using intramedullary nails, bundle nails. Kirschner wires or elastic titanium nails in children, extramedullary over plates
- Bridging: external and internal fixator
- Support: counteracting the forces and loads by supporting plates, e.g. B. in the tibial head fracture
- Zuggurtung: Conversion of a torque into compression, e.g. B. on the elbow or on the kneecap
Processes can and must be combined with one another, but without contradicting one another biomechanically. Splinting can be combined well with interfragmentary compression, but not e.g. B. with bridging.
Procedure choice
The correct selection of the appropriate surgical procedure is at least as important as its execution and depends on a variety of factors.
The ideal goal of osteosynthesis is the early restoration of fractures that are stable in terms of movement and stress. However, this goal can only be achieved for a small fraction of the fractures. The minimum requirement is movement-stable (previously: exercise-stable) care, in which immobilization of the extremity can be dispensed with. The possibilities of achieving this goal depend heavily on the location as well as the type of fracture. The general condition of the patient, his individual compliance as well as age and demands on the treatment result must be taken into account as further criteria . In special cases, a movement-stable osteosynthesis is not possible or not possible with an acceptable risk, so that postoperative immobilization, e.g. B. by means of plaster must be carried out.
The time of the definitive osteosynthetic treatment also depends on several criteria: the condition of the soft tissues near the fracture, general condition, accompanying injuries, availability of the procedure.
Mistakes that are made when choosing the procedure or the appropriate time can have dramatic effects on the healing process and the treatment result and can often no longer be corrected or can only be corrected with great effort.
Closed procedures
Kirschner wire
The closed reduction and fixation of a fracture using a rotating drill wire (known as Kirschner wire since 1931 ) is - introduced in the 1920s - one of the oldest methods of surgical fracture treatment that is still regularly used today. Stainless steel and pure titanium are available as materials.
It is used as a
- percutaneous intramedullary splint, for example on the metacarpal bones
- Percutaneous “spiking”, ie fixation of a fracture by inserting a Kirschner wire, if possible with fixation of the wire in the opposite cortex .
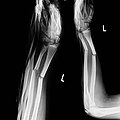
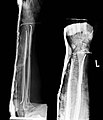
Due to the flexibility of the wires and the non-positive anchoring of the wires in the bone, the result of the operation is usually not stable in terms of movement, so that further immobilization procedures, e.g. B. plaster cast or the external fixator illustrated here must be used.
In the case of the wrist fracture shown here, a movement-stable treatment was required, e.g. B. using an angle-stable plate (see below) due to the high degree of osteoporosis and the significant soft tissue damage, therefore the closed reduction with Kirschner wire fixation and additional immobilization with an external fixator was carried out. A plaster immobilization would not have been possible here either because of the poor soft tissue conditions.
The advantage of the Kirschner wire fixation is the low procedural effort and the low invasiveness. The wires are usually removed immediately after the fracture has healed (i.e. after approx. 4 to 6 weeks).
The disadvantage of the Kirschner wire fixation is the combination of the risks of invasive surgery ( infection , risk of anesthesia ) with the disadvantages of prolonged immobilization ( muscle atrophy , stiffening of the joint, no early functional treatment possible).
Specific complications and risks are "wandering" of the wires, wire breakage and loss of correction.
External fixator
The external fixator (“external tensioner”) is an important instrument for fixing a fracture without manipulating the fracture itself . The basic principle of its application is the percutaneous insertion of several strong screws (Schanz screws or Steinmann nails) away from the fracture, which are connected to one another by means of rods and adjustable assembly elements.
The external fixator is used alone or in combination with other procedures as described above in a variety of situations:
- Open fractures with confirmed or suspected bacterial contamination : Here the primary use of foreign material in the fracture area is generally prohibited, as it increases the risk of a wound or even bone infection with the consequence of osteomyelitis .
- Closed fractures with considerable soft tissue damage: for the same reason, here tissue necrosis with subsequent infection of the fracture area must be expected.
- Closed fractures with a complicated fragmentation zone: The success of an open reconstruction appears questionable due to the shape of the fracture or due to additional problems (e.g. osteoporosis as above).
- Necessity of rapid, less invasive stabilization: This generally comes to the fore in patients with multiple injuries (multiple trauma ) or patients with life-threatening comorbidities (e.g. decompensated heart failure , multiple organ failure ).
The external fixator can be used as a definitive, “one-step” treatment or as a primary measure in the context of “ two-step ” treatment. In the latter case, after the situation has improved, definitive surgical treatment in the sense of a "change of procedure" is followed.
Possible uses of the external fixator outside of fracture treatment:
- Treatment of osteomyelitis
- Treatment of pseudarthrosis
- Length correction primarily (growth disturbance ) or secondarily (after fractures) of shortened long tubular bones ( osteodistraction , often with the Ilisarov ring fixator ).
Specific risks: Loosening of the Schanz screws, infection of the screw holes (pintrack osteitis ), development of pseudarthroses due to fragment distraction .
Intramedullary nail
The intramedullary nail and its further development, the locking nail (→ below), represent the two most important methods of intramedullary splinting. The first intramedullary nail was successfully used by Gerhard Küntscher in 1939 and was used in its original form until the early 1980s. The basic principle of the Küntscher nail was that of the internal splint: By inserting a profiled hollow nail that is clamped in the drilled out medullary canal, a high degree of stability in terms of length and transverse axis is achieved. When loaded, the nail directs the axial force across the fracture gap in such a way that pressure is exerted in the longitudinal direction on the fracture gap and the fracture healing is additionally stimulated. With this procedure it was possible for the first time to treat shaft fractures of the thigh and lower leg with stable movement and, in many cases, even load-bearing.
At the beginning of the 1970s the disadvantages of the Küntschernagels became obvious:
The nail could only be used successfully for transverse, short angled and uncomplicated fractures in the central shaft area. The wider medullary canal in the proximal and distal third of the shaft led to reduced tension on the nail with the occurrence of rotational errors. Complicated debris fractures could not be treated with the nail, since a shortening regularly occurred by sideways evasion of the debris.
In addition, the importance of the medullary canal for the blood supply to the bone and the healing of the fracture became increasingly clear (“endosteal callus formation”), which were disturbed by the generous reaming of the medullary canal.
Locking nail
The problems mentioned led to the development of the locking nail (initially somewhat hesitantly because the Working Group for Osteosynthesis Questions (AO) at that time was almost exclusively concerned with the systematization of plate osteosynthesis). This was first introduced in a form-fitting manner in the traditional manner and fixed by means of several locking bolts inserted proximally and distally transversely. This solved the problem of length loss and rotation error.
The next stage of further development was the unreamed locking nail (UTN = unreamed tibial nail, UFN = and femoral nail). These nails are now made of massive titanium alloys , are significantly thinner than the diameter of the medullary cavity and therefore do not damage the blood circulation in the fracture area. By inserting the locking bolts at a stable angle, even at the outermost nail end, even fractures close to the joint can now be treated with them.
Locking nails are now also available for the upper arm; depending on the fracture, these can be inserted from the proximal (shoulder) or distal (elbow) (UHN = and humeral nail).
Bundle nails
Bundle nails are relatively thin (2–6 mm) steel nails which, after creating a window in the cortex, are inserted in the area of a long tubular bone near the joint and advanced over the fracture. By inserting several nails, these clamp in the narrowest area of the medullary canal and thus stabilize the fracture. By variable selection of the number and strength of the nails, these can be adapted very precisely to the current situation.
Historical examples are the Hackethal nails, which were inserted into the upper arm from shoulder height or from the elbow joint to treat simple humerus shaft fractures, as well as the stronger, pre-bent Ender nails, which were inserted just above the knee and both in the femoral head and in the The greater trochanter was placed to treat thigh fractures near the hip joint ( femoral neck fractures , pertrochanteric femoral fractures ). Disadvantages of these methods were the frequent shifting of the nails, which required corrections, as well as the occurrence of material fatigue fractures with the consequence of pseudarthroses , especially with Hackethhalnageling .
These methods were largely abandoned after the 1980s, as other methods were able to establish themselves that are less problematic and have a broader range of application, e.g. B. the above locking nails or the plate osteosynthesis described below.
A modern variant of bundle nailing, the Henning nails, are increasingly being used again to treat the upper arm fracture near the shoulder joint and the humerus head fracture. The special shape of these nails, which are introduced on the one hand as flat nails with corkscrew-like twisting of the tip (so-called helix nails) and on the other hand with a thickened tip (button nails), ensures a good hold in the fragments of the humerus head, which become jammed in the medullary canal achieved by additional smooth, round filling nails.
Elastic stable intramedullary nailing (ESIN)
This modification of the procedure with bundle nails is used today almost exclusively in children and adolescents with open growth plates. The procedure developed from the application of the endernails. In contrast to intramedullary wire nailing, which has been abandoned in adults, ESIN (synonyms: Prevot nailing, Nancy nailing) has proven its worth in growing patients due to better fracture healing and simple and reliable application.
The implants are flexible, elastic nails made of stainless steel or titanium, which have a flattening and an angle at their tip in order to slide in the medullary cavity of long bones and to become wedged in the medullary cavity by the elastic tension. In the event of suitable fractures of all large tubular bones (thigh, shin, upper arm, radius and ulna), the medullary cavity of the bone is opened with an awl through a small skin incision in the vicinity, but while protecting the growth plate. A first elastic nail is inserted through this opening in a descending or ascending direction. It is pushed with rotating movements over the fracture region, which is correctly closed under X-ray view or, if it cannot be repositioned, is opened through an incision. The upturned tip can also be used as an aid in setting up (repositioning aid). With further advancement, the nail is finally anchored just below the respective other growth plate of the long bone. For sufficient stabilization, with the exception of the paired forearm bones, a second (or rarely a third) nail is inserted through a separate access in the same direction.
When both nails have been driven in, they are shortened with a bolt cutter so that they disappear under the skin, but still stand out of the bone long enough to be removed again. Mostly the treatment is carried out from both sides of an extremity (inside and outside), but it is also possible to use both nails e.g. B. be introduced from the side descending on the upper arm, if on the inside vessels or nerves would be endangered by the implantation. In children and adolescents with suitable fractures, the ESIN achieves good exercise stability and early stress stability. No additional plaster treatment is necessary. The nails can be removed after a few months with an equally small incision.
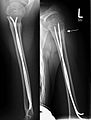
- Case studies
Upper arm fracture near the shoulder joint treated with ESIN in children. Healing image with clearly visible fracture callus (arrow)
Open procedures
Cerclage
The treatment of a fracture by simply looping wire is extremely rarely used as a stand-alone procedure for very long oblique breaks. A soft wire is looped around the bone - usually twice - and tightened by twisting it. In the case of plate osteosynthesis, the cerclage is also used if necessary in order to hold long wedges together. In the case of sternotomies , the split sternum is fixed with cerclagen for healing. The cerclagen remain in the body.
Tension belt
The tension belt osteosynthesis is a process, the physical basis of which comes from reinforced concrete construction. Tensile steel elements in the concrete absorb the tensile stresses and convert them into compressive stresses in the concrete. For this reason, engineers among orthopedic surgeons have referred to the technology for the first time and scientifically substantiated its effect. The team around the biomechanically thinking Friedrich Pauwels from Aachen developed the theoretical basis and carried out the first applications of the process. Pauwels himself presented the concept for the first time in 1958 in Freiburg as part of the so-called Aschoff lecture.
The procedure is surgically used only for fractures that run in joints and whose fragments are under tension from tendons, so that the muscle pull inevitably separates the fragments from each other. Such fractures are always caused by a combination of direct force acting on the bones and the tensile stress of the muscles, even when falling. Typical examples of such fractures are transverse fractures of the hook of the elbow and the kneecap as a result of a fall or impact on the elbow and knee with the corresponding muscle tension to ward off the fall. To a very limited extent, the tears on the inner and outer ankle of the upper ankle joint and on the base of the 5th metatarsal as well as on the greater tuberosity of the humerus could be counted among these avulsion fractures and treated with a wire loop. There is no real tension band effect.
The principle of the procedure is that the tensile stresses acting on the fragments are absorbed by a wire loop that is attached around the tendon attachments or on the bone and rests on the fragments as far as possible from the joints. During the active movement (flexion) of the joint after the operation, the tensile stress acting within the joint (i.e. opposite the wire loop) leads to a compressive stress that pushes the fracture gap together. This holds the fragments in the correct position and the break can heal safely. This simple basic principle (conversion of tensile stress into compressive stress) can be implemented with a minimum of material costs (a few cents for the stainless steel wire) and with a relatively small surgical intervention, which explains the triumph of this process since it was first described in 1958. All simple fractures of the kneecap and the elbow hook are operated almost exclusively with this procedure. And the process has another advantage: The post-treatment is exclusively functional, i.e. That is to say, correctly, no plaster or similar may be used, so it is a classic dynamic procedure. In order to be able to carry out the process even with more complicated fractures with several fragments and in order not to let the fragments gape under the tensile stress even in the stretched position, the use of about two additional straight wires has proven to be useful, which, while setting up the fragments, along the one fragment be drilled into the other fragment via the fracture gap. Where the wires protrude from the bone in the area where the tendons are attached, the tension cord wire loop is placed around these wire ends instead of just around the tendon attachment, thus further increasing stability.
Screw connection
In the case of simple fractures, screwing the bones with two or more bone screws can in principle be sufficient for stabilization. The method is used e.g. B. in longitudinal kneecap fractures, as well as transverse and spiral fractures of the finger bones or metatarsal bones or simple fractures of the outer ankle .
The principle of interfragmentary compression can be used for screwing. For this purpose, a hole larger than the outer diameter of the screw is drilled on the screw head side (so-called sliding hole) so that the screw inserted approximately perpendicular to the fracture compresses the fracture gap and only engages in the thread in the corticalis far away from the head (lag screw). Screws with a considerably larger thread diameter are used in the cancellous bone area near the joint. In order to achieve a lag screw function with these, cancellous bone screws with a short thread end are available. So that the screw head does not break into the softer cancellous bone with these cancellous screws, a so-called washer is usually used.
The screw connection is often combined with other methods, e.g. B. as a lag screw through a plate or in addition to it. A pure lag screw osteosynthesis is occasionally possible with long spiral fractures, if the fragments can be anatomically reduced to one another so that the fracture has its own "intrinsic stability". Such fragments can be supplied in a stable manner with 2 or more lag screws.
- Screw fixation using the example of a fracture of the capitulum humeri
Plate fixation
In the case of plating, a plate is screwed on after open reduction of the fracture as a fixation and thus fulfills the principle of extramedullary splinting, comparable to plaster of paris, only directly on the bone. The plate must rest on the bone, so minimally invasive insertion is hardly possible. At least three screws should be anchored bicortically, i.e. through the entire bone, on both sides of the fracture. At best, conventional plates guarantee a supply that is stable when exercising. The compression of the periosteum also restricts the blood supply, which is improved by locking compression plates (LCP). Newer plates, so-called “dynamic compression plates” (LC-DCP), enable interfragmentary compression through oval screw holes and conical screw heads that pull the plate and the already screwed fragment against the other fragment when tightened. Anatomically preformed plates are still frequently used in the surgical treatment of distal radius fractures and other forearm fractures, in childhood femoral fractures and in combination with other principles, e.g. B. in the treatment of ankle fractures. In many areas, the plates have been replaced by superior techniques such as intramedullary nails and the internal fixator.
Internal fixator
A special form of plate osteosynthesis is offered by a new generation of implants which, in addition to the conventional holes for screws, also offer the possibility of angle-stable screw connections. Self-drilling or self-screwing bolts are used, which can be inserted minimally invasively at right angles to the plate, often using an aiming arm, and which enable force to be transmitted from the bone to the plate thanks to the fixed anchoring. The internal fixator no longer has to be in contact with the bone like a conventional plate and is gentle on the periosteum and thus the blood circulation. A similar principle is used in spondylodesis , the stiffening of the spine, in which angle-stable screws are connected to the longitudinal force carrier and thus take over the load.
Prostheses
- Hemiendoprosthesis (HEP)
- Total endoprosthesis (TEP)
Special forms
- Implant combinations z. B. Cerclage
- Composite osteosynthesis
- Special prostheses
- Vertebral Body Cage
- Herbert / Bold screw on the navicular bone
- Hook plate for lateral clavicle fracture
literature
- Axel Rüter, Otmar Trentz, Michael Wagner (Eds.): Trauma Surgery , 2nd, completely revised and expanded edition. Urban & Fischer, Munich Jena 2004, ISBN 3-437-21850-6 .
- Augusto Sarmiento Rosillo , Loren L. Latta: Non-operative functional fracture treatment . Springer, Berlin Heidelberg New York Tokyo 1984, ISBN 3-540-13189-2 .
- Lutz von Laer, Ralf Kraus, Wolfgang E. Linhart: Fractures and dislocations in growing age . Thieme, Stuttgart 2007. ISBN 978-3136743041 .
- Bernhard Weigel, Michael L. Nerlich: Practice book accident surgery . Springer 2011, ISBN 978-3642107887 .
- Rüdiger Döhler , Anett Gudat, Silke Mein: Treatment of fractures , in: Margret Liehn, Brigitte Lengersdorf, Lutz Steinmüller, Rüdiger Döhler (eds.): OP manual. Basics, instruments, operating procedures , 6th, updated and expanded edition. Springer, Berlin Heidelberg New York 2016, ISBN 978-3-662-49280-2 , pp. 178-181.
Web links
- The official website of the AO Foundation
- The official website of the German Society for Trauma Surgery
- Guidelines of the German Society for Trauma Surgery (AWMF)
Individual evidence
- ↑ with own ears heard in Bochum, July 1984. The auditorium responded with "ohohoh" and "hear, hear!"
- ↑ A. Sarmiento in the foreword to non-operative functional fracture treatment , s. above .
- ↑ Lorenz Böhler: The techniques of bone fracture treatment. 13th edition, Maudrich Publishing House, Vienna 1951.
- ↑ H. Tscherne in L. Schweiberer (Ed.): Traumatology 1 - Conservative and operative fracture treatment. 2nd Edition. Urban & Schwarzenberg publishing house, Munich / Vienna / Baltimore 1987, ISBN 3-541-14482-3 , p. 3. (Breitner et al .: Surgical Operations Theory . Volume VIII)
- ↑ Since January 1, 2004, the official job title has been “ health and nurse ”.
- ↑ Christoph Weißer: The bone fracture treatment at Martin Kirschner and the development of the "Kirschner wire". Notes on a brilliant idea in surgery. In: Würzburg medical history reports. 12 (1994), pp. 5-18; Pp. 8-11
- ↑ Walther Müller: On the technique of wire extension of fractures (drilling through thin wires with the rotating cannula. "Drill wires" for lateral pulling.) In: Zentralblatt für Chirurgie 58, 1931, pp. 1490-1493; here: p. 1493
- ↑ Here you can find a review of fractures near the hip joint, see pp. 11, 34, 60ff., 84
- ↑ F. Pauwels: About the importance of the construction principles of the supporting and musculoskeletal system for the stress on the long bones. In: Acta Anat. 12, 1951, pp. 207-227.
- ↑ F. Pauwels: Manuscript of the Aschoff lecture June 24, 1958. In: Ingo Klute, Norbert M. Meenen: The fracture of the kneecap. Booklets for the trauma surgeon. No. 269, 1998.
- ↑ AO Principles of Fracture Management, Thomas P. Rüedi, Richard E. Buckley, Christopher G. Moran
- ^ AO Surgery Reference