wound
A wound (from Old High German wunte 'wound', 'blow', 'injury', like Latin vulnus from Indo-European wen , 'suffer'; Greek trauma ) is a defect in the protective covering tissue (separation of the tissue connection ) on the outside (skin) or inside (Mucous membrane) Body surfaces with or without tissue loss. In most cases it is due to external force caused, but also the sole result of a can disease be like as an ulcer ( ulcer ).
In psychological damage is commonly known in the broad sense of a psychological wound , an emotional trauma or psychological scar spoken (see Trauma (psychology) ) .
Classification
root cause
Through external violence :
- Occasional wounds are accidental injuries from accidents or intentionally damaging injuries, e.g. B. with cutting and stabbing weapons . They are always colonized ( contaminated ) with germs and tend to secondary healing without adequate treatment .
- Surgical wounds occur during medical operations and are methodologically unavoidable. Clean surgical wounds that were created under sterile conditions can primarily heal. Classic surgical wounds are cuts that are inflicted with a scalpel . Minimally invasive operations create stab wounds with the trocar that are much smaller. The skin is seldom opened with the thermocautery (heat from electricity) , rather the mucous membrane . Also lasers come on the skin ( dermatology and cosmetic surgery ) and the eye ( ophthalmology ) in application.
Because of illness . The causes are:
- Sensory disturbances or painlessness that do not allow minimal injuries or constant pressure to be felt: coma, diabetic or alcohol-toxic neuropathy and much more,
- motor inability to change position independently: motor paralysis, infantility,
- Circulatory disorders that prevent problem-free healing of even minor wounds: arteriosclerotic or diabetic micro- and macroangiopathies .
Types of wounds
A distinction is made between the following types of wounds:
- Wounds mechanically caused arise either by sharp force (cut, puncture, blunt or bite) or by blunt force ( survey (excoriation) , cracking, crushing or laceration , bullet wound , impalement , degloving wound (décollement) (by shearing forces caused ), Scalping and decubitus (due to constant pressure mostly on support points) or as combined mechanical wounds. Both sharp and blunt force can lead to partial or complete separation of limbs .
- Thermal wounds are caused by burns , scalds, or frostbite .
- Chemical wounds are caused by chemical burns on the skin or mucous membranes caused by acids (coagulation necrosis ) or alkalis ( colliquation necrosis).
- Radiation-related (actinic) wounds occur when the skin is exposed to ionizing rays such as X-rays , radioactive isotopes or UV radiation . In some ways, radiation wounds resemble burn wounds. However, their healing is much more problematic because the radiation effect on the entire organism has an additional negative effect on healing.
topography
A distinction is made topographically (in terms of location), external and internal wounds: The latter can be observed in gunshot or deep stab wounds from weapons, but also in speared bone fractures and in rapid injuries (motor vehicle accidents ). What is feared here is, on the one hand, pronounced bleeding from vascular or heart damage or from tears in the spleen or liver . On the other hand, there is a risk of infection through the opening of germ-colonized hollow organs such as the intestine or urinary bladder . Thirdly, life-threatening dysfunctions in injuries to the brain , heart or lungs are encountered in such wounds.
On the other hand, what is probably the most common internal injury, bleeding into loose soft tissue in the event of a bruise , does not count as a wound by definition if it is found without cutting the body surface at the same time.
complexity
A simple wound is distinguished from the complicated wound .
A simple wound is an injury to the skin, subcutaneous tissue (fat layer), possibly fascia (connective tissue body shell) and, in the case of a compound wound, also muscle . A lesion of the mucous membrane without perforation is also assigned to this group. Here healing is often easy and safe to achieve. The simple wound caused by external violence, which affects the muscle tissue but is not organs and not life-threatening, is also called a flesh wound .
A complicated wound includes an injury to the tendon sheaths , tendons, joints , vessels, or nerves. Wounds with organ damage and opening of cavities (body cavity, chest , skull) also belong to this group. The treatment requires great medical knowledge and should not be attempted by any layperson.
Healing process
- Primarily healing (p. P. = By primary intention) wounds only occur on clean wounds with no gaping edges. This condition is aimed at through the definitive wound care . A scar is line-shaped or barely visible.
- Secondary healing (p. S. = By secondary intention) wounds are those in which there is a tissue defect that the organism has to close through newly formed connective tissue (scar) and skin, or those with massive germs that prevent primary healing. The germ type can be prepared by a wound smear identified and the efficacy of antibiotics are determined by antibio- or resistogram. When the healing process is complete, a broad scar is visible.
- The regenerative type of wound healing, epithelial wound healing, is a special case. It sometimes takes place under scabs and only in very superficial wounds in which only the epidermis has been damaged by an injury, and not in those with primary or secondary healing wounds deeper tissue layers are affected. In epithelial wound healing, the epidermis grows from the edge and the defect closes through epithelialization. With this type of wound healing, neither granulation tissue forms nor does a contraction occur. Since only the top layer of skin was injured, no scar forms.
infection risk
The greatest risk is caused by injuries from contaminated instruments at the pathologist, skinner, butcher, fisherman or injuries to contaminated laboratory glass fragments (microbiologist). One rightly fears contamination with germs that have already passed through humans or animals and have become more virulent. This risk group also includes needle stick injuries to medical staff and addicts (from used cannulas ). Transmission of HIV and hepatitis is possible with both.
Wounds soiled with garden soil or street dust or even wounds acquired in the trenches are classified in a completely different group . There is a threat of infection with dormant spores ( tetanus or gas fire ).
Another group includes machine injuries such as on conveyor belts, rollers, mowing machines or gearboxes. The tissue destruction and subsequent blood flow throttling favors addressing any wound germs.
The lowest risk of infection in the group of occasional wounds is a cut from an unused, clean kitchen knife.
Wound healing
The wound healing is a natural biological process and already begins minutes after wounding. The goal of healing measures is a complete, functional and cosmetic restoration ( restitutio ad integrum ), which can only rarely be achieved in full. A visible scar often remains ( defect healing ).
It is only up to the doctor to optimize the conditions to alleviate symptoms ( wound pain ), to prevent complications or infections , to prevent delays and to make the cosmetic result as optimal as possible. There is still no real acceleration of wound healing. When changing dressings , doctors or nurses observe the healing progress, clean the wound area and, if necessary, the wound area and protect the wound with an artificial cover.
A distinction is made - not uniformly and without contradiction - between three to five phases of wound healing that overlap in time, are based on classic light microscopic examinations and are only visible to the naked eye in secondary healing wounds. The starting point of every wound healing is a disturbance of the blood flow through capillary injuries . The initial bleeding initiates blood clotting , the destroyed blood vessel is closed by a clot (blood clot) .
- It begins with the latency phase or the resting phase , since apparently no macroscopically or microscopically visible reactions occur. (In many classification schemes, it is assigned to the following phase, as it is usually short and difficult to define.)
- Exudation phase , cleaning, inflammation or inflammation phase : During the clot formation, a fibrin network is formed, which enables the edges of the wound to stick together. Clear wound secretion, which consists of serum , is interspersed with inflammatory cells. In clean conditions, this phase should not last longer than one to three days. Excess wound secretion ( exudate , "escaping liquid") can "wash out" foreign bodies and germs from the wound in secondary healing wounds. During this phase, mitosis (cell division) increases in the wound area. Monocytes mature into macrophages in the wound area , which clear away cell debris and plug. Fibroblasts , which develop from immigrated, but also from connective tissue cells located in the wound edge and multiply through cell division, perform the actual construction work in the following phase. This requires a moist wound environment, which is reproduced by modern bandages.
- Proliferative phase , granulation : Through Education (proliferation) of the wound defect is increasingly populated by new connective tissue, it creates the visible coarse grained Füllbindegewebe ( granulation tissue ) . Hand in hand with the cell-rich filling of a wound defect is the breakdown of the fibrin network (through fibrinolysis ). At the same time, the number of blood vessels increases due to the sprouting hair capillaries ( angiogenesis / vascularization) . With very small wounds, this phase can begin after a few hours. In general, it lasts from the fourth to the twelfth day. Between the sixth and tenth day, the collagen fibers begin to mature. The entire process is very complex and is subject to the influence of numerous growth factors ( cytokines ). The granulation tissue can only develop in a timely manner if there is no general or local malnutrition (no insufficient blood circulation ) and no uncorrected metabolic diseases hinder growth.
- In the regeneration phase, the surface wound is closed by epithelialization ( covering tissue of the epidermis as epithelial tissue ). The diameter of a well granulated wound closes to one third only by shrinkage to two-thirds by new formation (cell division of surface cells and cell migration on the "slideway" liquefied fibrin) from the edge of the wound for wound centers. The granulation tissue underneath increasingly forms collagen fibers , with the restoration of all skin layers being almost complete. However, since no elastic fibers are formed, the scar tissue inevitably lacks the elasticity of healthy skin. That is why a minimal scar is aimed for in therapy planning. The regeneration phase lasts from about the thirteenth day up to several weeks.
- Maturation ("maturation") is sometimes referred to separately as a further functional adaptation of the scar tissue to the different local requirements. The further increase in the tear strength of the scar tissue depends on the cross-linking, solidification and alignment of the collagen fibers. The water content of the tissue decreases, the scar that initially protrudes slightly above the skin level regularly shrinks below the skin level. The number of vessels in the scar tissue also decreases. The originally fresh red stigma turns white. This process takes one to two years.
Wound treatment
A distinction is made between two treatment phases only for occasional wounds:
- provisional wound care
- definitive wound care
Temporary or provisional wound treatment
It is a first aid item and does not apply to surgical wounds. The wound of opportunity requires one:
- The wound is covered with a wound pad, for example made of gauze or with newer dressing materials, and is fixed with elastic bandages. Cyanoacrylate adhesive can be used to cover wounds for simple grazes or cuts . Foreign bodies that have penetrated deeply must not be removed before the patient is transported because, on the one hand, they may have perforated vessels or hollow organs which cannot be supplied on site and, on the other hand, it is difficult to precisely determine the extent of the injury in the operating room due to premature removal. They remain fixed, protected from movement during transport and further intrusion. On large burns or scalds not want ointments are applied. The clothing should be extinguished, but left unchanged on the victim's body, provided it or its combustion products are not toxic. However, in the case of acid or alkali burns, the soaked clothing must also be removed in order to avoid further damage.
- Immediate immobilization of extremities.
- The immobilization as part of the first aid is usually done with vacuum or other positioning rails.
Definitive wound care
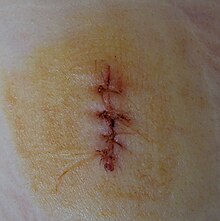
This section applies to all types of wounds. Here, too, the fight against pain and hemostasis for shock prophylaxis are imperative and important.
The fight against pain
- In the case of extensive injuries, systemic analgesia affecting the entire body can be carried out and is supplemented by local anesthesia as part of surgical wound care, or the entire care is performed under anesthesia .
Surgical wound care
- includes the removal of foreign bodies and definitive hemostasis by means of vascular sutures or ligation of vascular stumps.
Operative wound dressing for occasional wounds
- The following two alternative treatments are not used on aseptic surgical wounds.
- A distinction is made in terms of effort, healing success and practicality:
- a wound toilet according to Erich Lexer : cleaning, debridement with or without a lock
- the excision of the wound according to Paul Leopold Friedrich : total excision including the wound base, only with a knife, with or without wound closure
- It is based on Friedrich's attempts at wound healing, who examined the temporal spread of germs in contaminated wounds and postulated an excision within six hours to avoid an effective infection. But it is often not practical for casual wounds. In this way, nobody will cut out a nerve or important vessel at the wound base.
The wound closure
The methods of closure are more diverse today than they were a century ago. The edges of the wound can be:
- Approach (adapt), e.g. B. with special plasters (Steristrip®, Leukostrip®),
- Sewing (with various stitch techniques and needle designs),
- Brackets and finally
- glue
These procedures can occur in combination.
Wound coverage
- Open wound treatment in the narrower sense is only permitted in rare cases. A closed, i.e. primary healing wound can be adequately protected from renewed contamination with a spray bandage . However, sterile gauze plasters are still common. In the case of damaged wounds and especially secondary healing , newer wound dressings such as hydrocolloid -containing moist dressings , which promote undisturbed biological wound healing , products made from seaweed or silver-containing dressings because of their oligodynamic effect , which are intended to promote infection control, are used despite higher costs .
Immobilization
- Immobilization is a double-edged matter. The biological healing takes place in the early phase under complete rest undisturbed. Infections from unavoidable contamination seem to be less common. Therefore, splints or plasters, or at least immobilizing bandages made of soft material, are still applied. On the other hand, the early functional dosed mobilization is important for the sliding of sutured tendons, for the prevention of capsular shrinkage of the joints, for the maintenance of muscular strength (otherwise catabolism ), and even for the physical and psychological well-being.
Tetanus prophylaxis
- Because a more than 30% fatal infection with tetanus can be avoided by simple, harmless and inexpensive vaccination , the injured person has to be checked for vaccination protection within 6 to 12 hours and, if necessary, immunized. The prophylactic vaccination in the event of injury should be carried out according to the recommendations of the Standing Vaccination Commission ( STIKO ) of the German Medical Association .
Antibiosis
- Not every wound heals undisturbed. Therefore prophylactic or therapeutic antibiosis can also be part of wound treatment.
Prophylactic antibiosis
- A preventive dose is simply unnecessary in the case of simple wounds, to be rejected because of the increased resistance to antibiotics, especially in hospitals (see infectious hospitalism ) and, thirdly, it is costly.
- The situation is different when it comes to operations on organs that are contaminated with bacteria, such as the large intestine, or when it comes to risky operations such as the heart. In this case, standardized antibiotics based on randomized and recognized studies are required. This is usually administered parenterally ( intravenously or intramuscularly ), i.e. it has a systemic (= body-wide) effect .
Therapeutic antibiosis
- A wound healing disorder inside the body after severe, traumatic violence can lead to blood poisoning ( sepsis ). In such cases, therapeutic antibiotic treatments are undisputed. However, in the case of a severe wound, it should not automatically be concluded that there is a therapeutic necessity.
Wound healing disorder
A wound healing disorder occurs when the physiological course of wound healing is prevented. This either leads to the spontaneous rupture of the wound or makes surgical wound revision necessary. Not only septic (infectious) wound healing disorders are problematic. Wounds with haemophilia ( blood disease) also tend to have dangerous bleeding and more difficult wound healing due to coagulation disorders due to missing or insufficient coagulation factors in the blood.
Wound healing disorders can be classified according to time and cause.
| Wound healing disorder |
acute | chronic |
| aseptic |
Hematoma seroma Wundrandnekrosen wound dehiscence wound rupture ( burst abdomen ) |
hypertrophic scar keloid atrophic ulcer |
| septic (infection) | pyogene W. putride W. anaerobe W. toxic W. viral-toxic W. |
Fistula infected ulcer |
Brief comments on those listed in the classification:
Acute wound healing disorders
Aseptic wound healing disorders
These wound healing disorders are not caused by germs. The most well-known are:
- The wound hematoma and seroma
- A wound hematoma is an accumulation of blood and blood clots in the wound gap, which is painfully dispersed as a result. The pain is proportional to the increase in pressure in the tissue. Small amounts of blood are removed from the body with the formation of colored breakdown products of hemoglobin, which diffuse into the wound area and are visible blue-red, then purple, and later green. Larger clots, on the other hand, liquefy and sediment. The almost colorless supernatant is called a seroma .
- Liquefied hematomas and seromas can be punctured aseptically with a cannula in the event of pain and excessive size . The risk of infection must be weighed against loss of pain and cosmetic improvement. Large hematomas that are not relieved are ultimately “organized” as a scar , which can lead to a reduction in functionality.
- The wound edge necrosis
- Here the wound edge is no longer supplied with blood, but has died. It looks yellow instead of pink. Since this condition does not affect all layers and the entire suture area, the wound does not have to diverge. But the necrotic tissue "demarcates" and, if left untreated, a secondary healing wound with a poor appearance results.
- The wound dehiscence or the suture gap
- This is the term used to describe the divergence of the wound edges. In most cases, this complication only becomes visible when the suture material is removed at the usual appointment. If the tension is too great, it is possible that the threads at the edge of the wound tear prematurely, i.e. cut through and the wound therefore gapes. If internal wounds do not heal, i.e. if they gape, it is called suture insufficiency . Since excreta (gastric, intestinal juice, stool, bile) get into the free abdominal cavity, the dangerous clinical picture peritonitis develops
- The seat stomach
- A space belly is a special case of seam insufficiency related to the abdomen . It often doesn't appear until a few days after the operation. A distinction is made between two forms, the open space belly , in which all layers of the abdominal wall have moved apart and the intestines, mesh , liver or other organs appear visibly in the wound. One must distinguish from this the covered space belly , in which mainly only the deeper, supporting layers of the abdominal wall ( fascia ) have moved apart. Since the skin often only has a small gap, this condition is often misunderstood. A typical sign is the emergence of ascites like a spring.
- Both forms are apart from exceptional cases urgent re surgery. Possible causes that caused an increase in abdominal pressure are eliminated and the abdomen closed again. The urgency arises on the one hand from the imperative to rule out any other undesirable surgical complication in the body and on the other hand to avert an abdominal cavity infection ( peritonitis ).
Septic wound healing disorders
This group is usually not divided according to the clinical appearance, but according to the pathogen groups:
-
pyogenic wound infections
- They are caused by the classic pus pathogens such as streptococci or staphylococci . But mixed infections are also not uncommon. First and foremost, the wound abscess or the phlegmon should be mentioned , the pus of which spreads from the wound into gaps in tissue such as tendon spaces in the deep palm or on the forearm.
-
putride wound infections
- Putrefactive germs play an important role in such wound infections. The typical pus odor that occurs here is even noticeable to the layperson. Phlegmons dominate among the clinical pictures, the courses of which are much more difficult.
-
anaerobically unspecific wound infections
- Anaerobic germs in a mixed flora are dominant here. Such infections are more likely to occur with circulatory disorders.
- anaerobic- toxic wound infections. Two clinical pictures with very specific pathogens stand out here:
- The gas fire and the tetanus , detailed in the two main articles.
- Although the tetanus infection is one of the wound infections and is mentioned here, it must be noted that the wound itself often heals, it is not actually a wound healing disorder .
- The clinical picture of a gas fire is a serious, life-threatening wound infection.
-
viral-toxic wound infections
- Only rabies is generally known .
Chronic wound healing disorders
Wounds that take an unusual, chronic course to heal are also based on other diseases and are therefore only symptomatic of those. Even when using the most modern methods of local wound treatment, such a “chronic wound” can only be healed when the underlying disease has been cured or ameliorated.
Delayed wound healing can be caused by circulatory disorders ( PAD ) or varices . A diabetes mellitus alone can already delay healing for an unbalanced metabolism.
Noble metals, germ-free and chemically stable plastics, even certain glasses, can heal in the organism as so-called foreign bodies (Latin: Plur. Corpora aliena) after injuries or operations . If, on the other hand, the materials are incompatible, such as non-ferrous metal or large amounts of dead bone tissue (so-called sequesters ) or even infected, purulent secretion occurs, initially encapsulated in an abscess . The pus later empties through non-healing, tubular tissue crevices, the fistulas , to the surface of the body as long as the causative material is still in the body. This type of fistula, the so-called tubular fistula, has (in contrast to a lip fistula) no inner lining of the mucous membrane. Therefore, once its cause has been eliminated, it heals quickly.
There is no reliable information about the frequency of chronic wounds. It is estimated that 1–2% of the adult population of western industrialized nations suffer from a chronic wound. The probability of developing a chronic wound increases with age and is also estimated at 4–5% from the age of 80. The unclear data situation is due to the unclear definition, in particular from when one can speak of stagnation in the healing process or of chronicity .
See also
- Hospital infections
- Maggot therapy for wound healing disorders
- Care planning and care documentation
- Ignaz Semmelweis (is considered the founder of antisepsis, germ reduction in clinics)
- Multi-resistant germs and penicillin
- German Society for Wound Healing and Wound Treatment e. V.
literature
- Klaus-Jürgen Bauknecht, Joachim Boese-Landgraf: Wounds, wound healing, wound healing disorders, wound treatment, tetanus prophylaxis. In: Rudolf Häring, Hans Zilch (Hrsg.): Textbook surgery with revision course. (Berlin 1986) 2nd, revised edition. Walter de Gruyter, Berlin / New York 1988, ISBN 3-11-011280-9 , pp. 7-17.
- Liliane Juchli , M. v. Mügler, Dudli u. a .: care. Practice and theory of health and nursing care. 7th edition. Thieme, Stuttgart 1994, p. 1065 ff.
- V. Kozon, N. Fortner, E. Donaty, Th. Wild: Standard for performing a wound dressing. In: Austrian care magazine. 11, 2003, pp. 25-28. ( PDF file download ( Memento from September 17, 2011 in the Internet Archive ))
- P. Mahrhofer, A. Mayer: To connect or not to connect. Postoperative wound management in times of pronounced frugality in the healthcare sector. In: Speculum - Journal of Gynecology and Obstetrics. 24, 2, 2006, pp. 8-11. ( PDF file download )
- University Hospital Eppendorf: Standard for changing dressings . ( PDF file download )
- GMS : Interdisciplinary hospital hygiene . Journal of the German Society for Hospital Hygiene (DGKH). Volume 1 (2006): The infected problem wound. [with 33 contributions]. ( PDF file download )
- Peter Kujath, Angela Michelsen: Wounds - from physiology to dressing . In: Dtsch Arztebl . No. 105 (13) , 2008, pp. 239-248 ( Article ).
- S3 guideline for local therapy of chronic wounds in patients with the risks of peripheral arterial disease, diabetes mellitus, chronic venous insufficiency of the German Society for Wound Healing and Wound Treatment. In: AWMF online (as of June 2012)
- Joachim Dissemond : Visual diagnosis of chronic wounds. 3. Edition. Viavital, Cologne 2016, ISBN 978-3-934371-55-2 .
- Kerstin Protz: Modern wound care. 8th edition. Urban & Fischer, Munich 2016, ISBN 978-3-437-27885-3 .
Web links
Individual evidence
- ^ Friedrich Kluge , Alfred Götze : Etymological dictionary of the German language . 20th ed., Ed. by Walther Mitzka , De Gruyter, Berlin / New York 1967; Reprint (“21st unchanged edition”) ibid 1975, ISBN 3-11-005709-3 , p. 869.
- ↑ Klaus-Jürgen Bauknecht, Joachim Boese-Landgraf: Wounds, wound healing, wound healing disorders, wound treatment, tetanus prophylaxis. 1988, p. 9 f.
- ↑ Acute wounds. Schülke , accessed on March 17, 2019 .
- ↑ K.-J- Bauknecht, Joachim Boese-Landgraf: Wounds, wound healing, wound healing disorders, wound treatment, tetanus prophylaxis. 1988, p. 7.
- ↑ Hans Lippert (Ed.): Wundatlas Compendium of complex wound treatment. Georg Thieme Verlag, Stuttgart 2006, ISBN 3-13-140832-4 , p. 31.
- ↑ Klaus-Jürgen Bauknecht, Joachim Boese-Landgraf: Wounds, wound healing, wound healing disorders, wound treatment, tetanus prophylaxis. 1988, pp. 12-14.
- ↑ Joachim Dissemond: Blickdiagnose Chronic Wounds. About the clinical inspection for diagnosis. Viavital Verlag, Cologne 2016, p. 11




