Sleep disorder
The term sleep disorder ( syn. Agrypnia , insomnia and hyposomnia ) denotes differently caused impairments of sleep . Causes can be external factors (such as nocturnal noise , street lighting that is too bright ), behavioral factors (e.g. problematic sleep hygiene ) or biological factors.
The lack of restful sleep impairs performance in the short term and in the medium or long term can lead to worsening or recurrence of diseases. Sleep disorders are considered to be disease-related if they are the cause of physical or mental impairments and are also subjectively perceived as pathological by those affected. The opposite sleep behavior, sleep addiction (technical term hypersomnia) , can also be the result. In the German-speaking literature, however, this is mostly not grouped under the term sleep disorder .
A special form of sleep disorders are the parasomnia is: This is an unusual behavior during sleep (with the same disorder), the person concerned, however, do not wake up. Total insomnia that is not amenable to treatment (as occurs in fatal familial insomnia ) is fatal. However, this is an extremely rare form of prion disease (<1/1 million), which is less caused by the sleep disorder itself than by a generally reduced level of vigilance (= alertness) during the day and pronounced impairment of mental abilities, even when awake that goes far beyond the symptoms associated with the otherwise very common problems falling and staying asleep. In contrast to non-organic insomnia, which is associated with an inability to fall asleep during the day, fatal familial insomnia is primarily characterized by an increased permanent tendency to fall asleep / sleepiness / somnolence (in contrast to the inability to fall asleep / doze off during the day in most insomnia patients ) marked. Pathologically increased sleepiness during the day (e.g. assessable using the so-called Epworth sleepiness scale) is in most cases caused by a treatable biological disturbance of the quality of sleep. Above all, these include sleep-related breathing and movement disorders.
In order to differentiate between the individual sub-forms of sleep disorders, it is particularly necessary to carefully collect the patient's medical history and, of course, usually also to carry out further examinations, for example in the sleep laboratory . Treatment is essentially based on the causes. For example, if the sleep disorder is the result of an internal illness, therapy is paramount. However, if it is triggered by incorrect handling of sleep , the patient should be informed accordingly and - if necessary - behavioral therapy is indicated.
term
Definition of terms
Agrypnia traditionally describes insomnia in German-language literature. In the past, however, the term has been replaced more and more by the term insomnia (also known as insomnia), which is more common in Anglo-American literature and used synonymously . Both terms describe (and have also described in the past) not only the lack of sleep, but also disturbances in falling asleep and staying asleep, as a result of which those affected did not sleep well in the morning. Hyposomnia also stands for “too little” sleep in the sense of insomnia or “light insomnia”. In addition, the term insomnia is also used in the case of complete lack of sleep, for example in the case of fatal familial insomnia .
Dyssomnia is the generic term for disturbed sleep behavior. This includes both "too little" and "too much" sleep in terms of depth and duration. So the term includes the sleep disorder and the sleep addiction .
Hypersomnia describes sleep or bed addiction, in which the need for sleep of those affected is significantly longer than that of normal persons. The need for sleep can also occur during the day or in attacks ( catalepsy ) .
The idiopathic insomnia is also known as insomnia in childhood or lifelong known insomnia. A cause for this form of the disease is not known.
The pseudo , subjective or paradoxical insomnia refers to a subjectively experienced sleep disorder without objectively findings. A further designation for this can be found in the literature: misperception of the sleep state or the English term "sleep state misperception".
Insomnias due to mental illness are also referred to as psychiatric or, in the case of depression, as depressive insomnias.
Classification systems
| Classification according to ICD-10 | |
|---|---|
| F51 | inorganic sleep disorders |
| F51.0 | inorganic insomnia |
| F51.2 | Inorganic disturbance of the sleep-wake cycle |
| F51.3 | Sleepwalking (somnambulism) |
| F51.4 | Pavor nocturnus |
| F51.5 | Nightmares (anxiety dreams) |
| G47 | sleep disorders |
| G47.0 | Difficulty falling asleep and staying asleep |
| G47.2 | Disorders of the sleep-wake cycle |
| G47.3 | Sleep apnea |
| ICD-10 online (WHO version 2019) | |
There are different classifications with the aim of schematically depicting sleep disorders. This process is in flux; some of the divisions were short-lived or are used side by side. The use of the terms used in connection with sleep disorders is also not uniform. The corresponding guidelines of the AWMF are currently being revised.
For example, the following classification systems are available for classifying sleep disorders:
- ICD-10 ( International Classification of Disorders , WHO, 1993)
- DSM-5 ( Diagnostic and Statistical Manual of Mental Disorders , American Psychiatric Association)
- ICSD ( International Classification of Sleep Disorders , 1990), ISCD-R (1997), ICSD-2 (2005)
ICD-10
According to ICD-10, sleep disorders are classified under depending on the suspected cause (psychogenic versus organic)
- F51 non-organic sleep disorders (chapter Mental and behavioral disorders ) or
- G47 (organic) sleep disorders (chapter diseases of the nervous system ).
Inorganic dyssomnias are primarily psychogenic disorders of the duration, quality or timing of sleep due to emotional causes that are present to a considerable extent (at least three times a week for a period of at least one month), cause significant distress and / or interfere with the affect everyday functioning (daytime sleepiness):
- Inorganic insomnia (F51.0): The main characteristics are difficulty falling asleep and staying asleep, as well as poor sleep quality (unrefreshing sleep).
- Inorganic disorders of the sleep-wake rhythm (F51.2): the sleep-wake pattern deviates from the desired sleep-wake rhythm (which is determined by social requirements and shared by most of the people around the person concerned), consequently insomnia during the main sleep period and hypersomnia during the wake period.
Inorganic parasomnias are abnormal episodes that occur during sleep:
- Sleepwalking (F51.3): repeated episodes (two or more) in which people get out of bed while sleeping and walk for several minutes to an hour, usually during the first third of the night's sleep. During this episode, those affected usually have a blank, rigid facial expression, hardly react to other people and can only be woken up with great effort. After waking up, those affected do not remember the episode (amnesia), otherwise there is no impairment of mental activity or behavior after waking up (apart from a brief period of confusion or disorientation).
- Night terrors (Pavor nocturnus) (F51.4): repeated episodes (two or more) in which those affected (usually in the first third of their sleep) wake up from sleep with a cry of panic, accompanied by intense fear, body movements and vegetative overexcitation ( tachycardia , faster Breathing, sweating). Attempts by other people to influence the person affected during the episode are unsuccessful or result in disorientation and persevering movements. An episode lasts up to 10 minutes.
- Nightmares (F51.5.): Waking up from night sleep or afternoon sleep with detailed and vivid memories of violent anxiety dreams. These usually have threats to their own life, security or self-esteem as their content and cause considerable suffering in those affected. After waking up from the anxiety dream, those affected are quickly oriented and awake.
Organically induced sleep disorders are disorders of falling and staying asleep (G47.0), disorders of the sleep-wake rhythm (G47.2) and sleep apnea (G47.3).
DSM-IV
In contrast to the ICD-10, the DSM-IV does not classify sleep disorders according to psychogenic and organic cause, but according to whether the sleep disorder is primarily present or the result of another factor secondary , for example due to another mental illness, a medical disease factor or taking a substance.
Primary sleep disorders are divided into dyssomnias and parasomnias. Among the Dyssomnias include primary insomnia (difficulty sleeping), the breathable bonded sleep disorder (unless by another disorder or substance intake due) and the sleep disorder due to a malfunction of the circadian rhythm. One of the parasomnias include sleep disturbance with nightmares, the night terrors and sleep disorder with sleepwalking ( somnambulism ).
It is also divided into sleep disorders that occur in connection with another mental disorder: those that occur as a result of a medical illness and those that are associated with the use of a psychotropic substance such as alcohol, amphetamine, caffeine, cocaine, opiate or of drugs (substance-induced sleep disorder).
DSM-5
While older diagnostic systems attempt to differentiate between primary and secondary insomnia based on the cause, the DMS-5 is limited to a purely descriptive approach. It is assumed that medical and psychiatric disorders can be the cause and consequence of a sleep disorder, which results in unreliable criteria in individual cases.
The DSM-5 defines insomnia as the unsatisfactory amount or quality of sleep:
- Difficulty falling asleep and / or
- Difficulty staying asleep and / or
- awakening prematurely without being able to go back to sleep
The sleep disorder has a disease value if it leads to significant malaise or impairment of coping with the day, e.g. B. through (at least one criterion):
- Exhaustion, lack of energy
- Drowsiness during the day
- decreasing attention, concentration, retentiveness
- occupational or educational impairment
- deteriorated communication or social behavior
- decreased caring or family activity
The sleep disorder has disease value if it:
- occurs at least three nights a week and
- exists for at least three months and
- there would be enough time to sleep
ICSD-2
According to the international classification of sleep disorders (ICSD-2) from 2005, sleep disorders can be divided into 8 groups. These include insomnias (with various causes), sleep-related breathing disorders (e.g. sleep apnea), circadian sleep-wake rhythm disorders ( as in shift work or jet lag ), parasomnias (e.g. sleepwalking, pavor nocturnus, nightmares), sleep-related movement disorders ( e.g. restless legs syndrome , bruxism), isolated symptoms, apparently normal variants and unexplained problems (e.g. snoring, speaking while sleeping) and other sleep disorders (e.g. environmental sleep disorder, noise). As an eighth group, the ICSD-2 also lists insomnia (hypersomnia) of central origin, not caused by circadian rhythm disturbances, sleep-related breathing disorders or other causes of disturbance in sleep behavior.
Apparitions
Clinical manifestations

The main symptom of the sleep disorder is the lack of restfulness in sleep. Delayed falling asleep, disturbed sleeping through the night and waking up too early are subsumed under this term. In the case of uncomfortable sleep, more or less intense sleepiness can occur during the day, in which wakefulness and the ability to remain alert ( vigilance ) are reduced. In addition, those affected can be exposed to an urge to fall asleep that is not always equally pronounced during the day. Other typical symptoms are irritability, restlessness, anxiety and other symptoms generally associated with fatigue , from a decline in performance to a change in personality. In severe cases, these symptoms in particular also impair the patient's social and professional situation.
The symptoms must appear on three days of a week for at least one month in order to be able to assign a disease value to them. If sleep is not restful, performance and wellbeing are impaired during the day and are described as difficult . Specifically, a healthy person should fall asleep at least 30 minutes after going to bed, be awake no earlier than 30 minutes after falling asleep (for older people up to 2 hours) and not wake up before 5:00 a.m. (without being able to fall asleep again).
Clinically, idiopathic , learned and sometimes pseudo- insomnia are very similar , which is why the two are often difficult to distinguish .
An unsolved problem is the discrepancy between the subjective perception of sleep quality and the objective results of polysomnography (PSG). In contrast to healthy sleepers, people with sleep disorders feel the wake-up phases longer than the PSG measurement showed. This led to the concept of paradoxical imsomnia. More detailed analyzes showed that people with insomnia perceived awakening from REM sleep (mostly associated with dreams) as a long waking period, but not waking up from an N2 sleep phase.
Typical for breathing disorders during sleep (sleep apnea syndrome) are also nocturnal cardiac arrhythmias , high blood pressure , obesity , loud and irregular snoring with pauses in breathing, restless sleep as well as impairments of libido and potency .
In pseudo-insomnia , the clinical findings, such as decreased performance, do not correlate with the sleep disturbance experienced by the patient. However, those affected increasingly suffer from anxiety, especially for their own health and depression. They also have an increased risk of misusing drugs or other substances.
The Schenck syndrome , which almost only occurs in men, harbors a considerable potential risk. If, for example, the bed partner is mistaken for an attacker, he can be injured and, statistically speaking, in about two thirds of the cases there is danger to others, in about one third of the cases to self-endangerment - in 7% there are even broken bones .
Disturbances of deep sleep (they are recognized by a lack of delta waves in the electroencephalogram ) are considered to be the cause of high blood pressure, especially in older men.
In addition, lack of sleep is a risk factor for the development of overweight in adults and children ( see: Obesity # sleep habits ).
Consequences of lack of sleep
There are many studies on the psychological and physical effects of lack of sleep. In a major study by the American Cancer Society , over a million participants were asked only about their average length of sleep. It showed that participants who slept less than 6 hours and more than 9 hours a night had a higher mortality rate than expected for their age. Other studies have been able to document the psychological and physical consequences of lack of sleep more precisely: drowsiness, lack of concentration and attention, irritation, anxiety, depression, mood swings, lack of self-esteem, impulsiveness and impaired social relationships. Well-studied physical consequences of lack of sleep include obesity, impaired glucose tolerance, and higher levels of diabetes, high blood pressure, heart attack, and stroke.
distribution
Most people's expectation of a good, restful sleep is simple: They want to fall asleep quickly, sleep well and wake up in the morning “full of vigor”. More or less pronounced sleep disorders are a common phenomenon that is subjectively perceived and assessed by the patient. Even those who do not wake up well rested every morning can perceive this as a sleep disorder in some cases. The frequency of occurrence in the population ultimately depends on how one defines sleep disorder . It ranges from just under 4% to around 35%. The question of the point in time from which a disturbed sleep can be described as a pathological sleep disorder from a medical point of view cannot therefore be answered universally. In practice, however, it can be assumed that around 20 to 30% of all people in the western industrialized countries have more or less pronounced sleep disorders. In around 15% there is also tiredness during the day and a general limitation of performance, so that treatment is indicated here . About 2% of all adolescents and young adults show notable sleep disorders due to poor sleeping habits alone . Objective disturbances of the sleep-wake rhythm are rare. A too late point in time for falling asleep, the so-called delayed sleep phase syndrome , is found in around 0.1% of the population, and too early (advanced sleep phase syndrome) in around 1%.
Typically, older people wake up several times during the night and have a lighter sleep overall (lower wake-up threshold ). However, these changes alone are not perceived as pathological by the vast majority of those affected . At the same time, existing impairments to health as well as the influences of the environment and social situation are considered to be essential influencing factors. Abnormalities during sleep (parasomnias) occur more frequently in childhood. A parasomnia that typically only occurs after the age of 60 (almost 90%) is the relatively rare (0.5% of the population) Schenk syndrome in men (almost 90%) . 100% of all people experience a nightmare at some point , around 5% of all adults develop a significant level of psychological distress due to nightmares . Around 1 to 4% suffer from sleepwalking , sleep disorders from eating or drinking at night, or night terrors . About every third sleep disorder, based on the estimated 3% of the total population, is caused by a psychiatric disease , for example depression .
The acute sleep disorder triggered by stress for a short time affects an estimated 20% of all people annually and can occur in all age groups, but preferably in older people and women. The psychophysiological (learned) sleep disorder affects about 1–2% of the population. The so-called pseudo-insomnia , in which those affected only have the feeling that they are sleeping poorly, is also quite rare (around 5% of all sleep disorders), but this cannot be objectified.
The idiopathic or lifelong insomnia with no known cause affects less than 1% of all children and young adults. Congenital fatal familial insomnia affects less than 1 in 1 million people.
Sleep disorders in children
Overview
Basically, children can experience essentially the same types of sleep disorders as adults. However, in this age group, parasomnias make up a larger proportion. This also includes apnea for premature babies , a disease that is attributed to the immaturity of the respiratory center in the brain stem. Although it mainly affects underweight premature babies (occurs in around 85% of all under 1000 g), it also plays a role in everyday life. It can be assumed that around 2% of all children born healthy and timely at least once in the first six months of life experience an episode of at least 30 seconds of respiratory arrest and a drop in heart rate of at least 20 seconds to below 60 beats per minute. Other parasomnias typical of childhood are obstructive sleep apnea syndrome and primary alveolar hypoventilation syndrome . Another phenomenon that only occurs in children is benign sleep myoclonus .
Sleepwalking and Pavor nocturnus
Owing to its frequent occurrence in children, sleep or night walking, which also belongs to the group of parasomnias, occupies a prominent position . Almost a third of all children between the ages of 4 and 6 and around 17% of all children up to puberty are affected. The child can sit up, look around, speak, call, or write, and in some cases even hop out of bed and run around. Since it is still deeply asleep, it is difficult to wake it up, then reacts aggressively in a disorderly manner and no longer remembers the incident. Many children (over 17%) are above the age of 11 from the as sleeping or night terrors known night terrors affected. This disturbance, which usually only lasts a few minutes, cannot be strictly differentiated from sleepwalking in all cases and is impressive because of the partial awakening from deep sleep that typically begins with a scream. It can also happen that the children jump out of bed. Characteristic of the night terror is an intense fear experienced by the child, which is accompanied by an activation of the autonomic nervous system with an accelerated heartbeat and breathing as well as reddening of the skin. In both forms of sleep disorder, factors such as lack of sleep , stress and fever are triggers. Both occur in families and mostly lose themselves in adulthood.
Problems falling and staying asleep
In the case of behavior-dependent insomnia in childhood (in technical jargon: protodyssomnia ), difficulty falling asleep and staying asleep are the main symptoms. A distinction must be made between two main groups. For example, the sleep onset association type (translated as “organized falling asleep”) needs certain objects and rituals in order to find sleep. With the limit-setting type (translated as “the type to whom one has to set educational limits”), an excessively generous upbringing leads to a refusal of the child, which ultimately also culminates in sleep disorders. In the specialist and advisory literature today, two doctrines dominate with regard to behavior-dependent insomnias: Some research-oriented authors, including e.g. B. Richard Ferber , attribute the insomnia of many children to their parenting inability to calm themselves down , and recommend that parents of such children gently but consistently train the ability to find sleep on their own to help the child can become independent of the often excessive parental micromanagement of child fatigue. Others, especially attachment parenting supporters like William Sears , consider insomnia to be fear-related and recommend co-sleeping .
(→ main articles sleep training , emotional disorders in childhood , excessive crying in infancy , attention deficit / hyperactivity disorder and disorder of social behavior )
The clinical symptoms of insomnia in children are very similar to those in adults. In addition, however, not only the child but also the parents suffer considerably. This can lead to negative, aggressively charged emotions towards the child, or even the parental partnership can be threatened.
Structural anatomical changes
In chronic insomnia, structural anatomical changes in the brain could be demonstrated by magnetic resonance imaging . Specifically, it is a reduction in the size of the hippocampus . Even if this does not apply to all forms of primary sleep disorder , this fact could be reproduced in two independent studies, at least for patients with increased nocturnal movement activity.
In the hereditary -related fatal familial insomnia , a place spongy change in the brain . Particularly noticeable are gliosis and the loss of nerve cells, especially in the area of the anterior and dorsomedial thalamic nuclei .
root cause
→ For the sleep architecture of normal people, see the corresponding section in the main article Sleep
Different causes leading to a sleep disorder mean that sleep is not restful. Changes of duration or course of the same are responsible for this. There are no concrete measured variables from when sleep is no longer restful. With regard to the duration of sleep, the German Society for Sleep Research and Sleep Medicine formulates in the AWMF guideline : “There is no binding time standard for the amount of sleep that is necessary to ensure relaxation. Most people know the amount of sleep from their own experience ”. There are also no specific, generally applicable norms for the course of sleep, for example when, how often and how long the individual sleep phases must be present so that a night's sleep is refreshing.
Sleep disorders for which no cause can be found are also referred to as primary or idiopathic . Secondly , those are named for which reasons are understandable that the duration and course of sleep is disturbed. A special form is the parasomnia .
In addition, extrinsic and intrinsic disorders can also be distinguished. The former include all causes that have their origin outside the patient's body such as alcohol, lack of sleep or environmental influences such as B. light pollution . It may also include radiation from cell phones . Impairments to the circadian sleep rhythm such as jet lag (time zone change) and the sleep phase syndrome (advanced or delayed) are usually included. Primary insomnia , sleep apnea syndrome and restless legs syndrome , for example, are referred to as intrinsic .
Another specialty is pseudo-insomnia. With this misperception of the state of sleep, night sleep in the sleep laboratory is completely regular and normal, but those affected have the feeling when they wake up that they have not slept or slept poorly.
Sleep disorders in depression and anxiety disorders
There is a scientifically ascertainable connection between sleep disorders - especially insomnia - and depression . Often, insomnia is found in patients diagnosed with clinical depression, which is the core symptom. Also, anxiety disorders may be accompanied by insomnia. Vice versa, people with insomnia are more likely to develop depressive disorders and anxiety disorders.
People with depression respond more slowly to treatment for their sleep disorder than other people with sleep disorders.
Disease emergence
→ For the "Hypotheses on the function of sleep" see also the section of the same name in the main article sleep
Ultimately, the decisive question is what is restful in one sleep and what prevents the other from being it. In any case, in order to be refreshing, it must be long enough and run as undisturbed as possible. In particular, the deep sleep phases must be available in sufficient quantities. In depressed patients, for example, they are significantly reduced. Those affected wake up more often at night than healthy people, REM sleep not only occurs more often and prematurely , but is also accompanied by particularly intense eye movements. 90% of all depressed people do not have a restful sleep. The fatal familial insomnia is also characterized by an increasing loss of K-complexes and delta waves . Her REM sleep can also be changed.
In the learned insomnia , a disturbed process of sleep (delayed falling asleep, more light sleep and less deep sleep), an increased release of cortisol and interleukin-6 , changes in anatomical structures in the brain and a normal or increased tendency to fall asleep during the day were found.
The idiopathic insomnia impressed - sometimes even in childhood - with an extended period of time to fall asleep, increased lying awake at night and consequently a reduction in the total sleep time. In addition, the phases of deep sleep (stages III and IV) are significantly reduced compared to light sleep (stages I and II).

The Schenk syndrome, which usually only occurs in advanced adulthood, is characterized by an intense living out of dream contents about attacks, defense and flight. An increased tone of the chin muscle , often accompanied by arm or leg movements, is found in the sleep laboratory . Nightmares typically lead to immediate awakening, accompanied by vegetative symptoms such as rapid heartbeat, accelerated breathing, and excessive sweating . Both abnormalities are mainly found in the second half of the night. Even with sleep disorders caused by eating or drinking at night , there is an increased wake-up from NREM sleep . Difficulty falling asleep or staying asleep also occurs with nocturnal heartburn as part of reflux disease . With restless legs syndrome , too , the constant involuntary movements disrupt the architecture of sleep.
In central sleep apnea in Cheyne-Stokes breathing , a subtype of sleep apnea syndrome , the breathing disorder occurs particularly during light sleep (stages I and II), but is noticeable in the deep sleep phases (stages III and IV) and in REM sleep diminished or completely absent. If the body is insufficiently supplied with oxygen, it often leads to awakening. Sleep becomes fragmented, with deep sleep phases becoming rarer and sleep losing its restfulness. Another sub-form, central sleep apnea with altitude-related periodic breathing (occurs above 4000 m), also shows a reduction in deep sleep in favor of light sleep. Similar results can also be found with other clinical pictures from the group of sleep apnea.
In the case of time differences, such as those that occur during shift work or air travel, the light-dark rhythm of the times of day, the circadian rhythm of numerous body functions and the "clock genes" innate in humans as diurnal beings influence the course of sleep (→ see also jetlag ) . Here too, deep sleep decreases in duration and severity. For the similar but chronic changes in sleep times , predisposition , long-term disturbances of the light-dark rhythm, poor sleep hygiene and the compensation of insufficient amounts of sleep on previous days are discussed.
In contrast to the other forms of sleep disorders, pseudo-insomnia lacks objectifiable findings in the sleep laboratory. Those affected still perceive their sleep as not restful.
Primary and Secondary Insomnia
The primary insomnia is defined by the fact that no concrete causes can be found.
The causes of secondary, i.e. acquired, insomnia are, for example, diseases or substances that have a correspondingly negative influence on the sleep phases. This is quite easy to understand in the case of diseases such as benign enlargement of the prostate gland or heart failure , which can lead to frequent nocturnal urination . As a result, the night sleep is interrupted several times and loses its relaxation.
This is similarly easy to understand in the case of short-term changes in the internal clock and thus in the sleep-wake rhythm, whereby - to put it colloquially - night sleep becomes afternoon nap and thus has a different sequence (for example, fewer deep sleep phases). Analogous changes can also be seen in shift work , when actual bedtime becomes working time. It is less common, but similar, for people who sleep normally, but whose internal clock slows down or slows down for unexplained reasons ( chronic sleep-wake rhythm disorder ), who can only fall asleep between one and six in the morning, for example and then have to sleep until noon to get enough sleep for recovery . Preferred for blind people who, due to the lack of vision, also lack the alternation of light and dark as a clock for the internal clock. But even with normally sighted people, the time to fall asleep can shift backwards by one to two hours a day (free-running rhythm). Each of the three forms of chronic sleep-wake rhythm disorders can be caused in the same way by diseases such as fibromyalgia , dementia , personality and obsessive-compulsive disorders, or by the use of medications such as haloperidol and fluvoxamine or drugs.
In the vast majority of patients, depression is associated with sleep disorders. A relative predominance of the cholinergic system and a deficient function of REM sleep are considered to be the cause .
Stress can seriously impair night sleep. The stress can be caused by disturbances in the social environment or at work (these include longer-term factors, but also short-term such as on-call or emergency doctor's service), but also through moving, changes in the environment when sleeping or the occurrence of serious physical illnesses and others Meaning even after previous excessive physical exertion (→ main article overtraining ). Because of the stressor, these patients often brood during the day and are affected by fear , sadness, and depression. The complaints usually end when the circumstances are of little or no importance for the respective person, which is why this form is also referred to as adaptation-related, transient, temporary or acute insomnia. This stress-related form is a common cause of learned, chronic, conditioned, primary or psychopathological insomnia, in which those affected internalize associations that impair sleep or wake up, i.e. they learn that restful sleep is no longer possible is possible. A simple example is a hospital doctor or emergency doctor who has internalized over decades, through weeks of on-call duty, that when an alarm is triggered, he suddenly and suddenly "works" optimally and without errors, and who thus cannot get a restful sleep even outside of his working hours. In the long term, this learned insomnia also leads to irritability, impairment of mood, performance, concentration, motivation and attention. Typically, these patients do not nap during the day either .
A "strong" or "very strong" Evocation of insomnia describes the German Society of Sleep Research and Sleep Medicine in the corresponding AWMF - Guideline for substances such as alcohol , caffeine , cocaine , amphetamines (including Ecstasy , Crystal ) and methylphenidate .
Further causes are in particular internal , neurological and psychiatric diseases such as varicose veins , hyperthyroidism , reflux disease , pain syndromes , psychoses , epilepsy , dementia and Parkinson's disease , which can impair sleep.
The fatal familial insomnia is genetic.
Parasomnia

These are phenomena that occur during sleep. These include, for example, nightmares , bed-wetting , sleepwalking , drowsiness , sleep paralysis , uncontrolled movements during sleep such as restless legs syndrome or paroxysmal dystonia , grinding teeth while sleeping and night terrors . These abnormalities do not affect the restfulness of sleep per se, but uncomfortable sleep is often associated with them. Symptoms can occur either during or outside of REM sleep, and independently of it. Sleepwalking, night terrors and drowsiness belong to the group of parasomnias as so-called wake -up disorders , as well as disorders of the transition from sleep to wakefulness such as speaking during sleep, leg cramps and twitching of the legs or rhythmic movements during sleep. The triggers for sleepwalking are external factors such as loud noises, as well as fever, pain and various drugs and alcohol. A hereditary change in chromosome 20 (locus 20q12-q13.12) could also be identified. Not only factors such as neuroticism , post-traumatic stress disorder and stress are considered to be the cause of nightmares , but also genetic changes that are currently unknown. Similar to sleepwalking, sleep disorders caused by eating or drinking at night , as occurs again and again during withdrawal or strict fasting, mean that those affected do not get enough sleep.
The type of symptom that occurs does not affect sleep in the same way in all cases. For example, sleep can be perceived as not restful due to a nightmare, because the person concerned woke up from an emotionally negative dream, is afraid that such an event will occur again or a breathing disorder occurred during the dream.
In Schenk's syndrome , around half of the cases have no apparent cause and the other half are caused by so-called synucleinopathies .
If a change in the tension of the muscles in the upper airways or a disturbance in the central respiratory regulation leads to impairments ( hypopneas ) or a more or less long respiratory arrest during sleep, this means that the body is temporarily supplied with too little oxygen becomes. It is not uncommon for there to be increased levels of carbon dioxide or a reduced pH value in the blood . If these impairments occur too often , there are also changes in the course of the sleep phases and sleep loses its restfulness. This is known as sleep apnea syndrome. The same changes can also occur in the context of an underlying disease (for example heart failure) and then count to the "secondary sleep disorders" (→ main article sleep apnea syndrome ).
therapy
Investigation methods
When patients seek medical advice and report uncomfortable sleep, problems falling asleep or staying asleep, early awakening or daytime sleepiness that make them feel significantly impaired, then a number of very different reasons come into consideration in addition to a sleep-related illness.
This can include false expectations of sleep as well as behaviors and living conditions that make sleep no longer restful. In such cases, education about proper behavior in terms of the rules of sleep hygiene can be helpful. It must also be clarified whether the ingestion of medication or other substances that impair sleep is the cause. In such cases, switching to other medications can be useful. When known to investigated triggering substances to a can weaning be necessary. If there are indications of a secondary sleep disorder caused by another existing illness, the causal illness must be treated accordingly.
If no causes for the symptoms can be identified by this point in time, a primary sleep disorder requiring treatment may be suspected and a corresponding specific approach with regard to diagnostics, advice and treatment is indicated.
Non-apparatus examination
At the beginning of the examination in sleep medicine there is also the relevant survey of the patient's medical history . This gives the sleep doctor clues about diseases that may be considered. The evaluation of one or more special questionnaires to be filled out by the patient provides further clarity. In some cases a sleep diary is used, which the patient must keep over a period of two weeks.
There is still a need for research into the survey of sleep-related medical histories and the questionnaires used in order to create generally recognized standards.
Apparative investigations
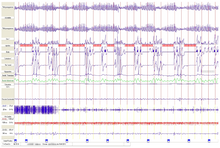
The basis of the apparatus-based examinations in the sleep laboratory is polysomnography , which can be used to determine the depth of sleep and disturbances in sleep. As part of this examination, for example, the electrical activities of the brain (EEG) and heart (long-term EKG), the oxygen and carbon dioxide content of the blood , the body temperature as well as respiratory flow and respiratory movement are recorded, and muscle tension as well as leg and eye movements are recorded. In addition, it is not only possible to document special features such as erections , blood pressure , snoring noises and gastric acid reflux , but also to create video recordings of the sleeper. With sleep apnea syndrome, it is also possible to determine the appropriate ventilation pressure (breathing masks are used for therapy). In addition to stationary facilities such as the sleep laboratory, portable aids known as polygraphy systems are available specifically for the detection of this clinical picture . This does not record the electrical activities (brain waves), but parameters such as long-term ECG, blood oxygen content, movements during sleep and the flow of breath in the mouth and nose. However, these polygraphy systems are afflicted with almost 20% false negative and up to more than 30% false positive results and are therefore unsuitable for definitively confirming or rejecting the diagnosis of “sleep-related breathing disorders”. Here, too, there is a need for research.
Numerous different test methods are available for recording performance that is restricted due to the lack of restful sleep. There are clearly recommended procedures for their use. These include the d2 test , the Frankfurt attention inventory and the Oxford Sleep Resistance Test . Stationary driving simulators can also be used. Here, too, there is still a need for research.
prevention
Some issues are of fundamental importance for prevention and treatment. The right amount of sleep needs to be mentioned, i.e. the length of rest time that a person needs for a restful sleep. In the industrialized countries it is an average of 7 hours, but it can vary individually. Therefore, every patient should find out for himself. Another important aspect is the correct behavior and handling of sleep, the so-called sleep hygiene . This also includes the correct and timely handling of the day-night rhythm .
Misconceptions about sleep
According to Volker Faust, these erroneous views are mistaken for norms:
- “8 hours of sleep as the norm.” Correct: 6 to 7 hours or individually as required.
- "Older people need more or less sleep than they used to." Correct: sleep becomes more prone to disruption.
- "Insomnia leads to mental illness." Correct: some mentally ill people can no longer sleep properly.
- "Exertion before going to bed makes you tired." Correct: Let the day end.
- “Sleep in after a bad night.” Wrong: Get up and work normally.
- “Go to sleep earlier if you have trouble falling asleep.” Wrong: Only go to bed when you are tired.
- “Whoever wakes up at night should stay in bed.” Wrong: leave bed temporarily and relax.
- “Those who cannot sleep should take sleeping pills.” Wrong: There is a risk of addiction.
- "Full moon disturbs sleep." Correct: darken the light source.
Can you learn to get by with less sleep?
Normal eight-hour sleepers can maintain their long-term performance even with five to six hours of sleep. This requires a regular sleep-wake cycle. For most people, this does not result in long-term physical changes or damage. Such a shortened sleep can improve in quality. The person then sleeps more effectively, with a complete preservation of deep sleep and shortened lighter sleep stages and REM sleep. The process of falling asleep is faster.
treatment
Causal diseases are to be treated professionally. In the case of sleep apnea syndrome, the use of positive pressure ventilation may also be necessary. Various substances such as pharmaceuticals and drugs , but also stimulants such as alcohol, tobacco products or coffee can severely disrupt the regulation of sleeping and waking. For example, the epilepsy drug lamotrigine leads to sleep disorders more often than other drugs such as pregabalin or levetiracetam for the same clinical picture. Appropriate adjustment of lifestyle or the necessary medication administration are promising here.
Substances
In Germany, around 5% of all men and 12% of all women use sleeping pills to treat sleep disorders. Approved for this are primarily substances from the group of benzodiazepines , (non- benzodiazepine ) hypnotics such as the Z-drugs and chloral hydrate , opipramol , antihistamines and herbal medicines , which mostly contain valerian . Also, in some cases, antidepressants , which are known to cause drowsiness , or low- potency antipsychotics are used. It is recommended, in particular to keep side effects as low as possible and to prevent dependence, the so-called interval therapy: The patient may only take the drug on 2 or 3 days per week. Long-term intake, in particular, has not yet been adequately investigated. In addition, in some cases these substances aggravate sleep disorders over the long term. Particularly in the case of chronic sleep disorders without a recognizable organic cause, special emphasis should be placed on weighing the benefits and risks , and other measures such as optimizing sleep hygiene, for example using cognitive behavioral therapy , should be exhausted. For patients over 55 years with insomnia with no known cause is melatonin , which the Troubleshooting sleep-wake rhythm seems to have some effect, are available. The current study situation indicates that valerian also has a certain sleep-promoting effect. There is no high-quality scientific evidence for the use of chloral hydrate, opipramol and antihistamines, and therefore no evidence-based recommendation .
Behavioral Therapy Techniques
In behavioral therapy, the following techniques can be used to treat sleep disorders:
- Rules of sleep hygiene,
- guide the structuring of the sleep-wake rhythm (stimulus control, sleep restriction)
- Reduction of nocturnal brooding through cognitive techniques.
Masturbating is also recommended to make falling asleep easier .
Meditation: For primary insomnia, it may be worth trying meditation. The deep relaxation technique has been shown to increase sleep time, improve sleep quality, and make it easier to fall asleep (and stay). These are some important facts about the practice that can help you overcome the hesitation in trying it out. Meditation can be a great tool for those looking for a natural, drug-free way to treat insomnia. In fact, meditation has even been shown to help reduce the use of sleeping pills. The practice likely improves insomnia symptoms by reducing the levels of arousal in the brain. And there are no risks or side effects associated with trying meditation.
history
The beginnings of "quantitative" sleep research go back to 1862. At that time, Ernst Kohlschütter determined the depth of sleep and presented it graphically in relation to the duration of sleep. For his experiment he used acoustic stimuli of different strengths and recorded the intensity at which his subjects woke up (wake-up threshold). Another milestone in basic research in this area is the electroencephalography (EEG) developed by Hans Berger . The use of electromyography and electrooculography made it possible to divide sleep into stages as described in 1968 by Allan Rechtschaffen and Anthony Kales .
The first classification system for sleep disorders appeared in 1979 under the title Diagnostic Classification of Sleep and Arousal Disorders . They were divided into four groups: insomnia (difficulty falling asleep and staying asleep ), hypersomnia (excessive drowsiness), disorders of the sleep-wake rhythm and parasomnias (partial awakening and disorders of the sleep stages).
(→ For further cultural and historical aspects see main article sleep culture )
Urban myths
Even in old medical publications there is an occasional statement that insomnia heralds an impending illness. Research has not been able to prove such a connection since then. A study published in 2015 by the psychiatrist Aric Prather ( UCSF ) indicates that, conversely, insufficient sleep increases the susceptibility to colds.
literature
- Svenja Happe, BW Walther, H. Schulz (Ed.): Sleep medicine in practice. The international classification of sleep disorders in case reports . ecomed, Landsberg am Lech 2009, ISBN 978-3-609-16406-9 .
- Markus B. Specht, Elena Spaude, Alexandra Kaluza: Brief intervention in insomnia (KI): Instructions for the treatment of problems falling asleep and staying asleep . Kohlhammer Verlag, 2014, ISBN 978-3-17-024187-9 .
- Kai Spiegelhalder, Jutta Backhaus, Dieter Riemann: Sleep disorders . 2nd Edition. Hogrefe, Göttingen 2011. ISBN 978-3-8017-2345-3 .
- Jürgen Staedt, Dieter Riemann: Diagnosis and therapy of sleep disorders . Kohlhammer, Stuttgart 2007. ISBN 978-3-17-019467-0 .
- Boris A. Stuck: Practice of sleep medicine. Sleep disorders in adults and children, diagnostics, differential diagnostics and therapy . Springer, Heidelberg 2009. ISBN 978-3-540-88699-0 .
Web links
- S3 guideline for non-restful sleep / sleep disorders - insomnia in adults of the German Society for Sleep Research and Sleep Medicine. In: AWMF online (as of December 2017)
- S3 guideline for non-restful sleep / sleep disorders - sleep- related breathing disorders of the German Society for Sleep Research and Sleep Medicine. In: AWMF online (as of December 2016)
- S1 guidelines for non-organic sleep disorders (F51) of the German Society for Child and Adolescent Psychiatry, Psychosomatics and Psychotherapy (DGKJP). In: AWMF online (as of July 2018)
- S2k guideline for insomnia in neurological diseases of the German Society for Neurology eV (DGN). In: AWMF online (as of March 2020)
- German Society for Sleep Research and Sleep Medicine (DGSM)
Individual evidence
- ↑ a b M. M. Ohayon: Epidemiology of insomnia: what we know and what we still need to learn. In: Sleep Med Rev. 2002 Apr; 6 (2), pp. 97-111, PMID 12531146
- ^ A b T. Roth et al.: Prevalence and perceived health associated with insomnia based on DSM-IV-TR; International Statistical Classification of Diseases and Related Health Problems, Tenth Revision; and Research Diagnostic Criteria / International Classification of Sleep Disorders, Second Edition criteria: results from the America Insomnia Survey. In: Biol Psychiatry. 2011 Mar 15; 69 (6), pp. 592-600. Epub 2010 Dec 31, PMID 21195389
- ^ A b D. Léger et al: Characteristics of insomnia in a primary care setting: EQUINOX survey of 5293 insomniacs from 10 countries. In: Sleep Med. 2010 Dec; 11 (10), pp. 987-998. Epub 2010 Nov 18, PMID 21093363
- ^ H. Frohnhofen: "Hygienic" sleep. In: The family doctor. 14/11, pp. 46-51.
- ↑ P. Reuter: The big Reuter: Springer universal dictionary medicine, pharmacology and dentistry. Birkhäuser, 2005, ISBN 3-540-25102-2 , pp. 446, 469 and 732, (online)
- ↑ P. Reuter: The big Reuter: Springer universal dictionary medicine, pharmacology and dentistry. Birkhäuser, 2005, ISBN 3-540-25102-2 , p. 721, (online)
- ↑ R. Klinke et al.: Physiology. Georg Thieme Verlag, 2010, ISBN 978-3-13-796006-5 , p. 862, (online)
- ^ S. Dressler: Elsevier's Medical Dictionary: English-German / German-English. Urban & Fischer-Verlag, 2007, S., ISBN 3-437-15200-9 , (online)
- ↑ CA Wunderlich: Handbook of Pathology and Therapy. Volume 2, Part 2, Verlag Ebner & Seubert, 1854, p. 1268 ff. (Online)
- ↑ UH Peters: Lexicon Psychiatry, Psychotherapy, Medical Psychology: with an English-German dictionary attached. Fischer-Verlag, 2007, pp. 14, 268 and 490, ISBN 3-437-15061-8 , (online)
- ↑ P. Reuter: The big Reuter: Springer universal dictionary medicine, pharmacology and dentistry. Birkhäuser, 2005, ISBN 3-540-25102-2 , p. 732, (online)
- ↑ P. Reuter: The big Reuter: Springer universal dictionary medicine, pharmacology and dentistry. Birkhäuser, 2005, ISBN 3-540-25102-2 , p. 774, (online)
- ↑ a b c d e f g h i j k l m n o p q r s t AWMF guideline for non-restful sleep / sleep disorders. (S3) pdf ( Memento from September 3, 2013 in the Internet Archive )
- ↑ UH Peters: Lexicon Psychiatry, Psychotherapy, Medical Psychology: with an English-German dictionary attached. Fischer-Verlag, 2007, pp. 74, 268 and 490, ISBN 3-437-15061-8 , (online)
- ↑ AWMF-online: Guideline detail view - register number 063 - 001. (online) ; last viewed on September 13, 2011.
- ↑ John W Winkelman: Insomnia Disorder . In: New England Journal of Medicine . tape 373 , no. 15 , October 8, 2015, ISSN 0028-4793 , p. 1437-1444 , doi : 10.1056 / NEJMcp1412740 ( nejm.org [accessed November 10, 2019]).
- ↑ Sleep Medicine Center of the Technical University of Munich: Classification of sleep disorders. Retrieved February 3, 2011 .
- ↑ Dieter Riemann, Chiara Baglioni, Claudio Bassetti, Bjørn Bjorvatn, Leja Dolenc Groselj: European guideline for the diagnosis and treatment of insomnia . In: Journal of Sleep Research . tape 26 , no. 6 , December 2017, p. 675-700 , doi : 10.1111 / jsr.12594 ( wiley.com [accessed November 10, 2019]).
- ↑ Bernd Feige, Svetoslava Nanovska, Chiara Baglioni, Benedict Bier, Laura Cabrera: Insomnia — perchance a dream? Results from a NREM / REM sleep awakening study in good sleepers and patients with insomnia . In: Sleep . tape 41 , no. 5 , May 1, 2018, ISSN 0161-8105 , doi : 10.1093 / sleep / zsy032 ( oup.com [accessed November 10, 2019]).
- ↑ a b M. M. Fung: inter alia: Decreased Slow Wave Sleep Increases Risk of Developing Hypertension in Elderly Men. In: Hypertension. 2011 Aug 29, pdf , PMID 21876072 ; quoted from aerzteblatt.de: Sleep disorders as a risk of hypertension , (online)
- ↑ HR Colten, BM Altevogt: Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. In: The National Academies Collection: Reports funded by National Institutes of Health. National Academies Press (US), Washington (DC) 2006, PMID 20669438 (English).
- ^ Rosalind D. Cartwright: The Twenty-four Hour Mind . The Role of Sleep and Dreaming in Our Emotional Lives. Ed .: Oxford University Press. 2012, ISBN 978-0-19-989628-8 (English).
- ↑ K. Tepperwein and others: How to give your best: A holistic mental training in 7 levels. MI Wirtschaftsbuch, 2006, ISBN 3-636-07178-5 , p. 86. (online)
- ↑ a b U. Schäfer et al .: Sleep well - fit during the day: A dream? ABW Wissenschaftsverlag, 2004, ISBN 3-936072-25-6 , p. 49, (online)
- ↑ a b c B. Stuck among others: Practice of sleep medicine: sleep disorders in adults and children. Diagnostics, differential diagnostics and therapy. Springer, 2009, ISBN 978-3-540-88699-0 , pp. 201 ff. (Online)
- ↑ a b c U. Schäfer et al: Sleep well - fit during the day: A dream? ABW Wissenschaftsverlag, 2004, ISBN 3-936072-25-6 , pp. 85 ff., (Online)
- ↑ a b c orphanet: Fatal familial insomnia. (on-line)
- ↑ a b D. Riemann et al. a: Chronic Insomnia and MRI-Measured Hippocampal Volumes: A Pilot Study. In: Sleep. 2007 August 1; 30 (8), pp. 955-658, PMID 1978381
- ↑ JW Winkelman et al .: Lack of hippocampal volume differences in primary insomnia and good sleeper controls: an MRI volumetric study at 3 Tesla. In: Sleep Med. 2010 Jun; 11 (6), pp. 576-582. Epub 2010 May 13, PMID 20466585
- ↑ Study: Cell phone radiation causes sleep disorders. In: Dtsch Arztebl. 2008; 105 (9), p. 15. (online)
- ↑ a b c H.-W. Delank et al.: Neurology. Georg Thieme Verlag, 2006, ISBN 3-13-129771-9 , p. 345 f., (Online)
- ↑ a b c d e B. Stuck among others: Practice of sleep medicine. Springer, 2009, ISBN 978-3-540-88699-0 , p. 2 ff., (Online)
- ↑ Buysse: Sleep and Depression. In: sleepfoundation.org. 2001, accessed September 20, 2019 .
- ↑ H. Koop: Sleep disorders due to nocturnal reflux. In: Dtsch Arztebl. 2003; 100 (47), pp. A-3093 / B-2570 / C-2400, (online)
- ↑ FATAL FAMILIAL INSOMNIA; FFI .. In: Online Mendelian Inheritance in Man . (English)
- ↑ PARASOMNIA, SLEEPWALKING TYPE; PSMNSW .. In: Online Mendelian Inheritance in Man . (English)
- ↑ Volker Faust : Liebenauer brochures mental health. Psychiatric and neurological information offered by the Liebenau Foundation. With the collaboration of Walter Fröscher and Günter Hole and the Psychosocial Health Working Group. Special issue Volume 5: Sleep disorders , (non-drug sleep aids, wrong views, hypersomnias, parasomnias), Liebenau in winter 2013/2014, pp. 42–46.
- ↑ Tillmann / Paterok: Successfully training sleep .
- ↑ M. Sonnenmoser: Sleep disorders: cognitive behavioral therapy as the means of first choice. In: Deutsches Ärzteblatt. Edition March 2011, p. 128. (online)
- ↑ Jürgen Staedt, Dieter Riemann: Diagnostics and therapy of sleep disorders . Kohlhammer, Stuttgart 2007, ISBN 978-3-17-019467-0 , pp. 127 ( limited preview in Google Book search).
- ↑ Lauren Streicher: Sex Rx: Hormones, Health, and Your Best Sex Ever [Sex Rx: Hormones, Health, and the Best Sex of Your Life]
- ^ How Meditation Can Treat Insomnia. In: sleepfoundation.org. Retrieved September 20, 2019 .
- ↑ E. Kohlschütter: Measurement of the firmness of sleep . In: Journal for rational medicine . Third row, no. 17 , 1863, p. 209-253 . , (online) (PDF; 5.9 MB), accessed on January 29, 2013.
- ^ Sleep Disorders Classification Committee, Howard P. Roffwarg: Diagnostic classification of sleep and arousal disorders . In: Sleep . tape 02 , no. 01 , 1979, p. 1-137 , PMID 531417 (en).
- ↑ Paul Hochmayer: Dissertatio inauguralis medico-chirurgica sistens semiologiam generalem . Vienna 1840, p. 23 ( limited preview in Google Book search).
- ^ Aric A. Prather et al .: Behaviorally Assessed Sleep and Susceptibility to the Common Cold . In: Sleep . tape 38 , no. 9 , September 1, 2015, p. 1353-1359 , doi : 10.5665 / sleep.4968 (English).
- ↑ Lisa Marie Potter, Nicholas Weiler: Short Sleepers Are Four Times More Likely to Catch a Cold. University of California San Francisco, August 31, 2015, accessed September 15, 2015 .