pancreas
The pancreas - technically also the pancreas ( Greek : πάγκρεας, pánkreas , πᾶν pân for "everything", κρέας kréas for "meat") - is a glandular organ of vertebrates lying across the upper abdomen behind the stomach .
The digestive enzymes ("pancreatic juices ") it produces are released into the duodenum . It is therefore an exocrine gland ( exocrine "emitting to the outside"; in this case into the digestive tract). The pancreatic enzymes break down proteins , carbohydrates and fats in food in the intestine into a form that can be absorbed by the intestinal mucosa . In addition, hormones are produced in the pancreas that are transferred directly to the blood . It is thus also an endocrine gland ( endocrine "emitting inwards"). This endocrine part of the pancreas is the islets of Langerhans (a specialized group of endocrine cells), which are primarily responsible for the regulation of the carbohydrate metabolism via the blood sugar level (through the hormones insulin and glucagon ) as well as digestive processes and through the formation of somatostatin also jointly responsible for regulated growth processes.
Inflammation of the pancreas ( pancreatitis ) leads to self-digestion of the organ due to the released digestive enzymes. If the production of digestive enzymes declines ( exocrine pancreatic insufficiency ), the food can no longer be sufficiently digested. The most common disorder of the endocrine part is diabetes ( diabetes mellitus ).
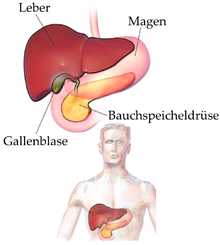
Human anatomy
Location and structure
The human pancreas is a wedge-shaped organ about 16-20 cm long, 3-4 cm wide and 1-2 cm thick. Their weight is between 40 and 120 g. The organ is divided into lobules, which also structure the surface in a characteristic way.
The pancreas is located in the retroperitoneal space , i.e. behind the peritoneum , between the stomach , duodenum , spleen , liver and the large blood vessels of the abdomen ( aorta and inferior vena cava ). It is hardly breathable, i. That is, in contrast to other organs of the abdominal cavity such as the liver, their position changes little when inhaling and exhaling.
Macroscopically (with the naked eye) one differentiates three sections of the pancreas: the pancreatic head (caput pancreatis) , the pancreatic body (corpus pancreatis) and the pancreatic tail (cauda pancreatis) . The head of the pancreas is encompassed by the duodenum and has a downwardly directed hooked process (uncinate process) . At the pancreatic notch (Incisura pancreatis) the head merges to the left into the body of the pancreas. The superior mesenteric artery and superior mesenteric vein run in this notch . The pancreas body crosses the spine horizontally at the level of the first to second lumbar vertebrae . There the organ bulges slightly inwards into the mesh bag , which is called the mesh cusp (tuber omentale) . Finally, the pancreatic body, which is triangular in cross-section, runs out into the tail of the pancreas without a clear border, which extends to the vascular pole of the spleen .
The approximately two millimeter wide excretory duct of the pancreas ( ductus pancreaticus , Wirsung duct ) opens together with the main bile duct ( ductus choledochus ) or near it into the duodenum. This opening represents a wart-shaped elevation ( papilla duodeni major or Father's papilla ). In some individuals there is a second, smaller duct, the ductus pancreaticus accessorius ( Santorini duct ), which then opens on the small duodenal wart ( papilla duodeni minor ) into the duodenum.
Feinbau
The pancreas is an exocrine and endocrine gland at the same time . As an exocrine gland, it produces digestive enzymes , and as an endocrine gland, it produces hormones (see also the Function section ).
The exocrine part consists of several thousand loosely joined lobules with a diameter of about three millimeters. Such a lobule contains several gland ducts ( acini ) surrounded by secretion-producing cells . The digestive enzymes formed by these gland cells are released in the form of an aqueous (serous) secretion without loss of cell components ( merocrine secretion ) and passed on via the acini and partly also stored. The acini are surrounded by a basement membrane that is supported by a fine network of reticular fibers . About three to five acini are interconnected to form a complex or "glandular tree" and lead to a common passage via so-called switching pieces . The cells of these contact pieces are called centroacinar cells . The execution aisles combine and ultimately become the main execution aisles. In the exocrine part of the pancreas, there are also cells between the acini that are known as pancreatic star cells . They play a role primarily in repair processes.

Fluorescence microscopy :
green - beta cells
red - alpha cells
blue - cell nuclei
The endocrine part is made up of the islets of Langerhans (Insulae pancreaticae) , which were discovered by Paul Langerhans in 1869 . These are clusters of endocrine epithelial cells that are predominantly found in the body and tail of the pancreas. They release the hormones they make directly into the blood. The islets of Langerhans make up one to two percent of the mass of the pancreas. Depending on the hormone produced, one differentiates:
- α cells produce glucagon (about 30% of islet cells)
- β cells produce insulin and amylin (about 60% of islet cells)
- δ cells produce somatostatin (about 5% of islet cells)
- PP cells produce pancreatic polypeptide (less than 5% of islet cells)
- ε cells produce ghrelin
Using immunohistochemical methods, the localization of the cell types within an islet of Langerhans can be determined, which does not reveal a specific pattern in humans.
The pancreas as a whole is surrounded by a thin capsule of connective tissue that sends septa (partition walls) inwards. These septa separate the individual glandular lobules from one another. In addition, the organ is traversed by a dense capillary network, which ensures a good blood supply and thus enables the secretion activity in the first place.
Blood supply and lymph drainage
The pancreas is supplied via three larger vessels: the upper pancreatic-duodenal artery ( Arteria pancreaticoduodenalis superior ) , the large pancreatic artery ( Arteria pancreatica magna ) and the lower pancreatic-duodenal artery ( arteria pancreaticoduodenalis inferior to the smaller arteria pancreaticoduodenalis ) connect ( anastomose ) with each other .
The venous blood from the body and tail of the pancreas is carried by small pancreatic veins (Venae pancreaticae) via the splenic vein ( Vena splenica ) into the portal vein (Vena portae) . The blood from the head of the pancreas passes through the pancreatic-duodenal vein (pancreaticoduodenal vein) into the upper mesenteric vein ( superior mesenteric vein ) and then also into the portal vein.
The lymph vessels of the pancreas run into the Nodi lymphoidei (Nll.) Pancreatici and the Nll. pancreaticoduodenales superiores et inferiores . These lie close to the pancreas and carry the lymph into the intestinal trunk .
Innervation
Like almost all internal organs, the pancreas is supplied by both parts of the autonomic nervous system ( sympathetic and parasympathetic ). The parasympathetic supply is provided by the vagus nerve . Alpha and beta cells are stimulated via the M3 receptor . Sympathetic fibers reach through the thoracic splanchnic nerves , the celiac ganglion , where the second sympathetic neuron are switched, which then moves into the pancreas. The secretion of the β- and δ-cells is lowered and that of the α-cells is increased via α2-adrenoceptors . The secretion of the β and δ cells is increased via β2 adrenoceptors .
Animal anatomy
Cells that produce pancreatic hormones and those that produce digestive enzymes have been found in a wide variety of invertebrates . However , they only appear as an independent organ in vertebrates . In the case of the black-bellied fruit fly , for example, insulin-like peptides are still formed in the brain , and glucagon -like peptides are formed in the corpora cardiaca (a neurohemal organ ). But there are also structural differences in vertebrates, which are caused by different ways of life and diet as well as metabolic peculiarities.
In the tunicates and lancetfish no pancreas has yet developed. There are only specialized cells in the intestinal epithelium that produce the corresponding hormones. In round mouths , the endocrine and exocrine parts are separated: while the cells that produce digestive enzymes are scattered in the intestinal mucosa, and in the case of hagfish also in the liver, the hormone-producing cells form a separate island organ at the mouth of the bile duct in the intestine. The island organ of the hagfish and lampreys consists of β cells and a few δ cells, whereas α cells are located in the intestinal mucosa. Bony fish have an exocrine pancreas, while the endocrine tissue is often grouped together in independent structures. These island organs, also known as Brockmann's bodies , arise from the dorsal pancreas and are located in the adjacent mesentery . In some species there is a single large Brockmann body (e.g. gobies ), in some there are several Brockmann bodies, in others additional scattered islet cell tissue. In bony fish, PP cells are usually not yet located in the islet organ. In some fish species, the exocrine pancreatic tissue is located in the liver ( hepatopancreas ). Cartilaginous fish have an endocrine-exocrine pancreas, with most representatives with all four main cell types (α, β, δ, PP), in the sea cats the δ cells remain in the intestine. Despite the presence of an islet organ, many α, δ and PP cells in cartilaginous fish also remain localized in the intestine.
In amphibians , reptiles , birds and mammals , the pancreas basically shows the same structure.
Tail amphibians have endocrine tissue that is either diffusely distributed or clustered in islets, and some species lack α-cells. The islet organ of the frog has all four main cell types and is similar to that of mammals, but there are differences in the cell proportions: α-, β- and PP-cells are present in about the same amount, plus some δ-cells. In clawed frogs , ghrelin-producing ε cells appear for the first time. There are also considerable differences in cell composition in reptiles. In crocodiles , β cells make up about half of the islet organ cells, while in lizards there are four to five times more glucagon-producing cells than insulin-producing cells. In the ornamental turtle , the islets of Langerhans only consist of α and β cells, while PP and δ cells are scattered in the exocrine part. So far, ε-cells have only been found in a few species such as the red-eared sliver of reptiles . In some snakes the islet cells form a sheath around the ducts of the exocrine part. PP cells have not yet been detected in the islet organ. In birds, the pancreas is made up of many lobules that lie between the two legs of the duodenum. In birds there are not only mixed islands but also islands in which almost exclusively α or β cells occur. The number of α-cells in birds seems to generally outweigh that of the other cell types. Ghrelin has been detected in domestic chickens; this has not been investigated in other species.
In mammals , the structure of the pancreas is basically similar, in the islets of Langerhans all five cell types are formed. In veterinary anatomy, the pancreas is macroscopically divided into a body (corpus pancreatis) , a right lobe adjacent to the duodenum ( lobus pancreatis dexter , "duodenal thigh") and a left lobe adjacent to the viscera of the stomach and reaching to the spleen ( lobe sinister , "Spleen thigh"). In horses and pigs, the body of the pancreas surrounds the portal vein in a ring shape (anulus pancreatis) . When Egyptian fruit bat , the islets of Langerhans almost nine percent make the organ mass, which is more than twice as much as in other mammals.
Due to its origin in a paired and an unpaired organ system (see section Development ), the pancreas has one to three ducts, depending on the species. The “additional passage” is the only one for pigs and cattle , while horses and dogs always have both, some birds (e.g. ducks ) have all three originally created passage ways.
development
In the embryo , the pancreas develops from the inner cotyledon ( endoderm ). Initially, two epithelial buds develop in the area of the duodenum, the front being formed in the abdominal suspension of the duodenum (mesoduodenum ventral) near the bile duct , the rear in the back mesentery (mesoduodenum dorsale) . The main shoots of these buds become the ducts through the formation of a cavity (canalization), their branches become the actual glandular tissue.
The posterior (dorsal) pancreatic anlage is the larger and forms the main part of the later pancreas. Its duct is the additional pancreatic duct ( ductus pancreaticus accessorius ) . The smaller abdominal (ventral) pancreas system is initially paired. In mammals, both ventral rungs unite during embryonic development and form the pancreatic duct ( ductus pancreaticus ) . In birds, however, both rungs of the ventral system remain separate for life. The uncinate process ("hooked process") and the lower part of the head of the pancreas arise from the ventral pancreas.
With the embryonic rotation of the stomach around its longitudinal axis, the ventral abutment moves over to the right into a position on the back. The original peritoneum coating merges with that of the left abdominal wall. The pancreas, which is initially located inside the body cavity, then moves to a position outside the peritoneum - in the so-called retroperitoneal space . With this rotation, the two cavity systems and thus both systems are also united. In humans, this takes place around the sixth to seventh week of pregnancy. The second turn of the stomach brings the pancreas into a lateral position.
The originally two main execution passages of both systems are only retained for some mammals (e.g. horses, dogs). In humans as well as sheep and cats, the (proximal) section of the duct of the dorsal system that opens directly into the intestinal tube is closed (obliterated) so that the pancreatic duct becomes the common duct for both systems. In pigs and cattle, on the other hand, only the accessory pancreatic duct - that is, that of the dorsal anus - remains .
The islets of Langerhans - i.e. the endocrine part of the pancreas - also arise from epithelial cones that extend from the rungs of the exocrine part. These "island cones" lose the connection to the duct system and are separated from the exocrine part by vascularized connective tissue. Activation of the transcription factor Neurogenin3 is necessary for the first step in the differentiation of the precursor cells for the later islet cells . The further differentiation is controlled by the transcription factor Rfx6 (Transcriptional regulatory factor X6) . In addition, a number of other transcription factors (NeuroD1, Pax4, Nkx2.2, Nkx6.1, Arx, MafA, Pax6, Isl1 and others) are involved in cell differentiation and organogenesis of the pancreas.
evolution
Comparative studies suggest that both the endocrine and exocrine portions of the pancreas are phylogenetically of endodermal-epithelial origin, although this question has not yet been conclusively clarified. In lancet fish , for example, cells within the midgut epithelium can be detected that form an insulin precursor molecule (protoproinsulin) and release it into the intestinal lumen together with other enzymes. After splitting in the lumen, it is absorbed from the intestine into the blood and develops an insulin-like effect. In addition, “mixed” cells can be found in some lower vertebrates, which perform both endo- and exocrine functions.
Probably even the insulin-producing β-cell is the starting point for the phylogenetic development of the pancreas as an organ. The island organ of the round-mouthed mouth consists almost entirely of β-cells, in sea cats there are α-cells, in sharks then PP-cells - there is a gradual expansion of the organ function. The expression of the transcription factors involved in the development of the pancreas also seems to confirm this theory of common phylogenetic origin.
function
Function as an exocrine gland
As an exocrine gland , the pancreas is a purely serous gland and the most important digestive gland . It produces up to two liters of secretion daily in humans and up to 35 liters in horses. The formation of digestive secretions (also known as pancreatic juice ) is stimulated by the smell and taste of the food and the chewing process via the vagus nerve . The expansion of the stomach wall (also mediated by the vagus nerve) and the hormones secretin , cholecystokinin and probably gastrin increase the formation and release of pancreatic juice. Cholecystokinin stimulates thereby together with the vagus nerve (via acetylcholine ) primarily the secretion of pancreatic enzymes from the acinar cells , while secretin the Gangepithelzellen of the pancreas to form a bicarbonate stimulates -rich secretion, of a Cl - / HCO 3 - - antiporter chloride from exchanges the secretion in the pancreatic duct with bicarbonate. A large part of the chloride used for this is transported via the CFTR channel into the lumen of the pancreatic duct, which plays a major role in the development of cystic fibrosis . The hormones somatostatin , glucagon , pancreatic polypeptide , peptide YY and the influence of the sympathetic system , on the other hand, inhibit the formation and release of pancreatic juice.
The pancreatic secretion contains the precursors of protein-splitting enzymes ( trypsinogen , chymotrypsinogen , procarboxypeptidases , proelastase ), the starch - splitting enzyme α-amylase , ribo- and deoxyribonucleases and enzymes that split fat ( lipases ). The protein-splitting enzymes are in an inactive form during production in the gland to prevent the organ from digesting itself. The trypsinogen is only through targeted cleavage by the enzyme enteropeptidase of the brush border converted duodenal intestinal mucosa in trypsin and thus effective. Trypsin in turn activates the other protein-splitting enzymes. The lipase becomes active only through the protein colipase . The latter also comes as a preliminary stage from the pancreas and is only activated by trypsin. With regard to the enzyme composition of the pancreatic juice, there are diet-related animal species differences. The pancreas in animals with low starch content in the diet, for example pure carnivores such as cats or herbivores such as horses and ruminants, hardly produces any starch-breaking amylase. In monogastric animals , the enzyme pattern of the pancreatic juice also changes after a few days, depending on the composition of the food.
The hydrogen carbonate ions (HCO 3 - ) produced in the epithelial cells of the pancreatic ducts increase the pH value of the pancreatic juice to 8. The alkaline pancreatic secretion neutralizes the intestinal contents acidified by the gastric juice and thus creates an optimal environment for the digestive enzymes.
Function as an endocrine gland
In addition to this exocrine gland function, the endocrine gland, the islets of Langerhans , releases hormones directly into the blood. Glucagon is synthesized in the α cells, insulin in the β cells, somatostatin in the δ cells, the pancreatic polypeptide in the PP cells and ghrelin in the ε cells .
The stimulus for insulin release is the rise in blood sugar . There is further stimulation via the parasympathetic nervous system and some intestinal hormones ( gastrin , secretin , GIP , cholecystokinin and GLP-1 ). The insulin lowers blood sugar to a physiological level by absorbing grape sugar (glucose) in the liver , skeletal muscles and adipose tissue . In addition, glucose storage is promoted and the formation of new glucose is inhibited. If the blood sugar drops sharply, glucagon is released from the α cells, which leads to the release of grape sugar from the liver and thus to an increase in blood sugar.
Somatostatin serves to inhibit the exocrine part and the α cells. In high concentrations, it also inhibits the β cells. The function of the pancreatic polypeptide has not yet been sufficiently clarified; it presumably inhibits the appetite.
In addition to the classic five hormones, the islet cells produce a large number of other peptides, such as cholecystokinin , calcitonin gene-related peptides , insulin-like growth factors , peptide YY , cocaine and amphetamine regulated transcript and thyreoliberin , and in frogs also secretin .
Diseases
Diseases of the exocrine part
An acute inflammation of the pancreas (pancreatitis) causes severe pain in the upper abdomen ("rubber belly"), nausea, vomiting, constipation and fever. The most common cause of acute pancreatitis in humans is gallstones ; for chronic pancreatitis it is alcohol abuse . A traumatic rupture of the pancreas can also trigger pancreatitis. In the case of acute pancreatitis or pancreatic rupture, the organ self-digestion due to released enzymes and thus a strong inflammatory reaction.
The insufficient secretion or release of pancreatic enzymes is called exocrine pancreatic insufficiency . It can be acquired through loss of pancreatic tissue in chronic pancreatitis or pancreatic cancer (see below), but it can also be congenital through genetic diseases such as cystic fibrosis . The exocrine pancreatic insufficiency leads to digestive problems with large-volume fatty stools and is treated by administering pancreatin or rizoenzymes with meals.
Pancreatic cysts and pseudocysts, blister-shaped formations in the pancreas, can arise as a developmental disorder, through trauma, inflammation or tumors. Pancreatic cysts often cause no symptoms. Pseudocysts do not have an epithelial lining and usually arise after pancreatitis as a result of tissue melting. They can be accompanied by signs of inflammation such as fever and are prone to abscess formation and other complications.
Pancreatic tumors affect the exocrine part in 98% of cases. The majority are malignant adenocarcinomas (ductal adenocarcinomas), which are feared because of their high mortality rate .
Some flukes parasitize the duct system of the pancreas. The pancreatic fluke (Eurytrema pancreaticum) occurs mainly in arthropods in East Asia and South America, but can also affect humans. The raccoon pancreatic gel (Eurytrema procyonis) is found in the United States of America and parasitizes in raccoons , and rarely in cats. Lyperosomum intermedium occurs only in the US southern states of Florida and Georgia and affects rice rats .
Diseases of the endocrine part

The most common disease of the endocrine part is diabetes (pancreopriver diabetes mellitus ). In diabetes mellitus, there is an absolute or relative insulin deficiency or a reduced effectiveness of the insulin. Diabetes is a mass disease that is widespread around the world and of considerable economic importance. About 380 million people (8.3% of the population) suffer from this disease, but only about five to ten percent of diabetes diseases are caused by an underfunction of the Langerhans Islands. Diabetes mellitus is also one of the most common endocrine diseases in domestic dogs and cats .
In the case of hereditary nesidioblastosis , the islet cell tissue is increased and the secretion of insulin is increased, which leads to severe hypoglycaemia even in infants .
Endocrine tumors only make up about two percent of pancreatic tumors . Here, tumors of the insulin-producing β cells ( insulinoma ) and tumors that produce gastrin ( Zollinger-Ellison syndrome ) predominate . An accumulation of endocrine pancreatic tumors occurs in Wermer syndrome .
Malformations
Various malformations can occur during the development of the organ .
If the pancreas is not or only incompletely developed, it is called pancreatic agenesis . While total pancreatic agenesis is associated with severe digestive disorders and diabetes in newborns, partial pancreatic agenesis usually remains asymptomatic, as the existing tissue has sufficient synthesis capacity.

The pancreas divisum ("divided pancreas") is based on a lack of fusion between the two organ systems. Here there is a tendency to blockage in the area of the excretory duct, since the pancreatic juice from the larger dorsal system drains through the smaller duct (ductus pancreaticus accessoryius) . In the rare pancreas bifidum ("split pancreas"), the main duct in the area of the tail of the pancreas is split open like a fish's tail.
The pancreas annulare ("ring-shaped pancreas") is a rare ring-shaped adhesion around the duodenum, which can lead to duodenal stenosis (narrowing of the duodenum). In the literature, a non-obliterated (sclerosed) left bud of the ventral appendix or a generally abnormal development of a two-part ventral pancreatic appendix is given as the cause . This appendix grows around the duodenum and merges with the dorsal appendix. Therapy is a duodenojejunostomy , a surgical connection of the duodenum with the jejunum (empty intestine) , or a short bridging of the narrowed area within the duodenum (duodenum-duodenum anastomosis).
Ectopic tissue of the pancreas (disrupted pancreatic tissue) can u. a. occur in the stomach, in the small intestine (especially in Meckel's diverticulum ) or in the liver.
In the context of rare syndromes , the pancreas can be involved, such as in Mitchell-Riley syndrome .
Investigation methods
The previous history and the physical examination results already indicate the presence of a pancreatic disease.
For the detection of pancreatitis , the laboratory determination of the pancreatic lipase in the blood has proven itself. Alternatively, the pancreatic amylase can be determined in the serum. However, it is not that specific and sensitive. The PLI test is mainly used in veterinary medicine . In human medicine, the secretin-pancreozymin test or the determination of the concentration of pancreatic elastase in the stool are used to detect exocrine pancreatic insufficiency ; in veterinary medicine, the TLI test in particular .
To assess the function of the endocrine part, blood and urine sugar , HbA1c , C-peptide , fructosamine and the remaining intrinsic secretion rate are determined. Autoimmune diseases of the pancreas can also be diagnosed by determining autoantibodies .
Imaging methods such as sonography , computed tomography , magnetic resonance tomography and a combined endoscopic-radiological method, the so-called endoscopic retrograde cholangiopancreatography , are used to detect tumors of the pancreas . In addition, the organ can be assessed directly by opening the abdominal cavity ( laparotomy ) and mirroring ( laparoscopy ). The Flexible Transgastric peritoneoscopy is a befindliches be considered experimental investigation procedures. Pancreatic pseudocysts, pancreatic stones or pancreatic calcifications can also best be recognized with the imaging methods mentioned. As a useful tumor marker has CA 19-9 proven.
Pancreas transplant
The combined pancreas and kidney transplant is the best therapy to date for carefully selected patients with insulin-dependent type I diabetes and dialysis-dependent or impending kidney failure . Organ mediation takes place centrally via Eurotransplant . There, the data of all patients are saved and available organs within Europe are mediated according to defined criteria. Since the first pancreas transplant in 1966, over 7,000 pancreases have been transplanted worldwide. Most of the operations, about two-thirds, took place in the US followed by Europe. Few transplants are performed anywhere else in the world. In Germany 150 to 200 pancreatic transplants are performed annually. The islet cell transplantation is currently considered still considered experimental therapy method.
use
Pig pancreases are obtained at slaughter and technically processed. As pancreatin , this enzyme mixture is used to treat exocrine hypofunction of the pancreas. Pancreatin must be consumed with meals. In addition, insulin for insulin therapy is obtained from the pancreas of cattle and pigs . The first insulin preparations made from bovine pancreas came on the market as early as 1923. Due to the possibility of producing recombinant insulin, however, insulin obtained from the organ no longer plays a role in the treatment of diabetes in humans.
In Asia in particular, the pancreas of pigs is also used as a food.
Research history
The pancreas was probably first dubbed by Herophilos of Chalcedon - also called the "father of anatomy" - around 300 BC. BC, although he did not designate it as such and many of his writings no longer exist. The term “pancreas” already existed before, Hippocrates already used the word, but it was probably common for lymph nodes . It is unclear whether the "glands in the network " mentioned by Hippocrates are the pancreas or the mesenteric lymph nodes . Around the same time as Herophilos, Eudemus of Alexandria is said to have mentioned a gland that releases a saliva-like secretion into the small intestine. Galenus refers to Herophilos' writings and the pancreas, but considered them to be a cushion of the vessels surrounding them. Due to Galenos' high reputation, this view was considered an irrefutable fact until the 17th century.
The first clear distinction between the pancreas and the lymph nodes of the abdominal cavity and the assignment of the term pancreas to this organ goes back to the doctor and anatomist Rufus of Ephesus , who developed the first anatomical nomenclature at the end of the first century . Nevertheless, in the middle of the 2nd millennium there was again some conceptual imprecision. Marked Frederik Ruysch (1638-1731) by Gaspare Aselli mesenteric described the early 17th century as "Pancreas Aselli" and Johann Conrad Brunner , the 1686 first described by him Brunner's glands as "Pancreas secundarium" ( "second pancreas"). The organ was hardly noticed in the Middle Ages. Jean François Fernel considered the pancreas to be the seat of melancholy , hypochondria and a refuge for recurring fevers.

Jacopo Berengario da Carpi (1470–1550), who published the first printed anatomy textbook, described the pancreas as a secretory gland, but without mentioning its duct. The oldest surviving drawing of the pancreas comes from Bartolomeo Eustachi , whose anatomical tables were published by Giovanni Maria Lancisi in 1714 . The organ is not shown in Leonardo da Vinci's detailed drawings ; it was probably removed with the mesentery from the sections . Andreas Vesalius , who initiated a renaissance in anatomy, made precise anatomical drawings and for the first time described the precise topography of the organ. He thought the pancreas was just a pillow of the stomach.
In 1642 Johann Georg Wirsung discovered the duct of the pancreas, but could not interpret its function. Wirsung made an engraving of the pancreas and duct and sent prints to numerous anatomists, asking for help in interpreting its function. This also reached Thomas Bartholin , who, in a letter to his brother-in-law Ole Worm, interpreted the duct as the duct of a pancreatic secretion and 10 years after Wirsung made an even more detailed drawing of the pancreas and its duct. Although Wirsung's numerous letters substantiate the first authorship of his discovery, according to his own statement, it was that of his son and, in the opinion of some medical historians, perhaps Wirsung's student Moritz Hofmann who first found the passage in a turkey , although he never published this discovery. The discovery of the additional duct (ductus pancreaticus accessorius) is attributed to Giovanni Domenico Santorini , although it was described by Thomas Wharton as early as 1656 . Santorini was the first to recognize that this additional gait is not a malformation, but a "normal" anatomical structure. The ontogenetic basis, namely the embryology of the pancreas, was discovered in 1812 by Johann Friedrich Meckel the Elder. J. described. Meckel also explained the origin of the split pancreas ( pancreas divisum ). In 1879 Albert von Kölliker discovered the two pancreatic systems. In 1711 (first published in 1720) Abraham Vater then precisely described the anatomy of the joint opening of the biliary and pancreatic ducts on the papilla Vateri, which is now named after him . As early as 1654, Francis Glisson discovered the small sphincter muscle at the junction of the biliary and pancreatic ducts. Ruggero Oddi examined its existence comparatively anatomically in 1887 and interpreted it functionally more precisely, which is why this sphincter muscle is now also named after Oddi (Musculus sphincter Oddi) .

With the discovery of the ducts of the pancreas and the ducts of the salivary glands in the middle of the 17th century, the way to the functional interpretation of the exocrine part was paved. After Thomas Bartholin suspected a secretion released by the pancreas into the intestines in 1651, Reinier de Graaf put the first pancreatic fistula in a dog in 1664 and was thus able to collect the secretion for the first time. The similarities of the salivary gland and pancreatic ducts found by De Graaf inspired Samuel Thomas von Soemmerring in 1796 to coin the German term “pancreas”, which is still used today. In 1669, Marcello Malpighi processed these findings in his book and concluded that the secretion chemically changes the food pulp in the intestine - the breakdown of food components by pancreatic enzymes was postulated.
At the end of the 17th century, Johann Konrad Brunner performed operations on dogs with partial removal of the pancreas and tying off of the ducts. However, he concluded from his experiments that the organ apparently does not have an essential function in digestion. In 1826 Leopold Gmelin and Friedrich Tiedemann recognized that pancreatic juice changed the food pulp into a form that the intestine could absorb. However, they suspected that saliva breaks down proteins and pancreatic juice breaks down starch. A little later Johann Eberle recognized the starch-splitting and fat- emulsifying properties of pancreatic juice. In 1838, four years later, Jan Evangelista Purkyně showed that fats are not only emulsified but also split when mixed with bile and pancreatic juice. This work was the starting point for extensive research by Claude Bernard , the "father of pancreatic physiology". In 1846 he discovered pancreatic lipase and realized that pancreatic juice can break down starches, fats and proteins into smaller molecules. The protein-splitting component trypsin was first isolated by Alexander Danilewski in 1862 and extracted almost in its pure form by Wilhelm Kühne in an improved process in 1876 . Ivan Pavlov and his students carried out numerous experiments at the end of the 19th century to control the formation of pancreatic juice, especially by the vagus nerve . Pavlov's student Nikolai Shepovalnikov discovered in 1899 that trypsin is only activated by the contents of the duodenum and thus by enteropeptidase . In their pancreas experiments in 1902, William Bayliss and his brother-in-law Ernest Starling found the very first hormone, secretin , which stimulates the pancreas . In 1928/1929 Andrew Conway Ivy and Eric Oldberg discovered the second enteric hormone that acts on pancreatic secretion, cholecystokinin , while the others were not detected until the 1970s.

With the improvement of light microscopes and microscopic techniques in the 19th century, the technical prerequisites for research into precision engineering were also given. Moyse presented the first histological description of the fine structure of the exocrine part in his dissertation in 1852, in which the acini was also described for the first time . In 1869 the German pathologist Paul Langerhans discovered the endocrine cell aggregates in the pancreas, later named after him as Langerhans islands, but could not interpret their function.
In 1880, Étienne Lancereaux recognized that diabetes, known since ancient times, is definitely related to changes in the pancreas. In 1889, Oskar Minkowski and Josef von Mering caused diabetes by removing the pancreas in dogs, but it was not until 1900 that the Russian Leonid Sobolew recognized the direct relationship with the Langerhans Islands, an observation that was experimentally confirmed in 1909 by William George MacCallum . From 1904 to 1908 Georg Ludwig Zülzer made numerous attempts to treat diabetes mellitus using pancreatic extracts. Although he achieved improvement in symptoms of diabetes, the severe side effects caused him to abandon his attempts. Michael Lane was able to differentiate between two cell types (α and β cells) for the first time in 1907 using different fixations , δ cells were discovered by William Bloom in 1931. Between 1938 and 1950, György Gömöri decisively developed the staining process for cell differentiation. They only lost their importance with the advent of immunohistochemical staining methods from 1976 onwards.
Frederick Banting and Charles Best are considered to be the discoverers of insulin . They isolated it from dog pancreases in 1921 and successfully used it to treat a diabetic boy in 1922. The Romanian Nicolae Paulescu had already produced an insulin-effective extract from pancreatic tissue in 1916 and patented the process in 1922, but only used it on dogs. In 1923, Charles P. Kimball and John R. Murlin discovered another hormone, glucagon, during extraction attempts . The vasoactive intestinal polypeptide was first isolated from a pancreatic tumor in 1966 by Jerry D. Gardner and James J. Cerda , and somatostatin in the pancreas was not isolated from islet cell tumors until 1977.
literature
- Hans-Gunther Beger u. a .: The Pancreas: An Integrated Textbook of Basic Science, Medicine, and Surgery . 2nd Edition. John Wiley & Sons, New York City 2009, ISBN 978-1-4443-0013-0 (English).
- Markus W. Büchler u. a .: pancreatic diseases. Acute pancreatitis, chronic pancreatitis, tumors of the pancreas . 2nd Edition. Karger, Basel 2004, ISBN 3-8055-7460-6 .
- Detlev Drenckhahn (ed.): Cell and tissue theory, development theory, skeletal and muscle systems, respiratory system, digestive system, urinary and genital system . 16th edition. Urban & Fischer, Munich 2003, ISBN 3-437-42340-1 .
- John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 (English).
- Franz-Viktor Salomon: Anatomy for veterinary medicine . 2nd Edition. Enke, Stuttgart 2008, ISBN 978-3-8304-1075-1 , pp. 321-323 .
- K. Zimmermann: pancreas. In: FX Sailer, FW Gierhake (ed.): Surgery seen historically: beginning - development - differentiation. von Industri-Verlag, Deisenhofen near Munich 1973, ISBN 3-87185-021-7 , pp. 89-106.
- Benedikt Ignatzek: pancreatic diseases. In: Werner E. Gerabek , Bernhard D. Haage, Gundolf Keil , Wolfgang Wegner (eds.): Enzyklopädie Medizingeschichte. De Gruyter, Berlin / New York 2005, ISBN 3-11-015714-4 , p. 1094 f.
Web links
Individual evidence
- ↑ Detlev Drenckhahn (Ed.): Anatomie, Volume 1 . 17th edition. Urban & Fischer, Munich 2008, ISBN 978-3-437-42342-0 , pp. 723 .
- ^ A b Walther Graumann, Dieter Sasse: Compact Textbook Anatomy, Volume 3 . Schattauer, Stuttgart 2004, ISBN 978-3-7945-2063-3 , pp. 120-122 .
- ↑ a b c d e Renate Lüllmann-Rauch: Histology . Georg Thieme, Stuttgart 2009, ISBN 978-3-13-129243-8 , pp. 408-413 .
- ^ A b Over Cabrera: The unique cytoarchitecture of human pancreatic islets has implications for islet cell function . In: Proceedings of the National Academy of Sciences (PNAS). 103, 2006, ISSN 0027-8424 , pp. 2334-2339, pnas.org (PDF; 800 kB).
- ↑ Helga Fritsch, Wolfgang Kühnel: Pocket Atlas of Anatomy: Inner organs . 10th edition. Georg Thieme, Stuttgart 2009, ISBN 978-3-13-492110-6 , p. 44-45 .
- ↑ Gerhard Aumüller u. a .: Dual series anatomy . 2nd Edition. Georg Thieme, Stuttgart 2010, ISBN 978-3-13-152862-9 , p. 675 .
- ↑ Michael Schünke u. a .: Prometheus - Learning Atlas of Anatomy: Internal Organs . 3. Edition. Georg Thieme, Stuttgart 2009, ISBN 978-3-13-139533-7 , p. 273 .
- ^ EJ Verspohl, R. Tacke, E. Mutschler, G. Lambrecht: Muscarinic receptor subtypes in rat pancreatic islets: binding and functional studies. In: European Journal of Pharmacology . 178, No. 3, March 1990, ISSN 0014-2999 , pp. 303-311, PMID 2187704 .
- ^ Vay Liang W. Go: The Pancreas - Biology, Pathophysiology and Disease . Ravers Press. Second Edition, ISBN 0-88167-986-0
- ↑ FC Brunicardi, D. Elahi, DK Andersen: splanchnic neural regulation of somatostatin secretion in the isolated perfused human pancreas. In: Annals of Surgery . 219, No. 3, March 1994, ISSN 0003-4932 , pp. 258-266, PMID 7908511 , PMC 1243133 (free full text).
- ↑ a b c d e f g R. S. Heller: The comparative anatomy of islets. In: Advances in Experimental Medicine and Biology . 654, 2010, ISSN 0065-2598 , pp. 21-37, doi : 10.1007 / 978-90-481-3271-3_2 , PMID 20217492 (review).
- ↑ a b c J. MW Slack: Developmental biology of the pancreas. In: Development 121, 1995, pp. 1569-1580, full text (PDF).
- ↑ David J. McKenzie et al .: Fish Physiology: Primitive Fishes: Primitive Fishes . (= Fish Physiology. Volume 26) Academic Press 2011, ISBN 978-0-08-054952-1 , p. 385.
- ↑ a b c P. J. Bentley: Comparative Vertebrate Endocrinology. Cambridge University Press, 1998, ISBN 978-0-521-62998-0 , p. 47.
- ↑ Franz-Viktor Salomon and Maria-Elisabeth Krautwald-Junghanns: pancreas. In: Anatomy for veterinary medicine. 2nd Edition. Enke, Stuttgart 2008, ISBN 978-3-8304-1075-1 , p. 779.
- ^ A b c Franz-Viktor Salomon: pancreas, pancreas. In: Anatomy for veterinary medicine. 2nd Edition. Enke, Stuttgart 2008, ISBN 978-3-8304-1075-1 , pp. 321-323.
- ↑ a b c Norbert Ulfig: short textbook embryology . Georg Thieme, Stuttgart 2009, ISBN 978-3-13-139582-5 , p. 109 .
- ↑ a b c Bertram Schnorr and Monika Kressin: Embryology of Pets . 6th edition. Georg Thieme, Stuttgart 2011, ISBN 978-3-8304-1147-5 , p. 181-182 .
- ↑ SB Smith et al .: Rfx6 directs islet formation and insulin production in mice and humans. In: Nature. 463, No. 7282, February 2010, ISSN 1476-4687 , pp. 775-780, doi: 10.1038 / nature08748 , PMID 20148032 , PMC 2896718 (free full text).
- ↑ E. Sh. Gerlovin: Evolutionary morphology and classification of pancreatic acinar-islets cells. In: T. Adesanya et al. (Ed.): The Evolution of Pancreatic Islets . Elsevier, 1976, ISBN 978-1-4832-8072-1 , pp. 113-120.
- ↑ OD Madsen: Pancreas phylogeny and ontogeny in relation to a 'pancreatic stem cell'. In: Comptes rendus biologies. 330, No. 6-7, 2007, ISSN 1631-0691 , pp. 534-537, doi: 10.1016 / j.crvi.2007.03.006 , PMID 17631449 , PMC 1988839 (free full text) (review).
- ↑ a b c Behrends et al. (Ed.): Dual series Physiology. Thieme, Stuttgart 2009, ISBN 3-13-138411-5 , pp. 492-494.
- ↑ Wolfgang von Engelhardt: Physiology of domestic animals . Georg Thieme, 2009, ISBN 978-3-8304-1078-2 , p. 410.
- ↑ Wolfgang von Engelhardt: Physiology of domestic animals . Georg Thieme, 2009, ISBN 978-3-8304-1078-2 , p. 415.
- ^ Detlef Doenecke: Karlsons Biochemie und Pathobiochemie . Georg Thieme, 2005, ISBN 978-3-13-357815-8 , pp. 536-539.
- ↑ Bernhard Kleine, Winfried Rossmanith: Hormone and hormone system - textbook of endocrinology. 3. Edition. Springer Spectrum, Berlin / Heidelberg 2014, ISBN 978-3-642-37091-5 , pp. 117, 120.
- ↑ Wolfgang Huber, Roland M. Schmid: Acute pancreatitis: Evidence-based diagnostics and therapy . (PDF; 291 kB). In: Deutsches Ärzteblatt . 104, No. 25, June 22, 2007, pp. A-1832-A-1841. Retrieved December 17, 2014.
- ↑ Johannes-Martin Hahn: Checklist internal medicine. Georg Thieme, 2010, ISBN 978-3-13-107246-7 , pp. 367-369.
- ↑ Verena Arzbach: Enzymes: can be used in many ways . In: PTA-Forum , issue 2/2016.
- ^ Edouard Battegay: Siegenthaler's differential diagnosis: Internal diseases - from symptom to diagnosis . 20th edition. Georg Thieme, 2012, ISBN 978-3-13-152520-8 , p. 315.
- ^ Information on pancreatic tumors , Center for Cancer Registry Data at the Robert Koch Institute. Retrieved December 17, 2014.
- ↑ Georg von Samson-Himmelstjerna et al .: Textbook of Parasitology for Veterinary Medicine . 3rd edition, Georg Thieme, 2012, ISBN 978-3-8304-1205-2 , p. 175.
- ^ JF Denton, JM Kinsella: Lyperosomum intermedium sp. N. (Digenea: Dicrocoeliidae) from the rice rat, Oryzomys palustris, from southeastern salt marshes. In: The Journal of parasitology. 58, No. 2, April 1972, ISSN 0022-3395 , pp. 226-228, PMID 5022855 .
- ^ IDF Diabetes Atlas 6th edition , International Diabetes Federation, 2014. Accessed December 17, 2014.
- ^ Reto Neiger: Differential Diagnoses of Internal Medicine in Dogs and Cats. Enke, 2009, ISBN 978-3-8304-1064-5 , p. 340.
- ↑ A. Raffel et al .: Hyperinsulinemic hypoglycemia due to adult nesidioblastosis in insulin-dependent diabetes. In: World Journal of Gastroenterology: WJG. 12, No. 44, November 2006, ISSN 1007-9327 , pp. 7221-7224, PMID 17131493 , PMC 4087792 (free full text).
- ↑ a b c Helmut Messmann: Clinical Gastroenterology: The book for advanced and advanced training plus DVD with over 1000 findings. Georg Thieme, 2011, ISBN 978-3-13-165991-0 , p. 709.
- ↑ Helmut Messmann: Clinical Gastroenterology: The book for advanced and advanced training plus DVD with over 1000 findings. Georg Thieme, 2011, ISBN 978-3-13-165991-0 , p. 710.
- ↑ Detlev Drenckhahn (ed.): Benninghoff: Anatomie. Macroscopic anatomy, histology, embryology, cell biology (Volume 1) . 16th edition. Urban & Fischer, Munich 2003, ISBN 3-437-42340-1 .
- ↑ Keith L. Moore: Embryology - Textbook and Atlas of the history of human development . 3. Edition. Schattauer, Stuttgart 1990, ISBN 3-7945-1356-8 .
- ↑ a b Jörg M. Steiner (Ed.): Small Animal Gastroenterology . Schlütersche, Hannover 2008, ISBN 978-3-89993-027-6 .
- ^ A b Paul Georg Lankisch, Iris Schmidt: Pancreatic function tests. In: Deutsches Ärzteblatt 96, 1996, full text (PDF), accessed on December 17, 2014.
- ↑ C. Löser, A. Möllgaard, UR Fölsch: Faecal elastase 1: a novel, highly sensitive, and specific tubeless pancreatic function test. In: Good. 39, No. 4, October 1996, ISSN 0017-5749 , pp. 580-586, PMID 8944569 , PMC 1383273 (free full text).
- ↑ Markus Vieten: Understanding laboratory values made easy: All important values from A – Z - laboratory diagnostics for the most common diseases . Georg Thieme, 2009, ISBN 978-3-8304-6284-2 .
- ↑ KS Goonetilleke, AK Siriwardena: Systematic review of carbohydrate antigen (CA 19-9) as a biochemical marker in the diagnosis of pancreatic cancer. In: European journal of surgical oncology: the journal of the European Society of Surgical Oncology and the British Association of Surgical Oncology. 33, No. 3, 2007, ISSN 0748-7983 , pp. 266-270, doi: 10.1016 / j.ejso.2006.10.004 , PMID 17097848 (review).
- ^ TR Srinivas and Daniel A. Shoskes: Kidney and Pancreas Transplantation: A Practical Guide . Springer Science & Business Media, 2010, ISBN 978-1-60761-642-9 .
- ↑ Pancreas Transplantation, German Organ Transplantation Foundation. Retrieved January 9, 2015.
- ^ P. Layer, J. Keller, PG Lankisch: Pancreatic enzyme replacement therapy. In: Current gastroenterology reports. 3, No. 2, 2001, ISSN 1522-8037 , pp. 101-108, PMID 11276376 (review).
- ^ Andreas Liebl, Eric Martin: Diabetes mellitus type 2: with 13 tables . Govi, Eschborn, 2005, ISBN 978-3-7741-1042-7 , p. 76.
- ↑ PatriCa BB: Chinese Tonic Soup with Pork Pancreas and Radishes on mywoklife.com, October 23, 2011. Last accessed on December 16, 2014.
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 3 .
- ^ A b John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 4 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 6 .
- ^ A b John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 9 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ. Springer, 2002, ISBN 0-306-46742-9 , p. 8.
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 12 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 16 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 22 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 20 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 28-29 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 17 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 32 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 34 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 38 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 40 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 43 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 52 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 55 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 58 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 68 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 75 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 77 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ. Springer 2002, ISBN 0-306-46742-9 , p. 83.
- ^ J. Reynolds Green: The Soluble Ferments and Fermentation. Cambridge University Press, 2014, ISBN 978-1-107-67395-3 , pp. 195-196.
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 88 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 89/90 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 93 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 59-60 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 105/106 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 107 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 111 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 112 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 113 .
- ^ SJ Cooperstein: The Islets of Langerhans: Biochemistry, Physiology, and Pathology . Elsevier, 2012, ISBN 978-0-323-14733-0 , pp. 5 .
- ^ SJ Cooperstein: The Islets of Langerhans: Biochemistry, Physiology, and Pathology . Elsevier, 2012, ISBN 978-0-323-14733-0 , pp. 8-9 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 117 .
- ↑ Vivienne Baillie Gerritsen: Protein of the 20th century . In: Protein Spotlight. April 9, 2001. Retrieved December 17, 2014.
- ^ CP Kimball, John R. Murlin: Aqueous extracts of pancreas. III. Some precipitation reactions of insulin. In: J. Biol. Chem. 58, 1923, pp. 337-346.
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 151 .
- ↑ John Malone Howard, Walter Hess: History of the Pancreas: Mysteries of a Hidden Organ . Springer, 2002, ISBN 0-306-46742-9 , pp. 152 .












