Anterior tooth trauma
| Classification according to ICD-10 | |
|---|---|
| K08.1 | Tooth loss due to accident, extraction, or localized periodontal disease |
| K08.3 | Remaining tooth root |
| K08.81 | Pathological tooth fracture |
| K08.88 | Other specified diseases of the teeth and the tooth supporting system |
| K08.9 | Diseases of the teeth and of the gums, unspecified |
| S00-S09 | Injury to the head |
| S02.5 | Tooth fracture |
| S02.08 | Alveolar process fracture |
| S03.2 | Tooth Dislocation |
| S0.050-S0.058 | Superficial injury to the lip and oral cavity |
| ICD-10 online (WHO version 2019) | |
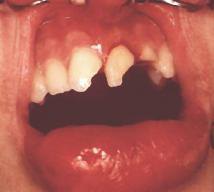
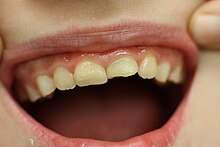
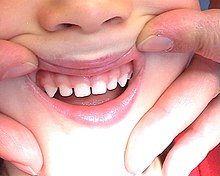
An anterior tooth trauma or anterior tooth injury is an injury to the anterior teeth and neighboring structures caused by force. Front teeth are incisors and canines . In the case of anterior tooth trauma, the upper incisors are almost exclusively affected and the canines or lower incisors only very rarely. Such mechanical trauma is usually caused by a blow, impact or fall.
Traumatic tooth injuries (so-called dental accidents) almost exclusively affect the front teeth. Fractures of teeth in the premolar and molar area due to external force are very rare. It must be an extremely strong punch or kick.
The anterior tooth trauma is divided into tooth compression, tooth dislocation and tooth fracture, the latter again into crown fractures and root fractures.
As prevention against a front tooth trauma is one of some sports mouth guard worn.
Frequency and causes
There has been a significant increase in anterior tooth trauma in children, adolescents and adults for years. About half of children will suffer tooth trauma before leaving school. In the foreseeable future, dental trauma will exceed the number of dental caries and periodontal diseases and will become the main threat to dental health.
With a prevalence of 22%, injuries to permanent teeth pose a major threat to dental health in children, and the extent of damage caused by tooth decay and periodontal disease in the future will even exceed them.
About 30% of eight to twelve year old children have suffered anterior trauma to the permanent incisors. The incisors of the upper jaw in particular are most frequently affected because of their exposed position. Anterior tooth trauma affects 90% of the upper jaw and only 10% of the lower anterior teeth.
The most common causes are falling, falling, brutality offenses (punch), traffic accidents , household accidents and others (e.g. hoof kicks). Bicycle accidents are very common among falls. Game and sports injuries (e.g. colliding with another player while playing soccer) are often the cause of anterior tooth trauma, with particularly modern fast sports such as mountain biking , rollerblading , skateboarding , and snowboarding increasingly being represented in anterior tooth trauma. Anterior tooth injuries are also typical and very common in ice hockey . When swimming , the front teeth are often damaged by falling on the edge of the pool. In Australia, surfing is the leading cause of dental intrusion. For a while, with the advent of the aluminum scooter fad , these were a common cause of accidents.
The frequency peak of traumatic dental injuries to the milk teeth is at the age of 18 to 40 months, as the toddler learns to walk and becomes very mobile at this age , but on the other hand is still very careless and moves very uncoordinated. Trauma to the milk teeth is usually caused by falling or colliding while the child is learning to walk and run.
The causes of anterior tooth trauma in the deciduous dentition are mostly falls while playing (fallen on the swing or the slide), falls on stairs or simply the unsteady gait of the toddler, for example stumbling over an obstacle and holding his hands in his pocket.
Classification of tooth injuries
On May 13, 2016, a new S2k guideline was published by the AWMF . In charge : German Society for Dentistry, Oral and Maxillofacial Medicine (DGZMK) and German Society for Oral and Maxillofacial Surgery (DGMKG) for the therapy of dental trauma to permanent teeth.
| Fractures | Dislocations |
|---|---|
| Enamel fraction: visible crack in the enamel without loss of substance | Concussion no dislocation. no relaxation. only percussion sensitivity. |
| Crown fracture: limited to the enamel (= enamel fracture) | Loosening; no discocation; increased mobility; Percussion sensitivity; Bleeding from the sulcus is possible. |
| Crown fracture (enamel, dentin. Without pulp involvement): uncomplicated crown fracture. Enamel-dentin fracture. | Oral lateral displacement. often wedging in this position. Bite disorder; Dislocation in the vestibular direction with or without wedging i. S. an intrusive dislocation (Both forms have in common the dislocation of the tooth including the fractured, firmly adhering buccal lamella.) |
| Crown fracture (enamel, dentin. With pulp involvement): Complicated crown fracture. Enamel-dentin fracture with exposure of the pulp. | Extrusion incisal dislocation. high mobility (the tooth is attached to the pulp or some dentogingival fibers.) |
| Crown-root fracture (with and without pulp involvement) Crown fracture extending into the root: Mobile crown fragment is often still attached to the gingiva. Exposure of the pulp is not mandatory. | Intrusion dislocation towards the apical; Wedging in the alveolar bone; Discrepancy between gingiva and tooth circumference; Alveolus distended buccally; No percussion sensitivity; no sulcus bleeding; metallic percussion sound. |
| Root fracture without communication with the oral cavity: Horizontal or oblique fracture of the tooth root; often increased mobility of the coronal fragment, possibly with discocation. | Avulsion; complete detachment of the tooth from its alveolus. |
| Root fracture communicating with the oral cavity: Horizontal or oblique fracture of the tooth root; often increased mobility of the coronal fragment, possibly with discocation. | |
| Longitudinal root fracture: complete longitudinal tear with communication with the oral cavity. |
- modified by Bastone according to WHO
Fracture of the dentate alveolar process
Vertical or oblique fracture of the alveolar process with / without course through the alveolar compartment, i. d. Usually concerning several teeth; with / without dislocation (occlusion disorder); Resilient deflection possible under pressure. Tears in the gingival mucosa i. d. R. interdentally visible; with / without bleeding from the sulcus.
Soft tissue injuries (lip, cheek, tongue)
Accompanying tear / crush / laceration of the soft tissue in close positional relationship to the impact of the traumatic forces; i. d. R. accompanied by heavy bleeding; with / without penetration of foreign bodies (tooth fragments, etc.).
dislocation
In the case of dislocation, there is a displacement or loss of the tooth, the tooth is partially or completely detached from the alveolus ( tooth socket ). At the same time, the tooth supporting apparatus is injured.
A total dislocation is the complete absence of the tooth in the alveolus; the tooth was completely knocked out of the alveolus ( tooth socket ) due to the trauma , which is empty. This type of tooth loss is also known as complete or complete dislocation, disarticulation or avulsion ( Avulsio = violent pulling out).
In the subluxation , as well as partial dislocation, called incomplete dislocation or incomplete dislocation, there has been a tooth to a traumatic abnormal change in position. This goes hand in hand with a significant mobility of the tooth (tooth loosening), which far exceeds the normal degree of tooth mobility . However, the tooth is still in its normal position in the row of teeth .
In the case of lateral dislocation , the tooth is shifted to the side (usually in the vestibular or palatal / lingual direction ).
The subluxation (incomplete dislocation) and the lateral dislocation (complete dislocation) are also combined to form the peripheral dislocation and contrasted with the central dislocation .
In the central dislocation , also known as intrusion or impression referred to, this is a shifting of the tooth in the jaw, into the alveolus into it. The tooth looks shorter than normal. It is often pressed very deeply into the alveolus. It may have been driven almost completely into the socket and is no longer visible. The bone of the alveolus has inevitably been compressed and fractured by the tooth root of the tooth hammered into the jaw.
With an extrusion , the tooth protrudes from the tooth socket. It looks longer than normal, is highly mobile and is only partially held in the alveolus by root fibers. Since no direct tensile forces are applied to the tooth in the event of a trauma, as is the case with tooth extraction , for example , the elongation of the tooth can be explained by a previous brief lateral dislocation, whereby the tooth is in front of some remaining fibers of the tooth support system ( Sharpey fibers ) the total dislocation was preserved.
In addition to central dislocation (intrusion), tooth dislocation is always accompanied by loosening of the tooth. This forceful loosening of a tooth is always accompanied by a complete or partial tearing of the Sharpey fibers (holding fibers of the tooth root).
Compression (contusion)
A dental upset (Kontussion / bruise , engl. Dental concussion ) is a strong vibration of the tooth, with an injury of the gums (contusion of the periodontal ligament / ligament ), a periodontal edema and possibly also accompanied by a Pulpaschaden. Most of the time, however, there is only a minor injury when a tooth is struck. When the tooth is struck, the tooth is not loosened, but temporarily more or less painful for tapping and bite pains can be triggered. Even if there is no dislocation (loosening) of the tooth and it has remained in its correct anatomical position, it may have been briefly compressed a millimeter into its alveolus, which can damage the tooth supporting structure. In the case of tooth contusion, the x-ray shows an inconspicuous or widened periodontal gap, as there is an injury to the periodontium.
The main problem with contusion is that it can initially lead to a negative vitality reaction for a few days to weeks. So a negative sensitivity test immediately after the accident and in the first few weeks afterwards is not a sure sign of a non-vital pulp. In the case of a negative vitality test, this must therefore be repeated regularly, usually weekly, as a tooth after a compression occasionally only reacts negatively to the vitality test temporarily and there is still the prospect of improvement. Even with a positive vitality test, regular vitality checks are recommended in the first few weeks and months.
Because pulp necrosis may occur later, long-term follow-up checks are advisable, including regular sensitivity checks for at least one year and, if the root growth has not yet been completed (in mixed dentition), monitoring the root development with x-rays ( dental film ). Parents should be informed about possible late signs of pulp necrosis:
- vestibular swelling
- vestibular fistula
- Tooth discoloration
- Bite pain
- Root resorption
As long as the tooth is definitely not devitalized, no urgent therapy is required for tooth contusion. Initially, only rest is recommended, which is why the patient should only eat soft foods. If the bite is more severe, the tooth may have to be ground in (taken out of the occlusion ) so that it is no longer stressed during normal biting.
Even an additional tooth discoloration is not a sure sign of a non-vital pulp, as it can also be hemorrhage in the vital pulp. A tooth bite sensitivity can still be rated as a normal pain reaction to a contusion and is not necessarily a sign of a devital pulp.
It is advisable to wait for several weeks, especially in the case of teeth with not yet completed root growth, where, due to the wide open apical foramen, it is very likely that no exact root filling can be made up to the tip of the root. The treating dentist can only be sure that the tooth is devitalized and that a root canal treatment is required when the tooth becomes more sensitive to bite bite and more painful knocking occurs and the follow-up of the vitality test continues to be negative.
Root canal treatment of immature teeth
A root canal treatment is with an open foramen apical quite problematic. Since there is no clear stop in the area of the foramen during preparation of the root canal, the root canal can easily be over-instrumented. Due to the lack of a stop (lack of apical constriction), there is a risk of overfilling the root during root filling. Without this stop, which has not yet formed due to the incomplete root growth, there is no control during the filling of the root canal.
With normal, complete root growth, the root filling should extend to the narrowest point at the tip of the root, the physiological foramen, which is approx. 1–2 mm higher than the actual anatomical foramen. If the root growth is incomplete, the area of the wound on the foramen that is in contact with the root filling is one order of magnitude larger. The root filling is often delayed by months of deposits of calcium hydroxide, which are changed weekly, in the hope that during this time the root tip closes or is closed by regrowing bone. The root filling, the technique of which is normally based on advancing the gutta-percha point to the mechanical stop, is also very problematic. As a last resort in the event of an unsuccessful root filling (too short or too long), a subsequent root trimming is available in the event that the tooth discomfort occurs again.
It is controversial whether a root canal treatment is indicated in the case of tooth discoloration (gray coloration) after an anterior tooth trauma, but without further symptoms. In these cases, it is often not known exactly whether and when a trauma occurred. Discolored milk teeth without further discomfort (no vestibular swelling or fistula) can be left in place and do not have to be trephined. Often the children are still too small and unapologetic to endure a root canal treatment with the necessary calm. Later on, the milk front teeth are just about to change teeth and with a root treatment there is a risk of damage to the permanent tooth that follows.
Even more severe anterior tooth trauma, such as crown fractures or root fractures (see below in the section tooth fractures ), are accompanied by tooth contusion. In particular, enamel-dentin fractures without a pulp opening do not normally require a root canal treatment. Because of the accompanying tooth contusion, however, the vitality test can also turn out negative here, with all the associated problems of vitality assessment - as described above.
Therapy of the dislocated tooth
A partially dislocated tooth is digitally repositioned (pushed back into the alveolus) and fixed with a splint .
A completely dislocated tooth can possibly be re-implanted.
In the case of deciduous teeth, however, replantation is not indicated after a total dislocation, since on the one hand a possible infection can damage the subsequent permanent tooth, on the other hand its loss does not weigh so heavily.
Despite the dramatic appearance, an intruded tooth must not be manipulated. The greatest chance of success is to wait for the spontaneous eruption, which usually occurs in deciduous teeth and in permanent teeth with not yet completed root growth . The intruded tooth is usually firmly wedged in the socket. Only when there is loosening has it appeared to be. An attempt at extrusion should only be made after waiting several weeks without success.
Splint
A splint is intended to fix a loosened tooth in its anatomically correct position in order to enable healing. The splint also stabilizes the tooth and thus reduces the pain during movement when eating and during oral hygiene. In the case of a replanted tooth, splinting enables it to remain in the alveolus. There are various options for splinting a dislocated tooth:
- Directly manufactured composite splints are manufactured in the patient's mouth without the involvement of a dental laboratory. These composite splints are suitable for temporary restoration. However, they are not very durable when exposed to stress for several days, such as chewing or grinding at night, and the plastic (composite) quickly detaches from the tooth or breaks. They also hinder oral hygiene considerably
- Reinforced composite rails consist of the same material as the directly manufactured composite rails, which, however, is reinforced with other materials in the sense of a composite material (similar to the principle of fiberglass-reinforced plastic or reinforced concrete ). Wires or small glass fiber mats can serve as reinforcement material
- Ring adhesive splints are made of titanium , for example , they can be manually adapted to the dental arch and are then fixed on the teeth using composite (acid etching technology).
- that are bonded to the teeth with composite and then connected with wire.
- Mini plastic splints according to Drum ( bite splint ) consist of a 1 mm thick plastic film that is deep-drawn on a tooth model (deep-drawn splint)
Depending on the author, the type of splint and the degree of loosening of the teeth, the splint should remain in the mouth for 1–2 weeks or, in the case of extensive injuries to soft tissue and bones, 6–8 weeks. At the same time, the vitality of the loosened tooth must be checked regularly.
Because of the restricted oral hygiene due to the pain and the splint, a mouthwash with chlorhexidine is recommended during this time . This antiseptic rinse, which should be done several times a day, can be very effective in improving oral hygiene for one to two weeks.
The wire splints used for the fracture splint (for the intermaxillary lacing ) are practically impossible to fix in the deciduous dentition because the deciduous teeth have a deep tooth equator . As a result, the contact point is located close to the tooth neck and the ligature wires for fastening a splint can only be threaded through under the contact point with considerable damage to the gingiva. The wire ligatures also do not find a hold on the conical tooth crowns. These wire ligature-based splints, adopted from the treatment of jaw fractures, should no longer be used for the fixation of dislocated teeth; instead, the plastic arch wire splints described above are the method of choice for tooth dislocations. The wire ligature splints are the Schuchardt archwire plastic splint and consecutive figure eight ligatures :
- In the Schuchardt archwire plastic splint (combination splint according to Karl Schuchardt , 1901–1985), a curved wire splint made of semicircular soft steel wire is adapted to the vestibular tooth surfaces of the row of teeth. This arch wire, located halfway between the incisal edge and the gingival margin, is attached to the individual teeth by means of ligature wires, which are passed under the contact points of the teeth and then individually twisted. Finally, the ligature wires and the splint are covered with a self-curing plastic (Paladur) so that they do not slip. The arch wire is made of rung rail (with cross struts on both sides), the rungs on one side are bent onto the wire surface so that the rail does not slip when the ligature wires are put on. If these are then applied, twisted and covered interdentally with plastic, the archwire can no longer slip and these rungs are cut off. After the plastic has hardened, the occlusal hooks are removed. The splint then sits absolutely firmly in the interdental spaces due to the retention. The rungs on the other side can be cut off before the rail is attached, as they are not required. Normally, in the case of jaw fractures for which they were originally designed, they take up the rubber rings for the intermaxillary lacing.
- Continuous figure eight ligatures without an additional arch wire splint must be attached in such a way that they do not come to lie under the tooth's equator on the loosened tooth, as otherwise they develop an extraction force. The splint must encompass at least two adjacent healthy teeth on either side of the loosened tooth. Such figure-of-eight ligatures are now more likely to be viewed as emergency measures for short-term splinting if no other materials are available.
- The Pfeiffer plastic cap splint can also be used well in deciduous teeth. It is made hands-free from a plastic, self-curing plastic (auto-polymerisation). To do this, the plastic, which is formed into a roll, is pressed onto the chewing surfaces of the row of teeth and manually modeled on the tooth surfaces vestibular and palatal. The splint, which has not yet fully hardened, is removed from the mouth again, since otherwise it would be fixed to the undercutting tooth surfaces if it had hardened completely in the mouth. The fully hardened splint is then worked out outside the mouth - the excess is removed so that the gingiva is exposed, the splint is smoothed so that the "chewing surface" of the splint allows grinding movements. For the final adjustment of the splint, it is used again, this time with a thinly mixed plastic. It is recommended that small children work in a band that can be put out of the mouth and attached to clothing to prevent them from swallowing or losing the splint.
The bone fragments of a limited alveolar process fracture that are firmly attached to the tooth root can possibly also be adequately fixed using a dental splint, so that if there is sufficient immobilization, no oral surgery is necessary on the bone.
Too rigid fixation of the injured tooth was recognized as a problem, since there is then the risk of dentoalveolar ankylosis or progressive pathological external root resorption (replacement resorption). The physiological mobility of the traumatized tooth and the neighboring teeth should also be maintained during splinting. The Schuchardt archwire plastic splint was originally intended for splinting broken jaws. According to a basic principle of bone fracture treatment, the fragments should be rigidly fixed in order to achieve absolute immobilization and thus primary bone healing . Dislocated teeth, in which the fibers of the tooth-holding apparatus are always entrained, can, however, heal osseously in the alveolus if the splint is rigid, which is undesirable. Further information on the problem of dentoalveolar ankylosis can be found in the section Tooth Rescue Box .
Tooth rescue box
A knocked out tooth must be found again. It should then only be touched by the tooth crown. In no case should the root of the tooth be touched. Even if the tooth is dirty, it should not be cleaned by laypeople. It must be stored as moist as possible. A special tooth rescue box is best. If necessary, the tooth can be kept moist in cold UHT milk, sterile saline solution or in the mouth of the parents (or the child).
The tooth rescue box is offered in pharmacies. It is a screw cap container with a cell culture medium . The tooth can be stored in the storage solution of the tooth rescue box at room temperature for up to 24 hours. When placing the tooth in the tooth rescue box, the tooth may only be touched by the crown of the tooth so that the periodontal membrane is not additionally damaged.
The periodontal membrane must not dry out if the tooth is to heal properly again. In the case of dead periodontal skin, the tooth can only heal in the bone (ankylos). Such an ankylosed tooth will be resorbed by the osteoclasts of the bone over the course of the next few years as part of the constant bone remodeling and replaced by normal bone. In the X-ray image, a hint of a root outline in the bone can often be seen even years later - similar to a petrified tree, where actually only the stone has taken the shape of the remains of the tree. Ultimately, such teeth soon fall out as the root is completely resorbed by the bone.
Even with heavily soiled, knocked out teeth that are found again, the dirt particles adhering to the tooth must not be rinsed under tap water (or in other water), as this does not have the same salt concentration as isotonic saline solution and the cells of the periodontal membrane are additionally damaged by the osmotic gradient can be.
The further prognosis of the knocked out tooth after the replantation depends on how much time has passed between the knocking out and placing in the tooth rescue box. The manufacturer of the tooth rescue box recommends a maximum period of 30 minutes. Other sources state that all the cells of the periodontal membrane of a knocked out tooth have died after two hours.
The storage liquid in the tooth rescue box has an anti-infectious effect. The tooth should therefore remain in the tooth rescue box for at least 30 minutes, so that the storage solution can better develop its full anti-infectious effect, the box should be gently swiveled regularly to ensure that new, unused fluid washes around the tooth.
Tooth fracture
Main article: Tooth fracture
In the case of tooth fractures, a distinction is made between crown fractures (on the clinical crown of the tooth) and root fractures (on the tooth root ) , depending on the location . Depending on the course of the fracture lines, a distinction is made between transverse, longitudinal and oblique fractures.
Crown fracture
Fractures of the tooth crown are divided into
- Tooth enamel fractures ( enamel facture) (often only small breaks). It is rarely just cracks (infracture). The break line then extends into the dentine. However, no hard tooth substance has been lost. There are also the regularly occurring small, harmless enamel cracks / cracks in the enamel that do not go beyond the enamel-dentin boundary . As a rule, enamel cracks do not require any special therapeutic measures.
-
Dentin fractures (in the dentin) - more precisely: enamel-dentin fracture, since a dentin fracture can only occur if the enamel fractures at the same time - with or without pulp involvement
- Dentine fractures without opening the tooth pulp (tooth pulp , "tooth nerve")
- Dentin fractures with opening of the tooth pulp
Tooth enamel fractures on incisors can be treated very well with a composite filling (plastic filling, adhesive technique ). In the case of very small tooth enamel fractures, often no filling is required; more or less light grinding and rounding of the sharp fracture edges is sufficient, also for aesthetic correction. After all, over the course of a few years, the cutting edge wears off naturally while chewing.
In the case of dentine fractures without pulp opening (without pulp involvement), a composite filling is placed or the tooth shape is restored using a tooth crown. The exposed dentin is more yellowish than the tooth enamel and is sensitive to pain. It should be covered with a filling as it can become infected. In the case of larger dentin fractures that are already close to the pulp, an indirect capping of the pulp is necessary before filling or crown therapy (usually with calcium hydroxide ).
In dentine fractures with pulp opening (with pulp involvement), there is depending on the time that has passed since the tooth fracture, depending on the severity and other circumstances (age of development of the tooth; is the apical foramen - the tip of the root - still open - in younger children or is it already closed?) different treatment options:
- direct capping
- Vital amputation (pulpotomy, removal of the living pulp in the tooth crown) or
- Vital extirpation (removal of the living pulp up to the tip of the root - root canal treatment ).
After the pulp wound has been treated, the fractured crown can then be treated with a filling or a dental crown.
Pure tooth enamel fractures are always without pulp involvement (pulp opening), since the pulp lies only in the dentin and is completely enclosed by it.
Reattachement restoration of enamel-dentin fractures
In the case of uncomplicated crown fractures (i.e. without opening or damaging the pulp and without tooth loosening), there is the possibility of reattaching the broken tooth fragment. The prerequisite is that the broken fragment of the traumatized tooth is still present. This technique in the sense of minimally invasive dentistry often offers an advantage over the aesthetic restoration of tooth fractures with composites, where the choice of color and shade coordination does not always produce optimal results. Composite restorations also have the disadvantage of lower abrasion resistance compared to tooth enamel.
The reattachment of the tooth fragment by means of the adhesive technique, also called reattachement restoration ( reattachement is pronounced in English), is a time-saving and very aesthetic restoration process.
The refixation of the fragment is best done using a nano-hybrid composite (because of the lower polymerization shrinkage than conventional composites), after conditioning using bonding. The breaking strength is improved if a bevel is prepared on the fracture line of the tooth before refixation. The bevel also has a positive effect on the C-factor (the ratio of bound and free surface). It should be noted that aesthetic restorations of tooth fractures that are made exclusively from composites (i.e. without the tooth fragment) have a very high C-factor, which is why they often last a very long time.
Broken tooth fragments that were stored dry for a long time before refixation change their color due to dehydration. However, this is not a further problem, since this aesthetic impairment soon disappears on its own after reattaching. However, multiple, non-repositionable or missing fragments do not allow a reattachment restoration, so that the dentist only has the option of a conventional composite or ceramic restoration.
Root fracture
The decisive factor for the subdivision and treatment of the root fractures is their location in the upper, middle or lower third of the root.
In the case of fractures in the upper third of the root, the tooth crown cannot be preserved; it must be extracted. To preserve the tooth, a root canal treatment and then a prosthetic restoration with a tooth crown is required. The crown must be anchored using a root post ( post crown ). The clinical crown can only be built up with composite (plastic filling) if the fracture occurred directly at the level of the tooth neck . A pen assembly is then required.
In the case of fractures in the middle third of the root, preservation of the tooth is not possible - the tooth must be extracted . The fracture in the root is not expected to heal, on the other hand, after the removal of the upper half of the root and the crown, no prosthetic restoration with a pin crown can be performed, as this is technically impossible. Even the attempt to preserve the tooth by surgical removal of the apical root fragment has no prospect of success, since the coronal tooth fragment does not have sufficient anchoring in the bone.
In the case of fractures in the lower third of the root, the apical root fragment (the root tip) is removed by means of a root tip resection . In the case of advanced periodontal disease ( periodontitis ) with advanced bone resorption, however, there is also the risk that the tooth will no longer be held firmly enough in the bone, especially with root fractures in the upper part of the lower root third.
In the case of longitudinal fractures of the tooth root, only extraction is possible as therapy. These teeth often still seem to have sufficient stability, and they can also be obtained painlessly with a root canal treatment, but the longitudinal gap that creates a connection between the oral cavity and the tooth supporting structure is a source of constant infections that ultimately lead to tooth problems and tooth loss. Longitudinal fractures of the root occur very rarely in anterior tooth trauma. Rather, they are a relatively common complication of endodontic teeth, teeth with post abutments and teeth with large amalgam fillings . The longitudinal fracture of the crown then continues as a longitudinal fracture in the root, whereby it can only reach a few millimeters below the gums or to the tip of the root.
If the root fracture is subgingivally at the level of the tooth neck, sufficient drainage for a composite filling is not possible. The fractured tooth root can possibly be lengthened:
- surgical tooth lengthening (dislocation of the root in an occlusal direction, possibly with an additional gingival excision)
- Orthodontic extrusion of the root: for this purpose, brackets are glued to the neighboring teeth, an archwire is attached to them, a lag screw is anchored in the root canal of the fractured tooth after a root canal treatment and elastic bands are then stretched between the lag screw and the archwire, thus providing an extraction force for six weeks to exercise on the root, then the root is fixed for another two to three months.
Accompanying injuries
The accompanying injuries are no longer counted as part of the actual anterior tooth trauma.
Common intraoral associated injuries of Fronzahntraumas are injuries to the oral mucosa, lacerations (Rissquetschwunde / laceration / Vulnus lacero-contusum) the marginal gingiva ( gums to the tooth neck), especially with dislocations. The associated bleeding is usually not dramatic, as there are no larger vessels in this region. By the time the patient is presented to the dentist, they have usually come to a spontaneous standstill and the dentist only recognizes the bleeding that has occurred from the blood-soiled clothing.
If the upper lip is subjected to violence, the force of which is then passed on to the upper incisors, cracks or bruises can also occur on the inside of the upper lip (labial mucosa / lip mucosa ) or in the vestibule. These can be accompanied by mostly slight bruises ( hematoma ) and often severe swellings ( edema ), with the massive swelling of the lip usually disappearing very quickly, within one to two days.
A rare and therefore easily overlooked complication is the blasting of smaller tooth crown fragments into the lacerated wound on the inside of the upper or lower lip. The mostly frightened, psychologically traumatized, crying child is often spared the detailed and painful examination of the already painful lip wound, so that such fragments can easily be overlooked. In addition, there is regularly the psychological pressure of accompanying parents who want to spare their child further pain and take a natural parental protective position. If necessary, the detailed examination of the lip wound must be postponed for a day or two when the parents and child have calmed down again, the lip has swollen a little and palpation of the lip and probing the wound is no longer quite as painful. A tooth fragment overlooked in the lip wound can heal into the wound without irritation, be encapsulated in a fibrous manner and remain symptom-free for years. It can then be discovered as an incidental finding due to a cartilage-hard hardening in the lip. The tooth fragment can then be recognized on an x-ray (dental film) of the lip and removed from the lip with a minimal surgical procedure.
Extraoral soft tissue injuries in anterior tooth trauma mainly affect the chin, the outer lip (red lips) and the nose. Most of them are abrasions. These must be cleaned and disinfected thoroughly because of the risk of infection, but also because of the risk of dirty tattoos . In the case of very sharp-edged or very strong violence (e.g. hoof kick), severe injuries to the external soft tissues can also be present (e.g. splitting / tearing of the red lips).
Tetanus immunization should be considered, especially with accompanying extraoral wounds . If there is no tetanus immunization, a passive and active vaccination must be initiated immediately - tetanus simultaneous vaccination .
The dentist must absolutely rule out a jaw fracture ( upper jaw fracture , lower jaw fracture ). For this he studied orienting whether the occlusion by a dislocated is disturbed (moved) fracture. He shakes the teeth of the upper jaw to roughly convince himself that it is not mobile or sensitive to pain because of a fracture.
For an exploratory examination to exclude a jaw fracture, anamnesty is asked whether the patient has pain when biting in the posterior region - in order to eliminate the bite pain in the anterior region, the patient can bite on a roll of cotton to increase the bite. If there are no indications of a mandibular fracture, pressure on the mandible can be used to determine whether pain has been provoked at a possible fracture gap. By applying moderate lateral pressure on the right and left lower jaw area, an attempt is made to compress the rigid dental arch, which in the absence of a lower jaw fracture causes no pain and also excludes a non-dislocated fracture of the body of the lower jaw ( corpus mandibulae ).
Especially in the case of a lower jaw fracture at the level of the joint neck (near the temporomandibular joint ) or at the head of the mandibular joint ( caput mandibulae ), there is a risk that the growth zone of the lower jaw on the epiphysis ( epiphyseal plate ) of the joint head is affected and the growth of the lower jaw is interrupted, resulting in a so-called bird's face. which greatly disfigured the person affected as an adult. For a preliminary examination of such a fracture of the articular process ( processus condylaris ), pressure must be exerted on the chin several times. The mouth must be open so that it is not fixed by the teeth with the upper jaw. The pressure must be in the direction of the tongues, in the direction of a chin hook . The examiner's hand, lying on the patient's chin, only needs to perform very light and then somewhat stronger "pushes". If there is a fracture on the ascending branch of the jaw, this causes pain. Finally, the movement of the temporomandibular joint head on the temporomandibular joint should be palpated (scanned). To do this, the dentist inserts a finger into the patient's external auditory canal (index finger or, better, little finger) and lets the patient open and close their mouth several times. The movement of the joint head of the lower jaw can be felt on the front of the external auditory canal. Alternatively or additionally, the movement of the temporomandibular joint can also be felt directly in front of the auditory canal, directly in front of the tragus . Again, ask about pain and check for tenderness. In the absence of pain from provocation, this fracture can be excluded. In cases of doubt, a specialist ( oral surgeon ) should always be called in. A fracture of the joint neck must under no circumstances be overlooked by the treating dentist.
If a jaw fracture is suspected, X-rays must be taken for further diagnosis ( orthopantomogram ) and a maxillofacial surgeon should be called in, who will have X-rays made in further projections (upper jaw overview, computer tomography ) if necessary .
Other accompanying injuries in the mouth, jaw and face area can include:
- Alveolar process fractures (the bone fragment can contain, for example, all four upper incisors including their alveoli - a combination with tooth fractures or tooth dislocation is possible)
- Impal injuries to the soft palate or the posterior wall of the pharynx
traumatic brain injury
In addition to an anterior tooth trauma, traumatic brain injury (TBI) can also exist. Especially if the dentist is the first to treat recent trauma and the patient was not presented to a doctor after the trauma, the dentist must always think about a possible traumatic brain injury. The diagnosis of a possible traumatic brain injury does not belong in the specialist field of a dentist. Nevertheless, the dentist should also question the traumatized patient for signs and examine them: Was the patient briefly unconscious after the trauma? Is there retrograde amnesia ? Did he vomit after the trauma ? Are the pupillary reflexes to light normal? Is there an anisocoria ? Is the eye movement disturbed? Are there double vision ? Do you have a headache ? Are there any signs of whiplash (showing normal neck mobility)? Are there bruises or minor wounds on the skull (palpate the skull for orientation)? Do you feel dizzy ? Do you have hearing or vision problems?
However, if there is no evidence or suspicion of a traumatic brain injury, no referral to a doctor is required. At the slightest suspicion, e.g. B. because of the severity of the accident described, a referral to a doctor is always appropriate in case of doubt.
documentation
Good documentation of the accident data is very important for the treating dentist (how?, When? Where?, Exact accident location, accident time, described course of accident, first aid doctor / doctor / dentist / rescue specialist), damage (cracks in the gingiva, bleeding, exact location and size of the fracture fragments, degree of tooth loosening, tooth displacements, accompanying abrasions and lacerations, bone loss due to periodontal disease, caries as a secondary finding), diagnostics (vitality test) and therapy.
Accidents and tooth injuries on the way to school and at school (school accident ) are insured (in Germany) outside of the statutory health insurances through the statutory accident insurance: Employer's liability insurance association , community accident insurance association ( accident fund ). They cover the treatment costs and often send detailed questionnaires to the treating dentist after weeks . With these accident reports, the cost bearers regularly ask for detailed information on the course of the accident, place, time, etc. Accidents can also lead to increased claims for damages by the accident victim.
Despite medical confidentiality, there is an obligation to provide information to these service providers. According to § 201 SGB VII "data collection and data processing by doctors", the insured person is to be informed by the doctors about the collection purposes and about the doctors' obligation to provide information. According to §§ 60 ff. SGB I, there is also an obligation to cooperate for the beneficiary (the patient) .
These cost bearers are often also obliged to assume the costs of consequential damage even after many years and strive to precisely delimit the actual accident damage from previously existing damage or later illnesses, so they want complete and careful documentation from the treating dentist, who is particularly involved in such anterior tooth trauma must take the legal documentation requirement very seriously. Dental accidents must be reported to the insurance company by the patient and the dentist.
Ellis classes
In the Anglo-Saxon region, fractures of the tooth crown are divided into Ellis classes . This classification distinguishes Ellis I - III:
- Ellis class I - enamel fracture
- Ellis class II - enamel-dentin fracture without pulp involvement
- Ellis class III - enamel-dentine fracture with pulp involvement
Dentition of the maxillary anterior teeth in the primary and permanent dentition
The physiological eruption time of the central incisors is in the seventh / eighth year of life. According to the dentition table by Schour and Massler (1941), at the age of 3 years (plus / minus 6 months) the root growth of the milk threes in the upper jaw is not yet complete. However, the apical foramen is already closed on the milk ones and twos (milk incisors) . The roots of the milk ones and twos are still completely preserved at the age of three. The crowns of the central and lateral permanent incisors are at the level of the root tips of the deciduous incisors. At the age of 4 years (plus / minus 9 months) the resorption of the roots of the milk ones begins. The crowns of the permanent ones and twos are already fully mineralized and enclosed by the upper jawbone. At the age of 5 years (plus / minus 9 months) the roots of milk ones and milk twos are approximately one third resorbed. At 6 years of age (plus / minus 9 months) the roots of milk ones and milk twos are approximately half resorbed, while the roots of milk three have not yet begun. At the age of 7 years (plus / minus 9 months) the permanent 1 has partially broken through and half of its root is formed. The permanent twos, whose root is 30% developed, is about to break through. At the age of 8 years (plus / minus 9 months) the permanent twosome has partially broken through and 50% of its roots are formed. At 9 years of age (plus / minus 9 months) the roots of the permanent ones and twos (central and lateral permanent incisors) are two-thirds developed. By the age of 10, the roots of the permanent ones and twos are 95% developed, their apical foramen is still not closed. At the age of 11, the apical foramen is closed on the permanent single and double of the upper jaw.
The deciduous incisors of the upper jaw erupt at 8 to 10 months (one) or at 10 to 14 months (two).
The milk ones break through at 6 to 10 months, the milk twos at 10 to 14 months, whereby the teeth of the lower jaw usually break through a little earlier than those of the upper jaw. The eruption times of permanent teeth are subject to greater individual fluctuations than those of milk teeth. Often there are deviations of ± 3 years from the normal breakthrough time.
Anterior tooth trauma to the permanent (permanent) teeth usually occurs in adolescents. The eruption age of the upper permanent incisors in the upper jaw is:
- Boys
- Permanent ones (central incisors, teeth 11 and 21): 6.94 years ( standard deviation 0.65)
- Permanent twos (lateral incisors, teeth 12 and 22): 8.25 years (standard deviation 1.15)
- girl
- Permanent ones (central incisors, teeth 11 and 21): 6.2 years (standard deviation 1.05)
- Permanent twos (lateral incisors, teeth 12 and 22): 7.59 years (standard deviation 1.11)
Because of the frequent deviation of the chronological age from the biological age, there is a fluctuation range of plus / minus 9 months for the breakthrough times.
See also
literature
- Horst Kirschner, Yango Pohl, Andreas Filippi: Accidental injuries to teeth: Prevention - Rescue - Treatment. Elsevier, Munich 2006, ISBN 978-3-437-05106-7
- Gert J. Grubwieser, Michael Baubin, Heinrich J. Strobl, Robert B. Zangerle: Checklists for current medicine, checklist for dental emergencies: guidelines and compendium for emergency management in dental practices and clinics. Thieme, 2002.
- Johannes Einwag, Klaus Pieper: Practice of dentistry. Elsevier, Munich 2007, ISBN 978-3-437-05251-4 .
- Jens O. Andreasen, Francis M. Andreasen, Lars Andersson: Textbook and Color Atlas of Traumatic Injuries to the Teeth. 2007, Blackwell Publishing, ISBN 978-1-4051-2954-1 , text of the book on google-books
Web links
- Information about first aid for dental accidents
- zahnunfall.de
- International Association of Dental Traumatology (IADT)
- dentaltraumaguide.org
- Herbert Deppe: The anterior tooth trauma - current diagnostic and therapeutic aspects.
Individual evidence
- ^ Jens O. Andreasen, Frances M. Andreasen: Dental traumatology: quo vadis. Endod Dent Traumatol 1990; 6: 78-80
- ↑ The consequences of tooth injuries in adolescents . ( dentaly.org [accessed May 6, 2018]).
- ↑ Barbara Brückmann: Orthodontics: Braces - yes or no? Ed .: Stiftung Warentest . 2015, ISBN 978-3-86851-875-7 .
- ↑ Therapy of dental trauma to permanent teeth , S2k guidelines, AWMF . Retrieved June 19, 2016.
- ↑ EB Bastone, TJ Freer, JR McNamara: Epidemiology of dental trauma: a review of the literature. In: Australian dental journal. Volume 45, Number 1, March 2000, pp. 2-9, PMID 10846265 (review).
- ↑ Springer Medicine (ed.): The Maxillofacial Surgeon . Volume 1/2008 - Volume 11/2018 edition.
- ↑ Splint therapy after dentoalveolar trauma . (PDF) Joint scientific statement of the German Society for Dentistry, Oral and Maxillofacial Medicine (DGZMK) and the German Society for Dental Preservation (DGZ), July 16, 2005
- ↑ Studies on splint therapy for dentoalveolar injuries (Dissertation, 2002, PDF; 1.5 MB)
- ↑ Thomas von Arx, Andreas Filippi , Daniel Buser, Splinting of traumatized teeth with a new device: TTS (Titanium Trauma Splint). Dental Traumatology 2001; 17: 180–184, online (PDF; 190 kB)
- ^ Andreas Neff, Christoff Pautke and Hans-Henning Horch: Traumatology of the facial skull. In: Heinz-Henning Horch (editor): Oral and maxillofacial surgery. Publisher: Urban & Fischer bei Elsevier; 2006; ISBN 978-3-437-05417-4
- ^ Karl Schuchardt: A suggestion to improve the wire splint associations. 1956, Deutsche Zahn-Or-Kieferheilkunde 24: 39-44
- ↑ Norbert Schwenzer: Dental, Oral and Maxillofacial Medicine: Dental Surgery: 35 tables / ed. by Norbert Schwenzer; Michael Ehrenfeld. With contrib. By Uwe Eckelt ... . Georg Thieme Verlag, 2009, ISBN 978-3-13-116964-8 , p. 67–.
- ↑ Gabriel Krastl, Andreas Filippi, Roland Weigersdorf: Anterior trauma: dental hard tissue injuries. Retrieved May 3, 2018 .
- ↑ Bhargava Megha, IK Pandit, N. Srivastava, N. Gugani, M. Gupta: An evaluation of various materials and touth preparation designs used for reattachement of fractured incisors. In: Dental Traumatology , 2010, 26, pp. 409-412, PMID 20831637
- ↑ dentalresource.org management of dental trauma in children
- ↑ I. Schour, M. Massler: The development of the human dentition. 1941, Journal of the American Dental Association , 28: 1153-1160
- ↑ Peter Schopf: Curriculum Orthodontics. Volume I . Quintessent Verlag, Berlin 1994, ISBN 3-87652-569-1
- ↑ Jürgen Stefan Wedl, V. Schoder, M. Guertekin, R. Schmelzle, RE Friedrich: The eruption times of the permanent teeth in boys and girls. Oral Prophylaxis & Pediatric Dentistry 26 (2004) (PDF; 100 kB)