puberty
Under puberty (of lat. Puberty "puberty") is meant been around since the 16th century, the part of the adolescence , in which the development physiological course of sexual maturation sexual maturity in terms of fertility , including by functional reproductive organs reached, and in the further course also leads to a full-grown body through growth and body shape changes. Then there is the growth of armpit and pubic hair.
This phase of life begins when the pituitary gland sends a hormonal signal to the body to increase the production of sex hormones in certain organs and release them into the blood . In boys it is primarily testosterone , in girls it is estrogen . Normally, the puberty in girls between 10 and 18 years and in boys between 12 and 21 years of age go through.
At this stage of development, the significantly increased concentration of sex hormones in both sexes leads to the full expression of the secondary sex characteristics , such as sex-specific body hair and the female breast . In girls, menstruation ( menarche ) begins during puberty and shortly afterwards the formation of fertile egg cells ( ovulation ) in the ovaries , in boys increase in muscle mass, growth of the penis and testicles, sperm production in the testicles ( sperm arche ), and beard growth and the deepening of the voice . The onset and course of puberty are primarily genetically controlled, with the puberty genes KiSS1 and KiSS1R (formerly GPR 54 ) being of particular importance.
While it was previously assumed that human sexuality only develops with puberty, it is now recognized that human beings have sexual impulses even as children (see also: Infantile sexuality ).
Physiological basics

Regardless of gender, there is a simultaneous production of estrogens and androgens such as testosterone in children long before puberty , albeit slight compared to the period of sexual maturity , but in boys and girls in different proportions. Since significantly more estrogens are produced and released in girls and more androgens in boys, estrogens are referred to as female and androgens as male sex hormones.
Boys
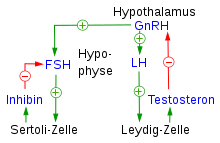
In male children and adults, the production of testosterone and thus of the closely related, but clearly masculinizing, androsterone, as well as the production and release of estrogens in very small quantities in the Leydig cells of the testes ( 8 ) takes place.
This flow is via the in hypothalamus (directly above 2 ) of GnRH neurons distributed gonadotropin releasing hormone (GnRH), which in the anterior pituitary ( 2 formed) follicle stimulating hormone (FSH), and which is also formed there gonadotropin luteinizing hormone regulated (LH) .
The total testosterone consists of 40 to 50% bioactive, i.e. H. Albumin- bound testosterone as well as SHbG- bound testosterone (50 to 60%) and free testosterone (1 to 2%). Independent of this regulation, the adrenal glands ( 5 ) develop androgenic adrenal glands .
girl
Here, the hypothalamic gonadotropin-releasing hormone and the gonadotropins FSH and LH formed in the anterior pituitary gland regulate the estrogens produced in the ovaries (over 7 ). The estrogens also formed in the adrenal glands ( 5 , also on the female side) are not subject to this regulation. The estrogens include the most biologically effective estrogen 17-β-estradiol (17β-estradiol), the much weaker and so far only recognized as biologically insignificant estrone (estrone), as well as at least 20 other estrogens.
Hormonal changes before puberty
Nowadays, in a healthy, well-nourished human body , the hormonal changes that underlie puberty usually begin at the age of eight or nine. The increased production of sex hormones triggers and promotes sexual maturation. On the one hand due to an interaction with the increasingly formed sex hormones under the regulation of the produced in the hypothalamus somatotropin-releasing factor (SRF = GHRH = GRF) and somatostatin in the anterior pituitary intensified growth hormone ( somatotropin ) and on the other hand in the thyroid ( 3 ) thyroxine prepared and poured out. In the course of sexual maturation, this leads not only to the testosterone effect but also to an increased increase in body size ( puberty growth spurt ). With the onset of puberty, the thymus ( 4 ) recedes ( involution ) in both sexes , so that later in adults only a residual thymus body or retrosternal fat body remains, which mainly consists of adipose tissue .
Boys
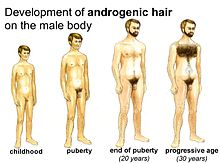
As the gonadotropin concentration in the blood rises, the testosterone production in the Leydig cells of the testes increases in boys well before puberty itself. This male sex hormone shapes the secondary sexual characteristics in general, leads to muscle and body growth and is also responsible for increasing body hair . The gonadotrophin initially controls the onset of pubic and armpit hair ( pubarche ) and, in the course of puberty, also the development of beard hair , chest hair and other body hair.
As a result of the testosterone level increase by two to three times shortly before puberty, the growth of the penis , scrotum , testicles, epididymis , spermatic ducts , seminal vesicle , prostate , preputial and bulbourethral glands is stimulated. Therefore, it is possible for boys that shortly before puberty occurs for the first time during an orgasm - albeit a very small - excretion of predominantly prostate secretions ( ejakularche ), which very often also as ejaculation in the sense of "seedless effusion" referred to as. In general, the prerequisites for this are a particularly strong expression or development of the primary genital organs, slight sexual excitability, sexual interest and more frequent sexual activity that is perceived as unencumbering, pleasurable and satisfactory (mostly masturbation ). Boys masturbate for the first time on average around the age of twelve, according to several studies. During puberty, the proportion of boys and men who masturbate regularly is very high and is close to 100% in 15-year-old men. Most teenagers masturbate on average several times a week to several times a day; the average is around eight to nine times a week.
girl
In girls, too, the ovaries slowly and continuously begin to produce more estrogens before puberty and the gonadotropin concentration in the blood rises, which they also release into the blood. This increase in sex hormones then triggers the onset of breast development ( thelarche ) and the development of the uterus and vagina . The development of female proportions and the regulation of menstrual cycles are also dependent on estrogens.
On the other hand, small amounts of androgens are formed in the adrenal glands of girls before puberty begins, which stimulate length growth and the beginning of pubic hair development ( pubarche ).
Maturation in puberty
The age at which these changes occur is variable, but the sequence of changes is usually constant. The Tanner stages classify these changes and divide pubertal physical development into five categories from child to adult.
Boys

Under the influence of the testosterone level increase triggered by the increased gonadotropin concentration, the enlargement of the testicles continues in the course of puberty and the surface texture and color of the scrotum begin to change. In addition, this hormone stimulation continues the growth of the penis, the epididymis and the accessory sex glands and the first pubic hairs appear at the latest at the beginning of puberty. Only then does the boys' body growth increase. Even before the peak of this growth, the testes usually begin to produce their first sperm in the middle of puberty . The spermarche occurred within the years 1980 to 2001 by 1.7 years earlier. At the end of this period it averaged between 11.9 and 12.4 years. Although, according to projections and estimates since 1860, girls have had their first menstruation several years earlier, compared with the beginning of the surveys at the end of the 19th century, boys are more likely to reach sexual maturity than girls. The figures are approximate. In close proximity to this - about 14 days - there is then a first ejaculation in the sense of "ejaculation" ( ejakularche ), either with an orgasm that is consciously triggered by sexual activity or with a first pollution (polluarche). This means that sexual maturation has reached its target point, “sexual maturity”. With the desire to function, due to the synchronous central control by the pituitary gland, the psychological component of the ability to choose and accept partners is also regulated and just as fertility is present.
Initially, the ejaculate contains only a few sperm, mostly of poor quality, so that fertility is initially significantly reduced, but not completely excluded. When, on average, body growth has reached its peak at around 13 years of age, the enlargement of the testicles and penis is almost complete. The first pubic hair appears as the hairline after the sperm ark ( Tanner stage 2 ). The boundaries of the pubic and head hair remain unchanged in boys (as in girls) for two years (the thesis of some researchers is that although boys are sexually mature, they do not look like men), until this time window is closed within 14 days the whole body hair begins to sprout. The thickness of full body hair varies greatly both individually and in different populations . After the end of puberty, the increased testosterone level in male adolescents with its anabolic effect, together with somatropin, thyroid hormones and insulin, increases bone growth up to the genetically determined extreme value , at which the epiphyseal plates are then closed and thus the growth in length is also stopped.
During puberty, on the other hand, the testes also increase the production and release of estrogen, which, however, is significantly lower compared to testosterone production as it was before puberty. In about 50% of boys, a usually temporary and usually painless swelling of the breasts can occur during puberty . For a long time it was believed that this puberty gynecomastia is caused by the increased formation of estrogen and a resulting shift in the estrogen / testosterone ratio towards estrogen. A study in Denmark could not confirm this assumption. Instead, appeal to new findings that the significantly increased insulin-like growth factor insulin-like growth factor 1 (1 IGF) brings together with the increased estrogens that pubertal breast growth, also increased testosterone levels and an unchanged ratio of estrogen to testosterone.
The following table shows when the individual changes take place:
| change | Period |
|---|---|
| Testicular growth | 9-14 age |
| First effusion without semen (not mandatory) | 10-12.5 years of age |
| Penis growth | 10-14 age |
| First pubic hair | 9.5 - 12.9 years of age |
| First adolescent growth spurt | 11-14 age |
| First armpit hair | around 12-14. age |
| Upper lip fluff | 12-15 age |
| Voice wavers | 11-16 age |
| Voice deep | 13-17.5. age |
| First sperm cells ( Spermarche ) | 9-13 age |
| First ejaculation | after the time of Spermarche |
| Acne (not mandatory) | 14.-21. age |
| End of growth in length | 15-21 age |
girl
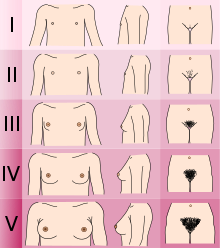
Through an increased production of the hypothalamic gonadotropin releasing hormones and the gonadotropins FSH and LH , the increased production and release of estrogens in the ovaries also continues in girls during puberty. The effects of these estrogens largely determine the subsequent development of puberty.
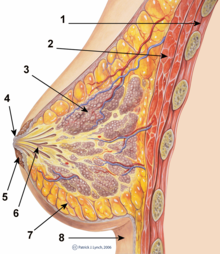
At the beginning, they are responsible for the continuation of breast development and promote the general growth of the mammary glands (Mamma, -ae; Latin Glandula mammaria , 3) - and thus also breast enlargement - at the same time a gradual, differentiating further development of these glands. In addition, the estrogens mediate the growth of the nipples ( nipples , lat. Papilla mammaria , 4) and the areola (lat. Areola , 5), as well as the pigmentation of the nipples and their erectability . In addition, the development of the overall typical female body shape with the associated fat distribution increases (here on the breast: 7).
However, these increased estrogen concentrations then also close the epiphyseal plates in girls during puberty and thus stop the growth in length. In addition, the estrogens also cause the relatively smooth border of the pubic hair.
The vulva also changes significantly in the course of puberty, since the external genitalia also reacts to sex hormones . The skin color changes, and the structures of the vulva become larger and more pronounced. This development affects the clitoris (5) and the inner (labia minora pudendi) and outer labia (labia majora pudendi) , but especially the hormone-sensitive skin of the vagina and its atrium.
The menarche (first menstruation) occurs only at the height of body growth when the girl's body is large enough to carry a child. However, no ovulation has taken place beforehand , which is why such a bleeding is also referred to as “withdrawal bleeding” and such a cycle is referred to as an “anovulatory cycle”. Only after a few more irregular bleeding of this type does the first ovulation ( ovularche ) occur and then the first real menstruation.
The significantly lower production and release of androgens in the adrenal glands of girls compared to estrogen production continues through puberty, stimulates length growth and the formation of pubic hair and is later also responsible for the appearance of armpit hair and possibly further body hair. The development of the breasts, pubic and armpit hair is usually complete at the end of puberty.
The following table shows when the individual changes take place:
| change | Period |
|---|---|
| First pubic hair | 8-13 age |
| First adolescent growth spurt | 8-15 age |
| The vagina and uterus begin to grow | 9-13 age |
| Beginning of breast development | 9-16 age |
| First menstrual period (menarche) | 10-16 age |
| Full breast development | 12-17 age |
| Acne (not mandatory) | from around 14-15. age |
Triggers for differences in puberty
Different factors have different degrees of influence on the course and severity of puberty in healthy individuals or groups.
Inheritance
Puberty is largely genetically controlled. The puberty genes KiSS1 and KiSS1R (GPR 54) are of particular importance within a so-called "hypothalamic gene network" with superordinate and subordinate genes, which interacts with other genes and gene networks of the body at all levels . The entire gene network influences the GnRH neurons in amplifying ( excitation ) and inhibiting ( inhibition ) control loops and thus influences the amount of gonadotropin-releasing hormones released by them. The KiSS1 gene encodes kisspeptin , which docks within a reinforcing control loop to the KiSS1 receptor encoded by the KiSS1R gene on the surface of the GnRH neurons and stimulates them to increase the release of gonadotropin-releasing hormones.
Identical twins develop almost synchronously . For example, the beginning of menstruation in female identical twins is one to two months apart, while it is up to twelve months for dizygotic twins.
Diet / exercise
Fat cells stimulate the production of sex hormones in girls so that sudden weight gain and an increase in body fat percentage can trigger sexual maturity. Eating disorders that set in early can delay puberty. Accordingly, girls who are very active in sport or girls with a very low fat percentage often only reach sexual maturity late.
Physical health
Various genetic defects with the resulting damage to various control circuits and nerve centers or disorders of the thyroid gland in childhood can either cause puberty to set in early or delay it, as well as preventing sexual maturity entirely. The first menstruation is often delayed in areas of poverty and consequently more infectious diseases and malnutrition.
Emotional health
Poor emotional health can cause puberty to start earlier. In families with many problems, starting a family early seems to be an adjustment.
Deviations from the normal course of puberty
In addition to the fluctuations in the beginning and course of puberty, which are regarded as normal, these can also occur prematurely or late outside of the normal fluctuations. Possible causes can be hereditary or triggered by certain diseases.
Premature puberty
Certain diseases or genetic reasons can lead to the premature onset of puberty symptoms, around the age of nine. This is known as precocious puberty . The causes include genetic defects and hormone-active tumors of the pituitary gland and hypothyroidism . Girls are significantly more often affected by precocious puberty than boys.
Delayed, stopped or missed puberty
A delayed onset of puberty ( Pubertas tarda ) occurs, for example, with mutations in the genes KiSS1 and KiSS1R (GPR 54) and with chronic diseases such as congenital heart defects , diabetes mellitus and, less often, with endocrine disorders such as Fröhlich's syndrome . The most common reason, however, is the constitutional development delay , which is genetically determined in the family and which subsequently leads to a normal puberty sequence (so-called late bloomers ). In addition, puberty can be halted or completely absent and is also classified as puberty tarda .
Mental symptoms of puberty
Puberty not only results in physical changes, it also influences the emotional state and social behavior of adolescents.
Mood swings, moodiness
While mood swings during puberty were often attributed to elevated hormone levels in the past, it is now clear that this relationship does exist, but is not as strong as assumed. Rather, a combination of hormonal and situational factors is responsible for mood swings and moodiness. Adolescents increasingly find themselves in problematic situations during puberty, especially when these situations are structured by adults ( lessons , work , family activities). The increased release of hormones means that people react to these situations with stronger feelings.
Relationship with parents
During puberty, both parents and teenagers report that they no longer feel so close to one another. One reason for the problems that arise between child and parents can be the child's improved judgment , which tends to question and criticize the parents' actions. In addition, the roles of young people in their lives change with physical maturity and they want to be treated as adults accordingly. The adolescents also want to take on more responsibility for their leisure time. However, the parents want to protect their children from harm and thus adopt a counter-position. Most of these quarrels are superficial and do not endanger protective family ties. The young people also quarrel with their siblings more often. Puberty is often referred to as the “second phase of defiance ” because of the arguments .
Sexual activity and contraceptives
How early and how often adolescents engage in sexual activity is linked to various factors. On average, adolescents have sex earlier for the following factors, especially when these are coupled:
- early onset of puberty
- Divorce of parents / single parents
- big families
- little or no religious commitment
- sexually active siblings and friends
- poor school performance
- low educational goals
- Tendency to non-standard behavior
In this context, it should be mentioned that 15% of boys and 12% of girls in Germany did not use any contraceptive during their first sexual act (focus report of the health reporting of the federal government 2004).
According to the 2006 Youth Sexuality study by the Federal Center for Health Education, twelve percent of 14-year-old girls have already had sex, which is exactly the same as in 2001.
After a few irregular "false" menstrual bleeding, ovulation sets in and with the sexual maturity achieved, the actual readiness to conceive also occurs. The period between the first “false” menstrual period (menarche) and the first ovulation varies in length for each girl and cannot be clearly determined solely by external observation without any aids. Puberty can be a little different for every girl and so the first "fake" menstruation can be so inconspicuous that it is overlooked or mistaken for white flow. Girls can be receptive a few days before the first ovulation, even before the first "real" menstruation, as the sperm can survive in the body for a few days.
In 2001, 7,447 children were born to teenage mothers in Germany, compared with 6,969 in 2004. The frequency of pregnancies among girls from socially weaker social classes is five times higher than that of the more established social classes.
enlightenment
Above all, responsible, practically active physicians, sex therapists, researching and teaching sexologists and also educators who are also or particularly concerned with the area of body and sexuality give parents or other legal guardians again and again the emphatic advice, in good time before the start of the sexual maturation physical changes to inform the children or adolescents concerned personally about these processes with factual accuracy, but in the simplest possible terms, in accordance with their age. A conversation that is as uninhibited, friendly as possible and, while respecting the privacy of the adolescent, is not to be replaced, for example, by simply providing educational literature. Without any proper personal explanation, there is a risk that either great or complete ignorance will be exploited by others to the disadvantage of adolescents, or incorrect information can trigger and perpetuate general uncertainty, perhaps even fears. On the other hand, there is the risk of inappropriate carelessness, so that a girl who has become sexually mature unnoticed may become pregnant unintentionally and the boy involved, who may also have become sexually mature unnoticed, is jointly responsible for such a pregnancy.
Web links
- Overview of puberty boys / girls from netdoktor.at
- Loveline - Information for young people on the subject of puberty and sexuality (BzGA)
- Ripe earlier and earlier - the trend towards earlier sexual maturity continues unabated in Germany (May 2006)
- Development in adolescence, exercise in educational psychology
literature
- EJ Haeberle: Human sexuality. De Gruyter, Berlin / New York 1983, ISBN 3-11-008753-7 .
- Lois Jovanovic, Genell J. Subak-Sharpe: Hormones. The medical manual for women. (Original edition: Hormones. The Woman's Answerbook. Atheneum, New York 1987) From the American by Margaret Auer, Kabel, Hamburg 1989, ISBN 3-8225-0100-X , pp. 13 f., 63 ff., 72 ff., 79 ff., 263 f. and 384 f.
- WD Keidel: Brief textbook of physiology. 2nd edition, Thieme, Stuttgart 1970.
- Laura E. Berk: Developmental Psychology (= Psychology: Developmental Psychology ). 3rd updated edition, Pearson Studium, Munich / Boston [ua] 2005, ISBN 3-8273-7110-4 .
- Jürgen Brämswig, Angelika Dübbers: Disorders of puberty development . (Disorders of Pubertal Development.) In: Deutsches Ärzteblatt . Volume 106, number 17, April 24, 2009, pp. 295-304, doi: 10.3238 / arztebl.2009.0295 .
- Willem Heuves: puberty. Developments and problems. Help for adults. Brandes & Apsel, Frankfurt a. M. 2010, ISBN 978-3-86099-634-8 .
- Jesper Juul : puberty. When education is no longer possible. Left through stormy times. Kösel, Munich 2010, ISBN 978-3-466-30871-2 .
- Angela Kling, Eckhard Spethmann: Puberty. The guide for parents. With 10 golden rules through all stages of puberty. Humboldt, Hannover 2010, ISBN 978-3-86910-613-7 .
- Reinhard Winter : Boys & Puberty. Stay in relationship when things change. Beltz, Weinheim / Basel 2020, ISBN 978-3-407-86642-4 .
Individual evidence
- ↑ Allan Herbison, Jenny Clarkson: Estrogen and kisspeptin regulation of GnRH neurons at puberty . In: Endocrine Abstracts. 2008, No. 16, p. 29.3.
- ↑ Michael R. Bieber: Infantile Sexuality. In: Fedwa Malti-Douglas (Ed.): Encyclopedia of Sex and Gender Vol. 2 (= Macmillan social science library ). Macmillan Reference USA, Detroit 2007, ISBN 0-02-865960-0 , p. 765.
- ↑ Sabine Heger: Neuroendocrine regulation of GnRH neuron function. Lecture at: 51st Symposium of the German Society for Endocrinology (DGE), 7. –10. March 2007, Salzburg; Symposium III: Puberty Development and Reproduction. on March 8, 2007.
- ^ J. Griffin, J. Wilson: Disorders of the testes and the male reproductive tract. In: P. Reed Larson, Henry Kronenberg, Shlomo Melmed, Kenneth S. Polonsky (Eds.): Williams Textbook of Endocrinology. 10th edition, Saunders, Philadelphia 2003, pp. 709-769.
- ↑ a b c W. D. Keidel: Brief textbook of physiology. Stuttgart 1970, p. 205.
- ↑ a b c d W. D. Keidel: Brief textbook of physiology. Stuttgart 1970, p. 206.
- ↑ Humboldt University Berlin, Magnus Hirschfeld Archive for Sexual Science: Growing Up Sexually, The Sexual Curriculum (Oct., 2002), Section 16: Prespermarchic Ejaculation? On "Prostatarche" (Childhood Orgasm) ( Memento from May 12, 2013 in the Internet Archive )
- ↑ masturbation . Lifeline; accessed on December 25, 2019.
- ↑ a b A Young Man's Guide to Masturbation (PDF) HealthyStrokes.com; accessed on August 27, 2019.
- ^ Norbert Kluge - University of Koblenz Landau: Contributions to sex science and sex education. From: Ripe earlier and earlier . In: Bild der Wissenschaft from May 26, 2006.
- ^ Research Center Landau University for Sexology and Sex Education, Landau University, Norbert Kluge, Maria Sonnenmoser, Publications, July 2001
- ↑ Werner Stangl: Physical and sexual development in adolescence . From: Werner Stangl's worksheets.
- ↑ Rainer Silbereisen u. a. (Ed.): Developmental Psychology of Adolescence (= Encyclopedia of Psychology. Subject area C: Theory and Research. Series V: Developmental Psychology. Volume 5). Hogrefe, Göttingen et al. 2008, ISBN 978-3-8017-0592-3 , Part 1, Chapter 4: Psychosomatic aspects of physical changes. / see also chapter 2.4. Development of secondary gender characteristics. ( limited book view on Google books )
- ↑ C. Thoeger Nielsen et al .: Onset of the Release Spermatozia (Supermarche) in Boys in Relation to Age, Testicular Groth, Pubic Hair, and Height. In: JCEM - The Journal of Clinical Endocrinology & Metabolism. from July 1, 2013, doi: 10.1210 / jcem-62-3-532 quote: "In particular, spermarche may occur when little or no hair has developed, and testes have grown only slightly."
- ↑ COPENHAGEN Puberty Study → Mikkel G. Mieritz1, Lars Lau Rakêt, Casper P. Hage u. a .: A longitudinal study of growth, sex steroids and insulin-like growth factor I in boys with physiological gynecomastia. In: The Journal of Clinical Endocrinology & Metabolism. (J Clin Endocrinol Metab.) Published online August 19, 2015, doi: 10.1210 / jc.2015-2836 ( full text as PDF file ).
- ↑ An involuntary ejaculation (pollution) does not necessarily have to occur even with healthy development, see: Pollution #Zeitpunkt
- ↑ Christian De Geyter, S. Steimann: Menarche and disorders in the menstrual cycle. University Hospital Basel, Women's Clinic, ( PDF file ( Memento from March 14, 2014 in the Internet Archive )).
- ↑ Gerd Mietzel: Ways in Developmental Psychology. Childhood and youth. 4th, completely revised edition, Beltz Psychologie Verlag Union, Weinheim 2002, ISBN 3-621-27477-4 , p. 354: first menstrual period. ( limited preview in Google Book search).
- ↑ WD Keidel: Brief textbook of physiology. Stuttgart 1970, p. 208.
- ↑ Hans-Heinrich Thiemann, Inna Nitz, Andreas Schmeling et al. (Ed.): X-ray atlas of the normal hand in childhood. 3rd revised and expanded edition, Thieme, Stuttgart 2006, ISBN 3-13-766603-1 , Section 9: General findings, menarche. limited preview in Google Book search.
- ^ S. Ojeda et al .: The systems biology of puberty-searching for hypothalamic gene networks . In: Endocrine Abstracts. 2008, No. 16, p. 29.1
- ↑ Ora Hirsch Pescovitz, Emily C. Walvoord (Ed.): When puberty is precocious: scientific and clinical aspects. In: Contemporary Endocrinology. Humana Press, Totowa (NJ) 2007, ISBN 978-1-58829-742-6 .
- ↑ Nicolas de Roux: Human genetics of pubertal onset . In: Endocrine Abstracts. 2008, No. 16, p. 29. 4
- ^ BJ Ellis, J. Garber: Psychosocial antecedents of variation in girls' pubertal timing: maternal depression, stepfather presence, and marital and family stress. In: Child development. (Child Dev) March-April 2000, Vol. 71, No. 2, pp. 485-501, PMID 10834479 .
- ↑ Bruce J. Ellis, S. McFadyen-Ketchum, KA Dodge, GS Pettit, JE Bates: Quality of early family relationships and individual differences in the timing of pubertal maturation in girls: a longitudinal test of an evolutionary model. In: . (J Pers Soc Psychol) August 1999, Vol. 77, No. 2, pp. 387-401, PMID 10474213
- ^ TE Moffitt, A. Caspi, J. Belsky, PA Silva: Childhood experience and the onset of menarche: a test of a sociobiological model. In: Child Development. (Child Dev) February 1992, Vol. 63, No. 1, pp. 47-58, PMID 1551329 .
- ^ The three previously cited studies by Laura E Berk: Developmental Psychology. Munich / Boston [ua] 2005, Section 11.2 Puberty: the physical transition to adulthood. P. 490 ff. ( Limited preview in Google Book search)
- ↑ Lois Jovanovic, Genell J. Subak-Sharpe: Hormones. The medical manual for women. (Original edition: Hormones. The Woman's Answerbook. Atheneum, New York 1987) From the American by Margaret Auer, Kabel, Hamburg 1989, ISBN 3-8225-0100-X , pp. 79 ff. And 385.
- ↑ Felix Alexander Schröter: Constitutional developmental delay and familial and idiopathic short stature on the test bench - distinguishable clinical diagnoses or existence of a continuum? Dissertation, Philipps-Universität Marburg, Marburg 2010, pp. 25–28 Section: 1.5.2 Constitutional developmental delay. ( PDF file ).
- ↑ a b Süddeutsche Zeitung. No. 253; Friday November 3, 2006; P. 12.